How Is Parkinson’s Disease Diagnosed
Someone with the symptoms of Parkinson’s disease may be sent to see a neurologist, a doctor who specializes in the brain, nerves, and muscles. The neurologist may do some tests, including a brain scan and blood tests. These tests will not make the diagnosis of Parkinson’s disease, but the doctor will want to make sure that there is no other problem causing the symptoms. To diagnose Parkinson’s disease, the doctor relies on a person’s medical history, symptoms, and a physical exam.
Living Well With Parkinson’s
While medication and DBS surgery are the most effective treatments for PD, individuals often choose to delay these treatments because of their adverse side effects. Until a therapy is developed that can halt the progression of PD, there is a significant need for strategies that provide symptom relief without causing negative side effects.
Diet, Exercise, and Stress Reduction
Findings from several studies suggest that exercise has the potential to provide relief from certain PD symptoms. Anecdotally, people with Parkinsons disease who exercise typically do better. However, many questions remain. Among them is whether exercise provides a conditioning effect by strengthening muscles and improving flexibility or whether it has a direct effect on the brain.
In an NINDS-funded trial comparing the benefits of tai chi, resistance training, and stretching, tai chi was found to reduce balance impairments in people with mild-to-moderate PD. People in the tai chi group also experienced significantly fewer falls and greater improvements in their functional capacity.
Technologies that Improve Quality of Life
So What Do We Know So Far
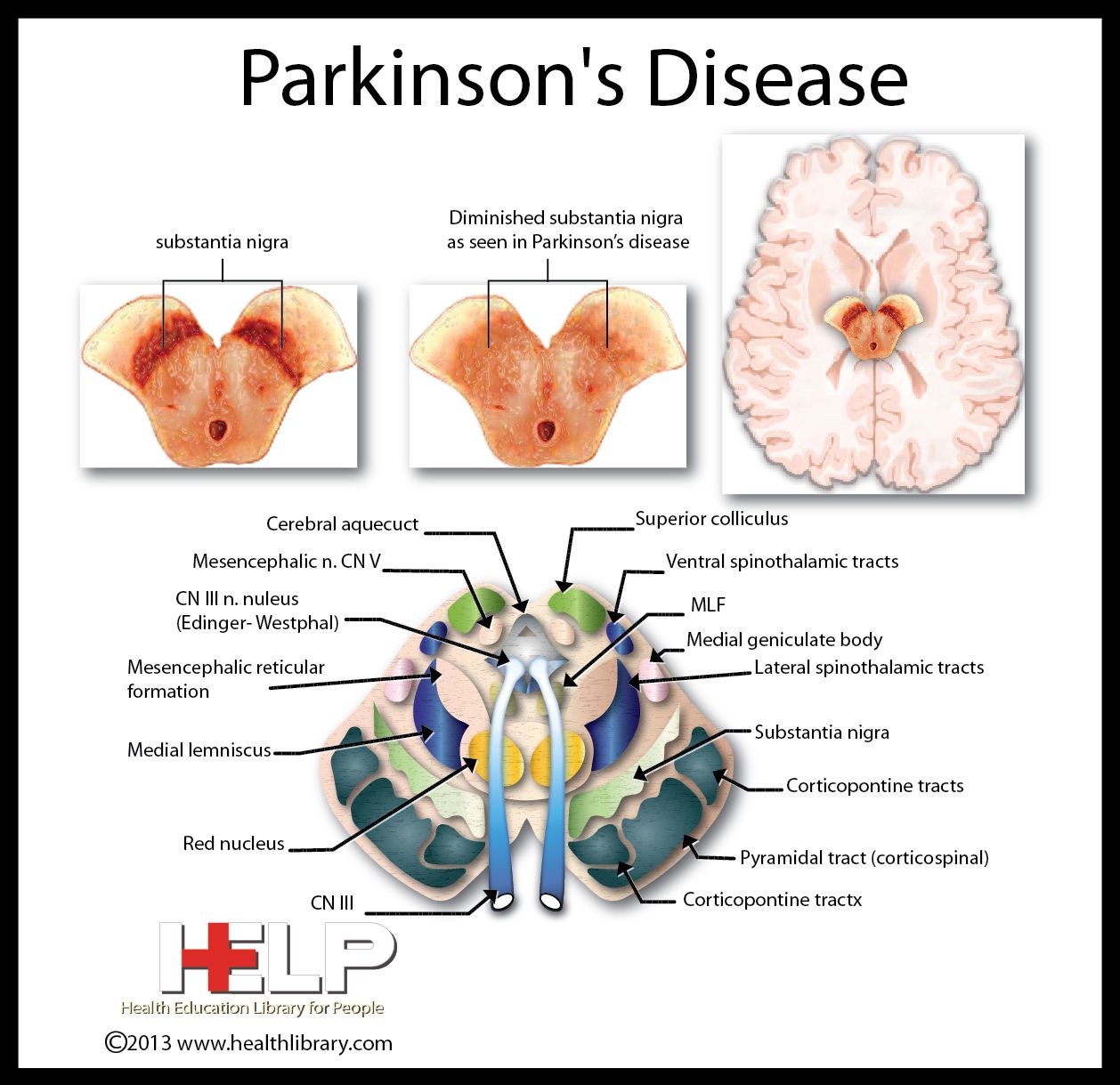
Location of the substantia nigra. FrozenManCC BY-SA 4.0
The substantia nigra is an area of the mid brain located at the top of the spinal cord, which has been the focus of much work into how Parkinsons affects the brain.
There are a right and a left substantia nigra, and often one side is affected before the other. Because of this, people with Parkinsons often experience symptoms primarily on one side of their body, particularly in the early stages. Indeed, this common feature of the condition often helps to distinguish Parkinsons from other similar conditions.
When it comes to confirming a diagnosis, it is the substantia nigra where pathologists look for changes at the end of life in brain tissue that has been donated to research. And the loss of the dopamine-producing cells in this area of the brain, accompanied by the presence of clumps of alpha-synuclein protein , has been the hallmark of Parkinsons for decades.
You can read more about the alpha-synuclein protein, and how it plays a role in the spread of Parkinsons, in a previous blog post:
Recommended Reading: Parkinson’s Disease And Vision
How Parkinsons Disease Affects The Autonomic Nervous System And The Heart
In PD, there are two major reasons why the automatic control of the cardiac system is impaired. First, areas of the brain that control this system often contain Lewy bodies and have undergone neurodegeneration. In addition, the autonomic nervous system itself is directly affected by Lewy body-like accumulations and neurodegeneration. This means, when the baroreceptors in the heart and carotid artery sense a drop in blood pressure and try to generate a signal to the heart and blood vessels to increase the blood pressure, the message may not get through. This results in neurogenic orthostatic hypotension , or drops in blood pressure upon standing due to autonomic nervous system dysfunction. There are no medications that can cure nOH by restoring the autonomic nervous system in PD. nOH however, can be treated. Read more about nOH and its treatments here.
Structural problems of the heart such as coronary artery disease or cardiomyopathy are not thought to be part of the pathology of PD, although of course, could co-exist with PD.
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
Also Check: Parkinson’s Staring Into Space
What Is Parkinson’s Disease
Parkinsons disease is a degenerative, progressive disorder that affects nerve cells in deep parts of the brain called the basal ganglia and the substantia nigra. Nerve cells in the substantia nigra produce the neurotransmitter dopamine and are responsible for relaying messages that plan and control body movement. For reasons not yet understood, the dopamine-producing nerve cells of the substantia nigra begin to die off in some individuals. When 80 percent of dopamine is lost, PD symptoms such as tremor, slowness of movement, stiffness, and balance problems occur.
Body movement is controlled by a complex chain of decisions involving inter-connected groups of nerve cells called ganglia. Information comes to a central area of the brain called the striatum, which works with the substantia nigra to send impulses back and forth from the spinal cord to the brain. The basal ganglia and cerebellum are responsible for ensuring that movement is carried out in a smooth, fluid manner .
The action of dopamine is opposed by another neurotransmitter called acetylcholine. In PD the nerve cells that produce dopamine are dying. The PD symptoms of tremor and stiffness occur when the nerve cells fire and there isn’t enough dopamine to transmit messages. High levels of glutamate, another neurotransmitter, also appear in PD as the body tries to compensate for the lack of dopamine.
Dural Lymphatic Vasculature: A New Player In The Pathophysiology Of Parkinsons Disease
Many researchers are drawn to studying the brain because theyre still making basic discoveries about how this mysterious organ works. One of those recent discoveries may be key to deciphering the causes of Parkinsons disease.
Most organs in the body have a lymphatic system to drain toxins, waste and other unwanted materials. After long believing it did not exist, researchers have realized the brain, too, has a lymphatic system to do this cleansing work.
At Toronto Western Hospital, Scientific Associate Naomi Visanji, a neuroscientist, immediately saw the implications of this discovery. Shes investigating the lymph vessels in the brain to see if they door coulddrain alpha-synuclein, a protein that accumulates in the brain cells critical to Parkinsons disease. That accumulation kills the brain cells producing dopamine, the chemical that signals other cells to initiate movement.
Because lymph vessels are involved in drainage of fluid, waste and other unwanted material, its a natural idea that the vessels might be involved in the drainage of excess toxic proteins in the brain, says Visanji.
Using imaging equipment, Visanji will compare the brains of two mouse models. One has been genetically engineered to remove its lymphatic vessels in the brain the other is a normal mouse.
The next questionrequiring a further studyis whether these vessels are damaged in people with Parkinsons disease.
Search
Recommended Reading: Parkinson’s Phase 3 Trials
What Are The Symptoms Of Parkinson Disease
Parkinson disease symptoms usually start out mild, and then progressively get much worse. The first signs are often so subtle that many people don’t seek medical attention at first. These are common symptoms of Parkinson disease:
- Tremors that affect the face and jaw, legs, arms, and hands
- Slow, stiff walking
How Is Parkinsons Disease Treated
There is no cure for Parkinsons disease. However, medications and other treatments can help relieve some of your symptoms. Exercise can help your Parkinsons symptoms significantly. In addition, physical therapy, occupational therapy and speech-language therapy can help with walking and balance problems, eating and swallowing challenges and speech problems. Surgery is an option for some patients.
Also Check: What Causes Tremors Besides Parkinson’s
Medicines For Parkinson’s Disease
Medicines prescribed for Parkinson’s include:
- Drugs that increase the level of dopamine in the brain
- Drugs that affect other brain chemicals in the body
- Drugs that help control nonmotor symptoms
The main therapy for Parkinson’s is levodopa, also called L-dopa. Nerve cells use levodopa to make dopamine to replenish the brain’s dwindling supply. Usually, people take levodopa along with another medication called carbidopa. Carbidopa prevents or reduces some of the side effects of levodopa therapysuch as nausea, vomiting, low blood pressure, and restlessnessand reduces the amount of levodopa needed to improve symptoms.
People with Parkinson’s should never stop taking levodopa without telling their doctor. Suddenly stopping the drug may have serious side effects, such as being unable to move or having difficulty breathing.
Other medicines used to treat Parkinsons symptoms include:
- Dopamine agonists to mimic the role of dopamine in the brain
- MAO-B inhibitors to slow down an enzyme that breaks down dopamine in the brain
- COMT inhibitors to help break down dopamine
- Amantadine, an old antiviral drug, to reduce involuntary movements
- Anticholinergic drugs to reduce tremors and muscle rigidity
Pathophysiology Of Parkinsons Disease
Although we are learning more each day about the pathophysiology of Parkinsons disease, it is still considered largely idiopathic . It likely involves the interaction of host susceptibility and environmental factors. A small percentage of cases are genetically linked and genetic factors are being intensely studied.
Physiologically, the symptoms associated with Parkinsons disease are the result of the loss of a number of neurotransmitters, most notably dopamine. Symptoms worsen over time as more and more of the cells affected by the disease are lost. The course of the disease is highly variable, with some patients exhibiting very few symptoms as they age and others whose symptoms progress rapidly.
Parkinsons is increasingly seen as a complex neurodegenerative disease with a sequence of progression. There is strong evidence that it first affects the dorsal motor nucleus of the vagus nerve and the olfactory bulbs and nucleus, then the locus coeruleus, and eventually the substantia nigra. Cortical areas of the brain are affected at a later stage. Damage to these various neuronal systems account for the multi-faceted pathophysiologic changes that cause impairments not just to the motor system but also to the cognitive and neuropsychological systems .
Don’t Miss: Can You Be Tested For Parkinson’s
What Causes Parkinson’s Disease
Parkinson’s disease occurs when nerve cells, or neurons, in an area of the brain that controls movement become impaired and/or die. Normally, these neurons produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinson’s. Scientists still do not know what causes cells that produce dopamine to die.
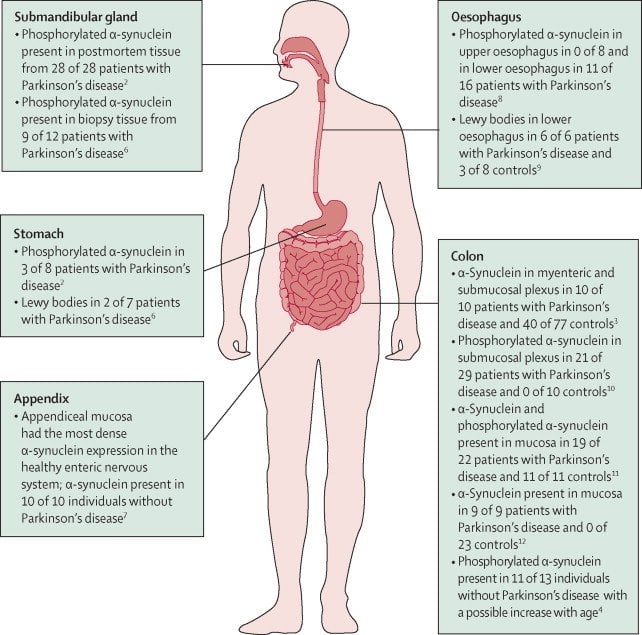
People with Parkinson’s also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinson’s, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying-down position.
Many brain cells of people with Parkinson’s contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons disease and Lewy body dementia.
Introduction: The Nervous Systems
In my pursuit of pragmatic solutions to Parkinson’s Disease, I found myself increasingly researching the nature of stress in humans, and inevitably drawn towards studying the Nervous System .
I have already shared much of what I’ve learned, together with the practical applications to lessening Parkinson’s symptoms, via this website, but here is a summary of my current understanding. We consist of many Nervous Systems in one body – we could say there are, at least, five of “me” in each of us. These include the Central , Sympathetic , Para-sympathetic , Enteric , and Somatic Nervous Systems . We may consider each one of these as a semi-autonomous “program”, which becomes more or less active in response to bio-rhythms and our internal/external environments. As each program is excited or inhibited, this can profoundly affect how we think, feel, move, act and re-act.
These internal and external imbalances can create circumstances in which some of the NS programs may become over-active or under-active for prolonged periods. These confused NS states can then lead to chronic illness, especially if the body receives contradictory signals from multiple “programs” at once, leading to a breakdown of self-identity.
Also Check: Does Sam Waterston Have Parkinson
How Will The Disease Affect My Life
Most people who have Parkinsonâs live a normal to a nearly normal lifespan, but the disease can be life changing.
For some people, treatment keeps the symptoms at bay, and they’re mostly mild. For others, the disease is much more serious and really limits what you’re able to do.
As it gets worse, it makes it harder and harder to do daily activities like getting out of bed, driving, or going to work. Even writing can seem like a tough task. And in later stages, it can cause dementia.
Even though Parkinson’s can have a big impact on your life, with the right treatment and help from your health care team, you can still enjoy the things you love. It’s important to reach out to family and friends for support. Learning to live with Parkinson’s means making sure you get the backing you need.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
You May Like: Wolf Parkinsons White Disease Treatment
Early Signs Of Parkinsons
Most people who are diagnosed with Parkinsons are 60 years of age or older, but early onset Parkinsons is possible, too.
In the first and second stages, the signs of Parkinsons are usually mild. Although 60-80% of the dopamine-producing cells in your brain are gone, you will still be able to go about your usual day-to-day activities.
Some of the most common symptoms during these stages include:
- tremors in the hands, arms, feet, or other body parts when resting
- stiffness and rigidity in muscles
- Bradykinesia , which can also cause a mask-like appearance of the face due to a lack of facial expressions.
What Is Parkinsonism
Parkinsonism is an umbrella term that includes Parkinsons disease, secondary parkinsonism and atypical parkinsonism. While the majority of parkinsonism cases are due to Parkinsons disease, cases also arise due to other neurological disorders, medication side effects, or toxins.Footnote 2 Footnote 3 Footnote 4
Parkinsonism refers to a set of signs and symptoms usually characterized by the following motor features:
- rigidity
- reduced sense of smell.Footnote 5 Footnote 6
Also Check: What Is The Difference Between Parkinson’s And Alzheimer’s
What Are The Causes
The cause of Parkinson’s is largely unknown. Scientists are currently investigating the role that genetics, environmental factors, and the natural process of aging have on cell death and PD.
There are also secondary forms of PD that are caused by medications such as haloperidol , reserpine , and metoclopramide .
When People Talk About Parkinsons They May Mention The Effects It Has On The Substantia Nigra But Did You Know That There Are Other Areas Of The Brain That Are Affected By The Condition
Parkinsons is a condition that causes the gradual loss of the dopamine-producing brain cells of the substantia nigra an area of the brain located just above where the spinal cord meets the midbrain. It is these cells that produce and release the neurotransmitter dopamine, which has a key role in turning thought about movement into action.
While this definition of the condition is useful to briefly explain Parkinsons, the whole story is somewhat more complex. Over the last 30 years, it has become accepted that Parkinsons also causes a number of non-motor symptoms, such as changes in sleep, smell and even the way we think, which likely involve other areas of the brain.
Now scientists are looking at the broader effects of the condition on the brain in an attempt to better understand why people experience different symptoms. The finding could lead us to new treatments that tackle more than just the motor symptoms of the condition.
Also Check: Types Of Parkinson’s Disease
Distinguishing Parkinson Disease From Other Parkinsonian And Lewy Body Syndromes
Pathologically, PD is categorized as a synucleinopathy along with dementia with Lewy Bodies, pure autonomic failure and multiple system atrophy . The first three of these disorders are all Lewy body disorders given their Lewy-related pathology. MSA is not a Lewy body disorder as it is characterized by glial cytoplasmic inclusions. Given the pathological overlap of Lewy body disorders, some have suggested that PD, dementia with Lewy bodies and pure autonomic failure may be considered Lewy body synucleinopathies with distinct but overlapping motor, cognitive and autonomic features. Clinical manifestations depend on the predominant sites of Lewy body formation and neuronal loss. Such a proposition is far from certain, however, given that the biological significance of Lewy-related pathology and its impact on neurodegeneration remains unclear. It is possible Lewy-related pathology interferes with normal cell function or that they are the result of a protective response to cytotoxic proteins.
The clinical and pathological overlap of Lewy body disorders is still being resolved and whether PD falls within the spectrum of Lewy body disorders or is truly distinct from pure autonomic failure or dementia with Lewy bodies remains to be seen.