How Effective Is Brain Surgery For Parkinsons Disease
Parkinson’s disease surgery known as deep brain stimulation is one of the possible treatment options for Parkinson’s disease. Deep brain stimulation was initially approved to ease tremors in PD patients in 1997, but it was later used to treat patients in the advanced stages of Parkinson’s disease. The surgery is also offered to patients in the early stages of Parkinson’s disease who do not respond to medication. Learn more about the effectiveness of Parkinson’s disease surgery and what it involves.
How Does The Neurosurgeon Know Where To Place The Electrodes In My Brain
Positioning the electrodes in the brain is the most critical step. The electrodes have to be placed in an exact location in the brain to improve symptoms. Computed tomography or magnetic resonance imaging scans are taken before and/or during the procedure to pinpoint the exact areas to target and guide the lead and electrode placement. Many times an electrode may be used to record brain cell activity at the target site to improve lead placement.
What Causes Parkinsons Disease
Parkinsons comes under the dementia umbrella. Its adegenerative disease of the nervous system that causes a loss of motor skillsand intentional movement. When someone has Parkinsons, the part of the brainthat controls muscular movements and mood function doesnt receive enough ofthe crucial dopamine chemical. Without enough dopamine, bodily movements,learning abilities and mood levels are severely affected. So-called normalfunctions such as speaking, writing, swallowing, walking and sleeping become difficultto perform. These challenges, combined with a lowering of mood levels is whymany Parkinsons patients suffer with depression.
Also Check: On Off Phenomenon
How Deep Brain Stimulation Works
Exactly how DBS works is not completely understood, but many experts believe it regulates abnormal electrical signaling patterns in the brain. To control normal movement and other functions, brain cells communicate with each other using electrical signals. In Parkinson’s disease, these signals become irregular and uncoordinated, which leads to motor symptoms. DBS may interrupt the irregular signaling patterns so cells can communicate more smoothly and symptoms lessen.
Preoperative Use Of Levodopa
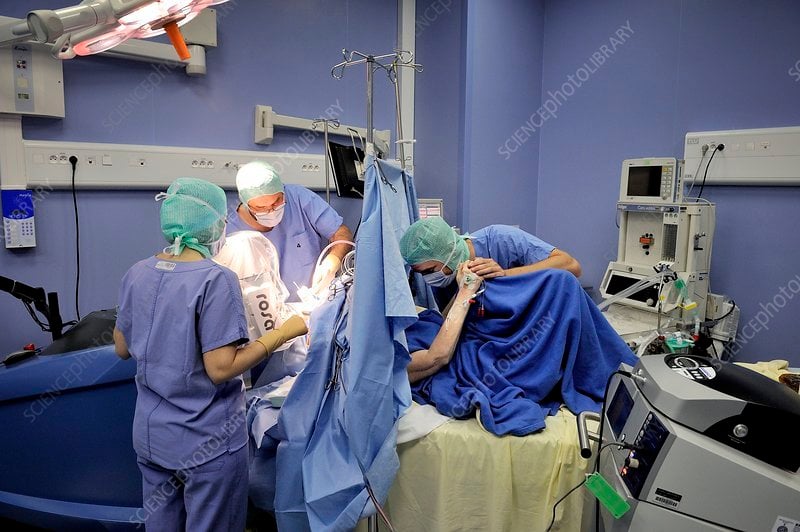
Patients with advanced Parkinson’s disease are at risk for exacerbations in the perioperative period. The timing of doses of Parkinson’s medication is very important, as abrupt withdrawal of drugs can often cause a very sudden return or even worsening of symptoms and in some cases can lead to the development of a condition known as neuroleptic malignant syndrome, which can be very dangerous. The half-life of levodopa is 13 h and so interruption should be as brief as possible, and therapeutic administration should be continued through the morning of surgery with sips of water. As it is absorbed from the proximal small bowel and thus has to first traverse the stomach making administration of tablets through gastric tube suboptimal or ineffective, because patients with Parkinson’s often have delayed gastric emptying. As such a duodenal feeding tube may be necessary when a prolonged period of normal feeding is expected. Patients may self-administer additional levodopa, so it is important to find out exactly how much they are taking.
Enteral levodopa has a clear advantage over intravenous levodopa and should be preferred. Treatment with and drug titration of levodopa for intravenous administration alone may be dangerous during general anesthesia because of interactions with anesthetic agents. It may increase the risk of a variety of arrhythmias or hypertension. These side effects of levodopa are mediated through its metabolite, dopamine.
Recommended Reading: Parkinson Bicycle Cleveland Clinic
Diagnosis Of Parkinsons Disease
A number of disorders can cause symptoms similar to those of Parkinson’s disease. People with Parkinson’s-like symptoms that result from other causes are sometimes said to have parkinsonism. While these disorders initially may be misdiagnosed as Parkinson’s, certain medical tests, as well as response to drug treatment, may help to distinguish them from Parkinson’s. Since many other diseases have similar features but require different treatments, it is important to make an exact diagnosis as soon as possible.
There are currently no blood or laboratory tests to diagnose nongenetic cases of Parkinson’s disease. Diagnosis is based on a person’s medical history and a neurological examination. Improvement after initiating medication is another important hallmark of Parkinson’s disease.
What Diseases And Conditions Resemble Parkinsons Disease
PD is the most common form of parkinsonism, in which disorders of other causes produce features and symptoms that closely resemble Parkinsons disease. Many disorders can cause symptoms similar to those of PD, including:
Several diseases, including MSA, CBD, and PSP, are sometimes referred to as Parkinsons-plus diseases because they have the symptoms of PD plus additional features.
In very rare cases, parkinsonian symptoms may appear in people before the age of 20. This condition is called juvenile parkinsonism. It often begins with dystonia and bradykinesia, and the symptoms often improve with levodopa medication.
Recommended Reading: Diseases Similar To Parkinsons
What Happens During Surgery
For stage 1, implanting the electrodes in the brain, the entire process lasts 5 to 7 hours. The surgery generally lasts 3 to 4 hours.
Step 1: attach stereotactic frameThe procedure is performed stereotactically, which requires attaching a frame to your head. While you are seated, the frame is temporarily positioned on your head with Velcro straps. The four pin sites are injected with local anesthesia to minimize discomfort. You will feel some pressure as the pins are tightened .
Step 2: MRI or CT scanYou will then have an imaging scan, using either CT or MRI. A box-shaped localizing device is placed over the top of the frame. Markers in the box show up on the scan and help pinpoint the exact three-dimensional coordinates of the target area within the brain. The surgeon uses the MRI / CT scans and special computer software to plan the trajectory of the electrode.
Step 3: skin and skull incisionYou will be taken to the operating room. You will lie on the table and the stereotactic head frame will be secured. This prevents any small movements of your head while inserting the electrodes. You will remain awake during surgery. Light sedation is given to make you more comfortable during the initial skin incision, but then stopped so that you can talk to the doctors and perform tasks.
What Are The Disadvantages
As with any surgical procedure there are risks, for example cognitive changes, speech problems and increased risk of stroke. These should all be discussed with your doctor in advance.
There is a 2-3% risk of a serious and permanent complication such as paralysis, seizure or infection, or changes in personality, memory and thinking. You also need to bear in mind that there are no guarantees that symptoms will improve after surgery, although in a majority of cases they do.
See also Surgical therapies.
You May Like: On And Off Phenomenon
What Are The Results
Successful DBS is related to 1) appropriate patient selection, 2) appropriate selection of the brain area for stimulation, 3) precise positioning of the electrode during surgery, and 4) experienced programming and medication management.
For Parkinson’s disease, DBS of the subthalamic nucleus improves the symptoms of slowness, tremor, and rigidity in about 70% of patients . Most people are able to reduce their medications and lessen their side effects, including dyskinesias. It has also been shown to be superior in long term management of symptoms than medications .
For essential tremor, DBS of the thalamus may significantly reduce hand tremor in 60 to 90% of patients and may improve head and voice tremor.
DBS of the globus pallidus is most useful in treatment of dyskinesias , dystonias, as well as other tremors. For dystonia, DBS of the GPi may be the only effective treatment for debilitating symptoms. Though recent studies show little difference between GPi-DBS and STN-DBS.
Patients report other benefits of DBS. For example, better sleep, more involvement in physical activity, and improved quality of life.
Recent research in animals suggest that DBS may “protect” or slow the death of dopamine nerve cells . While the scientific data is inconclusive, observation of DBS patients show potential slowing of the disease relative to their pre-DBS condition.
Will I Be Asleep During The Entire Procedure
You will be sedated or receive local anesthesia for part of the procedure, may or may not be awake for lead and electrode placement, and will be asleep when the impulse generator is implanted. To provide more details:
- A local anesthetic is applied to areas of the head where pins or screws are used to secure the head frame and sedation is given.
- You will be sedated during the beginning of the procedure, while the surgical team is opening the skin and drilling the opening in the skull for placement of the lead.
- Most patients will be awake for lead and electrode placement. This part of the procedure is not painful, as the brain does not feel pain. Being awake allows the surgical team to interact with you when testing the effects of the stimulation. However, some patients who cannot tolerate the procedure while awake can have the electrode and lead placed under general anesthesia. The lead placement is guided in real time by magnetic resonance imaging. The procedure is performed in a special MR-equipped operation room.
- Implantation of the pulse generator in the chest and connection of the leads from the device to the lead in the brain is usually done under general anesthesia.
Don’t Miss: Yopd Life Expectancy
Home Remedyfor Parkinsons #8 Green Tea:
Green tea contains theanine, a nutrient that increasesdopamine levels in the brain, and polyphenol antioxidants that help fight free radicals. Three separate studies all found that regularlydrinking tea can either delay or prevent the development of PD. A retrospectivestudy also found that drinking three or more cups of tea a day can delay the onsetof motor symptoms. And a 2007 study found that green tea polyphenols protect braincells and dopamine neurons, and this positive effect increases with the moregreen tea consumed. 10
The minimum amount that should be drank every day is 3cups, with 6-9 cups a day being the ideal.Matcha green tea is the most potent and beneficial so try and purchase this ifyou can. A strong cup of coffee first thing in the morning is thought tobe effective for reducing the symptoms of Parkinsons disease as well, however,we recommend you stick with green tea, or even a strong cup of black tea ifyou can for the theanine and EGCGs.
Living With A Stimulator
Once the DBS has been programmed, you are sent home with instructions for adjusting your own stimulation. The handheld controller allows you turn the stimulator on and off, select programs, and adjust the strength of the stimulation. Most patients keep their DBS system turned on 24 hours day and night. Some patients with essential tremor can use it during the day and turn off the system before bedtime. Your doctor may alter the settings on follow-up visits if necessary.
If your DBS has a rechargeable battery, you will need to use a charging unit. On average charging time is 1 to 2 hours per week. You will have a choice of either a primary cell battery or a rechargeable unit and you should discuss this with you surgeon prior to surgery.
Just like a cardiac pacemaker, other devices such as cellular phones, pagers, microwaves, security doors, and anti theft sensors will not affect your stimulator. Be sure to carry your Implanted Device Identification card when flying, since the device is detected at airport security gates.
Also Check: Judy Woodruff Health Problems
Symptomatic And Neuroprotective Therapy
Pharmacologic treatment of Parkinson disease can be divided into symptomatic and neuroprotective therapy. At this time, there is no proven neuroprotective or disease-modifying therapy.
Levodopa, coupled with carbidopa, a peripheral decarboxylase inhibitor , remains the gold standard of symptomatic treatment for Parkinson disease. Carbidopa inhibits the decarboxylation of levodopa to dopamine in the systemic circulation, allowing for greater levodopa distribution into the central nervous system. Levodopa provides the greatest antiparkinsonian benefit for motor signs and symptoms, with the fewest adverse effects in the short term however, its long-term use is associated with the development of motor fluctuations and dyskinesias. Once fluctuations and dyskinesias become problematic, they are difficult to resolve.
Monoamine oxidase -B inhibitors can be considered for initial treatment of early disease. These drugs provide mild symptomatic benefit, have excellent adverse effect profiles, and, according to a Cochrane review, have improved long-term outcomes in quality-of-life indicators by 20-25%.
Neuroprotective therapy aims to slow, block, or reverse disease progression such therapies are defined as those that slow underlying loss of dopamine neurons. Although no therapy has been proven to be neuroprotective, there remains interest in the long-term effects of MAO-B inhibitors. Other agents currently under investigation include creatine and isradipine.
How To Choose Among Surgical Therapies In Pd
Different surgical treatment options can be considered in selected PD patients to improve motor symptoms that are poorly controlled with oral medications. Both DBS or lesioning surgeries have shown to reduce “off time” and dyskinesia, treat medication-resistant tremor, and improve quality of life. Deciding on a specific therapy requires a multidisciplinary team and is tailored towards the individual patient, based on their symptoms, expectations, riskbenefit ratio, and local expertise.
Patients with significant cognitive impairment, those with unstable psychiatric symptoms , or those with significant medical comorbidities are not good surgical candidates for DBS or lesioning procedures. Some patients may opt against neurosurgical procedures based on personal beliefs and risk tolerance. For those patients, other advanced therapies including levodopacarbidopa intestinal gel infusion or continuous subcutaneous apomorphine infusion options should be considered. An in-depth discussion of infusion devices is beyond the scope of this review article, but a brief comparison of surgical procedures with other advanced therapies is presented in Table 3.
Table 3 Comparison of surgical therapies with other advanced treatments for PD
You May Like: Zhichan Capsule
Complementary And Supportive Therapies
A wide variety of complementary and supportive therapies may be used for PD, including:
A healthy diet. At this time there are no specific vitamins, minerals, or other nutrients that have any proven therapeutic value in PD. The National Institute of Neurological Disorders and Stroke and other components of the National Institutes of Health are funding research to determine if caffeine, antioxidants, and other dietary factors may be beneficial for preventing or treating PD. A normal, healthy diet can promote overall well-being for people with PD just as it would for anyone else. Eating a fiber-rich diet and drinking plenty of fluids also can help alleviate constipation. A high protein diet, however, may limit levodopas absorption.
Exercise. Exercise can help people with PD improve their mobility, flexibility, and body strength. It also can improve well-being, balance, minimize gait problems, and strengthen certain muscles so that people can speak and swallow better. General physical activity, such as walking, gardening, swimming, calisthenics, and using exercise machines, can have other benefit. People with PD should always check with their doctors before beginning a new exercise program.
Alternative approaches that are used by some individuals with PD include:
Who Gets Parkinsons Disease
Risk factors for PD include:
- Age. The average age of onset is about 70 years, and the incidence rises significantly with advancing age. However, a small percent of people with PD have early-onset disease that begins before the age of 50.
- Sex. PD affects more men than women.
- Heredity. People with one or more close relatives who have PD have an increased risk of developing the disease themselves. An estimated 15 to 25 percent of people with PD have a known relative with the disease. Some cases of the disease can be traced to specific genetic mutations.
- Exposure to pesticides. Studies show an increased risk of PD in people who live in rural areas with increased pesticide use.
Read Also: Fitflop Shoes For Parkinson’s
Intraoperative Exacerbation Of Parkinson’s Disease
Manifestations begin with fine skeletal muscle tremors that are grossly unrecognizable. Under regional anesthesia an acute exacerbation may present with patient remaining awake and alert and complaining of subjective feelings of discomfort. Examination of the patient’s chest and upper extremities reveals fine tremors that progress to more gross tremors and rigidity within 515 min. Skeletal muscle activity progressing to rigors can hinder the quality of surgical repair and prolong the operating time. In electrocardio gram a coarse fibrillatory pattern may be seen, which may be due to fine skeletal muscle tremors. This can be mistaken for ventricular fibrillation and the initial response to perform electrical defibrillation is unnecessary and potentially deleterious.
Arterial blood pressure, heart rate, respiratory rate, and oxygen saturation are usually unchanged. Levodopa and carbidopa can be given orally with a sip of water while surgery continued. Motor activity and the subjective feelings of discomfort usually resolve approximately 20 min after initiating therapy.
Patients with advanced Parkinson’s disease are at risk for exacerbations in the perioperative period. Even with patients complying with perioperative levodopa therapy, sometimes due to an unforeseen delay in the time of surgery, signs and symptoms of exacerbation may be seen intraoperatively.
The Symptoms That Dbs Treats
Deep brain stimulation is used primarily to treat the motor symptoms of Parkinsons disease, but this can vary somewhat between the different placement sites. Symptoms treated include:
- Stiffness
- Abnormal movements : Dyskinesias are often a side effect of medications for Parkinsons disease and include involuntary movements such as twisting, head bobbing, squirming, and more.
DBS is not usually helpful with walking problems or balance, though improvements in the symptoms above can indirectly affect walking. It also does not provide significant benefits for non-motor symptoms of Parkinsons such as cognitive changes, mood changes , or problems with sleeping.
The benefits of DBS can be estimated by looking at how a person responds to levodopa. Symptoms that respond to levodopa will often respond to DBS . But symptoms that are not changed with levodopa are unlikely to be improved by DBS.
DBS often allows for a reduction in the dosage of levodopa, which in turn can result in fewer involuntary movements and a reduction in off time. The result is often improved quality of life.
Also Check: Weighted Silverware