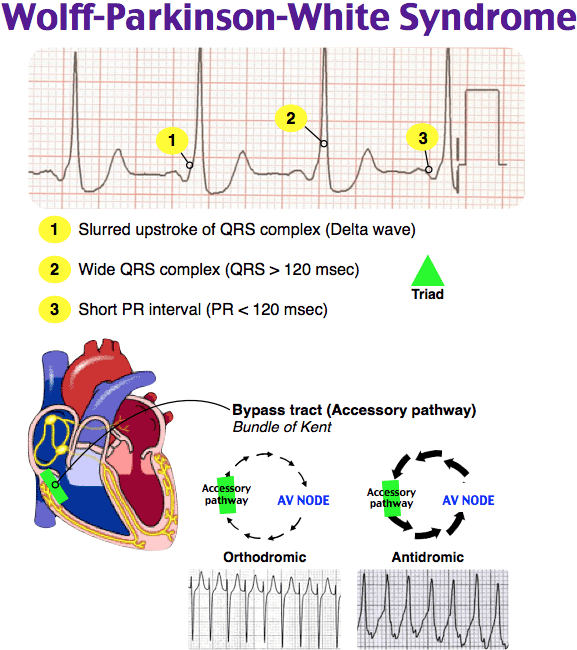
Orthodromic Svt In Wpw
In orthodromic SVT, the action potential enters the AV node, propagates down the bundle of His, depolarises the ventricles, reenters the atria via the accessory pathway, and stimulates the AV node again. As in any normal SVT, this is something that should respond well to AV nodal blockers. If you block the AV node, the reentry of the action potential will only stimulate the atria and then dissipate harmlessly against the blocked node, and propagate no further. That ends the cycle, as there will be no ventricular action potential to reenter and stimulate the atria, which means that the next pulse should be a good honest sinus beat. On the basis of this, the UpToDate boffins recommend standard anti-SVT pharmacotherapy:
The approach to patients with orthodromic AVRT is similar to patients with other types of paroxysmal supraventricular tachycardia AV nodal blocking agent should be instituted. We suggest intravenous adenosine rather than intravenous verapamil as the initial choice based on its efficacy and short half-life.
You May Like: Bicycle Therapy For Parkinsons Disease
Orthodromic Tachycardia With Concealed Accessory Pathway
Some APs are unable to conduct in an antegrade fashion. These are called concealed APs, because “manifest” preexcitation is a delta wave that is visible on a surface 12-lead ECG. They account for about 30% of all SVTs induced on EPS.
Although no evidence of the pathway is present during sinus rhythm , orthodromic tachycardias can occur. Orthodromic tachycardia may also occur when there are two or more accessory connections, and in that case, the retrograde conduction may occur through the AV node, through one of the accessory connections, or through both.
This type of SVT may be difficult to distinguish from the usual AV nodal reentrant tachycardia on a standard surface ECG. In adults, if the heart rate is higher than 200 bpm or a retrograde P wave is visible in the ST segment , a concealed AP-mediated orthodromic reentrant tachycardia may be the diagnosis. However, this determination is most accurately made with electrophysiologic studies , or if SVT terminates with a single PVC. Other differentiating factors include the following :
When To See A Doctor
Many things can cause a fast heartbeat. It’s important to get a prompt diagnosis and care. Sometimes a fast heartbeat, or heart rate, isn’t a concern. For example, the heart rate may increase with exercise.
If you feel like your heart is beating too fast, make an appointment to see a health care provider.
- Sensation of a fast or pounding heartbeat
- Difficulty breathing
- Chest pain
Also Check: Parkinson’s Double Vision
Fibrillation Auriculaire Et Syndrome De Wolff
La fibrillation auriculaire peut être particulièrement dangereuse en cas de syndrome de Wolff-Parkinson-White. La voie accessoire peut conduire les impulsions rapides vers les ventricules à un rythme beaucoup plus rapide que celui de la voie normale . Il en résulte une fréquence ventriculaire extrêmement rapide et potentiellement mortelle. Le cur est non seulement très peu efficace lorsquil bat aussi rapidement, mais ce rythme cardiaque extrêmement élevé peut également évoluer en une fibrillation ventriculaire Fibrillation ventriculaire La fibrillation ventriculaire est une série non coordonnée, potentiellement mortelle, de contractions très rapides et inefficaces des ventricules , provoquée par… en apprendre davantage , qui est mortelle si elle nest pas rapidement traitée.
Treatment Of Atrial Fibrillation And Wpw Syndrome
-
Direct-current cardioversion
The treatment of choice for Wolff-Parkinson-White syndrome is direct-current cardioversion Direct-Current Cardioversion-Defibrillation The need for treatment of arrhythmias depends on the symptoms and the seriousness of the arrhythmia. Treatment is directed at causes. If necessary, direct antiarrhythmic therapy, including antiarrhythmic read more . The usual rate-slowing drugs used in atrial fibrillation are not effective, and digoxin and the nondihydropyridine calcium channel blockers are contraindicated because they may increase the ventricular rate and cause ventricular fibrillation. If cardioversion is impossible, drugs that prolong the refractory period of the accessory connection should be used. IV procainamide or amiodarone is preferred, but any class Ia, class Ic, or class III antiarrhythmic drug Drugs for Arrhythmias The need for treatment of arrhythmias depends on the symptoms and the seriousness of the arrhythmia. Treatment is directed at causes. If necessary, direct antiarrhythmic therapy, including antiarrhythmic read more can be used.
Also Check: Yopd Life Expectancy
How To Manage Or Live With Wpw
There is no way to prevent WPW, but you can prevent complications by learning as much as you can about the disease and working closely with your cardiologist to find the best treatment. Ask your doctor to teach you how to do a Valsalva maneuver.
Here are helpful lifestyle suggestions:
-
Dont smoke.
-
Work with your doctor to keep conditions such as high cholesterol and high blood pressure under control.
-
Eat a heart-healthy diet.
How Is The Problem Treated
See supraventricular tachycardia. Patients may be treated with heart medicines to prevent episodes of SVT. In general, infants are treated until their first birthday and then the medicines can be stopped. In older children, radiofrequency ablation has become first line treatment as it is safe with high success rates.
Read Also: On-off Phenomenon
How Is Wpw Treated
Treatment depends on the type and frequency of arrhythmias, associated symptoms such as syncope, and presence of structural heart disease. Typically a physician will recommend an ablation procedure to further define the characteristics of the accessory pathway, and ultimately, to eliminate the pathway entirely.
- Observation – If you have no symptoms, you may not require treatment. Your doctor may choose to have regular follow-up without treatment.
- Medications – A variety of drugs are available to treat arrhythmias. Because everyone is different, it may take trials of several medications and doses to find the one that works best for you. It is important to know:
- The names of your medications
- What they are for
- How often and at what times to take them
Are There Different Types Of Accessory Pathways
Lown, B. The syndrome of short P-R interval, normal QRS complex and paroxysmal rapid heart action. Circulation. vol. 5. 1952 May. pp. 693-706.
James, TN. Morphology of the human atrioventricular node, with remarks pertinent to its electrophysiology. Am Heart J. vol. 62. 1961. pp. 756-71.
Lev, M, Leffler, WB, Langendorf, R. Anatomic findings in a case of ventricular preexcitation terminating in complete atrioventricular block. Circulation. vol. 34. 1966. pp. 718-33.
Murdock, CJ, Leitch, JW, Teo, WS. Characteristics of accessory pathways exhibiting decremental conduction. Am J Cardiol. vol. 67. 1991. pp. 506-10.
Ross, DL, Uther, JB. Diagnosis of concealed accessory pathways in supraventricular tachycardia. Pacing Clin Electrophysiol. vol. 7. 1984. pp. 1069-85.
Anderson, RH, Becker, AE, Brechenmacher, C. Ventricular pre-excitation: a proposed nomenclature for its substrates. Eur J Cardiol. vol. 3. 1975. pp. 27-36.
Mahaim, I, Benatt, A. Nouvelles recherches sur les connections superieures de la branche du faisceau de His-Tawara avec cloison interventriculaire. Cardiologia. vol. 1. 1937. pp. 61
Don’t Miss: Judy Woodruff Parkinson’s
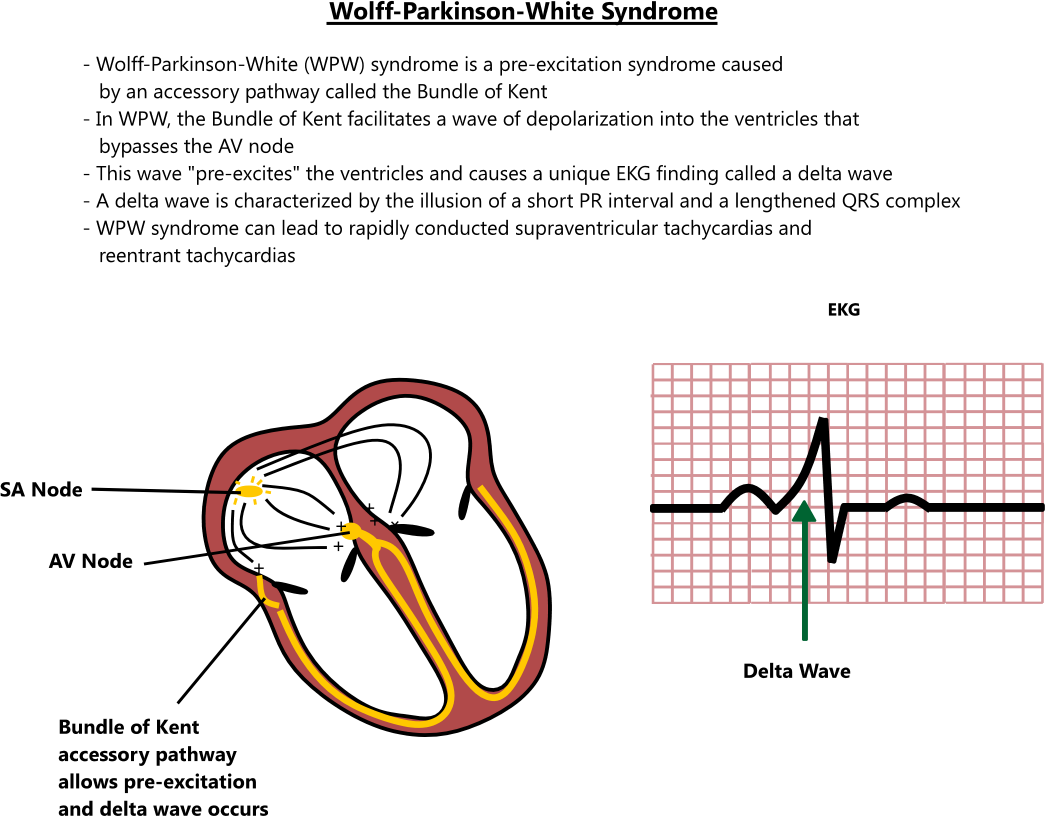
What Are The Signs And Symptoms Of Wolff
Individuals affected by Wolff-Parkinson-White syndrome can experience palpitations, rapid heart rates, difficulty breathing, and lightheadedness as well as near loss of consciousness and complete loss of consciousness. For the most part, these symptoms occur all of a sudden and are not associated with warning signs. Usually, there are no dramatic triggers, however, caffeine, alcohol, and exercise can cause the heart to start racing.
When To Seek Medical Advice
See a GP if you keep getting a fast heartbeat. It’s important to get it checked out in case it could be something serious.
Dial 999 for an ambulance if:
- your heartbeat doesn’t go back to normal in a few minutes
- you have chest pain that lasts more than 15 minutes you may also have pain in your arms, back or jaw
- you have chest pain and other symptoms like feeling sick, being sick , shortness of breath or sweating
- someone passes out and doesn’t regain consciousness
If you’ve been diagnosed with WPW syndrome and you experience an episode, first try the techniques you’ve been taught or take any medication you’ve been given.
Dial 999 or go to your nearest accident and emergency department if these measures don’t stop the episode within a few minutes, or if someone you know has WPW syndrome and collapses or faints.
Also Check: Does Sam Waterston Have Parkinsons
Traitement Du Syndrome De Wpw
-
Manuvres et médicaments pour convertir le rythme cardiaque
-
Parfois, ablation
La destruction de la voie de conduction accessoire par ablation par cathéter Destruction de tissu anormal Les troubles du rythme cardiaque sont des séquences de battements cardiaques irréguliers, trop rapides ou trop lents, ou transmis via une voie de conduction anormale à travers le… en apprendre davantage est réussie chez plus de 95 % des personnes. Le risque de décès pendant la procédure est inférieur à 1 sur 1 000. Lablation est particulièrement utile chez les jeunes qui devraient autrement prendre des anti-arythmiques à vie.
What To Expect From Your Doctor
Your health care provider is likely to ask you questions, such as:
- How severe are the symptoms?
- How often does the fast heartbeat occur?
- How long do episodes last?
- Does anything, such as exercise, stress or caffeine, seem to trigger the episodes or make symptoms worse?
- Is there a family history of tachycardia or heart disease?
You May Like: Sam Waterston Parkinson’s
What Drugs Are Contraindicated In Wpw
atrial fibrillationdigoxincalcium channel blockers
. Also question is, what medications should not be taken with WPW?
Do not give digoxin or nondihydropyridine calcium channel blockers to patients with atrial fibrillation and Wolff-Parkinson-White syndrome because these drugs may trigger ventricular fibrillation.
Also, why is digoxin contraindicated in WPW? The use of digoxin or verapamil for long-term therapy appears to be contraindicated for many patients with WPW syndrome, because these medications may enhance antegrade conduction through the AP by increasing the refractory period in the AV node.
Thereof, is adenosine contraindicated in WPW?
In the presence of WPW, traditional treatments may be contraindicated. Any AV nodal slowing agent, including adenosine, diltiazem and amiodarone, may cause an adverse reaction in the presence of WPW. Of those three medications, AHA recommends amiodarone. It is important to keep WPW in mind when treating a tachycardia.
What triggers WPW?
The extra electrical pathway that causes a rapid heartbeat is present at birth. An abnormal gene is the cause in a small percentage of people with WPW . The syndrome also is associated with some forms of congenital heart disease, such as Ebstein anomaly. Otherwise, little is known about why the extra pathway develops.
Also Check: Parkinsons Quality Of Life
Atrial Fibrillation And Wpw
Patients with Wolff-Parkinson-White syndrome have an accessory pathway or a bypass tract that connects the electrical system of the atria directly to the ventricles, thereby allowing conduction to avoid passing through the AV node.
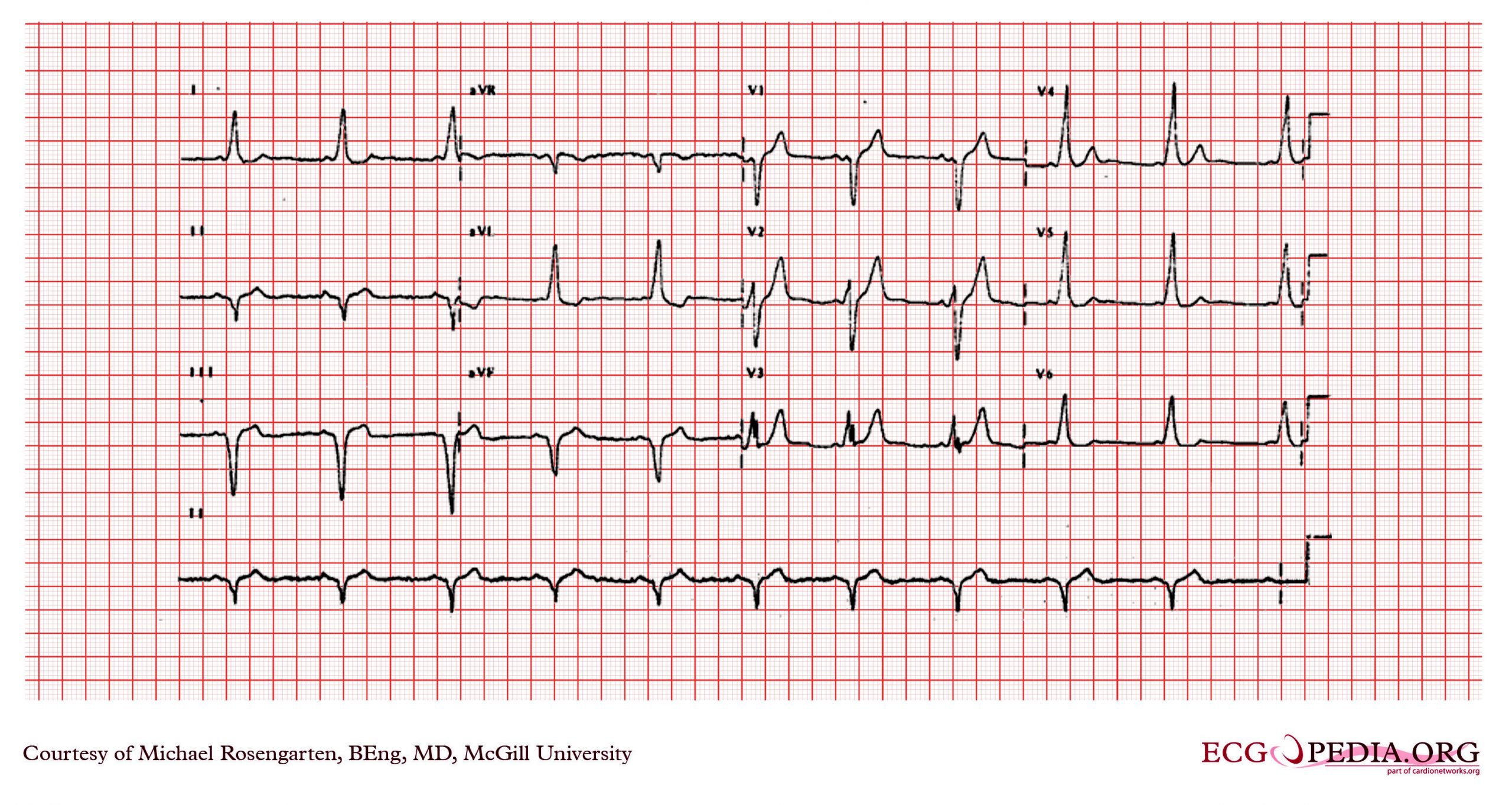
In normal individuals, when the sinus node creates an action potential it must pass through the AV node to get to the ventricles. When an accessory pathway is present, the sinus node action potential can pass through the bypass tract before the AV node, which causes the ventricles to become depolarized quickly. This is termed pre-excitation and results in a shortened PR interval on the ECG.
The combination of WPW and atrial fibrillation can potentially be fatal, especially if AV blocking agents are given . The medical treatment is procainamide, although electrical cardioversion is reasonable, especially if hemodynamically unstable.
In patients with WPW and atrial fibrillation, the erratic atrial action potentials can conduct through the accessory pathway very quickly . Therefore, WPW patients who develop atrial fibrillation have higher ventricular rates than those without WPW. If an AV blocking agent is given, fewer atrial action potentials will pass through the AV node and more will pass through the accessory pathway, paradoxically increasing the ventricular rate potentially causing ventricular fibrillation which is a fatal, hemodynamically unstable rhythm. Procainamide or electrical cardioversion is recommended in these situations.
You May Like: On Off Phenomenon
Cleveland Clinic Heart Vascular & Thoracic Institute Cardiologists And Surgeons
Choosing a doctor to treat your abnormal heart rhythm depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with Arrhythmias:
- Section of Electrophysiology and Pacing: cardiology evaluation for medical management or electrophysiology procedures or devices – Call Cardiology Appointments at toll-free 800.223.2273, extension 4-6697 or request an appointment online.
- Department of Thoracic and Cardiovascular Surgery: surgery evaluation for surgical treatment for atrial fibrillation, epicardial lead placement, and in some cases if necessary, lead and device implantation and removal. For more information, please contact us.
- You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute has specialized centers to treat certain populations of patients:
How Is It Treated
During an episode, your doctor may suggest that you try vagal manoeuvres. These are things that might help slow your heart rate. Your doctor will teach you how to do vagal manoeuvres safely. Examples include bearing down or putting an ice-cold, wet towel on your face.
Catheter ablation, a non-surgical procedure, might be used to stop the rhythm problem. This procedure can successfully eliminate WPW most of the time. There is a small risk of the arrhythmia recurring even after successful ablation of WPW. But a second session of catheter ablation is usually successful.
You might take medicine to control or prevent episodes.
Also Check: Prayer For Parkinson’s Disease
Preventing An Episode That Has Started
Your doctor can advise on ways to interrupt the abnormal electrical signals and slow down the fast heartbeats. They include actions as simple as coughing in a particular way, or applying an ice pack to your face. Only do these if your doctor recommends them. Your doctor might also recommend medication to treat an episode.
Symptmes Du Syndrome De Wpw
Le syndrome de Wolff-Parkinson-White est une cause fréquente de tachycardie paroxystique supraventriculaire Tachycardie paroxystique supraventriculaire La tachycardie paroxystique supraventriculaire est un rythme cardiaque rapide et régulier qui débute et sarrête brutalement et qui a son origine au niveau… en apprendre davantage . Très rarement, ce syndrome provoque un rythme cardiaque extrêmement rapide et potentiellement mortel pendant la fibrillation auriculaire Fibrillation auriculaire et flutter auriculaire La fibrillation et le flutter auriculaires sont des formes de décharges électriques très rapides qui entraînent une contraction très rapide des oreillettes quelques-unes… en apprendre davantage .
Si les nourrissons développent des arythmies dues à ce syndrome, ils peuvent devenir essoufflés ou léthargiques, perdre leur appétit, ou présenter des pulsations de thorax rapides et visibles. Une insuffisance cardiaque peut se développer.
Lorsque des épisodes de tachycardie paroxystique supraventriculaire due à un syndrome de Wolff-Parkinson-White surviennent chez des personnes plus âgées, ils provoquent en général plus de symptômes, comme un évanouissement, un essoufflement et une douleur thoracique.
You May Like: Pfnca Wellness Programs
Mill Hill Ave Command: Can You Give Adenosine To A
· 2) Second, there was a concern in the past that a certain percentage of wide-complex tachycardia were actually WPW with antidromic conduction, and so the advice was to avoid adenosine. The rationale was that since the bypass tract was capable of retrograde conduction, shutting down the AV node could expose the ventricles to potentially unregulated pacing.
Treatment Of Wpw Syndrome
-
Maneuvers and drugs to convert heart rhythm
-
Sometimes ablation
Destruction of the extra conduction pathway by catheter ablation Destroying abnormal tissue Abnormal heart rhythms are sequences of heartbeats that are irregular, too fast, too slow, or conducted via an abnormal electrical pathway through the heart. Heart disorders are… read more is successful in more than 95% of people. The risk of death during the procedure is less than 1 in 1,000. Ablation is particularly useful for young people who might otherwise have to take antiarrhythmic drugs for a lifetime.
Read Also: Zhichan Capsule
How Is Wpw Syndrome Treated
If youre diagnosed with WPW syndrome, you have several treatment options, depending on your symptoms. If youre diagnosed with WPW syndrome but dont have any symptoms, your doctor may recommend that you wait and continue follow-up appointments. If youre having symptoms, the treatment may include the following:
Understanding Medications Versus Catheter Ablation
Medications Versus Catheter Ablation Very often, when a patient complains of heart rhythm issues, their primary care physician or cardiologist will start them on medication to try to improve symptoms or restore normal rhythm. Medications are, after all, easy to TachycardiaTachycardia is the medical term for a heart rate over 100 beats per minute. There are many heart rhythm disorders that can cause tachycardia. Sometimes, its normal for you to have a fast heartbeat. For instance, its normal for your heart rate to rise
Don’t Miss: Cleveland Clinic Parkinson’s Bicycle Study 2017
What Are The Symptoms Of Wpw
People may first experience symptoms at any age, from infancy through adult years.
Symptoms of WPW may include one or more of the following:
- Heart palpitations a sudden pounding, fluttering or
- Racing feeling in your chest
- Dizziness feeling lightheaded or faint
- Shortness of breath
- Rarely, cardiac arrest
Some people have WPW without any symptoms at all.
How Is It Treated And Managed
Catheter ablation is the most common treatment for people who have WPW syndrome and symptoms of an arrhythmia. This procedure can cure WPW syndrome in most people. If this treatment works for you, you can go back to your normal activities.
You may need one of more of the following treatments for an irregular heartbeat:
- Medicines that can control or prevent a fast heartbeat
- Cardioversion, which uses an electrical shock to your heart to restore its rhythm
If you have no symptoms of arrhythmias, you may not need any treatment. You may need regular checkups to check for a rapid or irregular heartbeat. Tell your doctor right away if you have any symptoms.
Don’t Miss: Fitflop Shoes For Parkinson’s