Dystonia And Pain Management For Parkinson’s
Movement disorder specialist Alfonso Fasano, MD, PhD, outlines how to tease apart whether pain is a symptom of PD or due to an orthopedic issue. He explains how to approach the treatment of pain in concert with your medical team, going over several treatment options. Finally, Dr. Fasano focuses on causes of and treatments for dystonia and dyskinesias. After a 40-minute talk he spends 30 minutes answering questions.
Parkinsons Patients With Severe Pain Benefit From Oxycodone
In a recent paper published in The Lancet Neurology, researchers evaluated the analgesic effect of prolonged-release oxycodone-naloxone in patients with Parkinsons disease suffering from severe and chronic pain in a pioneer Phase II clinical trial. Pain is a very common, non-motory symptom in PD patients and is one of the symptoms associated with a depressed mood and reduced quality of life. Pain in PD patients has commonly only been treated by increasing the doses of dopaminergic therapy, and so far there is no full understanding on the different types of pain these patients suffer from either a medical or patient perspective.
The multi-center, double-blind randomized placebo controlled trial, funded by Mundipharma and named PANDA, included 202 patients, 93 assigned to OXN PR and 109 to placebo. The primary endpoint was set to average 24-hour pain scores at 16 weeks in the full analysis population. Although this endpoint was not significant, results were encouraging given the statistically significant differences at week 4 , week 8 and week 12 . Also, secondary endpoints revealed OXN PR treated patients used less rescue medications and had clinically relevant improvements, relative to placebo. Moreover, researchers observed an improvement in severe musculoskeletal and severe nocturnal pain compared to placebo. However, secondary adverse effects like nausea and constipation were more frequent in patients taking OXN PR than those administered with placebo.
Contraindicated Drugs For Parkinsons Patients
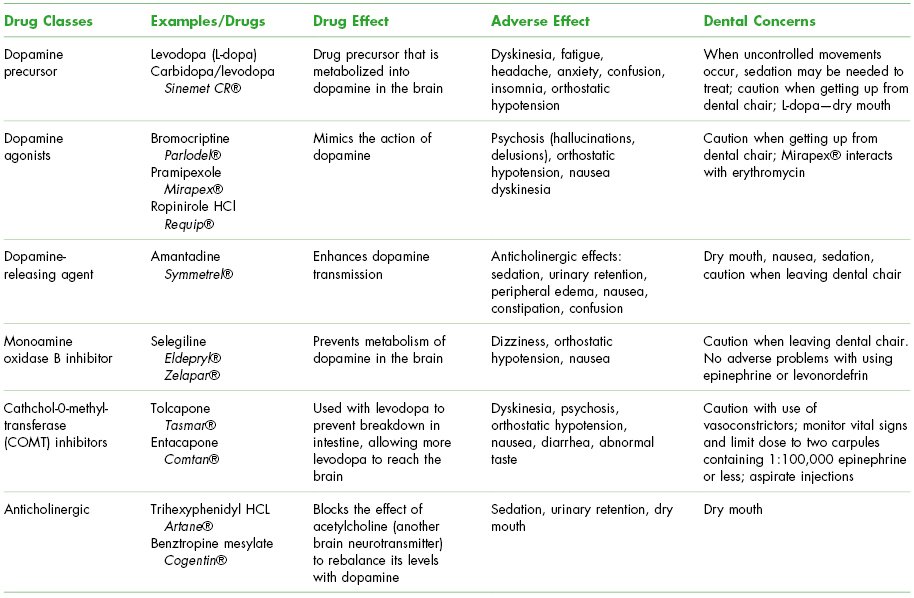
More than two dozen drugs should not be taken by Parkinsons patients because they alter the brains dopamine system. Always let your neurologist know before you have surgery, so he or she can work with your medical team to keep your Parkinsons in control. View a list of drugs that Parkinsons patients should not take.
You May Like: Parkinson Disease Medications To Avoid
Pain In Parkinsons Disease
Parkinsons patients suffer from the same pain other people have, often amplified by the motor dysfunction, but they also have additional pain problems unique to PD. Lower back pain and back of he neck pain are most common. Strengthening exercises or stretching may be helpful. Identifying the cause of the pain is essential in treating the pain. Treatments include physical therapy, medications, and alternative therapies like Reiki, acupuncture and massage.
Static And Dynamic Psychophysical Paradigms
So-called static psychosocial paradigms refer to a range of quantitative sensory testing protocols, which were recently standardised and defined by the German research network on neuropathic pain . In addition to sensory detection thresholds the DFNS protocol involves pain thresholds to thermal and mechanical stimuli. If QST responses are incongruous to normative reference values the dysfunction may be located anywhere along the neural axis, from peripheral nerve fibres,, to the spinal cord and cortical areas. However the value of QST to distinguish central and peripheral mechanisms is limited. Nociceptive withdrawal reflex thresholds offer a measure of central pain processing, specifically spinal nociceptive facilitation.
Read Also: What Part Of The Brain Does Parkinson’s Affect
What Is The Latest Treatment For Parkinsons
Research for new Parkinsons drugs and therapies is ongoing. Most people live a long time with Parkinsons disease, which means you might take medications for a long time. All of these main treatments cause side effects that are hard to live with, so new drugs to treat those side effects are also being studied.
Adenosine A2a antagonists
This medication was approved by the FDA in 2019 for Parkinsons disease as additional treatment alongside levodopa. It works by blocking a protein called the adenosine A2 receptor, which increases dopamine signaling. These medications lower off time and uncontrollable, jerky movements.
Other therapies
There are clinical trials and research happening for other therapies, including:
- Stem cell therapy that uses healthy cells to repair damage from Parkinsons
- Growth factors, which are proteins that support nerve cells and promote growth and survival
- Gene therapy to reprogram cells to stay healthy and work better for longer
- Drugs for side effects like NLX-112 that targets certain serotonin receptors
Lower Back Pain And Back Of The Neck Pain Are Most Common
Pain occurs for a number of reasons and its not always clear what the cause is, making it difficult to figure out how best to treat it. I believe that most common pain problems in Parkinsons Disease are the same as in the general population, but amplified. Low back pain and back of the neck pain are probably the most common pain conditions in PD. The reason Parkinsons Disease patients have so many problems with their low back and their neck is their posture. Parkinsons Disease causes a stooped posture. Some of this happens with age anyway, particularly in women after menopause when their bones soften, but is always worse from the PD. All Parkinsons Disease patients have some degree of stooped posture and many also tilt to one side. Because of the stooped posture, the muscles in the lower back have to pull much harder to keep the spine upright.
Don’t Miss: Electronic Implant For Parkinson’s
Functional Exercise For Chronic/persistent Pain
There are some simple exercises that you can try around the house to help:
- If you experience pain in your legs, keep them strong by practising standing up and sitting down in a chair.
- If your shoulders are aching, start by loosening them with some shoulder rolling actions, then by lifting an object that is slightly weighty from a shelf, and then replacing it. This increases the range of movement in your back, shoulders and arms, and then your strength.
Withdrawal Syndrome With Levodopa
Research has shown that withdrawal symptoms can happen when someone very suddenly stops taking levodopa, perhaps because they are experiencing impulsive and compulsive behaviour. It can lead to symptoms such as depression, anxiety and pain. Any withdrawal from Parkinsons medications needs to be done gradually, under the supervision of a health professional, to avoid the risk of developing this syndrome.
Dont Miss: Tell Me About Parkinsons
You May Like: Mri Guided Ultrasound Parkinson’s
Common Drugs For Parkinson’s Disease
Levodopa and carbidopa . Levodopa is the most commonly prescribed medicine for Parkinsonâs. Itâs also the best at controlling the symptoms of the condition, particularly slow movements and stiff, rigid body parts.
Levodopa works when your brain cells change it into dopamine. Thatâs a chemical the brain uses to send signals that help you move your body. People with Parkinsonâs donât have enough dopamine in their brains to control their movements.
Sinemet is a mix of levodopa and another drug called carbidopa. Carbidopa makes the levodopa work better, so you can take less of it. That prevents many common side effects of levodopa, such as nausea, vomiting, and irregular heart rhythms.
Sinemet has the fewest short-term side effects, compared with other Parkinsonâs medications. But it does raise your odds for some long-term problems, such as involuntary movements. An inhalable powder form of levodopa and the tablet istradefylline have been approved for those experiencing OFF periods, OFF periods can happen when Parkinsonâs symptoms return during periods between scheduled doses of levodopa/carbidopa.
People who take levodopa for 3-5 years may eventually have restlessness, confusion, or unusual movements within a few hours of taking the medicine. Changes in the amount or timing of your dose will usually prevent these side effects.
Dopamine agonists. These drugs act like dopamine in the brain. They include pramipexole , rotigotine , and ropinirole , .
Pain Management In Patients With Parkinsons Disease: Challenges And Solutions
This review focuses on the diagnosis and management of Parkinson-related pain. It reviews the incidence and prevalence of PD, general pain and PD-related pain, the pathophysiological pathways of pain in PD, physiological pathways of pain relief, measurements of pain, clinical diagnosis of PD-related pain, and treatment strategies.
Recommended Reading: Computer Mouse For Parkinson’s
Shooting Pain And Paraesthesia
Radicular pain is a sharp pain that shoots down a limb and often affects fingers or toes. Paraesthesia is sometimes described as a feeling of pins and needles or perhaps numbness in a limb which has fallen asleep. Such pain is usually related to trapped nerves in the spinal cord and can feel similar to an electric shock, a tingling or a burning sensation.
Treatment: Painkillers and exercise will generally settle the pain. If not your specialist may refer you for tests such as an MRI scan to check for a trapped nerve in the spinal cord.
Negative Impact Of Severity Of Pain On Mood Social Life And General Activity In Parkinson’s Disease
This case control study designed for clinicians and rehabilitation specialists to effectively identify pain from the patient’s point of view determined that PD patients had significantly higher pain severity scores compared to controls. PD patients with depressive symptoms had significantly higher pain severity and pain interference scores than controls without depressive symptoms. PD patients reported greater scores on Global BPI pain interference and all components of the pain interference subscale. Therefore, PD and depression seem to be correlated with higher perceived pain, severity and interference. A report on this study, by Jose Marques Lopes, PhD., was published in Parkinson’s News Today, September 21, 2018.
Don’t Miss: Can Trauma Cause Parkinson’s Disease
How Is Pain Treated In Patients With Parkinson Disease
Pain serves as 1 of the most frequent nonmotor complaints in patients with Parkinson disease , affecting 68% to 95% of patients across all clinical stages. Published in the Journal of Parkinson Disease, researchers highlight that similar to PD, pain is complex and even has different classifications of subtypes within the disease.
While prominent, real-life pain data in PD remains scarce. Researchers sought to provide an overview on pain in PD, including classification, assessment, presentation, and the existing therapy landscape.
As researchers highlighted, todays classifications of pain in PD include musculoskeletal, radicular/neuropathic, dystonia-related, akathic discomfort/pain, and central pain. Notably, the difference in pain directly related to PD and central pain, which is attributed to objective painprocessing and pain-perception disturbance within ascending and descending pathways, was referenced. Most frequently, pain presents as musculoskeletal/nociceptive pain in PD patients, but in nearly half of the PD population, comorbid conditions, such as spine and joint arthrosis, serve as contributors.
When it comes to treating pain in PD, interventions remain a major unmet need as only approximately 50% of those with the disease receive at least some type of pain therapy. In managing pain, researchers recommend that therapy should be optimized to address dopaminergic issues, which has been shown to be effective in 30% of patients with PD.
Reference
Search Strategy And Literature Sources
We reviewed both pharmacological and non-pharmacological treatments for pain in patients with PD. We searched for studies cataloged in PubMed and the Cochrane library, to October 31, 2019. An initial search was conducted between February and June 2018. An updated search was performed in November 2019 to look for new publications. The keywords Parkinson, pain, and treatment OR management were combined with and to search within the title and abstract fields for each database. We also included relevant keyword derivatives, such as Parkinsons Disease, Parkinsons, and PD. In addition to the title and abstract fields, we searched reference sections for all included articles.
You May Like: Cbd Dosage For Parkinson’s
Pain Presentation And Assessment In Pd
Most epidemiological data are based on questionnaires which were not specifically validated for PD patients so that results have to be interpreted with caution. The Kings Parkinsons disease pain scale is to date the only questionnaire that is specifically calibrated and validated for PD and is highly recommended to qualitatively and quantitatively assess pain and to ascribe the pain pathophysiologically. The scale contains seven different pain domains comprising musculoskeletal pain, chronic pain , fluctuation-related pain, nocturnal pain, oro-facial pain, discolouration or oedema/swelling and radicular pain as well as 14 sub-categories . This assessment tool is based on the pain classification according to Ford but also considers pain types of other classifications such as motor fluctuations or visceral pain .
In addition, there are some specific pain syndromes in PD which have to be kept in mind, including the so-called coat-hanger pain that occurs in cases of pronounced orthostatic dysregulation and although it is more frequent in multisystem atrophy it can occur also in PD and is often associated with strong headache and neck pain . Furthermore, pain due to constipation which is frequent in PD can cause abdominal pain.
Painful Symptoms Of Parkinsons Disease
Pain can sometimes be an early symptom of PD. For example, a person may complain of a painful shoulder and be diagnosed with an orthopedic condition such as a frozen shoulder, only to develop a rest tremor on that side at a later point. The painful shoulder was in fact not a frozen shoulder after all, but rather pain due to the rigidity of PD. Now of course, sometimes a frozen shoulder is really just a frozen shoulder, so theres no need to jump to conclusions when you are experiencing pain. Not every ache and pain is a sign of PD, but it is important for you to educate yourself, be aware of the possible connections, and be proactive about seeking medical attention for any notable pain you are experiencing.
If you have PD and develop pain, it is important to first bring this to the attention of your doctor. The pain may be related to your PD, or the pain may be due to a common problem such as arthritis which is exacerbated by your PD. However, in some cases, it may be a symptom of a more serious medical problem. So do not assume that the pain is related to your PD before getting an appropriate medical workup.
Recommended Reading: How Do You Know If You Have Parkinson’s
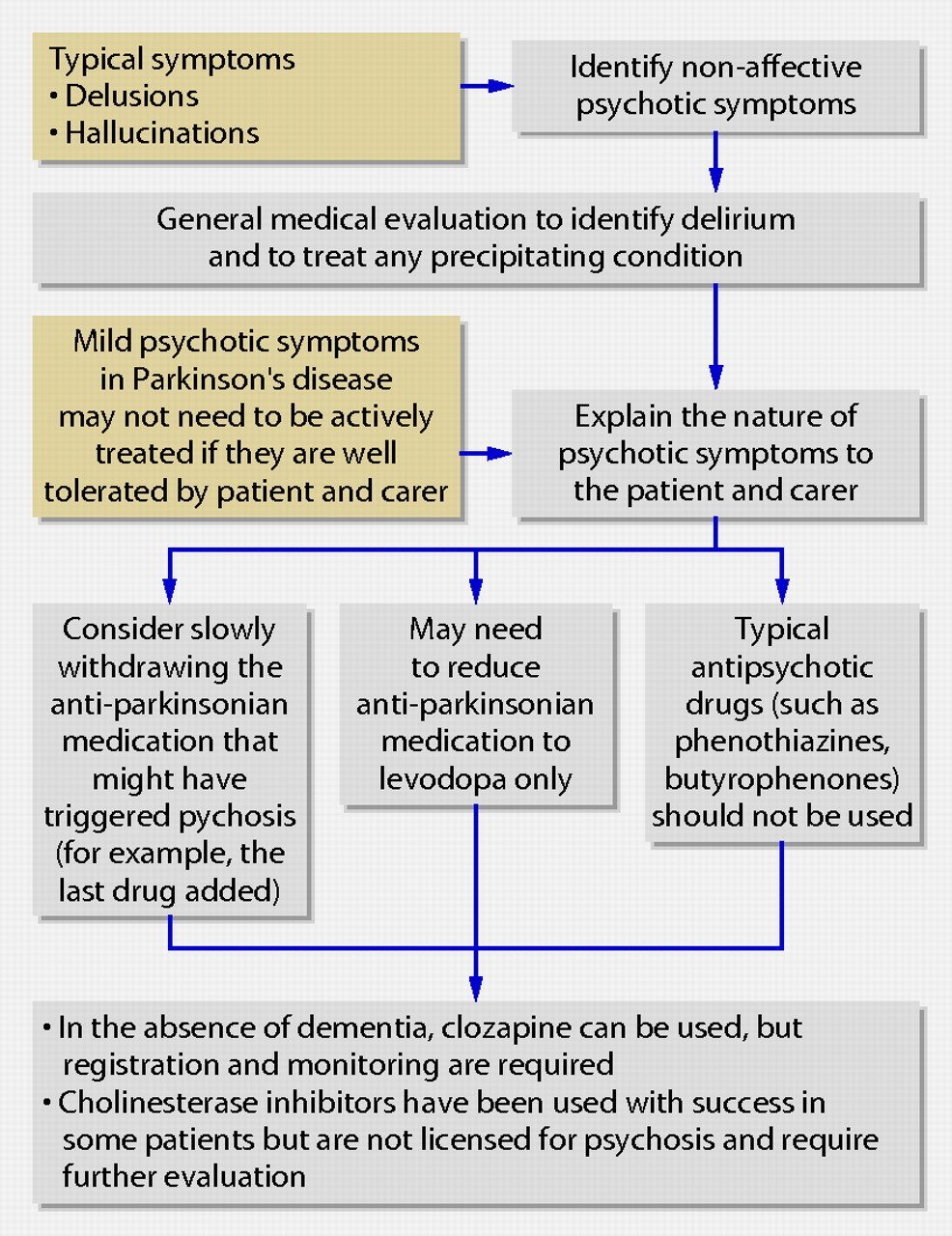
Antipsychotic Drugs Called Neuroleptics
Drug-induced parkinsonism is due primarily to drugs that block dopamine receptors, particularly the D2 receptors . These drugs are most often the antipsychotic drugs, called neuroleptics, such as haloperidol, chlorpromazine, and trifluoperazine, but include metoclopramide, a gastrointestinal motility enhancer, and the antiemetics prochlorperazine and droperidol. In addition, medications that block synthesis of dopamine, such as alpha-methyl para-tyrosine and alpha-methyl dopa or deplete dopamine also induce parkinsonism. In these cases the pathophysiology is presumably due to diminished dopamine receptor stimulation, resulting in a pharmacologic state closely resembling Parkinson disease.
However, the atypical antipsychotics also block D2 receptors. Yet there is no apparent correlation between the degree of this blockade and the risk for inducing parkinsonism. The explanation for this is uncertain. One current hypothesis is the fast off theory, postulating that the duration of the D2 blockade, rather than the percentage of receptors blocked, determines the likelihood of parkinsonism . A competing theory is that the ratio of 5 HT-2a receptor blockade versus the dopamine D2 receptor blockade is critical because of the interplay between the serotonin and dopamine systems in the brain. An older theory relating extrapyramidal side effects to anticholinergic activity is considered untenable because the concomitant use of anticholinergics does not eliminate the problem.
Considerations For The Inpatient Management Of Parkinsons Disease
Recognising and managing certain complications of Parkinsons disease can help improve care and reduce the risk of admission for people living with the condition.
Degenerative neurological disorders
Sergio Azenha / Alamy Stock Photo
Parkinsons disease is a neurological disorder in which there is progressive death of dopaminergic neurones in the substantia nigra the part of the mid-brain responsible for managing movement and the dopaminergic system with more than 50% of cell death occurring before symptom manifestation. The subsequent deficiency of dopamine synthesis, owing to this cell death, leads to the progression of motor symptoms including bradykinesia, rigidity, tremor and postural instability,.
Around 137,000 people in the UK have a PD diagnosis. The cause of the disease is yet to be discovered, but a combination of environmental and genetic factors are thought to increase its risk. Despite this, there is a lack of robust, large-scale evidence of a definitive link between any specific environmental risk factors. Around 20% of patients affected by PD have a first-degree relative that is affected by the disease. Prevalence is higher with increasing age and men appear to be at higher risk of developing the disease than women,. Patients with PD have a reduced life expectancy and studies have suggested up to a five-times higher mortality rate than people in the same age group without PD.
Dont Miss: Drugs That Cause Parkinson Like Symptoms
Also Check: 5 Signs You Ll Get Parkinson’s
What Makes Parkinsons Disease Worse
Stress and depression have been shown to exacerbate symptoms. You should also avoid medications that block dopamine, which includes some headache and gastrointestinal medications. Even if you avoid these, inevitably, Parkinsons disease will progress and time will, unfortunately, bring worsening symptoms.
Specific Warning About Mucuna

We assume that all contraindications, interactions, precautions and side effects that we know about synthetic levodopa should be considered when taking levodopa from mucuna.
Specific contraindications include thinning of the blood , and care should be taken with antiplatelet and anti-inflammatory drugs because mucuna increases clotting time.
Mucuna should not merge with anticoagulants or with antiplatelet drugs such as clopidogrel. Caution should be exercised and the additive effect should be taken into account if it is associated with acetylsalicylic and NSAIDs .
We should also be careful with antidiabetic medicines: mucuna lows glycemic index, and thus is to be considered a potential additive effect. Other interactions are possible, so always consult your regular doctor.
On the one hand, it can be argued that mucuna has been used for many centuries in India and has been available for several years online without a prescription, and yet serious problems have not been revealed. But that is just an observation.
Regarding Sinemet and Madopar, we have thousands of controlled studies, while publications on mucuna are still scarce. One must therefore use greater caution when choosing mucuna. While the future appears to be positive, we need the confirmation of more scientific studies.
Also Check: Can You Be Tested For Parkinsons
Don’t Miss: Neural Transplantation For The Treatment Of Parkinson’s Disease