What Is The Prognosis For Someone With Early
One of the challenges of early-onset Parkinsons disease is that you will inevitably live longer with the condition, as Parkinsons alone is not fatal. Early-onset Parkinsons disease does not always present the same way as late-onset Parkinsons disease, and there is no definite prognosis. Younger Parkinsons patients may be more at risk of developing non-motor symptoms, such as depression, sleep disorders, anxiety and urinary issues, which can cause health complications as the disease progresses.
However, early-onset patients also show slower disease progression, and it can take years to move between stages. Each case of Parkinsons is reviewed on an individual basis, so only your doctor can tell you your prognosis.
The Last Year Of Life In Parkinson’s Disease
The study also examined nearly 45,000 hospitalizations in people with terminal Parkinson’s, meaning their end-of-life period.
Of those with terminal PD, the most common reasons for being in the hospital were:
- Infection
- Heart disease
- Lung disease that was not from an infection
Less common causes for hospitalization were problems related to the stomach or intestines, muscles, nervous system, or endocrine system .
It is not surprising that infection was the most common hospitalization before death, as people with Parkinson’s are vulnerable to developing a number of infections as a result of their disease. For example, bladder dysfunction in Parkinson’s increases a person’s risk of developing urinary tract infections, which can become life-threatening if not detected and treated promptly.
In addition, research suggests that aspiration pneumonia is 3.8 times more common in people with Parkinson’s as compared to the general population. It has also been consistently reported to be the main cause of death in people with Parkinson’s.
Aspiration pneumonia results from underlying swallowing difficulties, which leads to stomach contents being inhaled into the lungs. Immobilization and rigidity, which can impair phlegm removal, also contribute to the development of pneumonia in people with Parkinson’s.
Increased Mortality In Young
1Department of Neuromedicine and Movement Science , NTNU, Faculty of Medicine and Health Sciences, Trondheim, Norway
2Department of Research and Innovation, More and Romsdal Hospital Trust, Ålesund, Norway
3Department of Neurosurgery, St. Olavs Hospital, Trondheim, Norway
4Department of Neurology, St. Olavs Hospital, Trondheim, Norway
Also Check: How Do They Test You For Parkinson’s Disease
Mean Life Expectancy In Patients With Pd Compared With The General Population
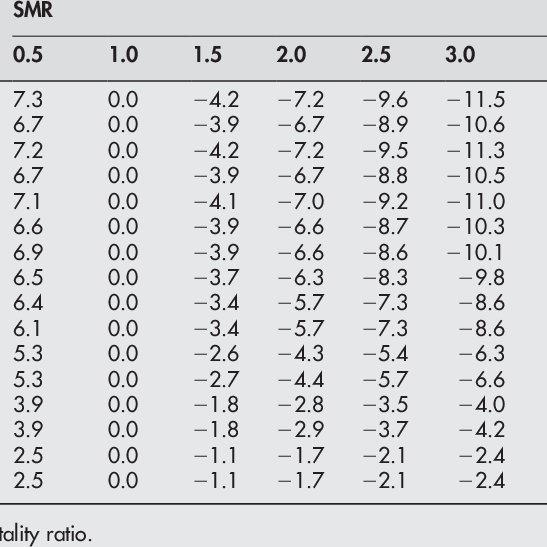
The estimated changes in LE compared with the general population for a range of possible SMR values, stratified by age and sex, using the Gompertz function and the 2003 UK mortality rates, are presented in table 2. Calculated LEs ) and AAD ) were compared between patients with PD and the UK general population. The graphical comparisons show that LE and AAD are considerably shorter or earlier in patients with age at onset before 50years compared with the general UK population. This difference decreases with increasing age in females and males. The mean LE of patients with PD with onset between 25 and 39years was 38 years, corresponding to an AAD of 71 years compared with an LE of 49 and AAD of 82 years in the general population. The mean LE of patients with PD with onset between 40 and 64years was 21 years, resulting in an AAD of 73 years compared with an LE of 31 and an AAD of 83 years in the general population. The mean LE for older individuals with PD was 5 years, resulting in an AAD of 88 years compared with an LE of 9 years and an AAD of 91 years in the general population. The SMR calculations were the same for both sexes, and therefore changes in LE were the same, but the actual LE and AAD estimates were higher in women because they live longer, on average, than males in the general population.
| Age |
|---|
Drug Testing For Diagnosis Of Parkinsons Disease
A diagnostic clue suggesting Parkinsons disease is provided by symptom improvement after the application of L-DOPA or apomorphine . The improvement should occur in 515 minutes after the injection of apomorphine.
The L-DOPA test is considered positive if a clinical improvement of approx. 20% is achieved. For a better assessment of clinical improvement, the Unified Parkinsons Disease Rating Scale is used.
Don’t Miss: Glutathione Injections For Parkinson’s
What Is The Treatment For Parkinson’s Disease
There is currently no treatment to cure Parkinson’s disease. Several therapies are available to delay the onset of motor symptoms and to ameliorate motor symptoms. All of these therapies are designed to increase the amount of dopamine in the brain either by replacing dopamine, mimicking dopamine, or prolonging the effect of dopamine by inhibiting its breakdown. Studies have shown that early therapy in the non-motor stage can delay the onset of motor symptoms, thereby extending quality of life.
The most effective therapy for Parkinson’s disease is levodopa , which is converted to dopamine in the brain. However, because long-term treatment with levodopa can lead to unpleasant side effects , its use is often delayed until motor impairment is more severe. Levodopa is frequently prescribed together with carbidopa , which prevents levodopa from being broken down before it reaches the brain. Co-treatment with carbidopa allows for a lower levodopa dose, thereby reducing side effects.
In earlier stages of Parkinson’s disease, substances that mimic the action of dopamine , and substances that reduce the breakdown of dopamine inhibitors) can be very efficacious in relieving motor symptoms. Unpleasant side effects of these preparations are quite common, including swelling caused by fluid accumulation in body tissues, drowsiness, constipation, dizziness, hallucinations, and nausea.
Early Onset/young Onset Parkinson’s
Parkinsons can occur at any age. Early onset Parkinson’s, also known as young onset Parkinsons , is defined as occurring in someone below the age of 40. Research suggests that genetics may play more of a role in early or young onset than in people who are diagnosed over the age of 40.
In early or young onset Parkinson’s, the symptoms you experience and how you respond to medication may differ slightly from older onset, although for some people these can be very similar.
Motor symptoms generally respond well to medication in both young and older onset Parkinsons. In early or young onset, motor fluctuations such as dyskinesia and wearing off tend to occur earlier but they generally progress more slowly. This is thought to be due to the most commonly prescribed medication, levodopa, and for this reason, young onset is usually treated initially with alternatives to levodopa such as MAO-B inhibitors or dopamine agonists. Levodopa is generally only added in when other medications do not provide adequate symptom control.
Dystonia is also a more common early motor symptom in early or young onset, whereas some of the non-motor symptoms that occur in older onset Parkinsons, such as memory problems, are less common.
Deep brain stimulation has also been shown to be effective at an earlier stage of Parkinsons if medication no longer controls motor symptoms so well, and you may want to discuss this option with your care team. See Deep brain stimulation.
Read Also: Home Exercise For Parkinson Disease
Do People Die From Parkinson’s
PD does not directly kill patients people with PD die from other causes, not from PD itself. Two major causes of death for those with PD are falls and pneumonia.
People with PD are at higher risk of falling, and serious falls that require surgery carry the risk of infection, adverse events with medication and anesthesia, heart failure, and blood clots from immobility.3
Pneumonia is a common cause of death, and those with PD are at risk for aspiration pneumonia.3 People with PD often have problems with swallowing, so the risk of aspirating food or drink, or having food or drink going down the wrong pipe is higher. In PD, the person may not be able to cough up the food or drink they aspirated, and it can remain in the lungs, eventually causing an infection.3 Even with general pneumonia, when coughing is weakened, as in PD, the mucus and other material that needs to be coughed up isnt able to be expelled, and this makes effective treatment of pneumonia more difficult in those with PD.
Parkinson’s Disease Diet And Nutrition
Maintaining Your Weight With Parkinson’s Disease
Malnutrition and weight maintenance is often an issue for people with Parkinson’s disease. Here are some tips to help you maintain a healthy weight.
- Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily.
- If you have an unexplained weight gain or loss , contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition.
- Avoid low-fat or low-calorie products. . Use whole milk, whole milk cheese, and yogurt.
Also Check: Is Massage Good For Parkinson’s
How Early Can Parkinsons Disease Be Treated
Every day, researchers around the world are working to find treatments and trying to slow down the progression and harmful effects of early-onset Parkinson’s and Parkinson’s disease. While no cure presently exists, there are certain medications that may reduce the symptoms and help a person to maintain their mobility.
The treatment approach to early-onset Parkinson’s has been to lay down medications until a person’s symptoms start to affect their daily life considerably.
Conversely, the Parkinson’s medication levodopa and its alternative, including Carbidopa-levodopa, are likely to cause increased symptoms in a younger person with Parkinson’s disease. Accordingly, healthcare professionals may recommend different medications, such as:
- MAO-B inhibitors, such as selegiline
- dopamine agonists, such as ropinirole
These drugs are associated with fewer side effects in young people as compared to levodopa.
About The Lecturio Medical Online Library
Our medical articles are the result of the hard work of our editorial board and our professional authors. Strict editorial standards and an effective quality management system help us to ensure the validity and high relevance of all content. Read more about the editorial team, authors, and our work processes.
Read Also: Idiopathic Parkinson’s Disease Life Expectancy
Lifespan Of Those With Parkinson’s
Many people think PD automatically means a shorter lifespan, but this isnt necessarily true. The area is under-researched, and the research that has been done has yielded variable results.
A study done at the Mayo Clinic found that overall, patients with PD had similar lifespans to those without PD, but if PD dementia or dementia with Lewy bodies were present, that did contribute to increased mortality rates.1 For those with typical PD without dementia, compared to the general population, they died approximately a year earlier.1,2 PD is not a direct killer like heart attack, and there are steps individuals can take to help maintain their functioning and health.
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Recommended Reading: Ultrasound Treatment For Parkinson’s Disease
What Is Parkinson’s Disease
Parkinson’s disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinson’s disease and the degree of impairment vary from person to person. Many people with Parkinson’s disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinson’s disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinson’s disease will increase in the future. Adult-onset Parkinson’s disease is most common, but early-onset Parkinson’s disease , and juvenile-onset Parkinson’s disease can occur.
Young Onset Parkinsons : An Introduction
Although the average age to develop Parkinsons is around 60, young onset Parkinsons occurs in 5-10% of people diagnosed. 20% are under the age of 50. Some challenges in Parkinsons are universal, regardless of age, but there are a number of issues specific to younger people.
Generally, Parkinsons proceeds more slowly in younger people. While no two people are the same, someone whose onset age is 40 can expect to work for another 15-20 years on average. For someone with an onset age of 60, the average figure would be half that. These figures are based on the kinds of treatment available today. Future treatment will be even more effective in prolonging the productive life of people with Parkinsons.
Larry Gifford hosts a panel discussion on Living Well with Young Onset Parkinsons in May of 2020.
The following characteristics tend to be present in young onset Parkinsons:
- Young onset Parkinsons is less likely to lead to dementia and balance problems
- It is more likely to include focal dystonia, which is cramping or abnormal posturing of one part of the body.
- Younger people are more sensitive to the benefits of Parkinson medications, but they tend to experience the dyskinetic side effects of levodopa sooner than older people.
- They also tend to experience dose-related fluctuations at an earlier stage of the disease, including wearing off* and the on-off effect. See Parkinson Canada Information Sheet, Parkinsons Medications: What you need to know!
Medication
Employment
Also Check: Deep Brain Stimulation For Parkinson’s Disease Success Rate
Eat Healthy Meals Throughout The Day
- Consuming a variety of foods from all five food groups provides consistent energy and keeps your immune system healthy. Focus on eating a minimum of five fruits and vegetables each day, eating a variety of high fiber foods, and staying hydrated, all of which help prevent constipation, which is often an issue for people diagnosed with YOPD.
- Watch this to learn how to use nutrition to help you live well with Parkinsons.
What Is Parkinsons Disease
Parkinsons disease is a progressive brain disorder that affects mobility and mental ability. If you or a loved one has been diagnosed with Parkinsons, you may be wondering about life expectancy.
According to some research, on average, people with Parkinsons can expect to live almost as long as those who dont have the condition.
Read Also: Do You Get Pain With Parkinson’s
Prognosis Of Parkinsons Disease
Of the three types of Parkinsons disease, the tremor-dominant type is associated with the best prognosis, showing the most therapeutic efficacy.
Successful therapy for Parkinsons disease results in life expectancy almost equivalent to that of the normal population. On average, care dependency sets in 20 years after the onset of the disease.
Burn, D. J. . Dementia in Parkinsons disease. Non-Motor Symptoms of Parkinsons Disease, 121-134. doi:10.1093/med/9780199237234.003.0010
Gaig, C., Santamaria, J., & Compta, Y. . Non-motor symptoms in the early motor stages of Parkinsons disease. Non-motor Symptoms of Parkinsons Disease, 24-43. doi:10.1093/med/9780199684243.003.0003
Meara, J., & Koller, W. C. . Parkinsons disease and parkinsonism in the elderly. Cambridge, U.K: Cambridge University Press.
Stephani, C. . Cognitive and Psychiatric Aspects of Parkinsons Disease. Symptoms of Parkinsons Disease. doi:10.5772/21171
Who Gets Early Onset Parkinsons Disease
About 10%-20% of those diagnosed with Parkinsons disease are under age 50, and about half of those are diagnosed before age 40. Approximately 60,000 new cases of Parkinsons are diagnosed each year in the United States, meaning somewhere around 6,000 12,000 are young onset patients.
Is it genetic or hereditary?
The cause of Parkinsons disease is not yet known. However, Parkinsons disease has appeared across several generations of some families, which could indicate that certain forms of the disease are hereditary or genetic. Many researchers think that Parkinsons disease may be caused by genetic factors combined with other external factors. The field of genetics is playing an ever greater role in Parkinsons disease research, and scientists are continually working towards determining the cause or causes of PD.
You May Like: Can Head Injury Cause Parkinson’s
Definition Of Parkinsons Disease
Parkinsons syndrome is characterized by the clinical triad of rigor, tremor, and akinesia as well as possible postural instability.
Based on etiology, one can further distinguish between idiopathic Parkinsons disease, which is synonymous with Parkinsons disease, and atypical and symptomatic parkinsonism.
Idiopathic Parkinsons disease or Parkinsons disease is considered a diagnosis of exclusion, in the absence of a specific cause.
Symptomatic Parkinsonism, however, is triggered by certain identifiable factors. For example, in the context of intoxication, manganese or lead may cause the disease. Parkinsons syndrome is also triggered by medication, e.g., neuroleptics.
Parkinsons syndrome occurring in the context of other neurodegenerative diseases is referred to as atypical Parkinsonism.
Parkinsons Disease Late Stages: What Will Happen To Me
With advanced Parkinsons disease, stage 5 life expectancy can be months or years depending on how your condition presents. You are likely to need round-the-clock care at this stage, and you may not be able to move around independently. Patients with late-stage Parkinsons disease are more susceptible to pneumonia, sepsis, pyelonephritis and decubitus ulcers. Late-stage Parkinsons also leads to Parkinsons disease dementia in 50% of cases. For all of these reasons, many late-stage Parkinsons patients are cared for by loved ones or in a hospice.
Don’t Miss: Caring For Someone With Parkinson’s
Identifying Risk Factors For Parkinson’s
The risk for early death increased by about 40% for every 10-year increase in age at diagnosis.
Parkinsonâs researcher Tobias Kurth, MD, agrees that identifying risk factors for early death could help clinicians better manage the disease.
Kurth is an adjunct associate professor of epidemiology at Harvard School of Public Health.
âThis is important research that adds to our understanding of the impact of specific features of Parkinsonâs disease on outcomes,â he tells WebMD.
His own study of Parkinsonâs-associated death matched Parkinsonâs patients with people without the disease who had similar non-Parkinsonâs-related illnesses.
Like the newly reported study, patients who were older when their Parkinsonâs disease was diagnosed had a greater risk for early death.