Depression May Be An Early Symptom Of Parkinsons
Depression is one of the most common, and most disabling, non-motor symptoms of Parkinsons disease. As many as 50 per cent of people with Parkinsons experience the symptoms of clinical depression at some stage of the disease. Some people experience depression up to a decade or more before experiencing any motor symptoms of Parkinsons.
Clinical depression and anxiety are underdiagnosed symptoms of Parkinsons. Researchers believe that depression and anxiety in Parkinsons disease may be due to chemical and physical changes in the area of the brain that affect mood as well as movement. These changes are caused by the disease itself.
Here are some suggestions to help identify depression in Parkinsons:
- Mention changes in mood to your physician if they do not ask you about these conditions.
- Complete our Geriatric Depression Scale-15 to record your feelings so you can discuss symptoms with your doctor. Download the answer key and compare your responses.
- delusions and impulse control disorders
The One Show: Michael J Fox On Hopes To Find Parkinsons Cure
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
Anosmia i.e. a loss of sense of smell sometimes occurs “several years” before other symptoms develop, the NHS stated. Parkinson’s is estimated to affect 127,000 people in the UK alone. Exactly why Parkinson’s occurs is still unknown, although a combination of genetic and environmental factors are said to be responsible. When dopamine levels plummet, physical movement is affected, which can lead to a number of side effects.
How Is Parkinson’s Disease Diagnosed
A person doesn’t need to have all the signs and symptoms of Parkinson’s disease to be diagnosed with it.
“In general, people have a combination of the motor symptoms and the non-motor symptoms,” says Dr. Nwabuobi. “Some people have more non-motor symptoms than motor and vice versa, but in order to have a diagnosis of Parkinson’s, you definitely need the motor symptoms. We’re looking for specific things , including a rest tremor, bradykinesia, rigidity, and poor balance.”
According to the Parkinson’s Foundation, a person needs to have two of the four main motor symptoms of Parkinson’s over a period of time to be diagnosed with the disease.
Also Check: Young Onset Parkinson’s Life Expectancy
Description Of The Included Studies
3.2.1. Methods Evaluating the Mechanical or Neurophysiological Properties of the Muscle
Eleven studies were included, which are summarized in . Of these, five used electromyography , three used myotonometry , and three used elastography . The study design chosen in all cases was casecontrol, except for the study by Hayashi et al., who used a prepost design. The sample size was quite low for all the studies . Five out of 11 studies did not reach 20 participants, whilst only 3 of 11 papers had a sample size 30 participants.
Muscle Rigidity Lead Pipe And Cogwheel Rigidity
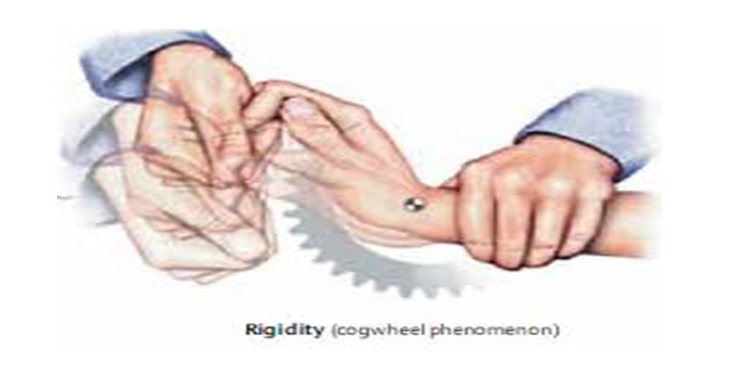
Muscle rigidity caused by Parkinsons disease may be misdiagnosed with arthritis or general tightness due to aging. Rigidity may affect your legs, arms, and torso, as well as your face. The rigidity can affect your legs, arms, torso, and face.
It is what rigidity feels like. It may be difficult for your muscles to move. They may also stiffen involuntarily like a muscle spasm. This stiffness can cause muscle and joint pain.
The rigidity can impact your daily life. This stiffness can cause problems in your everyday life. Because rigidity can make simple tasks such as cleaning or exercising difficult, it can also hinder your ability to fulfill hobbies and pursue other activities. Other symptoms include:
- You may feel stiffness in your facial muscles, which makes it difficult to express yourself
- Paralysis during sleep makes it difficult to fall asleep comfortably and get good quality sleep.
- Tension in the muscles can lead to muscle fatigue and a lack of energy.
- Difficulty in specific motor skills like writing and dressing
- Stiffness in the arms can make it difficult to walk with balance.
You May Like: Bicycle Therapy For Parkinson’s Disease
Make Commercial Breaks Movement Breaks
If youre watching TV, stand up and march while you swing your arms during the commercials. To increase your muscular strength, lift soup cans or a do a few downward dogs.
Moving more every day is easier said than done. Remember, even small changes can make a big difference. Pat yourself on the back for all of the movement activities you do each day. Every victory counts!
How Can You Be Tested For Cogwheeling
Your doctor will ask you to relax your muscles so that you can be tested for rigidity in the cogwheel. Your doctor will then stretch and flex your limb. They want to know if:
- When they try to move your muscle, it becomes stiff and rigid.
- Your limbs move with tiny, jerky movements .
Cogwheel rigidity is characterized by ratcheting movements. It might feel like a click in your muscle when you move your arm.
Cogwheel rigidity also manifests itself in jerky movements that occur even when the doctor moves your limb slowly. It distinguishes it from spasticity, another potential symptom of Parkinsons disease.
Also Check: How Does General Anesthesia Affect Parkinson’s
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
How Is Rigidity Assessed In A Physical Exam In Patients With Parkinson Disease
Rigidity refers to an increase in resistance to passive movement about a joint. The resistance can be either smooth or oscillating . Cogwheeling is thought to reflect tremor rather than rigidity and may be present with tremors not associated with an increase in tone . Rigidity is usually tested by flexing and extending the patient’s relaxed wrist and can be made more obvious by having the patient perform voluntary movements, such as tapping, with the contralateral limb.
You May Like: How Does Parkinson’s Disease Kill You
Every Person With Parkinsons May Experience Different Movements
There are multiple types of movements that a person with Parkinsons disease can experience. Some people may have just one or two of these symptoms, while another may experience all of them. Likewise, the degree of severity can vary from person to person, and symptoms that may bother some people may not bother others at all.
Its important to note that theres not a single answer that works for every person with Parkinsons, says Todd Herrington, MD, PhD, a neurologist at Massachusetts General Hospital in Boston and an instructor in neurology at Harvard Medical School in Cambridge, Massachusetts. You have to ask the person, What bothers you, and how much does it affect you? What the caregiver or the even the physician observes as the most severe symptoms may not feel that way to the person with Parkinsons.
Here are eight types of movements that people with Parkinsons may experience. Learn more about what these symptoms are and what can be done to prevent them.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Recommended Reading: Possible Causes Of Parkinson’s Disease
What Will My Doctor Do To Check For Rigidity
Your doctor will ask that you keep your limbs as loose and relaxed as possible during your appointment. The doctor will then gently stretch and extend your joints, such as elbows, wrists, and shoulders.
Your doctor will notice increased resistance to movement in either direction extension or flexion if you are experiencing rigidity. Cogwheel rigidity has a unique feature: the jerky motion can occur at both slow and high speeds.
Treatment And Management Options
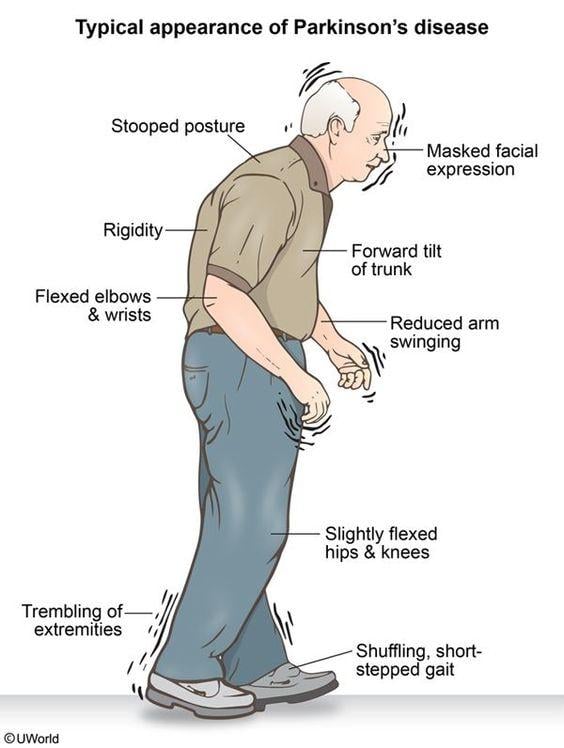
There are several treatment options available to alleviate the motor symptoms associated with Parkinsons disease. Most of them also help Parkinsons patients overcome issues related to rigidity. These include:
- Medications such as levodopa , dopamine agonists, anticholinergics, catechol-O-methyl transferase inhibitors, and monoamine oxidase-B inhibitors. One treatment or a combination of treatments is commonly prescribed to Parkinsons disease patients to improve motor problems, including rigidity, that occur due to dysfunction in dopaminergic neurons.
- Physiotherapy to improve mobility and the range of movement in muscles and joints, and to alleviate the muscle cramps common in Parkinsons disease patients. An occupational therapist or physiotherapist can advise on daily routines, exercises, and the use of assistive devices, such as walkers or canes, to help the patient stay as mobile and independent as possible. Occupational therapy is generally needed for patients to perform daily activities more effectively, such as rolling in bed or getting up from a chair, for example. Regular exercise and stretching can strengthen muscles and maintain flexibility.
- Speech therapy that teaches facial exercises to help with speech and communication.
- Deep brain stimulation for Parkinsons disease patients whose symptoms are not adequately controlled with medications and/or exercise.
Also Check: Does David Brooks Have Parkinson’s
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Gait & Balance Abnormalities
Parkinsons Disease Exam
Patients with Parkinsons disease can develop an alteration of the postural reflexes that causes instability in gait and balance control. Such alterations usually develop later in the course of the illness and are a major cause of disability, especially because of the high risk for falls that derives.
Using the exam to pick up postural instability is of the utmost importance for the management of patients with PD, since it will trigger either a medication adjustment or a physical therapy intervention both aimed at falls prevention.
We have three tests for this part of the PD exam:
1) Standing up from a chair
2) Free walking
3) Provoked pull test maneuver for balance
Don’t Miss: Is Parkinson’s A Form Of Cancer
Treating And Managing Rigidity
Talk to your doctor as rigidity tends to respond well to medication, for example levodopa. As with all Parkinsons medications though, what works for one person may not work for another. Be prepared for your doctor to try several approaches to see what works best for you.
He or she may refer you to a doctor who specialises in movement disorders or to a physiotherapist, occupational therapist or speech and language therapist depending on the country in which you live and your individual needs. Seeing a therapist soon after problems begin is more likely to result in successful treatment.
Treatment varies from country to country but the following broadly outlines the support you might receive:
- A physiotherapist can advise on exercises to maintain or improve both mobility and the range of movement in your muscles and joints. He or she can also suggest strategies to perform daily activities in a more effective way, for example how to roll in bed or get up from a chair.
- An occupational therapist or physiotherapist will be able to advise on devices and aids to help you in your everyday life. An occupational therapist will also be able to suggest changes to your routine to help you to stay mobile and independent.
- A speech therapist can teach you facial exercises to help with speech and communication.
Passive Manipulation Of Limbs
To test for the presence of rigidity, we need to passively manipulate the limbs of the patient. However, If the disease is in its early stage or the symptoms are well controlled with medications, we may not be able to see rigidity. We will need to use some activation maneuvers, that basically consist in performing repetitive movements with the limb contralateral to the one that is being tested.
Also, there are two types of rigidity:
– Lead-pipe rigidity: where the tone is uniformly and smoothly increased throughout the entire range of movement
– Cogwheel rigidity: where a tremor is superimposed on the hypertonia, making the movement irregular due to intermittent increase and reduction of tone
Upper Extremity Testing
For the upper extremity the most sensitive joint where to check for rigidity is the wrist. To uncover rigidity, passively rotate the wrist and feel for a resistance to the movement. It is very important that the arm of the patient is fully relaxed when rotating the wrist. To do this, place your proximal hand under the patients forearm, while your distal hand grabs and rotates the wrist of the patient. When rigidity is present, the range of motion will be preserved but you will feel a resistance in performing the movement.
Wrist rotation with activation maneuver.
It is also possible to test for rigidity in the elbow by passively flexing and extending the forearm.
Elbow flexion-extension with activation maneuver.
Lower Extremity Testing
You May Like: Parkinson’s And Bad Taste In Mouth
Data Extraction And Analysis
A systematic review was conducted by two independent authors. We used a standardized data extraction protocol, collecting information about population, intervention, methods, results, and outcome measures. For each study we defined the design, sample size, joint explored, type of system used for the quantification of rigidity, evaluation protocol, rigidity outcome measures, and other clinical variables related to PD severity, functional independence, quality of life, and results. Finally, both authors reached an agreement about each extracted data item. Studies employing objective assessment methods of muscle rigidity in PD patients were selected.
Reduced Sense Of Smell
If youre having trouble smelling pungent foods or can no longer pick up your favourite scents, it could have many causes. Its not the most common symptom of Parkinsons, but Dr. Hall says patients who suffer a loss of smell sometimes report it as being the earliest sign they experienced. The link between reduced sense of smell and Parkinsons isnt clear, but one theory is that the clumps of the protein alpha-synuclein, found in the brains of all Parkinsons patients, may form in the part of the brain responsible for smell before migrating to other areas and affecting motor function.
You May Like: How Long Does A Parkinson’s Patient Live
Apda In Your Community
APDAParkinson’s Disease SymptomsCould this be due to Parkinsons Disease? Uncommon non-motor symptoms of Parkinsons Disease
It is common for a person with Parkinsons disease to attribute every new symptom that develops to PD. That is largely because the list of non-motor symptoms commonly associated with PD is so varied, it can seem that almost anything is a symptom of PD! But if you take a closer look, there are some symptoms that are very commonly associated with PD, others that are virtually never associated with PD, and some in between.
Lets divide up non-motor symptoms into the following categories:
How Is Psp Different From Parkinson’s Disease
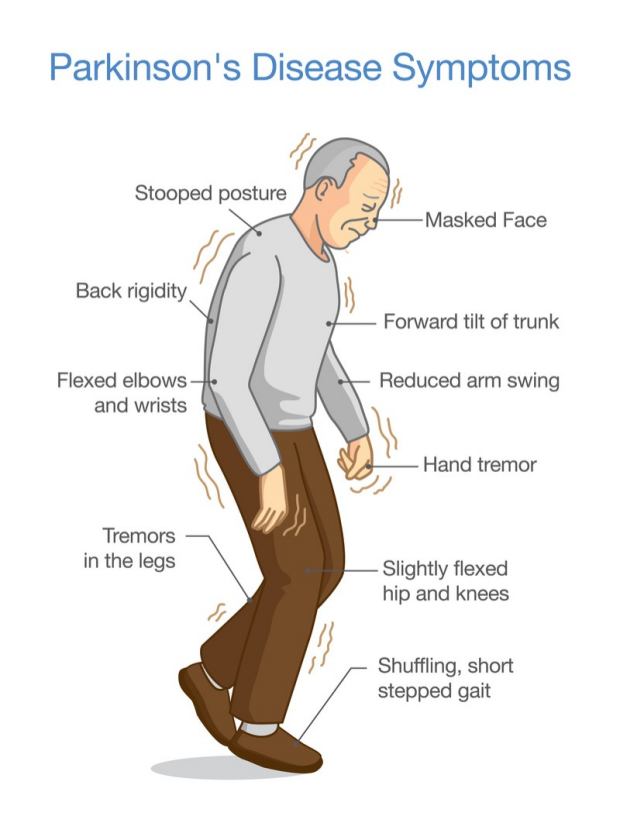
PSP is often misdiagnosed as Parkinsons disease, especially early in the disorder, as they share many symptoms, including stiffness, movement difficulties, clumsiness, bradykinesia , and rigidity of muscles. The onset of both diseases is in late middle age. However, PSP progresses more rapidly than Parkinsons disease.
- People with PSP usually stand exceptionally straight or occasionally tilt their heads backward . This is termed axial rigidity. Those with Parkinson’s disease usually bend forward.
- Problems with speech and swallowing are much more common and severe in PSP than in Parkinson’s disease and tend to show up earlier in the disease.
- Eye movements are abnormal in PSP but close to normal in Parkinson’s disease.
- Tremor is rare in PSP but very common in individuals with Parkinsons disease.
Although individuals with Parkinson’s disease markedly benefit from the drug levodopa, people with PSP respond minimally and only briefly to this drug.
People with PSP show accumulation of the protein tau in affected brain cells, whereas people with Parkinsons disease show accumulation of a different protein called alpha-synuclein.
You May Like: How Does Occupational Therapy Help Parkinson Disease