What Are On And Off Periods With Parkinsons Meds
While you might expect that taking a medication on a consistent schedule would guarantee your symptoms would be kept at bay, thats unfortunately not always the case with Parkinsons diseaseand thats the core of the on-off phenomenon, says Ling Pan, M.D., clinical assistant professor of neurology and neurosurgery at NYU Langone Health in New York, NY.
The on period is when the medication is doing its job to prevent tremors and other motor symptoms, explains Dr. Hui. Patients will often feel better fairly soon after taking their doseeven within half an hour, she says. Its almost like a light switch is being switched on, and they can move a lot easier.
That said, Dr. Hui explains, the effect can wear off over several hoursand thats when you hit that off period. When you first start taking the drug, though, its normal to experience a honeymoon period, she says. It may work all day, and you feel great, but overtime as the disease progresses, the medication doesnt less as long, and off-time creeps in slowly and then becomes more noticeable and more regular overtime. Typically, thats when folks with Parkinsons start to cycle between those on and off periods.
A Linearized Discrete Version
If, on the other hand, infectiousness were an onoff phenomenon such that individuals are either infectious, possibly at levels depending on their h-type, or not and if we again assume discrete h-states, we could express the change in the numbers infected as
is the number of infectious subjects of h-type at time t and a , n are transmission coefficients that also incorporate the numbers of susceptible. In the linearized situation, these numbers do not change .
Question 7.i
Obviously, Eqs. and look very different. Are they really different, though, in other ways than in their assumption regarding infectiousness over time allows for changing infectiousness while assumes constant infectiousness) and the discrete h-states in ? Is there anything funny about this equation that appears strange to you, especially if you recall the chapter on Kermack & McKendrick’s famous paper?
Paul Bentley, Pankaj Sharma, in, 2012
Characteristics Of The Patients
A total of 1,504 PD patients were enrolled into the survey. Of them, 119 patients were excluded from the statistical analysis due to incomplete medication information or incorrect CWOQ-9 filling . A total of 1,385 patients were finally included into the statistical analysis. 53.2% of the whole population were males, the mean age was 69.7 ± 9.5 years, the mean diagnosis duration was 5.8 ± 4.7 years, and the median H& Y staging was 2.0 ± 1.0. Most of the patients were treated with levodopa. The characteristics of the PD patients are shown in detail in Tables 1, 2.
Table 1. Baseline characteristics of the study population.
Table 2. Medication of the study population.
Recommended Reading: Ultrasound Treatment For Parkinson’s Disease
Will New Treatments Really Help
According to multiple clinical studies, treatment with Inbrija led to significant improvement in motor function, with an onset of 10 minutes. A review of 900 patients showed a reduction in the Unified Parkinson’s Disease Rating Scale, 30 minutes post-dose, after 12 weeks of treatment. Overall, 75% of patients who took Inbrija experienced a decline of daily OFF times.
According to Robert A. Hauser, MD, professor of neurology and director of the Parkinsons Disease and Movement Disorders Center at the University of South Florida:
Inbrija helps address a significant unmet need for people with Parkinsons, and we look forward to adding this new treatment option to our armamentarium.
Presynaptic Mechanisms In Wearing
The finding that motor improvement following acute intravenous levodopa challenge lasts longer in de novo and stable patients than in those who are already suffering motor fluctuations was key to the development of the storage hypothesis, which implies that loss of presynaptic dopaminergic terminals reduces the capacity of the striatum to store dopamine and buffer the oscillations in plasma levodopa levels . Certainly, the pharmacokinetics of levodopa-dopamine in the brain is drastically changed after dopaminergic denervation of the striatum. In the rat with a 6-hydroxydopamine lesion of the nigrostriatal pathway, peak striatal dopamine levels and the area under the curve for synaptic dopamine availability are significantly lower in animals with larger lesions , which correlates with a shorter duration motor response . In patients, the availability of dopamine in the synapse has been measured by PET using the D-2 receptor antagonist raclopride as the radioligand. Raclopride was administered before and after levodopa intake in patients with and without motor fluctuations, with the result that patients with motor fluctuations demonstrated a greater decrease in raclopride binding than stable patients. Because raclopride competes with dopamine for binding to D2 receptors, reduced raclopride uptake is an index of higher synaptic dopamine levels and, therefore, reduced numbers of dopaminergic terminals .
Also Check: What Kills A Person With Parkinson’s Disease
How The Parkinson’s On
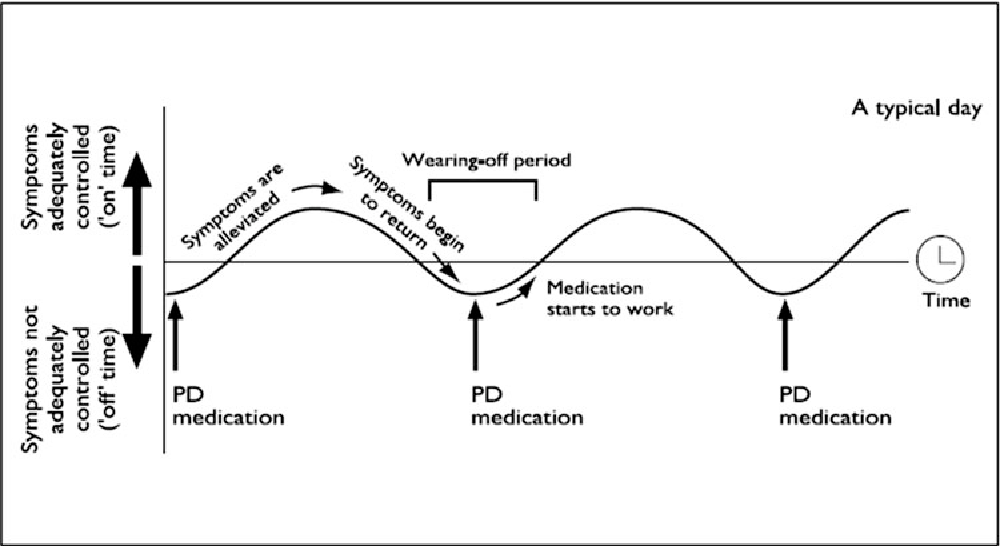
Ideally, when you take doses of a medication like levodopa on a regular schedule, you shouldn’t notice much of a difference in your symptoms between doses. In other words, your symptoms should remain relatively constant over time, regardless of when you last took your medication.
However, when the on-off phenomenon starts in Parkinson’s disease, you’ll feel better as a new dose of your medication starts to take effect, and worse before you’re due for another dose. Eventually, the duration of on states becomes shorter and the wearing off happens sooner .
Some experts have described the “on” period as akin to switching on a light, and the “off” period as the lights going off.
In an “on” state, the person with Parkinson’s disease may feel energetic and able to move around more easily. However, in an “off” state, the person may become very stiff, slow, and may even be unable to move at all for a few minutes. A person may also have difficulty speaking, and you may notice him or her slurring their words. As you can imagine, the “off” state can be quite uncomfortable.
Managing Wearing Off And Motor Fluctuations
If you think you are starting to experience wearing off or motor fluctuations, you should discuss this with your doctor promptly so that your medication can be adjusted to minimise your symptoms. Tell him or her how long your medication is lasting and what happens when it wears off. Remember to tell them about motor and non-motor symptoms.
Read Also: Interventions For Parkinson’s Disease
Can The Parkinsons Disease Kill A Patient
Parkinsons disease is not really fatal in nature. However, the symptoms associated with Parkinsons disease is actually life threatening that may lead to fatal accidents. Injuries are quite common in Parkinsons disease due to inability to move around effortlessly. This is actually dangerous. Thus, efforts must be taken in order to create a safe environment for patients with Parkinsons disease.
Clinician Assessments Of Wo
Clinicians identified WO in 763 patients, with the overall prevalence of WO being 55.1%. Most of the patients with WO were treated with levodopa, whereas 37 patients received dopamine agonists or non-dopaminergic medications. Further analysis showed that the WO frequency varied among different disease durations. WO was identified in 12.9% of patients within 1 year of disease duration. The percentage of patients with WO continuously increased with the disease progression. It reached the highest value of 76.2% in patients with 1015 years of disease duration. Then, it gradually dropped to 67.9% in patients with over 20 years of duration .
In terms of WO evaluation, the most frequently used question was symptom response to medications, with a frequency of 100%. It was followed by the fluctuating features of motor symptoms , timing of symptom response to medications , symptom fluctuation occurring at a fixed time per day, which lasts for days , and fluctuating features of non-motor symptoms . In addition, 56.9% of the clinicians considered that the presence of motor fluctuation was required for WO diagnosis.
You May Like: Are There Service Dogs For Parkinson’s Patients
Role Of The Ldr In The Development Of Motor Fluctuations
Fig. 1
Mean peak and baseline tapping speeds to the levodopa infusion on day 1 and day 4 and over 4 years of therapy with levodopa . The difference between peak and baseline tapping speeds is the magnitude of the SDR, which progressively increases to the levodopa infusion on day 4. Reproduced from Nutt et al. .
Similar results were reported by Zappia et al. who found that the duration of the SDR did not significantly change within the first year of therapy, but that 24% of patients lost the LDR to levodopa. These studies demonstrate the pivotal roles of the LDR and the magnitude rather than duration of the SDR in the development of motor fluctuations in the early years of levodopa therapy. They further suggest that when a sustained LDR is present, the SDR is usually masked and patients may therefore be classified clinically as stable responders to levodopa therapy even though they are experiencing fluctuations. As the LDR is progressively lost, patients lose the smooth drug effect and the magnitude of the SDR increases . Patients are then clinically observed to become fluctuators because the degree of benefit is now dependent on the magnitude of the SDR. Overall, the available evidence suggests that in the earlier stages of PD, where the difference between the ON and OFF states is less pronounced, any fluctuations in levodopa response are not noticed by the patient and therefore not reported.
Fig. 2
How Does The On
In the on state, the patient with Parkinsons disease may be able to move around easily and feel energetic. On the contrary, in the off phase the patient may become very stiff and slow. He may not be able to move at all or may have difficulty in moving for several minutes. The off phase occurs when the effect of the medicine wears out.
Recommended Reading: 5 Signs You Ll Get Parkinson’s
The Challenge Of On And Off Periods
On and off periods with Parkinsons medications can pose a significantand frustratingchallenge when it comes to managing your symptoms, says Dr. Pan.
On/off periods are a very relevant topic because it actually can cause a lot of disability in Parkinsons, she says. Because when patients are on medications, they can almost feel like normal and do a lot of things, and once medications wear off, they are very disabled and immobilized at times.
To address the issue, your doctor may have you start taking your medication dose more frequentlyfor example, switching from taking a pill every four hours to every three. However, it becomes a logistical challenge of taking medications so often, and there are also risks of excessive dopamine, she says. For example, non-motor symptoms of Parkinsonssuch as psychosisbecome more likely the higher the dose of a dopamine agent you are taking. It becomes a difficult balance of trying to reduce motor symptoms with your medications without taking so much that youre increasing other non-motor symptoms.
Thankfully, scientists have already worked to address this issue by developing new types of medications to help you manage those off-times, says Dr. Hui.
For example, one is a sublingual apomorphine, which is a drug placed under the tongue and can kick you on within 15 minutes. Theres also an inhaler form that works within 15-30 minutes, she says. These different delivery systems can help you maximize on-time quickly.
New Therapies For The Acute Treatment Of Off Episodes In Parkinsons Disease
Fabrizio StocchiDepartment of Neurology, IRCCS San Raffaele Pisana, Rome, Italy
The symptoms of OFF episodes can be caused by various factors including abnormal lingual control of swallowing and lingual festination. Patients with PD can also have a delayed swallowing reflex, which increases the risk of swallowing during inspiration, causing aspiration. Patients can also have a repetitive and involuntary reflux from the vallecula and piriform sinuses into the oral cavity.51 More importantly, many patients with PD have gastroparesis, which appears as postprandial bloating, early satiety, nausea, and vomiting.52,53 Delays in gastric emptying can cause slow delivery of levodopa to intestinal absorption sites, which, in turn, delays peaks in plasma levels leading to erratic drug responses, slow onset of action or dose failure.53â55 These issues were emphasized by gastroscopic examination of a patient, which found an intact levodopa/carbidopa tablet in the stomach 1.5 hours after it was swallowed.56 Furthermore, daytime gastroscopy has found food from the previous evening remaining in the stomachs of many patients with PD.
These developments in rescue therapies have the potential to substantially improve quality of life and help patients deal with the otherwise untreatable symptoms of OFF episodes, which are a serious burden and involve both motor and non-motor symptoms.
Recommended Reading: Is Drooling A Sign Of Parkinson’s Disease
Postsynaptic Mechanisms In Wearing
To evaluate the relevance of postsynaptic mechanisms, it is necessary to break down the wearing-off into its LDR and SDR components. Strong support for the involvement of postsynaptic mechanisms comes from the slow decay of the LDR on withdrawing dopamine agonist treatment in patients with de novo PD. For example, the time taken for motor symptoms to deteriorate back to baseline after stopping treatment with ropinirole was 6.2 ± 1.7 days and 9.0 ± 1.9 days with the short-acting agonist lisuride . Interestingly, similar studies in de novo PD patients with the very long-acting dopamine agonist cabergoline showed a shorter LDR compared to short-acting lisuride. From these results, it can be concluded that dopamine agonists have LDR effects that are similar to levodopa and that postsynaptic effects must contribute. We suggest that these postsynaptic changes include complex alterations in genes and protein at the striatal level mediating receptor and intracellular activity and also functional abnormalities in basal ganglia output pathways .
How To Manage Parkinsons Disease After It Is Diagnosed
Along with the medication so prescribed by the doctor, it is extremely important to bring some form of lifestyle changes in order to manage Parkinsons disease. They include-
Activity: As mentioned earlier Parkinsons disease affects the patients motor abilities, it is thus important to keep the body fit by indulging into exercise regularly. The patient may do any form of exercise which he may like every day to keep the body moving. This does not let the body parts to be stiff and also slows down the progression of the disease.
Additional Help: The caregivers and well-wishers should make attempts to make the environment safe for the patient with Parkinsons disease. Modifying the environment like installing grab bars in washroom and removing obstacles which may hamper movement of the patient is important.
Diet: Having nutritious food is important for patients with Parkinsons disease. It is seen to be beneficial to have right amount of nutrients in order to manage the symptoms of Parkinsons disease. The patient should also discuss with the doctor the food to avoid so that they do not interfere with the working of the medicines, especially levodopa.
Read Also: Does Sam Waterston Have Parkinson
Dopamine Depletion The Basal Ganglia And Motor Fluctuations
The overall determinant of the motor features in PD is the physiological state of basal ganglia output activity. Dopamine depletion can be very severe but motor features of PD can be controlled or prevented if subthalamic nucleus and globus pallidus pars interna neuronal firing stays within normal levels. Accordingly, therapeutic interventions aimed at reducing the abnormal and excessive activity of basal ganglia output neurons in PD should improve the SDR to levodopa. This is precisely what has been found in the 6-OHDA rat model where lesions of the STN ameliorated wearing-off and, more importantly, are a characteristic effect of functional neurosurgery for PD. Thus, modulation of basal ganglia output activity, without changing striatal dopamine availability, modifies the SDR. This has led to the suggestion that alterations of compensatory mechanisms involved in maintaining basal ganglia homeostasis in PD are compromised by the deleterious effects of pulsatile dopaminergic stimulation caused by the use of short-acting drug treatments .
What Are Off Episodes
Firstly, its important to understand what OFF episodes are and why they happen. OFF episodes are defined as a temporary returning of Parkinsonian symptoms such as tremor, rigidity, loss of postural reflexes and memory problems, while taking levodopa medication. OFF episodes affect the majority of people with PD, and it can occur at any stage of the illness.
Some patients experience OFF episodes when they first wake in the morning known as akinesia while others notice symptoms returning at the end of a dose when the drug starts to wear off. For some, the OFF episodes are random and severe. Uncontrolled Parkinson’s symptoms can significantly impact your quality of life, which is why scientists are committed to finding new and improved treatment options.
Also Check: Parkinson’s Staring Into Space
Clinical Relevance Of Early Recognition Of Wearing
In clinical practice, treatment is initiated once the compensatory mechanisms operative in early stages of the loss of the nigrostriatal pathway have failed. As a result, there is already a reduced capacity at the presynaptic dopamine terminal level to compensate for changes in dopamine availability associated with fluctuations in plasma and brain levodopa levels after oral administration. Therefore, the output of basal ganglia motor oscillates precariously between various abnormal states. The critical and therapeutically relevant point is that standard short-acting levodopa formulations lead to levels of striatal dopamine and dopamine receptor stimulation different from those prevailing under normal conditions and oscillating between subphysiological and supraphysiological levels. This being a reflection of the peaks and troughs associated with changes in plasma levodopa concentrations that characterize the use of standard levodopa preparations. Thus, standard levodopa administration does not restore the normal physiology of the basal ganglia , but induces, through pulsatile stimulation, molecular abnormalities such as phosphorylation of NMDA subunits and upregulation of AMPA receptors in medium spiny striatal neurons that underlie wearing-off .
Can An Off Episode Be Prevented
Eventually, most people with PD develop OFF episodes. Some people develop OFF episodes sooner than others.
Researchers have found evidence that taking high doses of levodopa may increase your risk of OFF episodes. It may cause greater fluctuations in your dopamine levels.
Its important for your doctor to prescribe the lowest dose of levodopa necessary to manage your symptoms. This may help limit fluctuations in dopamine and reduce your risk of OFF episodes.
If you think you might be experiencing OFF episodes, let your doctor know. They may adjust your prescribed dose or formulation of levodopa/carbidopa. They may also prescribe other treatments to manage OFF episodes.
If youre experiencing OFF episodes, your doctor may recommend one or more changes to your treatment plan.
They may:
In some cases, your doctor may recommend deep brain stimulation . In this procedure, a surgeon implants electrodes in the brain and a small internal pulse generator in the chest or abdomen. The internal pulse generator sends electrical signals to the brain to help control symptoms of DB.
Each treatment option carries a different risk of side effects. Ask your doctor about the potential benefits and risks of different treatment approaches.
Read Also: Prayers For Parkinson’s Disease