Managing Advanced Parkinsons Disease
Advanced Parkinsons disease, stage 4 or 5 of the Hoehn and Yahr Scale, is characterized by very limited mobility without assistance, severe motor deficits, risk of falls, and cognitive and psychotic problems. With the advent of L-dopa and other dopaminergic treatments, the progression of PD has become markedly slower however, over the years treatment loses its efficacy, while a number of complicationssuch as motor fluctuations and dyskinesiadevelop, probably due to the progressive loss of dopaminergic neurons and their striatal and cortical connections. These complications are observed in 50% of patients after 5 years of disease and in 80% of patients after 10 years of treatment .
Treatment of the advanced stages of PD is entirely different from earlier stages. Early treatment is geared towards symptom relief and prevention of motor symptoms. During the later stages, the palliative care model is introduced to provide the patient with comfort and support. In the advanced stages, the focus of treatment shifts to treating nonmotor symptoms using a more supportive and palliative approach .
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to person, and it is not possible to predict how quickly the disease will progress.
- Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease.
- Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death.
- Many treatment options can reduce some of the symptoms and prolong the quality of life.
How Can I Support Someone With Parkinson’s At The Advanced Or Palliative Stage
In the advanced stages of Parkinsons, your patients care needs may be more complex and require careful planning along with the patient, their family and other health and social care professionals involved.
Palliative care should be holistic, considering the whole person to support the personal, social, psychological and spiritual needs of your patient and their family. It should give your patient some control and choice over areas such as treatment options and where they will be cared for, as well as providing advice and support to all the people involved in their care.
Palliative care in Parkinsons may be supported by a number of professionals, including a Parkinsons nurse specialist, local hospice or specialist palliative care team, physiotherapist, occupational therapist, speech and language therapist or dietitian. Many people with Parkinson’s also find complementary therapies beneficial.
It is important that you find out whether the person has a care plan in place regarding their preferences for how the issues surrounding advanced Parkinsons should be managed. This could include legal documentation such as a Lasting Power of Attorney and an advance care plan. Advance care plans include information on what the persons wishes and preferences are for their care in the future. They may include decisions on any treatments the person doesnt want to have in the future this is called an Advance Directive, Advance Decision to Refuse Treatment or Living Will.
Recommended Reading: Similar To Parkinsons
Stage Four: Symptoms Are Severe And Disabling And You Often Need Assistance To Walk Stand And Move
Stage Four Parkinsons disease is often called advanced Parkinsons disease. People in this stage experience severe and debilitating symptoms. Motor symptoms, such as rigidity and bradykinesia, are visible and difficult to overcome. Most people in Stage Four arent able to live alone. They need the assistance of a caregiver or home health aide to perform normal tasks.
Causes Of Parkinson’s Disease
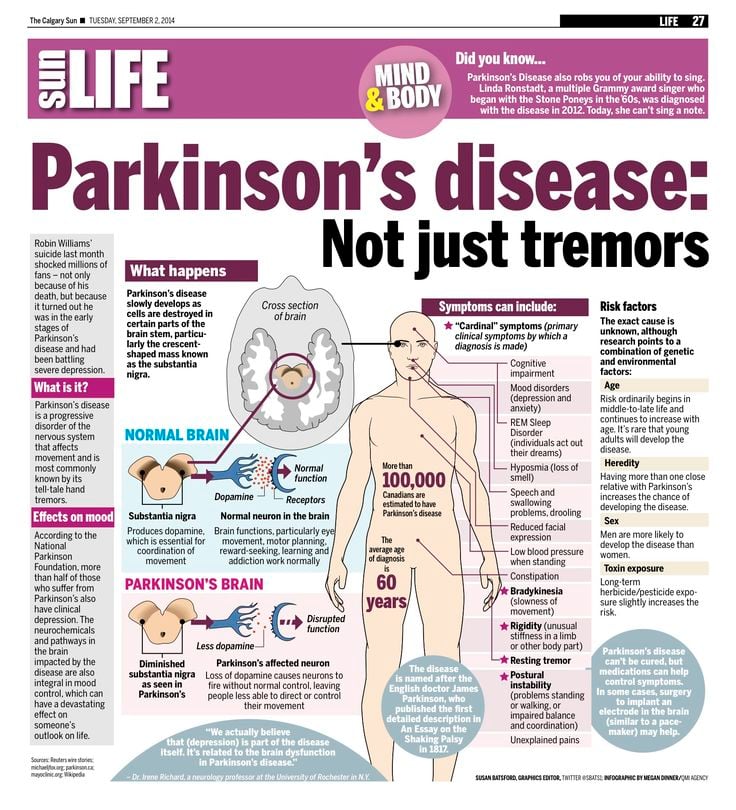
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Read Also: Diseases Similar To Parkinsons
Signs Of Parkinsons Disease
In 1817, Dr. James Parkinson published An Essay on the Shaking Palsy describing non-motor, as well as, motor symptoms of the illness that bears his name. Parkinsons is not just a movement disorder, explained Dr. Shprecher. Constipation, impaired sense of smell, and dream enactment can occur years before motor symptoms of Parkinsons. The latter, caused by a condition called REM sleep behavior disorder, is a very strong risk factor for both Parkinsons and dementia . This has prompted us to join a consortium of centers studying REM sleep behavior disorder.
How Care Providers Can Assist With Late Stage Parkinsons Care
With added hands-on care required, its essential for family caregivers to learn how to properly and efficiently provide this support to minimize the possibility of doing harm to either themselves or the loved one being cared for.
If the older adult isnt already receiving physical therapy services, check with the physician for a referral. The physical therapist, while helping optimize the persons ability level, may also advise family caregivers on the ideal approaches for hands-on assistance.
One new symptom that frequently develops in the later stages of Parkinsons is freezing, when the person is suddenly unable to move. Methods to help break a freezing episode include:
- Using a laser pointer and asking the person to step on the light
- Utilizing a rhythmic noise, such as clapping, and encouraging the person to take a step with each clap
- Playing music and prompting the individual to walk to the beat
As always, stay close at hand when the person is mobile to avoid a fall.
Make sure to provide an abundance of extra time for day-to-day activities such as getting dressed and eating, which are likely to take longer now. This is important in protecting the persons self-sufficiency. Even if it requires longer to accomplish a task, it is always better to foster as much self-reliance as you possibly can.
Don’t Miss: Parkinson’s Hallucinations Commercial
Hospice Eligibility Of End
Since Parkinsons disease is progressive, patients need hospice care. If your family member or any loved one has been diagnosed with Parkinsons disease, expect that there will be a decline in their motor abilities. They will need professional nursing care to attend to their needs because it will be harder for them to speak and express their struggles.
Here are the things you need to observe to determine if the patient already needs hospice care:
- Difficulty in breathing and oxygen supply is necessary
- Difficulty in walking where a wheelchair is already needed
- Hard to understand speech
- Difficulty in eating and drinking
- More complications occur, such as pneumonia, sepsis, pyelonephritis, decubitus ulcers, and other comorbidities
How Can Healthcare Professionals Support People With Parkinsons When They Are Making Decisions About End Of Life
Access to resources is a specific issue for different countries and communities, as palliative care and end of life management varies through European countries.
Still, there is an ongoing need for awareness about palliative care among healthcare professionals especially in the ability to explain the conditions progression, accompanying problems, interventions for relief and end of life activities. Skills for identifying spiritual distress and arranging an end of life should be included in the expertise of Parkinsons disease practitioners, to help people with the condition with any legal and financial issues, existential challenges, care plans, wishes for treatment, wills and anything else that needs to be considered.
Read Also: Judy Woodruff Health Problems
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
How Long Does It Take Parkinson’s Disease To Progress
In most cases, symptoms change slowly, with substantive progression taking place over the space of many months or years. Many people with PD have symptoms for at least a year or two before a diagnosis is actually made. The longer symptoms are present, the easier it is to predict how a person with PD will do over time.
Recommended Reading: Zhichan Capsule
Therapeutic Management Of Late
, December 12, 2011
This review of the Movement Disorder Societys guidelines for therapeutic management of late-stage Parkinsons applies the guidelines to a case scenario. The guidelines first appeared in the European Handbook of Neurological Management. This review cites the Annals of Long-Term Care: Clinical Care and Aging, 2011 19 : 42-46.
Parkinson’s Progression Palliative And End Of Life Issues
This 38-minute webinar provides an overview of Parkinson’s symptoms, and treatment challenges due to disease progression. 18-minutes in the topic turns to planning a good death, the euphemisms even doctors use to avoid discussing death, the most common cause of death in those with PD, putting your end-of-life preferences in writing. Palliative care can help families face these end-of-life issues.
Also Check: Voice Amplifiers For Parkinson’s
What Is Parkinson’s Disease
Parkinson’s disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinson’s disease and the degree of impairment varies from person to person. Many people with Parkinson’s disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinson’s disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinson’s disease will increase in the future. Adult-onset Parkinson’s disease is most common, but early-onset Parkinson’s disease , and juvenile-onset Parkinson’s disease can occur.
Caring For A Family Member With Late Stage Parkinsons Disease: Part 3 Of 3
The late stage of Parkinsons disease can present new caregiving challenges for family members.
A Parkinsons diagnosis affects family members along with the person who is afflicted. Understanding what to anticipate as the illness progresses is the key to being prepared for the changes to come and to making life the very best it can be each and every day.
Over the last few months, we have shared information about what to anticipate in the early and middle stages of Parkinsons disease. Information has included what family members can do to best help a loved one with Parkinsons and how Abby Senior Care, a provider of professional personal care in Denver, CO and the surrounding communities, can help. In this closing segment in the series, we provide information about taking care of someone with late stage Parkinsons disease.
Don’t Miss: Cleveland Clinic Parkinson’s Bicycle Study 2017
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
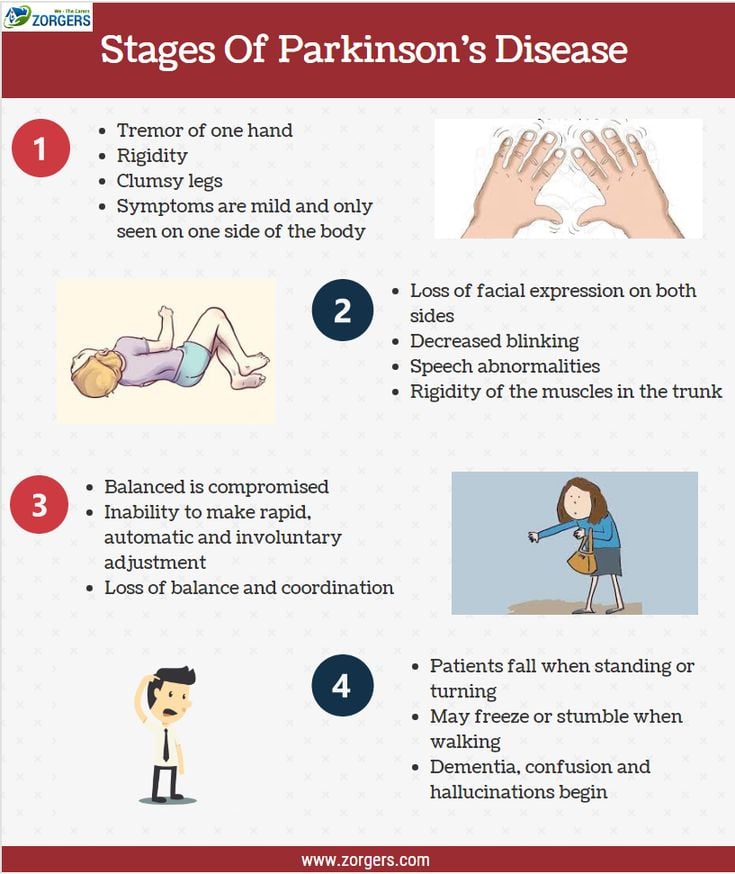
The Stages Of Parkinsons Disease
Stage One The Initial Stage: Symptoms are generally mild and may be easier to hide. Common symptoms include tremors, poor posture, balance issues, stooping of the back, and shaking of the limbs.
Stage Two Both Sides of the Body are Affected: The Parkinsons now affects both sides of the body, with increased symptoms that are more noticeable. Daily tasks become more difficult as symptoms now affect the entire body. It is harder to maintain your balance, walking becomes more difficult and tremors/shaking is more frequent.
Stage Three Increased symptoms & overall slowing down: By stage 3 the typical symptoms are more pronounced and the list of symptoms becomes more inclusive. One of the most noticeable changes is that movements and actions are much slower including facial expressions, speech, and motor skills. It is common to common to feel light headed, fainting, and experience hypo-tension .
Stage Five The Final Stage: During the final stages the person will require 24/7 one on one care and nursing skills. By stage 5, hospice care for late stage Parkinsons is a necessity and will help everyone involved with the acceptance of the final stage of the disease.Our trained hospice providers will guide you through these final stages. Our goal is to focus on the patient and the family unit as a whole.
Recommended Reading: Pfnca Wellness Programs
What Are The Important Points Regarding Apomorphine At The End Of Life
Apomorphine is a dopamine agonist, which is given as a subcutaneous infusion either continuously or intermittently and also as single subcutaneous injections. An overview of studies into apomorphine use shows improvement in motor off periods and in dyskinesias.39
Apomorphine has side-effects similar to other dopaminergic medication but also notably nausea and vomiting. Ondansetron is not recommended for nausea in patients using apomorphine due to adverse effects.21
Subcutaneous apomorphine has been used at the end of life in a patient with advanced PD although with the recommendation that this is by a healthcare professional experienced in its use.40
Parkinson’s Disease Symptoms: Life Expectancy
Even though Parkinson’s disease is a serious, progressive condition, it is not considered a fatal illness. People who have Parkinson’s disease usually have the same average life expectancy as people without the disease.
But when the disease is in its advanced stages, Parkinson’s symptoms can lead to life-threatening complications, including:
- Falls that lead to fractured bones
- Pneumonia
- Choking
Thinking about the progression of Parkinson’s disease can be frightening. But proper treatments can help you live a full, productive life for years to come. And researchers hope to one day find ways to halt the progression of Parkinson’s and restore lost functioning.
Recommended Reading: Prayers For Parkinson’s Disease
Dyskinesia Current And New Treatment Strategies
The occurrence of dyskinesia is still common in PD notably in those individuals treated with L-dopa . However, disabling troublesome dyskinesia does not appear to be as prevalent as in previous eras and this probably reflects the more cautious treatment of early PD with an emphasis on avoiding dyskinesia induction. The exception is those individuals with a young onset variant of PD who are highly vulnerable to the early occurrence of motor complications . In contrast, non-troublesome dyskinesia remains a frequent side-effect of L-dopa therapy in the PD population but often does not require treatment while other components of motor function are adequately maintained. A lessening of the impact of dyskinesia is also a reflection of the earlier detection and treatment of PD in general as the severity or duration of disease as judged by dopaminergic nigral cell loss, is a primary factor in determining the degree of exposure to L-dopa needed to initiate involuntary movements . However, the impact of dyskinesia is in its inevitable expression by all forms of dopaminergic medication, once involuntary movements are established.
Table 1 Examples of existing and novel approaches to the treatment of dyskinesia
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage

Parkinsons progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinsons about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinsons may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more off periods when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinsons symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinsons most often die because of an infection or another condition, usually caused by Parkinsons.
You May Like: Judy Woodruff Parkinson’s
Regular Physical Activity May Help Slow Parkinson’s Disease
A few hours of exercise a week may help slow Parkinson‘s disease, even if it’s just moderate activity such as walking or gardening, a new study suggests.
The key is to be consistent, the researchers found.
“Although medications can provide people with Parkinson’s some symptom relief, they haven’t been shown to slow the progression of the disease,” said study author Dr. Kazuto Tsukita, of Kyoto University in Japan.
“We found that regular physical activity, including household tasks and moderate exercise, may actually improve the course of the disease over the long run,” he said. “Best of all, exercise is low-cost and has few side effects.”
Tsukita and his team assessed physical activity in 237 people with early-stage Parkinson’s. The participants were followed for up to six years.
While their activity levels at the outset did not affect the progression of their Parkinson’s, those who regularly got at least four hours a week of moderate to vigorous exercise during follow-up had slower declines in balance and walking ability than those who were less active.
The patients’ Parkinson’s symptoms were rated on a scale of 0 to 4, with higher scores indicating more severe symptoms, according to findings published online Wednesday in Neurology.
More information
- Topics