Associated Factors As Predictor Of Death
The present study shows that low MMSE score at baseline was related to an increased risk of death among PD patients . The results are in accordance with the previous observations, which indicated that PD patients with cognitive impairment have a particularly high risk of mortalityReference Auyeung, Tsoi and Mok3,Reference Posada, Benito-Leon and Louis7,Reference Hughes, Ross, Mindham and Spokes9 and cognitive impairment is an independent predictor of decreased survival in PD.Reference de Lau, Verbaan, Marinus and van Hilten24,Reference Xu, Gong, Man and Fan25 It is well-known that cognitive impairment, especially Parkinsons disease dementia , occurs in 24% to 31% of PD patients,Reference Aarsland, Zaccai and Brayne26 and both reduced cholinergic activity in the cortex and the spread of fibrillar -synuclein pathology are thought to be the crucial mechanisms responsible for the development of PDD.Reference Chen, Xu, Wang and Chen23,Reference Irwin, Lee and Trojanowski27 Furthermore, the neocortical -synuclein pathology may confer a worse prognosis. Our results support the common hypothesis for PD with cognitive impairment as a predictor of death. The molecular pathological mechanism needs to be addressed in more detail in the future.
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
How Did They Do This
Dr. Backstrom works at Umea University, in Sweden. He and his colleagues work in an area in northern Sweden where approximately 142,000 people live. Umea University is the main medical center in this region, and most of the people who live there are referred to Umea University. In order to better understand the connection between PD and early death, Dr. Backstrom enrolled only people who had early PD and who were not yet taking medication for this. People were enrolled between January 1, 2004, and April 30, 2009, and were followed until August 31, 2017. Dr. Backstrom identified 182 people with symptoms of early PD.
In the study, many tests were done . All of the participants had neurologic examinations, filled out questionnaires, and had neuropsychological testing. Not everybody had the other tests . The first test was a detailed neurologic examination in order to confirm and firmly establish the diagnosis of PD. This is essential because there are several illnesses that are very similar to PD, and Dr. Backstrom wanted to be sure that the diagnosis was as precise as possible. Of the 182 patients, Dr. Backstrom found that 143 had classic PD, 13 had a similar disease called multiple system atrophy , and 18 had progressive supranuclear palsy . The other 8 had an unclear diagnosis or simply did not have PD.
Tests performed
The study was designed to look at the association of mortality with PD. During the study, 109 people died. For 98 of these , a cause of death was known.
Read Also: Fitflop Shoes For Parkinson’s
Can A Patients Ability To Make Decisions In The Last Days Of Life Be Impaired And How Is This Managed
In a North American study of 47 carers of idiopathic PD patients in the last months of life most described the goal of care as comfort, and almost half of the patients were described as unable to make any decisions in the last month of life. 10
When presenting, the patient may already be unable to communicate their symptoms and care preferences due to cognitive impairment and confusion. Also, there might be a physical difficulty in communication from severe rigidity. Care should be taken in considering the presence and consequent treatment of an intercurrent illness, and whether dopaminergic medication is exacerbating confusion due to hallucinations and/or psychosis.27
Continued attempts at verbal and non-verbal communication should be made throughout given the often fluctuating symptoms associated with PD and possible improvement in the intercurrent illness. In the absence of a next of kin or other person who is able to inform the clinical team, decisions should be made on a best interest basis as recommended in end of life care guidance.30
What Is Parkinsons Disease
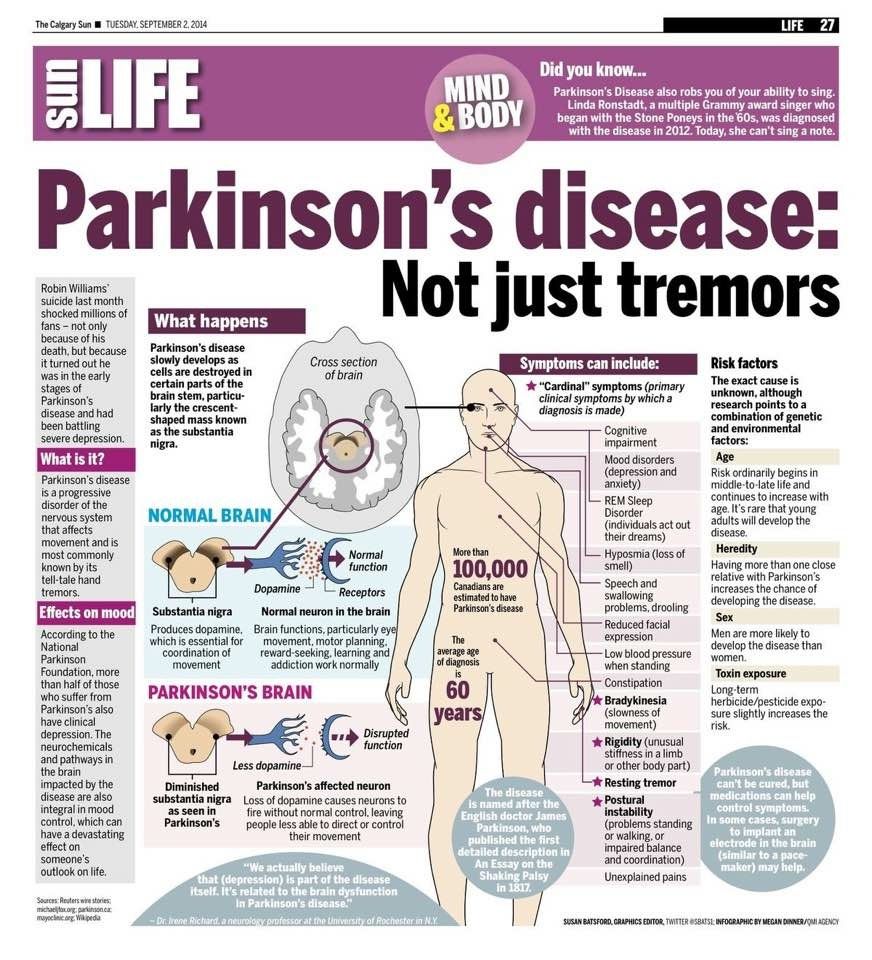
Before looking into the relationship between Parkinsons and death lets quickly review what Parkinsons is and how it affects the body.
Parkinsons Disease is a chronic neurologic condition which causes a gradual loss of the nerve cells in the brain that produce the neurotransmitter dopamine. Because dopamine carries signals to the part of the brain that control movement and coordination, decreased dopamine levels lead to the cardinal motor symptoms of Parkinsons disease like resting tremor, stiffness or slow movements. Because other parts of the brain and other neurotransmitters can be affected in Parkinsons disease, other symptoms can occur as well like lightheadedness, constipation and others. To learn more about Parkinsons .
Don’t Miss: Slowing The Progression Of Parkinson’s Disease
What Causes Parkinson Disease
Parkinson disease arises from decreased dopamine production in the brain. The absence of dopamine makes it hard for the brain to coordinate muscle movements. Low dopamine also contributes to mood and cognitive problems later in the course of the disease. Experts dont know what triggers the development of Parkinson disease most of the time. Early onset Parkinson disease is often inherited and is the result of certain gene defects.
Dont Miss: Are There Stages Of Parkinsons Disease
Myth : Deep Brain Stimulation Is Experimental Therapy
Fact: Deep brain stimulation, or DBS, is a procedure in which doctors place electrodes in the brain at the point when medications are less effective in masking motor symptoms, such as tremor, stiffness and slowness of movement.
While it may sound frightening and futuristic, its been around and successfully used for decades. DBS works very similarly to a pacemaker, except the wire is in the brain, not in the heart. Its been a standard procedure for the past two decades.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
How To Take Care Of Patients With Parkinsons Disease
The condition of Parkinsons disease progress with time and demands care from a care giver. The disease affects the motor abilities of the patient and the gradual loss of independence can be disheartening. Care givers should-
Emotional Support: Try maintaining the quality of life of the patient with proper mental support.
Read Also: What Are The Signs Of Parkinson’s Disease
How Can Falls Resulting From Parkinsons Disease Be Fatal
Patients with Parkinsons disease are seen to be at an increased risk of bad falls which can lead to death. Generally it is seen that death results from hip fractures that require hospitalization because surgery would be required. Hip surgery is a major operation which carries the risk of infection, heart failure and blood clots. Such clots become dangerous if they reach the lungs. Sometimes fall may even lead to fatal brain injuries if not taken care properly.
Read Also: Can You Reverse Parkinson Disease
Availability Of Data And Materials
Pseudonymised outcome data were supplied by NHS Digital under a data sharing agreement subject to there being no risk of identifying any individual in the publication. However, as our cohort data contains detailed information on each workers job-history and health outcomes, identification of an individual is a possibility if raw data would be freely available. Derived data from this cohort is available in our repository by writing to the corresponding author, but researchers who would like to use the data will need to obtain agreement from NHS Digital.
Also Check: How To Support Someone With Parkinsons Disease
Also Check: Parkinson’s Disease Fact Sheet
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38 and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patients handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
Recommended Reading: Judy Woodruff Parkinsons Disease
Theory Of Pd Progression: Braaks Hypothesis
The current theory is that the earliest signs of Parkinsons are found in the enteric nervous system, the medulla and the olfactory bulb, which controls sense of smell. Under this theory, Parkinsons only progresses to the substantia nigra and cortex over time.
This theory is increasingly borne out by evidence that non-motor symptoms, such as a loss of sense of smell , sleep disorders and constipation may precede the motor features of the disease by several years. For this reason, researchers are increasingly focused on these non-motor symptoms to detect PD as early as possible and to look for ways to stop its progression.
Page reviewed by Dr. Ryan Barmore, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
Also Check: Can Parkinsons Be Passed Down
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
What Is The Prognosis
The disease gets progressively worse, with people becoming severely disabled within three to five years of onset. Affected individuals are predisposed to serious complications such as pneumonia, choking, head injury, and fractures. The most common cause of death is pneumonia. With good attention to medical and nutritional needs, it is possible for individuals with PSP to live a decade or more after the first symptoms of the disease appear.
Recommended Reading: Rehabilitation Programs For Parkinsons Disease
Don’t Miss: Laser Pointer For Parkinson’s
Does Parkinsons Affect Your Lifespan
Parkinsons research and treatments have come a long way, so much so that the average life span of a person with Parkinsons is the same or near the same as someone without Parkinsons disease. However, the lifespan of a person can vary widely based upon that persons health choices, such as their diet, exercise routine, if they have a history of smoking and many other factors. So, for most people with Parkinsons, as long as you focus on managing your Parkinsons disease and make healthy choices your lifespan should not be shortened.
What Is Parkinson Disease
Parkinson disease is a movement disorder. It can cause the muscles to tighten and become rigid This makes it hard to walk and do other daily activities. People with Parkinsons disease also have tremors and may develop cognitive problems, including memory loss and dementia.
Parkinson disease is most common in people who are older than 50. The average age at which it occurs is 60. But some younger people may also get Parkinson disease. When it affects someone younger than age 50, its called early-onset Parkinson disease. You may be more likely to get early-onset Parkinson disease if someone in your family has it. The older you are, the greater your risk of developing Parkinson disease. Its also much more common in men than in women.
Parkinson disease is a chronic and progressive disease. It doesnt go away and continues to get worse over time.
Read Also: Does Parkinson’s Disease Affect The Brain
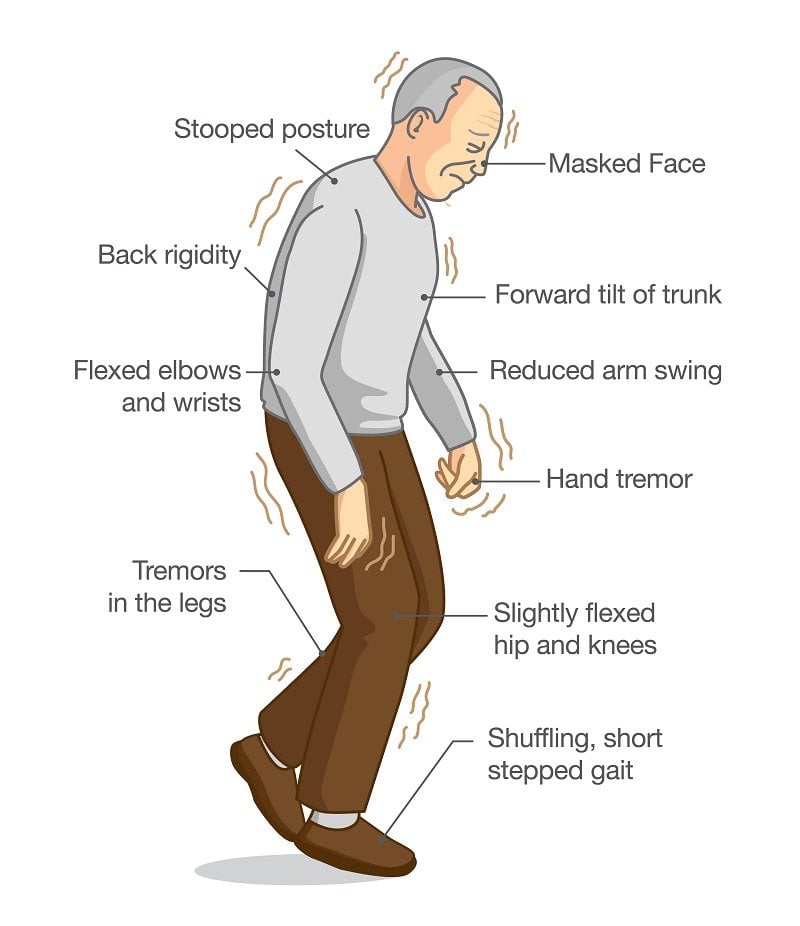
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
More Americans Are Dying From Parkinson’s Disease
HealthDay Reporter
THURSDAY, Oct. 28, 2021 — The number of Americans who are dying from Parkinson’s disease has jumped by 63% in the past two decades, new research shows.
The fresh analysis also revealed that men face double the risk of dying from the progressive and incurable disease than women. A notably higher death rate was also seen among white people, as compared with peers of other racial/ethnic backgrounds.
“The message is straightforward,” said study author Dr. Wei Bao. “This study showed that an increasing number of people died from Parkinson’s disease during the past 20 years, and this cannot be simply explained by population aging.”
Bao is an associate professor in the department of epidemiology at the University of Iowa’s College of Public Health, in Iowa City. He and his colleagues published their findings online Oct. 27 in the journal Neurology.
According to the Michael J. Fox Foundation, Parkinson’s affects roughly 1 million Americans and more than 6 million people around the world.
To get a handle on trends among Parkinson’s patients, Bao and his colleagues analyzed data collected by the U.S. National Vital Statistics System.
The team found that nearly 480,000 Americans died of Parkinson’s between 1999 and 2019.
That steady rise translated into nearly nine out of every 100,000 Americans succumbing to Parkinson’s by 2019. That figure is notably up from a little more than five Parkinson’s deaths for every 100,000 Americans just 20 years earlier.
Recommended Reading: Can Parkinson’s Disease Cause Dementia
Smr And Cause Of Death
Although some studies report survival time, SMRs allow comparison between population groups with different demographics and life expectancies.Reference Ishihara, Cheesbrough, Brayne and Schrag11 The SMR of this cohort was 0.62 , implying that the five year mortality ratio of the patients with PD was not significantly higher than the ratio of the general urban Chinese population. The SMR in the present study is consistent with the survival data from the highly selected subjects in the DATATOP study 12 and an Austrian study carried out by Diem-Zangerl and his co-workers ,Reference Diem-Zangerl, Seppi and Wenning4 and very close to the previous investigation from Hong Kong .Reference Auyeung, Tsoi and Mok3
Also Check: Parkinsons Education For Nurses
Identifying Risk Factors For Parkinsons
The risk for early death increased by about 40% for every 10-year increase in age at diagnosis.
Parkinsonâs researcher Tobias Kurth, MD, agrees that identifying risk factors for early death could help clinicians better manage the disease.
Kurth is an adjunct associate professor of epidemiology at Harvard School of Public Health.
âThis is important research that adds to our understanding of the impact of specific features of Parkinsonâs disease on outcomes,â he tells WebMD.
His own study of Parkinsonâs-associated death matched Parkinsonâs patients with people without the disease who had similar non-Parkinsonâs-related illnesses.
Like the newly reported study, patients who were older when their Parkinsonâs disease was diagnosed had a greater risk for early death.
Dont Miss: Homeopathic Medicine For Parkinson Disease
Don’t Miss: Nocturnal Leg Cramps Parkinson’s
Hoehn And Yahr Progression
Similar to the experience of Hoehn and Yahr, the rate of progression varied greatly and about 10% of patients followed a benign course. A comparison of our results for severely disabled patients and dead patients with Hoehn and Yahrs prelevodopa results shows considerable similarity with 22% of our patients disabled or dead by 4 years compared with their 28% of patients with up to 5 years of follow up. At 10 years 71% of our patients were disabled or dead compared with 61% of Hoehn and Yahrs patients who were followed up for 59 years and 83% who were followed up for 1015 years.
Do People Die From Parkinsons
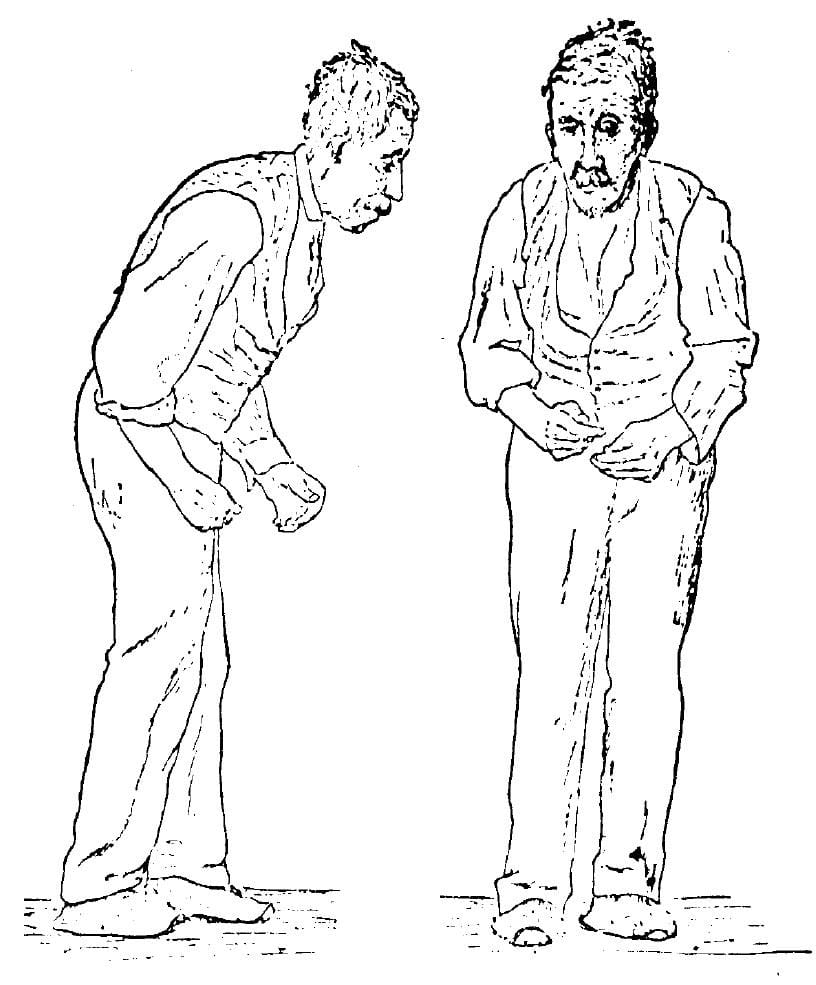
PD does not directly kill patients people with PD die from other causes, not from PD itself. Two major causes of death for those with PD are falls and pneumonia.
People with PD are at higher risk of falling, and serious falls that require surgery carry the risk of infection, adverse events with medication and anesthesia, heart failure, and blood clots from immobility.3
Pneumonia is a common cause of death, and those with PD are at risk for aspiration pneumonia.3 People with PD often have problems with swallowing, so the risk of aspirating food or drink, or having food or drink going down the wrong pipe is higher. In PD, the person may not be able to cough up the food or drink they aspirated, and it can remain in the lungs, eventually causing an infection.3 Even with general pneumonia, when coughing is weakened, as in PD, the mucus and other material that needs to be coughed up isnt able to be expelled, and this makes effective treatment of pneumonia more difficult in those with PD.
You May Like: Transcranial Magnetic Stimulation Parkinson’s