Progression Of Modified Columbia Score
Logistic regression was performed for patients not on anticholinergic drugs at baseline to discover which baseline variables predicted an increase in Columbia score by 20 or more points in 10 years. Univariate analysis showed that increasing tremor score , female sex , and increasing age were predictive. Multivariate analysis showed that only older age predicted deterioration by 20 or more points in the Columbia score ). Randomisation to bromocriptine or continued use of bromocriptine for more than 1 year did not influence deterioration in Columbia score by 10 or 20 points.
Gait Progression Over 6 Years In Parkinsons Disease: Effects Of Age Medication And Pathology
- 1Translational and Clinical Research Institute, Faculty of Medical Sciences, Newcastle University, Newcastle upon Tyne, United Kingdom
- 2The Newcastle upon Tyne NHS Foundation Trust, Newcastle upon Tyne, United Kingdom
- 3Auckland University of Technology, Auckland, New Zealand
- 4Department of Sport, Exercise and Rehabilitation, Northumbria University, Newcastle upon Tyne, United Kingdom
- 5Faculty of Medical Sciences, Newcastle University, Newcastle upon Tyne, United Kingdom
- 6School of Biomedical, Nutritional and Sport Sciences, Newcastle University, Newcastle upon Tyne, United Kingdom
Background: Gait disturbance is an early, cardinal feature of Parkinsons disease associated with falls and reduced physical activity. Progression of gait impairment in Parkinsons disease is not well characterized and a better understanding is imperative to mitigate impairment. Subtle gait impairments progress in early disease despite optimal dopaminergic medication. Evaluating gait disturbances over longer periods, accounting for typical aging and dopaminergic medication changes, will enable a better understanding of gait changes and inform targeted therapies for early disease. This study aimed to describe gait progression over the first 6 years of PD by delineating changes associated with aging, medication, and pathology.
When Should I See My Healthcare Provider Or When Should I Seek Care
You should see your healthcare provider as recommended, or if you notice changes in your symptoms or the effectiveness of your medication. Adjustments to medications and dosages can make a huge difference in how Parkinsons affects your life.
When should I go to ER?
Your healthcare provider can give you guidance and information on signs or symptoms that mean you should go to the hospital or seek medical care. In general, you should seek care if you fall, especially when you lose consciousness or might have an injury to your head, neck, chest, back or abdomen.
Don’t Miss: Ways To Prevent Parkinson’s
How Long Can A Person Live With Stage 5 Parkinson
When patients reach stage five the final stage of Parkinsons disease they will have severe posture issues in their back, neck, and hips. In endstage of Parkinsons disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
One may also ask, what do Parkinsons patients usually die from? But the most common cause of death in those with Parkinsons is pneumonia, because the disease impairs patients ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
what happens in stage 5 Parkinsons?
Stage Five of Parkinsons Disease Stage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
How quickly can Parkinsons progress?
While symptoms and disease progression are unique to each person, knowing the typical stages of Parkinsons can help you cope with changes as they occur. Some people experience the changes over 20 years or more. Others find the disease progresses more quickly.
How Is Parkinson Disease Treated

Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
You May Like: Sole Support For Parkinson’s
Associations Between Gait Changes And Change In Levodopa Dose Over Time
LEDD increased by 106 mg/day each year. Ninety-three percent of people with PD had increased LEDD compared to baseline assessment . Only one gait characteristic was related to LEDD change larger increases in step width variability related to greater increases in LEDD over time . Inclusion of the LEDD × Time interaction resulted in no significant change in step width variability , indicating that step width variability change is at least partially explained by a change in LEDD. All other gait characteristics meeting criteria 1 and 3 did not show associations between gait change and LEDD change and therefore exhibited disease-specific change that was not related to levodopa adjustments .
What Are The Symptoms Of Parkinson Disease
Parkinson disease symptoms usually start out mild, and then progressively get much worse. The first signs are often so subtle that many people don’t seek medical attention at first. These are common symptoms of Parkinson disease:
- Tremors that affect the face and jaw, legs, arms, and hands
- Slow, stiff walking
Read Also: Who Diagnoses Parkinson’s Disease
How Long Does It Take For Parkinsons Disease To Progress
See some of the possible complications of this disease and learn how to handle them. Parkinsons can come with other complications that may surprise you, including psychosis Discover the symptoms, causes, and treatments of Parkinsons disease right now. Here, learn about the symptoms and stages of this conditio For many people, the condition can take years to progress to a point where it has a real impact on daily life. The symptoms most often associated with Parkinsons are tremor, rigidity , and slowness of movement. Not everyone with Parkinsons experiences the same combination of symptoms they vary from person to person Coming to the moderate stage, which is usually between 3 and 7 years, one will notice significant changes. For instance, one can find trouble in buttoning a shirt. Furthermore, one will also see that the effect of the medicine begins to reduce between doses
You May Like: Primidone For Parkinsons Disease
What Are The Later Secondary Signs And Symptoms Of Parkinson’s Disease
While the main symptoms of Parkinson’s disease are movement-related, progressive loss of muscle control and continued damage to the brain can lead to secondary symptoms. These secondary symptoms vary in severity, and not everyone with Parkinson’s will experience all of them, and may include:
Also Check: Singing And Parkinson’s Disease
Mayo Clinic Q And A: Rate Of Progression Of Parkinsons Disease Hard To Predict
DEAR MAYO CLINIC: My father is 64 and was diagnosed with Parkinsons last year. So far his symptoms are very mild, but Im wondering what the typical progression of the disease is like. I have read that deep brain stimulation is sometimes recommended. When is this type of treatment usually considered? Is it safe?
ANSWER: The symptoms of Parkinsons disease, or PD, tend to begin very gradually and then become progressively more severe. The rate of progression is hard to predict and is different from one person to another. Treatment for PD includes a variety of options, such as exercise, medication and surgery. Deep brain stimulation is one surgical possibility for treating PD, but its usually only considered in advanced cases when other treatments dont effectively control symptoms.
Parkinsons disease is a syndrome which typically has no known cause. The diagnosis is based on symptoms. Neurologists who specialize in movement disorders typically have the most experience with PD diagnosis and treatment. There are many symptoms of parkinsonism. The most common include excessive slowness and lack of movement, as well as shaking or tremor.
As in your fathers situation, symptoms are often mild at the outset. How quickly they get worse varies substantially, perhaps because there may be multiple underlying causes of the disease. In most cases, symptoms change slowly, with substantive progression taking place over the space of many months or years.
What Are The Five Stages Of Parkinson’s Disease
Researchers may disagree on the number of stages of Parkinsons disease . However, they all agree the disease is a progressive disease with symptoms that usually occur in one stage and may overlap or occur in another stage. The stage increase in number value for all stage naming systems reflects the increasing severity of the disease. The five stages used by the Parkinsons Foundation are:
- Stage 1: mild symptoms do not interfere with daily activities and occur on one side of the body.
- Stage 2: Symptoms worsen with walking problems and both sides of the body are affected.
- Stage 3: Main symptoms worsen with loss of balance and slowness of movement.
- Stage 4: Severity of symptoms require help usually a person cannot live alone.
- Stage 5:Caregiver needed for all activities a patient may not be able to stand or walk and maybe bedridden and may also experience hallucinations and delusions.
A neurologist who specializes in movement disorders will be able to make the most accurate diagnosis. An initial assessment is made based on medical history, a neurological exam, and the symptoms present. For the medical history, it is important to know whether other family members have Parkinson’s disease, what types of medication have been or are being taken, and whether there was exposure to toxins or repeated head trauma previously. A neurological exam may include an evaluation of coordination, walking, and fine motor tasks involving the hands.
You May Like: Boyd Gaines Parkinson’s Disease
What Can I Expect If I Have This Condition
Parkinsons disease is a degenerative condition, meaning the effects on your brain get worse over time. However, this condition usually takes time to get worse. Most people have a normal life span with this condition.
You’ll need little to no help in the earlier stages and can keep living independently. As the effects worsen, youll need medication to limit how the symptoms affect you. Most medications, especially levodopa, are moderately or even very effective once your provider finds the minimum dose you need to treat your symptoms.
Most of the effects and symptoms are manageable with treatment, but the treatments become less effective and more complicated over time. Living independently will also become more and more difficult as the disease worsens.
How long does Parkinsons disease last?
Parkinsons disease isnt curable, which means its a permanent, life-long condition.
Whats the outlook for Parkinsons disease?
Parkinson’s disease isn’t fatal, but the symptoms and effects are often contributing factors to death. The average life expectancy for Parkinson’s disease in 1967 was a little under 10 years. Since then, the average life expectancy has increased by about 55%, rising to more than 14.5 years. That, combined with the fact that Parkinson’s diagnosis is much more likely after age 60, means this condition doesn’t often affect your life expectancy by more than a few years .
The Hoehn And Yahr Scale: Uses And Setbacks
To quantify disease progression, there is a commonly referenced staging scale. However, the staging of Parkinsons disease does have significant drawbacks. The Hoehn and Yahr scale was developed by Drs. Margaret Hoehn and Melvin Yahr in 1967:
- Stage I: Symptoms involve one side of the body
- Stage 2: Symptoms involve both sides of the body, or the midline
- Stage 3: Symptoms involve both sides of the body, with impairment of balance
- Stage 4: Symptoms have advanced to the point that although the person can stand and walk without the help of another person, he/she has significant disability. People in this stage typically need at least some help to perform their activities of daily living, or self-care activities such as eating, bathing, dressing, and toileting.
- Stage 5: The person cannot stand or walk without the help of another person
Hoehn and Yahr Scale Doesnt Factor in Progression of Non-motor Symptoms
The Hoehn and Yahr scale focuses solely on the progression of motor symptoms and does not consider the psychiatric, cognitive, and autonomic non-motor symptoms that often cause more disability than motor symptoms as PD advances. This is a major limitation of the Hoehn and Yahr scale.
Read Also: What Is The Difference Between Tremors And Parkinson’s Disease
Parkinsons Disease Is A Progressive Disorder
Parkinsons Disease is a slowly progressive neurodegenerative disorder that primarily affects movement and, in some cases, cognition. Individuals with PD may have a slightly shorter life span compared to healthy individuals of the same age group. According to the Michael J. Fox Foundation for Parkinsons Research, patients usually begin developing Parkinsons symptoms around age 60. Many people with PD live between 10 and 20 years after being diagnosed. However, a patients age and general health status factor into the accuracy of this estimate.
While there is no cure for Parkinsons disease, many patients are only mildly affected and need no treatment for several years after their initial diagnosis. However, PD is both chronic, meaning it persists over a long period of time, and progressive, meaning its symptoms grow worse over time. This progression occurs more quickly in some people than in others.
Pharmaceutical and surgical interventions can help manage some of the symptoms, like bradykinesia , rigidity or tremor , but not much can be done to slow the overall progression of the disease. Over time, shaking, which affects most PD patients, may begin to interfere with daily activities and ones quality of life.
Recommended Reading: Deep Brain Stimulation For Parkinsons Disease Before And After
How Is It Diagnosed
Diagnosing Parkinson’s disease is mostly a clinical process, meaning it relies heavily on a healthcare provider examining your symptoms, asking you questions and reviewing your medical history. Some diagnostic and lab tests are possible, but these are usually needed to rule out other conditions or certain causes. However, most lab tests aren’t necessary unless you don’t respond to treatment for Parkinson’s disease, which can indicate you have another condition.
You May Like: Gaba Supplement For Parkinson’s
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
Stages And Progression Of Lewy Body Dementia
Claudia Chaves, MD, is board-certified in cerebrovascular disease and neurology with a subspecialty certification in vascular neurology.
If you or someone you know has recently been diagnosed with Lewy body dementia, you might be wondering what to expect as the disease progresses. Is there a fairly typical progression like Alzheimers disease where it begins in early stages that are fairly uniform, then moves to middle stages and then to late stages? In Lewy body dementia, the answer is a bit more complicated.
You May Like: What Are The Environmental Causes Of Parkinson Disease
You May Like: Parkinson’s Disease Off Time
The Contribution Of Aging To Pd Gait Progression
Understanding how gait changes with normal aging is important as age-related changes cumulatively contribute to gait progression in people with PD alongside disease progression. Three characteristics changed in both PD and control cohorts over 6 years the change was therefore considered to be due primarily to aging mechanisms rather than disease progression. These changes met criteria 2.
Age-related change contributes to gait impairments observed in PD, suggesting that therapies addressing features of aging may be effective in reducing the burden of PD. It is important, therefore, to consider the mechanisms driving age-related gait change. Change may be due to atrophy and loss of muscle strength , physical inactivity , and development of age-related conditions, such as osteoarthritis causing increased pain and stiffness during movement . Age-related changes in the brain such as atrophy and white matter abnormalities also explain the slowing and increased variability of gait during aging . Increasing evidence implies that specific neural regions or networks underpin discrete gait characteristics , which could be specifically targeted to prevent discrete components of age-related gait decline. On this point, gait performance in PD is improved by exercise-based interventions aiming to increase muscle strength and activity speculatively these therapies may, at least partially, be targeting age-related changes which in turn positively impact PD gait.
Is Parkinsons Disease Fatal
Parkinsons disease itself doesnt cause death. However, symptoms related to Parkinsons can be fatal. For example, injuries that occur because of a fall or problems associated with dementia can be fatal.
Some people with Parkinsons experience difficulty swallowing. This can lead to aspiration pneumonia. This condition is caused when foods, or other foreign objects, are inhaled into the lungs.
You May Like: Fatigue In Parkinson’s Disease
Parkinsons Disease Symptoms Of Dementia
Up to one-third of people living with Parkinson’s disease experience dementia, according to the Parkinson’s Disease Foundation. Problems with dementia may include trouble with memory, attention span, and what is called executive function the process of making decisions, organizing, managing time, and setting priorities.
RELATED: 12 Famous People With Parkinson’s Disease
What Are The Primary Motor Symptoms Of Parkinsons Disease
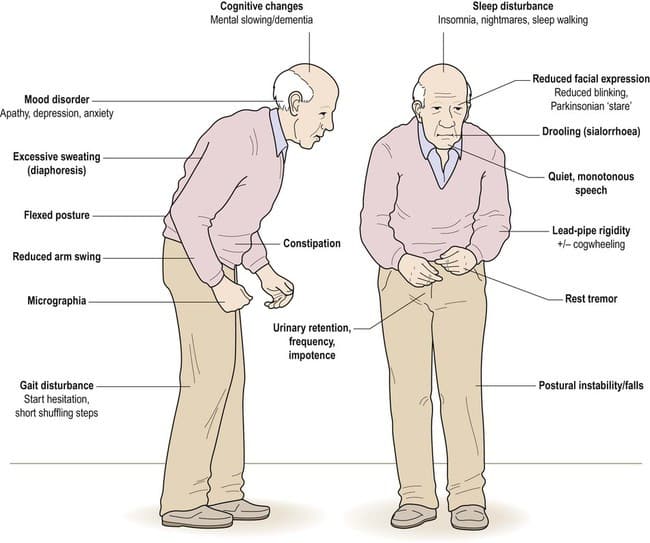
There are four primary motor symptoms of Parkinsons disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinsons.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinsons disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinsons disease has a tremor, nor is a tremor proof of Parkinsons. If you suspect Parkinsons, see a neurologist or movement disorders specialist.
Tremors
Vocal Symptoms
Recommended Reading: Wolff Parkinson White Syndrome Ecg