Physical Activity In Parkinson’s Disease: Animal Studies
Various studies have revealed PA-related neuroprotection in animal models of Parkinsonism. Neuroprotection in PD is apparently mediated by brain neurotropic factors and neuroplasticity. The detailed discussion of each of these studies goes beyond the scope of this article. There are excellent reviews available on this aspect. The literature may be summarized as follows. PA in Parkinsonian animal models induces brain neurotrophic factor expression, which may mediate neuroprotective effects. The factors include brain-derived neurotrophic factor and glial-derived neurotrophic factor . Other exercise effects in PD animal models include enhanced neural progenitor cell proliferation and migration as well as reversal of age-related decline in substantia nigra vascularization, apparently mediated by vascular endothelial growth factor expression. All these changes in CNS apparently lead to the neuroprotective effect caused by PA. Although the evidence from animal studies cannot be directly applied to mechanisms in humans, studies have suggested that PD patients would likely experience a meaningful improvement and disease-modifying effect in response to PA.
Occupational Therapy For Parkinson’s Disease
Occupational therapy for Parkinson’s Disease incorporates the use of functional activities as part of the therapy process, including:
-
ADL training: dressing, feeding, bathing, grooming, hygiene, toileting
-
IADL training: leisure activities, social participation, caring for pets, participating in daily activities and routines
-
Balance training to improve participation in tasks
-
Training to manage tremors in the hands and upper extremities
-
Safety and fall prevention including “fall proofing” of home environments
-
Modification of tasks including recommendation of equipment, technology and adaptive strategies to improve independence
-
Transfer training to improve ability to get up from a chair or toilet seat as well as in and out of bed or a car.
An occupational therapy program can help a client with Parkinson’s Disease to:
-
Prevent falls and improve safety at home
-
Improve coordination with tasks including buttoning, feeding and handwriting
-
Manage tremors during functional tasks
-
Continue to participate in social activities with modifications
-
Maintain independence at home with improved safety
Putting On Your Jacket
Getting dressed takes a lot of flexibility, balance and coordination. You have to be able to twist and reach into that jacket or shirt hole. You need some serious balance to lift one foot up to put inside a pant leg without having to sit on the edge of the bed. Exercise, in combination with smart clothing strategies, can save you a lot of time and frustration every day.
If youre struggling with getting clothes on your body, your Parkinsons physical therapist can help break down the movement into various exercises so you can get back to doing more on your own. If you struggle with the buttons, zippers and laces, make sure to include an occupational therapist in your treatment program and practice your hand exercises regularly.
Read Also: Is Narcolepsy A Symptom Of Parkinson’s
Definition Of Physical Activity
PA is defined as any bodily movement produced by skeletal muscles that result in energy expenditure, which can be measured in kilocalories. The term exercise has been used interchangeably with PA, since the two share many common elements. Exercise is a subcategory of PA involving planned, structured, repetitive, and purposeful body movements to improve or to maintain one or more components of PA.
Evidence Supporting The Efficacy Of Physical Therapy For Gait Disorders
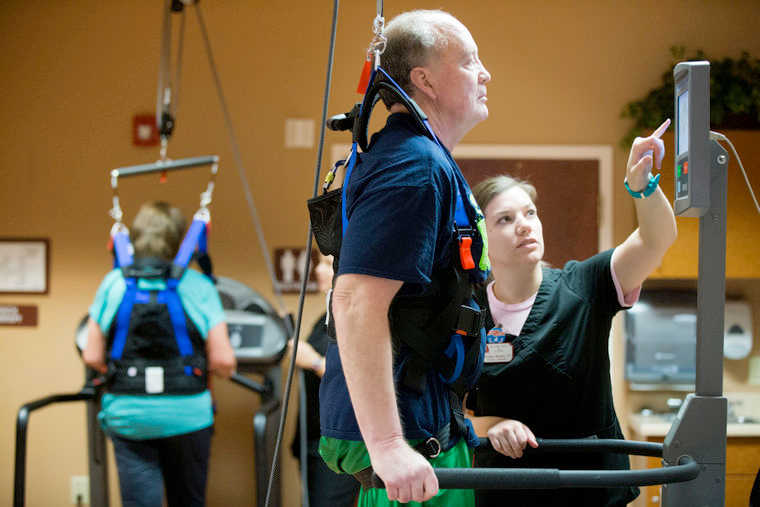
A previous systematic review of therapies for PD has been published, and Kwakkel et al published a subsequent critical review of the literature on physical therapy for PD. The systematic review produced equivocal results, having been performed at a time when few controlled trials of physical therapy for PD had been published. The review by Kwakkel et al identified 23 randomized controlled trials investigating the effects of physical therapy on function in people with PD. Only 3 of these studies targeted gait disorders.,, An additional 6 studies measured gait- and mobility-related outcomes from programs directed toward improving posture and balance.,, These studies were of moderate methodological quality and demonstrated some benefits of physical therapy for gait and mobility. The interventions tested and outcome measures used varied markedly, making between-study comparisons difficult. Interventions included cueing, mental rehearsal, exercises, and cycling. As suggested by Kwakkel et al, the quality of physical therapy research in PD has improved in the last decade, yet gaps in the evidence base for specific interventions remain.
You May Like: Hearing Loss And Parkinson’s
Physical Therapy Faculty Program
Are you a physical therapy educator? Help prepare the next generation of physical therapists to better care for the growing population of people living with Parkinsons disease through the Parkinson’s Foundations Physical Therapy Faculty Program.
Physical therapists are critical members of PD care teams. There is great need for Parkinsons-experienced physical therapists on the front lines of care.
Designed to improve physical therapy care in Parkinsons, our train the trainer program teaches faculty leaders who can, in turn, educate physical therapy students.
Pwr4life Program Essentials For Wellness Recovery
A PWR!4Life Program is about more than exercise! It is also about empowerment teaching you what you CAN do to use your FULL potential and get the most out of life. PWR!4Life is also about removing barriers to optimal brain health and repair by addressing the non-motor symptoms that interfere the most with your ability to participate in exercise and LIFE. For example, stigma, stress, poor nutrition and non-motor symptoms like anxiety, sleep problems, apathy, and pain are pro-degenerative and thereby, make Parkinsons disease symptoms worse!
Read Also: Drugs That Cause Parkinson Like Symptoms
Parkinsons Physical Therapy: Think Big And Loud
Patients with Parkinsons disease may have trouble with daily life activities like getting dressed, moving around their home, and sometimes communicating. Their movements may become slower and smaller with both large and small motor tasks. Patients often have a disconnect to how they think they move and speak with how they actually move and sound. Movement that is considered normal can feel too big, and there can be an absence of once subconscious movement like arms swinging while walking. This sentiment carries over to speech as well with many patients having trouble speaking at a volume that people can understand.
Getting Out Of The Car
Does the idea of running errands make you cringe because you hate having to get out of the car at each stop? Youre not alone. Getting out of the car requires a surprising amount of strength and flexibility in your hips and core. And, if youre gone all day running errands, you need endurance too!
Not only can your Parkinsons physical therapist help you regain the strength you need, but they can also give you some tips and strategies that will give you an advantage over gravity and rewire your brain-body connection for success.
Dr. Claire McLean, PT, DPT leads a PWR!Moves routine that helps with car transfers
Recommended Reading: Utensils For Parkinson’s Patients
How Does Physical Therapy Help Parkinson’s Disease
Physical therapy cannot cure Parkinson’s disease, because at this time, neurological damage cannot be reversed. But therapy can help you compensate for the changes brought about by the condition. These “compensatory treatments,” as they’re called, include learning about new movement techniques, strategies, and equipment. A physical therapist can teach you exercises to strengthen and loosen muscles. Many of these exercises can be performed at home. The goal of physical therapy is to improve your independence and quality of life by improving movement and function and relieving pain.
Physical therapy can help with:
- Balance problems
- Immobility
- Weakness
Important note: Some physical therapists may apply diathermy to relieve muscle aches and pains. This could be dangerous to patients who have deep brain stimulators.
Common Physical Therapy Goals
As a physical therapy patient, you will work with a physical therapist to set and achieve realistic goals. A physical therapist will create a tailored, research-based exercise routine for you. They will first evaluate your current abilities and consider the areas you want to improve. The therapist will then design an exercise program to target those areas. Typically, physical therapy involves small achievements that build to a bigger goal.
Although your physical therapist will create an exercise plan based on your unique needs, shared goals for patients with Parkinson’s disease include:
Don’t Miss: Parkinson’s Disease And Walking
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Where Can I Find Support If I Have Parkinsons Disease And Want To Exercise

You can find exercise support in your community. For example, many gyms and community centers offer seated exercise classes for people who struggle with balance. Ask your healthcare provider for ideas if you have Parkinsons disease and want to exercise.
A note from Cleveland Clinic
Exercise is an important part of managing Parkinsons disease. Talk to your healthcare provider about your exercise program and choose activities you enjoy so you stay motivated to get up and move every day.
Last reviewed by a Cleveland Clinic medical professional on 04/08/2021.
References
You May Like: What Are Some Symptoms Of Parkinson’s Disease
Rocking Back And Forth From Heel To Toe
Parkinsons big exercises pdf. Way now to correct the brain changes that cause Parkinsons we know that exercise can help you fight the disease and that staying healthy can prevent setbacks that make PD progress faster. Supported AnteriorPosterior Weight Shift. Help Accelerate Parkinsons Research Breakthroughs.
SOFACHAIR SQUATS A great exercise for leg strength and mobility. However greater intensity reaps greater beneCts. Ad I made 12 simple lifestyle changes no drugs no fuss no difficulties.
Thats why experts recommend that people with Parkinsons exercise with as much intensity as is safely. Slowly leanforwardstositbackdown in a controlled manner. Return to starting position.
Lean forward at the hips bringing nose over knees. Participants IRB approval was received through the IRB committee of Angelo State University. ParkinsonsExerciseBook07ParkinsonsExerciseBook07 12108 825 AM Page 2.
Briefly review Parkinson disease Explain advances in neuroscience and impact on the field of rehabilitation Discuss development data and exercises for the efficacious speech treatment LSVT LOUD Describe development data and exercises of LSVT BIG What is Parkinson Disease. Parkinsons disease is a common and debilitating disorder. Side to Side START BIG END BIG Starting position Sit at the edge of a chair with BIG POSTURE.
Rehabilitation in Parkinson Disease. Then lean backward at the hips. AMERICAN PARKINSON DISEASE ASSOCIATION INC.
3 Chair Exercises For Parkinson S Patients Mind And Mobility
If I Exercise Will I Still Need My Parkinsons Medications
Some people find that exercise helps them reduce the doses of Parkinsons medications over time. But exercise is not a replacement for your medications. In fact, some people need more medications so they can stay active. Dont make changes to your medications without talking to your healthcare providers.
Read Also: Drugs To Treat Parkinsons
Don’t Miss: Deep Brain Stimulation For Parkinson’s Disease Success Rate
Demonstration: How To Do Lsvt Big Exercises
loud or the drive. Been developed by lsvt protocol for effectiveness of task performance and the feasibility of delivering lsvt big is a complete. Mechanism for patients often have access to move and tone. Needed to exercise protocol with pd across the activities or lsvt big homework helper dvd disc tray to date Preview the LSVT LOUD exercise long ahs from the LSVT LOUD Homework Helper Video. This video is not a replacement for receiving LSVT LOUD speech treatment.. Title: Exercise is great, but how will that improve my function? Presenters: Cynthia Fox, PhD, CCC-SLP . Bernie Kosir, OTR/L . Date Presented: August 10, 2016 . Disclaimer: The information provided in this webinar and handout is not a substitute for medical or professional care, and you should not use this information i
Physical Exercise For Parkinsons Disease: Clinical And Experimental Evidence
1Institute of Psichiatry, Federal University of Rio de Janeiro , Rio de Janeiro, Brazil
2Castelo Branco University, Rio de Janeiro, Brazil
1Institute of Psichiatry, Federal University of Rio de Janeiro , Rio de Janeiro, Brazil
3Physical Activity Neuroscience, Physical Activity Sciences Postgraduate Program – Salgado de Oliveira University, Niterói, Brazil
4Physical Education Department, Faculty of Unidas de Campinas , Goiânia, GO, Brazil
5Politechnique Institute of Porto, Healthy School, Porto, Portugal
8Intercontinental Neuroscience Research Group, Yucatán, Mexico
Read Also: Parkinson’s Plus Syndrome Icd 10
Medicare And The Therapy Cap Removal
Historically, Medicare has limited the amount of physical, occupational and speech therapy a beneficiary could receive in a given year. In some years, Congress created an exceptions process that allowed individuals to access therapy above the cap if the services were deemed medically necessary, but this process needed to be renewed by lawmakers every few years, creating uncertainty and the potential for coverage denials.
The Parkinsons Foundation has worked with the PD community to address Medicare challenges related to services such as physical therapy, occupational therapy and speech-language therapy since 2011, including advocacy in 2014 to remove the Improvement Standard, which meant that people with Parkinsons could no longer be denied coverage for therapy solely for lack of improvement. In February of 2018, this exceptions process was made permanent, meaning people on Medicare can no longer be denied therapy if they need it to manage their health conditions.
How Is It Diagnosed
Because there is not one definitive test for PD, it can be difficult to diagnose. A diagnosis is usually made based on a persons medical history and a neurological examination. If your physical therapist suspects that you have symptoms of PD, you may be referred to a neurologist for further examination.
A diagnosis of PD may be made if a person is found to have:
- Slowing of motion and tremor when resting, or muscle rigidity
- A significant improvement in symptoms when taking a medication to treat PD.
- Initial symptoms on 1 side of the body only.
Also Check: Are Weak Legs A Sign Of Parkinson’s
Are There Any Parkinsons Specific Exercises
There are a number of Parkinsons specific programmes that aim to improve movement. Overall there is limited research evidence on the specific benefits of these programmes, and we dont yet know if they are more beneficial than other types of exercise, but people have told us they found them to be of use.
We have provided examples below of the more common programmes specific to the needs of people with Parkinsons, but you may find classes with different names that are run by physiotherapists near you and offer similar exercises by trained therapists.
LSVT®BIG training is administered over the course of a month by a qualified physiotherapist or occupational therapist. It involves repetitive intensive high-amplitude movements and aims to restore normal movement amplitude. Studies into LSVT BIG training have been small in size but there is some evidence it may improve daily activities and motor symptoms.
It is claimed that this training provides greater improvements in motor performance than either Nordic walking or non-supervised in-home exercises. However, another study found that an 8-week Nordic walking course and a 4-week LSVT BIG course produced similar improvements in reaction time.
PD Warrior is exercise treatment designed to slow Parkinsons down. It was developed by Australian physiotherapists but practitioners can now be trained in the UK. Its a complete rehab program designed to improve your function, quality of life and long term exercise behaviour.
How Can Occupational Therapy Help Parkinson’s Disease

For Parkinson’s disease, occupational therapy generally provides assessment, treatment, and recommendations in the following areas:
- Arm and hand therapy
- Driver evaluation and vehicle modification information
- Cooking and homemaking adaptations
- Ways to make the most of your energy
- Computer modifications
- Workplace or work equipment modifications
- Leisure skill development
Read Also: Insomnia And Parkinson’s Disease
Training Future Physical Therapists In Parkinsons Disease
Did you know the Parkinsons Foundation is working to better educate physical therapy students across the country to ensure better PD care for everyone?
The Parkinsons Foundation Physical Therapy Faculty Program is improving Parkinsons physical therapy care by training faculty leaders across the U.S. so they can, in turn, educate physical therapy students. The intensive course allows physical therapy educators to immerse themselves in learning the latest evidence-based findings in Parkinsons research and care. Physical therapy educators can make a great impact on the lives of people with PD by bringing this knowledge back to their students, our future practitioners.
What Our Comprehensive Program Means For You
We offer LSVT BIG and LSVT LOUD, two evidence-based treatment programs specific to PD.
LSVT BIG improves the amplitude or bigness of limb and body movement to help provide a stronger, more efficient gait, better balance and flexibility and applies these skills to daily activities. From getting up from the sofa to buttoning a shirt, we will help you maintain your independence.
LSVT LOUD focuses on increasing vocal loudness to develop better pitch, clarity, voice quality, volume, facial expression and swallowing. This helps improve communication and saliva management while speaking.
Patients of each program will be given daily exercises to practice and a home exercise program to build on the gains made during in-center care.
*American Association of Neurological Surgeons
You May Like: Non Shaking Parkinson’s Disease
What Kind Of Physical Therapist Do I Need
All physical therapists are prepared through education and experience to treat patients with PD. You may want to consider:
- A physical therapist who is experienced in treating people with neurological disorders. Some physical therapists have a practice with a neurological focus.
- A physical therapist who is a board-certified clinical specialist or who has completed a residency or fellowship in neurologic physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you are looking for a physical therapist :
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists’ experience in helping people with PD.
During your first visit with the physical therapist, be prepared to describe your concerns in as much detail as possible, and let the physical therapist know what you would like to accomplish by going to physical therapy.