What Are The Primary Motor Symptoms Of Parkinsons Disease
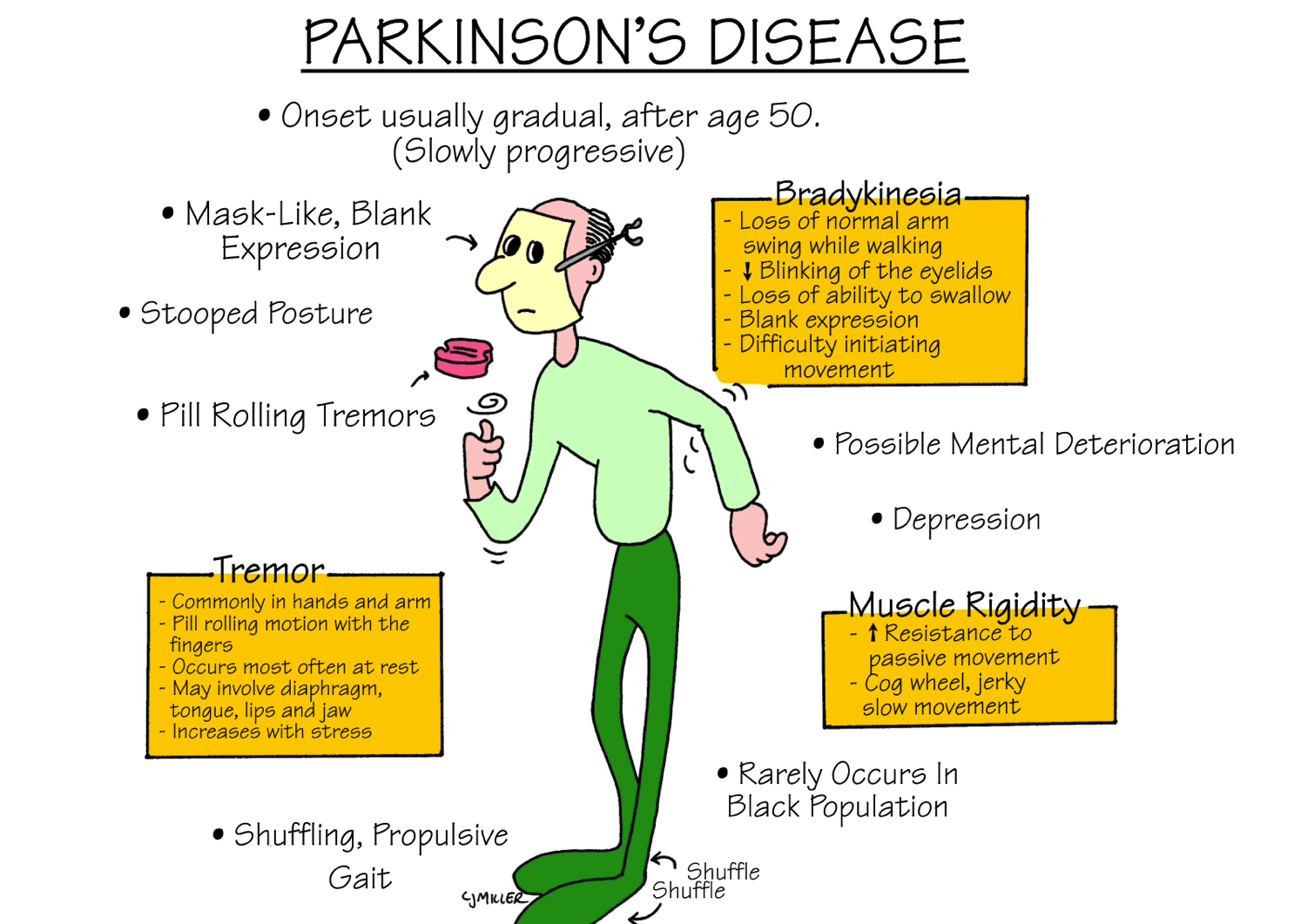
There are four primary motor symptoms of Parkinsons disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinsons.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinsons disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinsons disease has a tremor, nor is a tremor proof of Parkinsons. If you suspect Parkinsons, see a neurologist or movement disorders specialist.
Tremors
Rigidity
Bradykinesia
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
Why Is Expert Care Important
Early expert care can help reduce PD complications. Findings show that 60 percent of people with Parkinson’s fall short of getting the expert care they need. The National Parkinson Foundation has estimated that about 6,400 people with Parkinson’s die unnecessarily each year due to poor care.
Trained neurologists will help you recognize, treat and manage the disease. Common approaches include medication, surgical treatment, lifestyle modifications , physical therapy, support groups, occupational therapy and speech therapy. The best approach is interdisciplinary care, where you are seen by multiple specialists on a regular basis and all of the specialists talk and arrange the best possible coordinated care. This is what is referred to as a patient-centric approach to Parkinson’s care.
Further Testing In Parkinson’s
In other situations, where perhaps the diagnosis is not as clear, younger individuals are affected, or there are atypical symptoms such as tremor affecting both hands or perhaps no tremor at all, further testing may help. For example, imaging can play a role in differentiating between essential tremor and Parkinsons. It can also be important to confirm what is initially a clinical diagnosis of Parkinsons prior to an invasive treatment procedure such as surgical DBS
Recommended Reading: Diseases Similar To Parkinsons
Mri In Parkinson’s Testing
One of the more common tests done during a neurologic workup is an MRI scan and one may think that in the investigation of a disease that affects the brain such as Parkinsons, this imaging test would be a necessity. In the context of Parkinsons disease, however, an MRI is not particularly helpful. It looks at the structure of the brain which, for all intents and purposes, appears normal in this disease. An MRI may, however, be indicated when symptoms appear in younger people or if the clinical picture or the progression of symptoms is not typical for Parkinsons. In these situations, MRI can be used to rule out other disorders such as stroke, tumors, hydrocephalus , and Wilsons Disease .
Diagnosis Of Parkinsons Disease

A number of disorders can cause symptoms similar to those of Parkinson’s disease. People with Parkinson’s-like symptoms that result from other causes are sometimes said to have parkinsonism. While these disorders initially may be misdiagnosed as Parkinson’s, certain medical tests, as well as response to drug treatment, may help to distinguish them from Parkinson’s. Since many other diseases have similar features but require different treatments, it is important to make an exact diagnosis as soon as possible.
There are currently no blood or laboratory tests to diagnose nongenetic cases of Parkinson’s disease. Diagnosis is based on a person’s medical history and a neurological examination. Improvement after initiating medication is another important hallmark of Parkinson’s disease.
Read Also: Zhichan Capsule
What Can You Do If You Have Pd
- Work with your doctor to create a plan to stay healthy. This might include the following:
- A referral to a neurologist, a doctor who specializes in the brain
- Care from an occupational therapist, physical therapist or speech therapist
- Meeting with a medical social worker to talk about how Parkinson’s will affect your life
For more information, visit our Treatment page.
Page reviewed by Dr. Chauncey Spears, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
If Its Not Parkinsons Disease What Could It Be
Here are some possibilities:
Side effects of medication: Certain drugs used for mental illnesses like psychosis or major depression can bring on symptoms like the ones caused by Parkinsonâs disease. Anti-nausea drugs can, too, but they typically happen on both sides of your body at the same time. They usually go away a few weeks after you stop taking the medication.
Essential tremor: This is a common movement disorder that causes shaking, most often in your hands or arms. Itâs more noticeable when youâre using them, like when you eat or write. Tremors caused by Parkinsonâs disease usually happen when youâre not moving.
Progressive supranuclear palsy: People with this rare disease can have problems with balance, which may cause them to fall a lot. They donât tend to have tremors, but they do have blurry vision and issues with eye movement. These symptoms usually get worse faster than with Parkinson’s disease.
Normal pressure hydrocephalus : This happens when a certain kind of fluid builds up in your brain and causes pressure. People with NPH usually have trouble walking, a loss of bladder control, and dementia.
Recommended Reading: On-off Phenomenon
New Diagnostic Standards For Parkinsons
Until recently, the gold-standard checklist for diagnosis came from the U.K.s Parkinsons Disease Society Brain Bank. It was a checklist that doctors followed to determine if the symptoms they saw fit the disease. But thats now considered outdated. Recently, new criteria from the International Parkinson and Movement Disorder Society have come into use. This list reflects the most current understanding of the condition. It allows doctors to reach a more accurate diagnosis so patients can begin treatment at earlier stages.
How It All Fits Together
Diagnosing Parkinsons disease can be tricky. The process relies heavily on your doctors judgment. In addition, the causes and risk factors of Parkinsons are not entirely clear yet, which contributes to the difficulty in diagnosing this condition.
However, there have been efforts to try and detect this disease earlier. For instance, clinicians have started focusing more on prodromal symptoms, which are early symptoms that appear before movement-related difficulties begin.
These symptoms include:
- Loss of smell, which can sometimes occur years before other symptoms
- Chronic constipation, without any other explanation
- Rapid eye movement behavior disorder, which causes sleep disturbances
Read Also: Does Sam Waterston Have Parkinsons
What Is Parkinsons Disease
Parkinsons disease is a nervous system disease that affects your ability to control movement. The disease usually starts out slowly and worsens over time. If you have Parkinsons disease, you may shake, have muscle stiffness, and have trouble walking and maintaining your balance and coordination. As the disease worsens, you may have trouble talking, sleeping, have mental and memory problems, experience behavioral changes and have other symptoms.
Tremor In Other Conditions
While tremor is a common symptom of Parkinsons, it can also be a symptom of other conditions, most notably essential tremor. The main difference between Parkinsons tremor and most other types of tremor is that in Parkinsons resting tremor is most common. Other conditions are usually characterized by action tremor, which tends to lessen at rest and increase when youre doing something, like trying to make a phone call or take a drink.
Tremors of the head and voice are also common in essential tremor but rare in Parkinsons.
Recommended Reading: Yopd Life Expectancy
Is Parkinsons Disease Inherited
Scientists have discovered gene mutations that are associated with Parkinsons disease.
There is some belief that some cases of early-onset Parkinsons disease disease starting before age 50 may be inherited. Scientists identified a gene mutation in people with Parkinsons disease whose brains contain Lewy bodies, which are clumps of the protein alpha-synuclein. Scientists are trying to understand the function of this protein and its relationship to genetic mutations that are sometimes seen in Parkinsons disease and in people with a type of dementia called Lewy body dementia.
Several other gene mutations have been found to play a role in Parkinsons disease. Mutations in these genes cause abnormal cell functioning, which affects the nerve cells ability to release dopamine and causes nerve cell death. Researchers are still trying to discover what causes these genes to mutate in order to understand how gene mutations influence the development of Parkinsons disease.
Scientists think that about 10% to 15% of persons with Parkinsons disease may have a genetic mutation that predisposes them to development of the disease. There are also environmental factors involved that are not fully understood.
How Is Parkinsons Diagnosed
Doctors use your medical history and physical examination to diagnose Parkinson’s disease . No blood test, brain scan or other test can be used to make a definitive diagnosis of PD.
Researchers believe that in most people, Parkinson’s is caused by a combination of environmental and genetic factors. Certain environmental exposures, such as pesticides and head injury, are associated with an increased risk of PD. Still, most people have no clear exposure that doctors can point to as a straightforward cause. The same goes for genetics. Certain genetic mutations are linked to an increased risk of PD. But in the vast majority of people, Parkinsons is not directly related to a single genetic mutation. Learning more about the genetics of Parkinsons is one of our best chances to understand more about the disease and discover how to slow or stop its progression.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
Men are diagnosed with Parkinsons at a higher rate than women and whites more than other races. Researchers are studying these disparities to understand more about the disease and health care access and to improve inclusivity across care and research.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
The Michael J. Fox Foundation has made finding a test for Parkinsons disease one of our top priorities.
Also Check: Parkinson Silverware
Physical Examination And Tests
A trip to the neurologists office often includes what seems like dozens of questions, along with multiple tests.
There currently are no diagnostic blood tests for Parkinson’s disease, but your healthcare provider may do some routine blood and urine tests to assess your overall health. Your blood pressure will be taken sitting and standing to look for orthostatic hypotension.
A movement disorder specialist will do a variety of physical tests to assess you as well.
Stooping Or Hunching Over
Are you not standing up as straight as you used to? If you or your family or friends notice that you seem to be stooping, leaning or slouching when you stand, it could be a sign of Parkinson’s disease .
What is normal?If you have pain from an injury or if you are sick, it might cause you to stand crookedly. Also, a problem with your bones can make you hunch over.
Read Also: Similar To Parkinsons
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Who Is Affected By Tremor
About 70% of people with Parkinsons experience a tremor at some point in the disease. Tremor appears to be slightly less common in younger people with PD, though it is still one of the most troublesome symptoms. People with resting tremor usually have a more slowly progressing course of illness than people without tremor.
Don’t Miss: Parkinson Bicycle Cleveland Clinic
Tips For Daily Living
If you are already living with Parkinsons disease, here are some tips to manage it:
- Exercise your brain. Read, work on crossword puzzle, do Sudoku, or engage in other activities that use your brain.
- Get moving. If you feel comfortable walking, swimming, or riding an exercise bike, go for itand try to do it on a regular basis.
- Try tai chi. We think of as a mind-body exercise, and it is, but it also has roots as a martial art in China. A 2012 study found that practicing tai chi helped people with moderate Parkinsons disease maintain stability and balance. And a 2014 study found that tai chi can help people reduce their risk of falling. It incorporates a flowing series of coordinated movements to help you maintain flexibility, strength and balance, and it can be easily adapted to meet your abilities.
- Practice yoga. You dont have to perform headstands or other physically challenging poses to get significant benefits from . You can improve your balance, mobility, flexibility, and strength with a form thats adapted for you.
- Find a support group. Whether you prefer an online support group or a group that meets in person, a can be an invaluable resource for helping you live with Parkinsons disease.
Brain Imaging And Other Tools To Aid Diagnosis Of Parkinsons
In addition to taking a history and performing a detailed neurologic examination, physicians sometimes use brain imaging to help support a particular diagnosis. However, these studies have their limitations in the diagnosis of Parkinsons disease and are typically used only in select patients. Brain imaging is not routinely performed by neurologists or movement disorder specialists when they are considering a diagnosis, especially if the persons symptoms strongly suggest to the physician that idiopathic Parkinsons disease is the correct diagnosis.
Helping diagnose Parkinsons with DaTscan and other tests
Rather, use of imaging is most helpful when the diagnosis is uncertain, or when physicians are looking for changes in the brain that are more typical of one of several Parkinsonian syndromes and other conditions that can mimic Parkinsons. Imaging studies to evaluate Parkinsons disease and Parkinsonian syndromes include magnetic resonance imaging , which examines the structure of the brain, and DaTscan, an imaging test approved by the Food and Drug Administration to detect the dopamine function in the brain. A DaTscan may help differentiate idiopathic Parkinsons disease from certain other neurologic disorders. Most physicians offices will have access to MRI however, DaTscan imaging may only be available at larger hospitals or medical centers.
Recommended Reading: Prayers For Parkinson’s Disease
What Is And Isn’t Parkinson’s Disease
I am often asked if Parkinson’s Disease is a form of Alzheimers. Parkinson’s is not Alzheimers, ALS or a brain tumor, and the prognosis for Parkinson’s, though not a perfect scenario, leaves room to live a productive life.
PD is a progressive and chronic neurological disease that often begins with mild symptoms that advance gradually over time. Symptoms can be so subtle in the early stages that they go unnoticed, leaving the disease undiagnosed for years. For patients with Parkinson’s, there is a reduction in the body chemical dopamine, which controls movement and mood so simple activities like walking, talking and writing can be impacted.
Due to the complexity of PD, diagnosis is based on a variety of factors. The best diagnosis is made by an expert doing a careful history and exam followed by tracking responses to therapy. There is no blood or laboratory test to diagnose Parkinson’s disease.
While Parkinson’s reaches all demographics, the majority of people with PD are age 60 or older. Men and people with a family history of the disease have an increased risk.
The Diagnostic Criteria Used Today

In 2015, a Movement Disorder Society task force proposed a set of criteria that became known as the Movement Disorder Society United Parkinsons Disease Rating Scale , which includes non-motor symptoms in its criteria.9
The new criteria requires you to have slowness of movement, plus either a rest tremor or rigidity. It also requires that you do not meet any criteria in a list called absolute exclusion criteria. This list of symptoms indicates you most likely do not have PD or that you may have an atypical parkinsonism disorders that resemble Parkinsons disease but are ultimately different. If you meet any of those requirements, PD is ruled out. For example, one absolute exclusion criteria is if you are taking a drug that is known to cause Parkinsons-like side effects.
Next, you must meet at least two of the following four criteria:
- Dramatic improvement of motor symptoms when you take the gold-standard Parkinsons medication called levodopa
- The presence of dyskinesia as a result of taking levodopa dyskinesia is a possible side effect of levodopa among people with PD
- Rest tremor, meaning your tremor occurs when the body part is at rest
- Loss of smell, or if you have a test called MIBG scintigraphy and it indicates that you have autonomic dysfunction, which is when your autonomic nervous system doesnt work correctly, leading to issues with things like heart rate and blood pressure.
You May Like: Parkinson’s Bike Therapy