Dyskinesia And Wearing Off
If youve been taking a Parkinsons drug that contains levodopa for example, co-beneldopa or co-careldopa for some time, you may develop motor fluctuations, wearing off and dyskinesia. These are side effects that can affect your movement.
Dyskinesia is muscle movements that people with Parkinsons cant control. They can include twitches, jerks, twisting or writhing movements. Dyskinesia can affect various parts of the body such as the arms, legs and torso.
There are different types of movements, and when and how often they appear can be different for each person with Parkinsons. Some people can have dyskinesia for most of the day. Others may only experience it after taking their medication or just before the next dose is due.
People with Parkinsons can also experience this side effect when levodopa is at its highest level in the bloodstream , and the dopamine levels in their brains are at their highest. Dopamine is a chemical messenger made in the brain. The symptoms of Parkinson’s appear when dopamine levels become too low.
Because dyskinesia causes people to move around so much it can sometimes cause weight loss. If youre worried about this, speak to your GP, specialist or Parkinsons nurse. They can refer you to a dietitian, who will be able to help you maintain a healthy weight.
If you go from having good control of your movement symptoms to having less control, its called a motor fluctuation. This change can happen slowly or quickly.
What Is Tardive Dyskinesia Symptoms Causes Diagnosis Treatment And Prevention
Sometimes medications used to treat serious conditions can bring on serious conditions of their own. Thats the case with tardive dyskinesia , a neurological syndrome marked by random and involuntary muscle movements that usually occur in the face, tongue, lips, or jaw.
Its typically caused by long-term use of antipsychotic medications that block dopamine receptors. Antipsychotic medications are used to treat a number of mental illnesses and mood disorders, including schizophrenia, bipolar disorder, and depression.
Tic And Tourette Syndrome:
Motor tics are repetitive, usually quick movements that can usually be suppressed by the person who has them, at least for a few seconds. They are not a nervous habit, but are believed to be neurological in their origin. Tourette syndrome is the name applied when motor tics associated with vocal tics begin in childhood, last longer than a year, and change over time. Most people who have Tourette syndrome do not have the famous symptom of uttering obscenities.
Tic is common, particularly in childhood, and may improve or cease altogether as one grows older. Occasionally it is sufficiently troubling that medication is warranted. Teasing from other children, or misunderstanding and criticism from parents and teachers are sometimes more problematic than the tic itself.
Also Check: Parkinson’s Bike Therapy
Dystonia Sometimes Affects These Other Areas Of The Body
Though oromandibular dystonia specifically relates to the face, jaw, and tongue, there are several other types of dystonia that can be associated with PD and may affect different parts of the body. These other types can affect the neck and head , the legs, feet, arms, and hands , the vocal cords , or eyes .ae0fcc31ae342fd3a1346ebb1f342fcb
Be sure to speak with your medical provider if you notice involuntary movement or prolonged muscle contractions in any area of your body.
Fast Facts On Lip Twitching:

- Lip twitching is the involuntary movement of muscles in the lip.
- The muscles in the face and lips are controlled by the facial nerve.
- If the twitches are exaggerated and noticeable, they may feel embarrassing.
There are many causes for lip twitching, with some being simple everyday habits.
Twitching usually occurs in the upper or lower lip separately, as the lips are independent of one another.
Possible causes for lip twitching include ingesting too much caffeine, a potassium deficiency, reactions to certain medications or drugs, and various medical conditions. It can even be caused by stress or tiredness.
Twelve possible causes of lip twitching are discussed below.
Don’t Miss: Yopd Life Expectancy
What Causes Dyskinesia In Parkinson’s Disease
Unlike “off” time, patients typically experience dyskinesia in Parkinson’s when medications are working and other symptoms are under control. Researchers aren’t exactly sure what causes dyskinesia, but it is believed to be a side effect of long-term levodopa use, not a symptom itself. Levodopa-induced dyskinesia can look like fidgeting, writhing, wriggling, head bobbing, or body swaying. LID can sometimes be confused with Parkinson’s tremor, which is a back and forth shaking caused by the disease.
Because levodopa is taken throughout the day, dopamine levels in the brain rise and fall. These fluctuating levels of dopamine combined with the continued loss of dopamine in the brain make it difficult to maintain regular dopamine levels, and lead to dyskinesia.
Individuals diagnosed with Parkinson’s at a younger age are more likely to experience dyskinesia. It’s also more common in later stages of Parkinson’s or in those who have taken levodopa for several years.
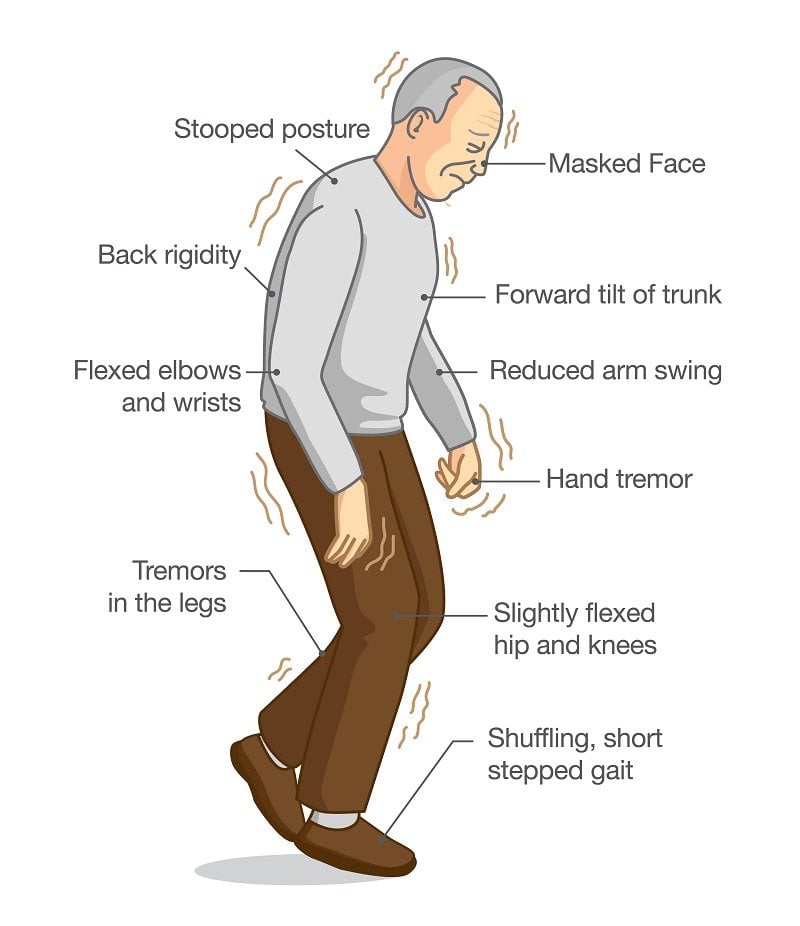
Every Person With Parkinsons May Experience Different Movements
There are multiple types of movements that a person with Parkinsons disease can experience. Some people may have just one or two of these symptoms, while another may experience all of them. Likewise, the degree of severity can vary from person to person, and symptoms that may bother some people may not bother others at all.
Its important to note that theres not a single answer that works for every person with Parkinsons, says Todd Herrington, MD, PhD, a neurologist at Massachusetts General Hospital in Boston and an instructor in neurology at Harvard Medical School in Cambridge, Massachusetts. You have to ask the person, What bothers you, and how much does it affect you? What the caregiver or the even the physician observes as the most severe symptoms may not feel that way to the person with Parkinsons.
Here are eight types of movements that people with Parkinsons may experience. Learn more about what these symptoms are and what can be done to prevent them.
Don’t Miss: Parkinson Bicycle Cleveland Clinic
Wake Forest Baptist Multidisciplinary Approach
The treatment of movement disorders at Wake Forest Baptist is a collaborative effort between neurologists and neurosurgeons.
Quality of life is further enhanced by the participation of physical, occupational and speech therapists, and otolaryngologists who have special expertise in speech and swallowing difficulties.
Involuntary Mouth Movements Can Signal Parkinsons Disease
Parkinsons is among the leading neurological ailments in the US and a topic of interest among health professionals. So, how does Parkinsons affect the body?
Parkinsons disease is an ailment associated with damage to the central nervous system, and it links with several genetic factors. The detriment of brain cells in the part of the brain called substantia nigra is among the leading causes of PD.
In addition, the disease is often associated with finger disorder because people often experience trembling in their hands. But it can be hard to relate some Parkinsons disease symptoms with the actual ailment. So now, experts are looking elsewhere for signs, specifically on the mouth.
Also Check: Weighted Silverware
Is There Any Treatment
There is currently no effective treatment for PSP and symptoms usually do not respond to medications.
- Parkinsons disease medications, such as ropinirole, rarely provide additional benefit. In some individuals, other antiparkinsonian medications, such as levodopa, can treat the slowness, stiffness, and balance problems associated with PSP, but the effect is usually minimal and short-lasting.
- Botulinum toxin, which can be injected into muscles around the eyes, can treat excessive eye closing.
- Some antidepressant drugs may offer some benefits beyond treating depression, such as pain relief and decreasing drooling.
Non-drug treatment for PSP can take many forms.
- Weighted walking aids can help individuals avoid falling backward.
- Bifocals or special glasses called prisms are sometimes prescribed for people with PSP to remedy the difficulty of looking down.
- Exercise supervised by a healthcare professional can keep joints limber but formal physical therapy has no proven benefit in PSP.
A gastrostomy may be necessary when there are swallowing disturbances or the definite risk of severe choking.
Deep brain stimulationwhich uses surgically implanted electrodes and a pacemaker-like medical device to deliver electrical stimulation to specific areas in the brain to block signals that cause the motor symptoms of several neurological disordersand other surgical procedures commonly used in individuals with Parkinsons disease have not been proven effective in PSP.
Tardive Dyskinesia Treatment: Surgical Options
Deep brain stimulation is a procedure where electrodes are placed in specific areas of the brain. The electrodes block the abnormal brain circuitry seen in patients with neurological conditions such as Parkinsons disease, essential tremors, dystonia and dyskinesia.
DBS does not destroy the overactive cells, like other movement disorders treatments such as pallidotomy and thalamotomy surgeries. Rather, it temporarily blocks the abnormal signals and is a reversible process. In DBS, a lead is permanently implanted into your brain and connected to a generator, which is attached under the skin of your chest.
An alternative to making a lesion with an electrode is to use highly focused radiation. Two types of devices can be used to deliver stereotactic radiosurgery, namely the Gamma Knife® and the LINAC-Scalpel.
Don’t Miss: Parkinson’s Hallucinations Commercial
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Neurological Or Neurodegenerative Diseases

These are progressive illnesses and slowly get worse over time. They are caused by disorders of the nerves in the brain and spinal cord, due to:
- Heredity: Many neurodegenerative illnesses run in families and are inherited, though not all family members need to be affected.
- Autoimmune conditions: The body’s own immune system turns against some of its other systems in this case, the nervous system. The reasons for this are not clear.
Recommended Reading: On Off Phenomenon
Pathophysiological Aspects Of Movement Disorders: A Link To Psychostimulants
Considerable overlap exists between the mechanisms influenced by psychostimulants and those involved in the pathophysiology of various movement disorders . Movement disorders affect the control of voluntary and involuntary movements and manifest as hypokinetic or hyperkinetic disorders including parkinsonism, tremor, dyskinesias, and myoclonus. Most of these disorders are either directly or indirectly related to the basal ganglia of the brain. Evidence of altered cortical function, white matter tract involvement and widespread neural network dysfunction is also becoming available.
Table 1. Examples of psychostimulants and an overview of their toxic effects mediated by monoaminergic systems.
Basal ganglia are a diverse group of interconnected nuclei that serve an important part in movement execution and the relay of the associated signals. The classical model proposes a direct and indirect pathway within basal ganglia involving subpopulations of striatal projection neurons . The circuits are activated by cortical signals and by regulating gamma aminobutyric acid release, they eventually exert an influence on dopamine-dependent signaling and thus increase or reduce locomotor activity. Selective contributions of these pathways have been verified in animals with dopamine- and cAMP-regulated phosphoprotein Mr 32 kDa loss in nigrostriatal neurons in reaction to cocaine .
Rem Sleep Behavior Disorder
In vivid dreaming states most peoples bodies are still. However people with RBD lack muscle paralysis resulting in their acting out their dreams. This can include talking, screaming, shouting, hitting, punching or kicking, even propelling them out of bed. This can be scary and dangerous if they strike their partners or other bedside objects involuntarily. RBD is common in and can begin long before the onset of declining motor function. Fortunately it is also a very treatable condition.
Also Check: Nursing Home Care For Parkinsons Patients
Also Check: On-off Phenomenon
What Is Tardive Dyskinesia
Tardive dyskinesia is a drug-induced movement disorder. Taking specific medications, often for a mental health disorder, can cause it.
Tardive dyskinesia causes involuntary facial tics . It can also cause uncontrollable movements like lip-smacking.
Tardive means delayed or late. Dyskinesia refers to involuntary muscle movements. With this condition, theres a delay between when you start a medicine and when you develop dyskinesia. Most people take a medicine for years before developing the disorder.
Vocalizations As Part Of Stereotypies
The precise definition of stereotypies and their exact phenomenological distinction from other repetitive motor behaviors, for example, tics, is difficult. The term denotes a repetitive, often continuous, non-goal-directed movement pattern that is typically distractible. As with echolalic behaviors, stereotypies are also part of physiological development that often abate within the first years of life. Although the persistence of stereotypic vocalizations may still be part of normal development, in many cases it signifies pathology, and indeed stereotypic utterances are part of the diagnostic criteria of ASD . One large case series of 83 patients with Rett syndrome described phonic stereotypies with repetitive sounds, words, or phrases in only 6% of patients. We recently observed loud stereotypic vocalizations in a patient with 15q13.3 microdeletion syndrome and late-treated cases with phenylketonuria. Further, stereotypic vocalizations have been documented in patients with schizophrenia.
Also Check: Sam Waterston Parkinson’s
Origins Of Breathing Disorders
The book by Leon Chaitow and co-authors cited above explains how breathing disorders are intrinsically linked to chronic stress and anxiety. The shallow, fast chest breathing through the mouth is a hallmark of the body preparing itself for the exertion of flight or fight due to a stress response. While this adaptive in acute stress situations, when stress is chronic and the body is spending a lot of time in fight or flight, the associated pattern of breathing becomes habitual, and eventually the system gets stuck in the new equilibrium of the CO2 intolerant state. However, the vicious circle work both ways, because overbreathing itself puts the body into a stress response state and feeds anxiety. A very good tutorial about the two way links between anxiety and breathing patterns is given by Robert Litman in the video below.
It is not surprising therefore that people with PD can present with disordered breathing associated with chronic stress and anxiety, since there are very significant overlaps between the other symptoms of chronic stress and those of Parkinsons Diseases, and ingrained fight or flight behaviours are common to the pre-diagnosis background histories of people with PD. Conversely, it is important to note that techniques which have been developed to treat breathing disorders should also help to decrease the symptoms of PD, including reduction of anxiety and increasing resilience to stress.
Recommended Reading: What Does Parkinsons Disease Do
How To Approach The Symptom
If youve experienced involuntary mouth twitches and ignored them or seen someone do the same, its best to reach for medical help immediately. You might not dwell much on it now, but PD disease symptoms keep getting worse.
What is now involuntary twitching might turn into the unintentional opening and shutting of the mouth.
Your first visit should be to a neurologist specializing in movement. They will examine you for other symptoms. They will also administer medications such as Klonopin or Valium to deal with the signs and give you some relief.
One of the most effective solutions to Dystonia, like many serious illnesses, is early detection and treatment. After that, it is pretty standard for patients to live long and healthy lives with the proper treatment.
Read Also: Adaptive Silverware For Parkinson’s
What Does Tardive Dyskinesia Look Like
TD looks like different, uncontrollable movements and patterns of the limbs and face. Sometimes referred to as stereotypy, the activity can be patterned, repetitive, and rhythmic movements that can involve one or more body parts. More than 3/4 of those with TD experience oral-facial-lingual stereotypic movements .1 The Baylor College of Medicine Movement Disorders Clinic conducted a videotape review of 100 people with tardive dyskinesia. The evaluation showed that the majority experienced irregular and chaotic movements in the OFL region, including lip smacking, chewing and other tongue and mouth movements. Other areas of the body can also show signs of TD like nodding and rocking, repeated body movements like crossing and uncrossing arms and legs, and random vocalizations.
Those who experience these involuntary movements may not even realize it. Like other conditions, these stereotypies can get worse under stress. They can manifest as muscle contractions or spasms, inability to be still, facial tics, or other jerking and abnormal movements.
How Is Tardive Dyskinesia Managed Or Treated
Your healthcare provider may gradually lower your medication dose. Eventually, you may stop the drug. If you need ongoing treatment, your healthcare provider may prescribe a different medicine.
For some people, these changes end tardive dyskinesia symptoms. You should only make medication changes under your healthcare providers care.
Some people still have symptoms despite medication changes. Over time, the symptoms may improve and go away. Rarely, symptoms become worse.
If symptoms persist, these treatments may help:
- Tetrabenazine, the only approved drug for the treatment of movement disorder symptoms.
- Botulinum toxin injections , which blocks facial nerve signals for a few months.
- Deep brain stimulation, an implantable device that blocks irregular nerve signals to areas of the brain that control movements.
Also Check: Sam Waterston Tremor
Several Treatment Options Are Available If This Happens To You
If you do notice symptoms of dystonia around your mouth or anywhere else, you should first contact a neurologist who specializes in movement disorders. They may prescribe an oral medication such as Klonopin, Valium, or Artane, which have been shown to improve involuntary movement symptoms in roughly one third of cases. Alternatively, they may recommend botulism injections, deep brain stimulation surgery, or muscle relaxants to minimize unintentional movement. The Michael J. Fox Foundation notes that physical and occupational therapy can also improve one’s outcome.
Though the diagnosis can be daunting, the Dystonia Foundation offers a message of hope to those experiencing these unsettling symptoms. “Living well with oromandibular dystonia is possible,” they write. “The early stages of symptom onset, diagnosis, and seeking effective treatment are often the most challenging.” The key is to seek medical evaluation as soon as you first notice a problem and begin treatmentâfor dystonia and Parkinson’sâas soon as possible.