What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to person, and it is not possible to predict how quickly the disease will progress.
- Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease.
- Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death.
- Many treatment options can reduce some of the symptoms and prolong the quality of life.
How Is Parkinson’s Disease Managed
Your doctors will tailor your treatment based on your individual circumstances. You will manage your condition best if you have the support of a team, which may include a general practitioner, neurologist, physiotherapist, occupational therapist, psychologist, specialist nurse and dietitian.
While there is no cure for Parkinson’s disease, symptoms can be treated with a combination of the following.
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Don’t Miss: Judy Woodruff Parkinson’s
Causes Of Parkinson’s Disease
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
Recommended Reading: Parkinson Silverware
No One Definitive Cause Of Parkinsons
There are no biomarkers or objective screening tests that indicate one has Parkinsons. That said, medical experts have shown that a constellation of factors are linked to it.
Parkinsons causes are likely a blend of genetics and environmental or other unknown factors. About 10 to 20 percent of Parkinsons disease cases are linked to a genetic cause, says Ted Dawson, M.D., Ph.D., director of the Institute for Cell Engineering at Johns Hopkins. The types are either autosomal dominant or autosomal recessive .
But that leaves the majority of Parkinsons cases as idiopathic, which means unknown. We think its probably a combination of environmental exposure to toxins or pesticides and your genetic makeup, says Dawson.
Age. The biggest risk factor for developing Parkinsons is advancing age. The average age of onset is 60.
Gender. Men are more likely to develop Parkinsons disease than women.
Genetics. Individuals with a parent or sibling who is affected have approximately two times the chance of developing Parkinsons. Theres been an enormous amount of new information about genetics and new genes identified over the past 10 or 15 years that have opened up a greater understanding of the disease, says Dawson.
What Treatments Are Available
Many Parkinson’s patients enjoy an active lifestyle and a normal life expectancy. Maintaining a healthy lifestyle by eating a balanced diet and staying physically active contributes to overall health and well-being. Parkinson’s disease can be managed with self-care, medication, and surgery.
Self careExercise is as important as medication in the treatment of PD. It helps maintain flexibility and improves balance and range of motion. Patients may want to join a support group and continue enjoyable activities to improve their quality of life. Equally important is the health and well being of the family and caregivers who are also coping with PD. For additional pointers, see Coping With Parkinsons Disease.
These are some practical tips patients can use:
Medications There are several types of medications used to manage Parkinson’s. These medications may be used alone or in combination with each other, depending if your symptoms are mild or advanced.
After a time on medication, patients may notice that each dose wears off before the next dose can be taken or erratic fluctuations in dose effect . Anti-Parkinsons drugs can cause dyskinesia, which are involuntary jerking or swaying movements that typically occur at peak dosage and are caused by an overload of dopamine medication. Sometimes dyskinesia can be more troublesome than the Parkinsons symptoms.
Recommended Reading: Parkinson’s Double Vision
Theory Of Pd Progression: Braaks Hypothesis
The current theory is that the earliest signs of Parkinson’s are found in the enteric nervous system, the medulla and the olfactory bulb, which controls sense of smell. Under this theory, Parkinson’s only progresses to the substantia nigra and cortex over time.
This theory is increasingly borne out by evidence that non-motor symptoms, such as a loss of sense of smell , sleep disorders and constipation may precede the motor features of the disease by several years. For this reason, researchers are increasingly focused on these non-motor symptoms to detect PD as early as possible and to look for ways to stop its progression.
Page reviewed by Dr. Ryan Barmore, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
Parkinson’s Disease Diet And Nutrition
Maintaining Your Weight With Parkinson’s Disease
Malnutrition and weight maintenance is often an issue for people with Parkinson’s disease. Here are some tips to help you maintain a healthy weight.
- Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily.
- If you have an unexplained weight gain or loss , contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition.
- Avoid low-fat or low-calorie products. . Use whole milk, whole milk cheese, and yogurt.
Don’t Miss: Does Sam Waterston Have Parkinsons
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Caregiving For People Living With Parkinsons
Caring for a loved one with PD can be a challenging job, especially as the disease progresses. Former caregivers of a loved one with PD suggest doing the following : Get prepared, Take care of yourself, Get help , Work to maintain a good relationship with your loved one, and Encourage the person with PD for whom you care, to stay active.
Preparing for caregiving starts with education. Reading this fact sheet is a good start. More resources are available to you in theResources section of this fact sheet. Early Parkinsonâs disease usually requires more emotional support and less hands-on care. It is a good time for family members/caregivers to educate themselves about the disease.
You May Like: Similar To Parkinsons
What Does Parkinson’s Do To The Brain
Deep down in your brain, there’s an area called the substantia nigra, which is in the basal ganglia. Some of its cells make dopamine, a chemical that carries messages around your brain. When you need to scratch an itch or kick a ball, dopamine quickly carries a message to the nerve cell that controls that movement.
When that system is working well, your body moves smoothly and evenly. But when you have Parkinson’s, the cells of your substantia nigra start to die. There’s no replacing them, so your dopamine levels drop and you can’t fire off as many messages to control smooth body movements.
Early on, you won’t notice anything different. But as more and more cells die, you reach a tipping point where you start to have symptoms.
That may not be until 80% of the cells are gone, which is why you can have Parkinson’s for quite a while before you realize it.
The Substantia Nigra And Movement
The reason that Parkinsons causes movement symptoms is that the substantia nigra makes up part of the circuitry, called the basal ganglia, that the brain uses to turn thought about movement into action.
The structures of the basal ganglia.
The substantia nigra is the master regulator of the circuit, it mainly communicates using the chemical dopamine, but other chemical transmitters are also used to communicate between other areas of the basal ganglia.
The balance of signals being sent between these structures allows us to control movement. But as Parkinsons progresses, and the dopamine-producing brain cells in the substantia nigra are lost, movement symptoms appear. Without enough dopamine, it becomes harder to start and maintain movements, which leads to symptoms such as slowness of movement, rigidity and freezing. And an imbalance of signals in the basal ganglia means people with Parkinsons can experience what is known as a resting tremor.
But while this is the description of Parkinsons you may find in most textbooks, it is now recognised that changes are not limited to the substantia nigra and basal ganglia.
Don’t Miss: Sam Waterston Tremor
What Causes Parkinson’s Disease
A substance called dopamine acts as a messenger between two brain areas – the substantia nigra and the corpus striatum – to produce smooth, controlled movements. Most of the movement-related symptoms of Parkinson’s disease are caused by a lack of dopamine due to the loss of dopamine-producing cells in the substantia nigra. When the amount of dopamine is too low, communication between the substantia nigra and corpus striatum becomes ineffective, and movement becomes impaired the greater the loss of dopamine, the worse the movement-related symptoms. Other cells in the brain also degenerate to some degree and may contribute to non-movement-related symptoms of Parkinson’s disease.
Although it is well known that lack of dopamine causes the motor symptoms of Parkinson’s disease, it is not clear why the dopamine-producing brain cells deteriorate.
- Genetic and pathological studies have revealed that various dysfunctional cellular processes, inflammation, and stress can all contribute to cell damage.
- In addition, abnormal clumps called Lewy bodies, which contain the protein alpha-synuclein, are found in many brain cells of individuals with Parkinson’s disease. The function of these clumps in regards to Parkinson’s disease is not understood.
In general, scientists suspect that dopamine loss is due to a combination of genetic and environmental factors.
Where Does Parkinson’s Disease Start In The Brain Or Gut Or Both
- Date:
- IOS Press
- Summary:
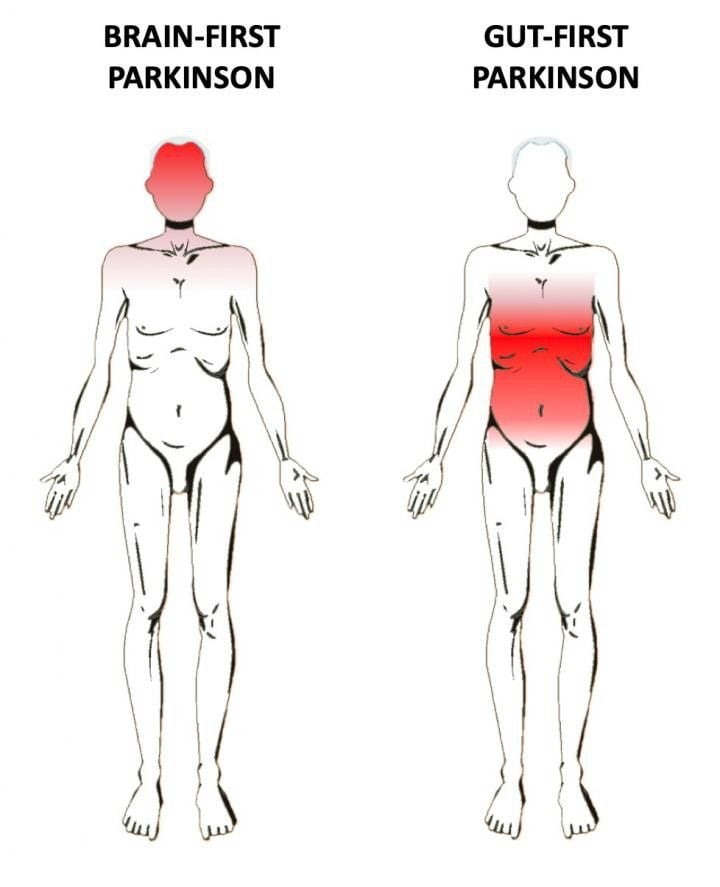
- Does Parkinson’s disease start in the brain or the gut? In a new contribution, scientists hypothesize that PD can be divided into two subtypes: gut-first, originating in the peripheral nervous system of the gut and spreading to the brain and brain-first, originating in the brain, or entering the brain via the olfactory system, and spreading to the brainstem and peripheral nervous system.
Does Parkinson’s disease start in the brain or the gut? In a new contribution published in the Journal of Parkinson’s Disease, scientists hypothesize that PD can be divided into two subtypes: gut-first, originating in the peripheral nervous system of the gut and spreading to the brain and brain-first, originating in the brain, or entering the brain via the olfactory system, and spreading to the brainstem and peripheral nervous system.
“The discussion about the origins of PD is often framed as an ‘either-or’, i.e., either all PD cases start in the gut or all cases start in the brain,” added Dr. Van Den Berge. “However, much of the evidence seems compatible with both these interpretations. Thus, we need to entertain the possibility that both scenarios are actually true.”
“If the brain-first vs body-first hypothesis is correct, we need to intensify the research into understanding risk factors and triggering factors for these two subtypes,” noted Dr. Van Den Berge.
You May Like: Yopd Life Expectancy
Surgery And Deep Brain Stimulation
Deep brain stimulation is a treatment for Parkinsonâs disease that uses an implantable pacemaker-like device to deliver electrical pulses to parts of the brain involved in movement. The DBS system consists of leads precisely inserted into a specific brain target, the neurostimulator implanted in the chest, and extension wires that connect the leads to the neurostimulator. Though implantation of the system requires a neurosurgical procedure, the treatment itself consists of long-term electrical stimulation. Advantages of DBS include its ability to reduce the high doses of medications , its adjustability , and its reversibility DBS was approved by the Food and Drug Administration as a treatment for PD in 2002 and according to Medtronic , more than 80,000 patients have undergone DBS surgery worldwide.
Typical candidates are those who have motor fluctuations or periods of âoffâ time with troublesome symptoms alternating with periods of âonâ time with good symptom control, and also with possible periods of excessive movement .
Not all patients with Parkinsonâs disease are good candidates for treatment with DBS. Approximately 10â20% of patients considered for possible treatment with DBS include those:
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Recommended Reading: On Off Phenomenon
Does Parkinsons Start In The Nose International Team Awarded Us$9 Million Asap Grant To Find Out
We will test the idea that certain environmental triggers, such as viruses, may be able to start a chain reaction in the odor-sensing cells in the nose,” says Dr. Michael Schlossmacher, professor at uOttawa’s Brain and Mind Research Institute.
More than 80 percent of people with Parkinsons disease suffer from a reduced sense of smell, something that often occurs years before the onset of typical movement-related symptoms. Now, thanks to a US$9 million grant from the Aligning Science Across Parkinsons initiative, a Canadian-led international team hopes to determine whether scent-processing nerves that connect the inside of the nose to the brain may play a role in the development of Parkinson disease.
While current treatments can help control some symptoms of Parkinsons, we cant stop this disease or even slow it down, said team leader Dr. Michael Schlossmacher, a neurologist and Bhargava Family Research Chair in Neurodegeneration at The Ottawa Hospital. This grant will allow us to explore an understudied but important aspect of Parkinsons, which could lead to new approaches for early treatment and prevention.
The team, which includes researchers from Germany and the United States in addition to Canada, will investigate possible links between environmental exposures in the nasal cavity, inflammation, odor processing centres in the brain and Parkinsons-related genes, in both animal models and people.
Media contact
Tips For Caring For Someone With Parkinsons Disease
Caring for a loved one with early onset Parkinsons can be difficult. If youre a caregiver for someone with this condition, its important that you remember your own emotional and physical health.
Not only are you dealing with a difficult diagnosis, youre also managing an increased number of responsibilities. Burnout is common in caregivers, so make sure youre checking in with your own needs.
The Michael J. Fox Foundation Center for Parkinsons Research recommends these tips for caregivers:
Don’t Miss: Weighted Silverware
What Is Parkinson’s Disease
Parkinson’s disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinson’s disease and the degree of impairment varies from person to person. Many people with Parkinson’s disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinson’s disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinson’s disease will increase in the future. Adult-onset Parkinson’s disease is most common, but early-onset Parkinson’s disease , and juvenile-onset Parkinson’s disease can occur.