Living With Parkinsons Disease
Depending on severity, life can look very different for a person coping with Parkinsons Disease. As a loved one, your top priority will be their comfort, peace of mind and safety. Dr. Shprecher offered some advice, regardless of the diseases progression. Besides movement issues Parkinsons Disease can cause a wide variety of symptoms including drooling, constipation, low blood pressure when standing up, voice problems, depression, anxiety, sleep problems, hallucinations and dementia. Therefore, regular visits with a neurologist experienced with Parkinsons are important to make sure the diagnosis is on target, and the symptoms are monitored and addressed. Because changes in your other medications can affect your Parkinsons symptoms, you should remind each member of your healthcare team to send a copy of your clinic note after every appointment.
Dr. Shprecher also added that maintaining a healthy diet and getting regular exercise can help improve quality of life. Physical and speech therapists are welcome additions to any caregiving team.
Managing Care In Late Stages
, March 3, 2017
What to expect in the late stages of Parkinson’s disease and the challenges of caring with those difficulties and needs. Tips for helping someone overcome freezing, accomplishing activities of daily living as long as possible, managing medications and swallowing issues, and ways to minimize caregiver stress.
Managing Advanced Parkinsons Disease
Advanced Parkinsons disease, stage 4 or 5 of the Hoehn and Yahr Scale, is characterized by very limited mobility without assistance, severe motor deficits, risk of falls, and cognitive and psychotic problems. With the advent of L-dopa and other dopaminergic treatments, the progression of PD has become markedly slower however, over the years treatment loses its efficacy, while a number of complicationssuch as motor fluctuations and dyskinesiadevelop, probably due to the progressive loss of dopaminergic neurons and their striatal and cortical connections. These complications are observed in 50% of patients after 5 years of disease and in 80% of patients after 10 years of treatment .
Treatment of the advanced stages of PD is entirely different from earlier stages. Early treatment is geared towards symptom relief and prevention of motor symptoms. During the later stages, the palliative care model is introduced to provide the patient with comfort and support. In the advanced stages, the focus of treatment shifts to treating nonmotor symptoms using a more supportive and palliative approach .
Also Check: Botox For Drooling In Parkinson’s
Care Of Patients With Advanced Parkinsons Disease
Presenting at the UCSF 9th Annual Conference of Parkinsons Disease for Patients and Caregivers, Dr. Maya Katz spoke for 38-minutes about caring for those with advanced Parkinsons disease, including a definition of advanced PD, medication considerations, non-motor symptoms, wellness and exercise, goals of care and taking a supportive care approach.
The Stages Of Parkinsons Disease
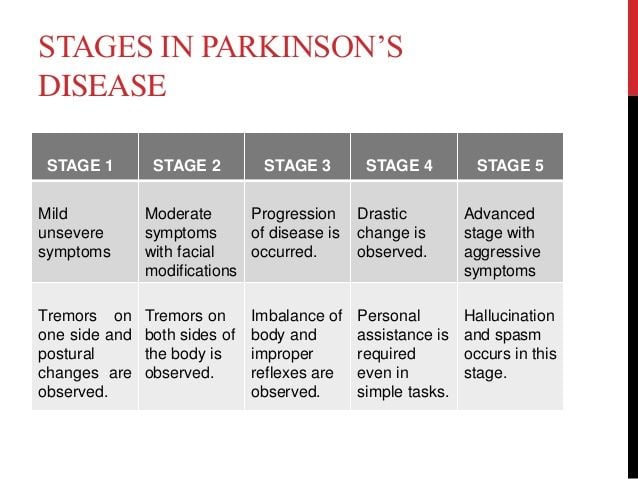
Stage One The Initial Stage: Symptoms are generally mild and may be easier to hide. Common symptoms include tremors, poor posture, balance issues, stooping of the back, and shaking of the limbs.
Stage Two Both Sides of the Body are Affected: The Parkinsons now affects both sides of the body, with increased symptoms that are more noticeable. Daily tasks become more difficult as symptoms now affect the entire body. It is harder to maintain your balance, walking becomes more difficult and tremors/shaking is more frequent.
Stage Three Increased symptoms & overall slowing down: By stage 3 the typical symptoms are more pronounced and the list of symptoms becomes more inclusive. One of the most noticeable changes is that movements and actions are much slower including facial expressions, speech, and motor skills. It is common to common to feel light headed, fainting, and experience hypo-tension .
Stage Five The Final Stage: During the final stages the person will require 24/7 one on one care and nursing skills. By stage 5, hospice care for late stage Parkinsons is a necessity and will help everyone involved with the acceptance of the final stage of the disease.Our trained hospice providers will guide you through these final stages. Our goal is to focus on the patient and the family unit as a whole.
Also Check: Parkinson’s And Personality Changes
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
What Are The Stages Of Parkinsons
Doctors sometimes use five stages to describe the progress of Parkinsons disease. Each stage presents changing or new symptoms that a person is likely to encounter.
It is worth noting that not everyone will reach the advanced stages. For some people, the symptoms remain mild, and they can continue to live independently and be mobile.
Dividing the condition into stages helps doctors and caregivers understand and address some of the challenges a person is experiencing as it progresses.
You May Like: Signs Of Parkinson Disease Early Symptoms
What Is Parkinson’s Disease
Parkinson’s disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinson’s disease and the degree of impairment vary from person to person. Many people with Parkinson’s disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinson’s disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinson’s disease will increase in the future. Adult-onset Parkinson’s disease is most common, but early-onset Parkinson’s disease , and juvenile-onset Parkinson’s disease can occur.
Parkinsons Disease Late Stage Complications
During the most advanced stage of Parkinsons typically between stages four and five a persons symptoms and medication regime become more complex.
Supporting care becomes especially important in advanced Parkinsons, with an estimated 50 to 80% of people eventually experiencing dementia and an increased number of falls.
Recommended Reading: Recipes For Parkinson’s Patients
Data Abstraction And Risk Assessment
Any two of three investigators independently screened titles, abstracts and retrieved full papers with eligibility criteria. Differences were resolved by review of the third investigator.
We assessed risk of bias by reviewing study design characteristics, including appropriate temporal relationships between exposures and outcomes, matching populations through individual variables or propensity scores and other adjustment methods. However, given we did not develop a meta-analysis from the findings, we did not exclude reporting any studies that met our inclusion criteria.
How Can Parkinson’s Affect Someone At The Advanced Or Palliative Stage
Parkinsons progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinsons about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinsons may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more off periods when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinsons symptoms, which become less predictable
- pain.
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinsons most often die because of an infection or another condition, usually caused by Parkinsons.
Also Check: How Can You Get Parkinson’s
Parkinson’s Disease And Palliative Care
This page outlines the decline of Parkinson’s disease and helps those coping with Parkinson’s understand what a palliative care team provides. There is a brief discussion of when and how to get palliative care, an online quiz to determine if palliative care is right for your family and a link to a palliative care provider search tool.
What Are The Non

Parkinson’s disease stages are defined by the severity of a patient’s motor symptoms and how much those symptoms impact one’s ability to function every day. But there are non-motor symptoms that are more likely to develop later in the disease, too, and a doctor may take those into consideration when assessing someone with the disorder.
For example, people with late-stage Parkinson’s disease might have difficulty chewing, eating, speaking, or swallowing , which is considered both a motor and non-motor symptom. Dysphagia in particular can lead to serious health problems like malnutrition, dehydration, and aspiration.
In the final stages of Parkinson’s disease, a person might develop cognitive changes, including slowness of memory or thinking, trouble planning and accomplishing tasks, and difficulty concentrating. Or they might notice changes in their bone health or vision.
But there’s no telling for sure if or when these symptoms will occur in any individual because Parkinson’s disease symptoms vary from person to person.
Don’t Miss: Signs Of Parkinson’s Disease
Parkinson’s Disease Diet And Nutrition
Maintaining Your Weight With Parkinson’s Disease
Malnutrition and weight maintenance is often an issue for people with Parkinson’s disease. Here are some tips to help you maintain a healthy weight.
- Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily.
- If you have an unexplained weight gain or loss , contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition.
- Avoid low-fat or low-calorie products. . Use whole milk, whole milk cheese, and yogurt.
Stages Of Parkinsons Disease
Experts have identified a general Parkinsons progression and created a set of Parkinsons stages, which can help determine where you are at in the disease and what your prognosis might be. However, not everybody progresses through Parkinsons disease in the same way or on the same time frame. Some people skip stages or rapidly progress to later stages. Others live for many years with mild or moderate Parkinsons and never reach the more advanced stage of the illness.
Here are five commonly recognized stages of Parkinsons, including what symptoms you might expect. Treatment also can occur during these stages to help prevent or delay later stages of the illness. This can include medication, , and lifestyle changes, such as a healthy diet and exercise program.
You May Like: Laser Treatment For Parkinson’s Disease
Bilateral Or Midline Involvement Without Impairment Of Balance
Months or years later similar symptoms and signs are noticed on the opposite side of the body, or other signs appear in midline what physicians call Axial signs. These may include: bilateral loss of facial expression decreased blinking speech abnormalities soft voice, monotony, fading volume after starting to speak loudly, slurring, stiffness of truncal muscles making the patient appear awkward and stiff or resulting in neck and back pain postural abnormalities causing stooping, generalized slowness in, but still capable of, carrying out all activities of daily living, sometimes an aggravation to those waiting for the patient to complete tasks.
Usually the diagnosis is easy at this Stage if it has been preceded by a clear cut tremor or other symptom on one side. But not all Parkinson’s patients have tremor or other definite signs of Stage I unilateral Parkinsonism. If Stage I was missed and the predominant symptoms at Stage II are only slowness and a lack of spontaneous movement, the diagnosis may still be in doubt. For example, even in Stage II, Parkinsonism may be interpreted as only advancing age.
How Is Parkinsons Disease Diagnosed
Diagnosing Parkinsons disease is sometimes difficult, since early symptoms can mimic other disorders and there are no specific blood or other laboratory tests to diagnose the disease. Imaging tests, such as CT or MRI scans, may be used to rule out other disorders that cause similar symptoms.
To diagnose Parkinsons disease, you will be asked about your medical history and family history of neurologic disorders as well as your current symptoms, medications and possible exposure to toxins. Your doctor will look for signs of tremor and muscle rigidity, watch you walk, check your posture and coordination and look for slowness of movement.
If you think you may have Parkinsons disease, you should probably see a neurologist, preferably a movement disorders-trained neurologist. The treatment decisions made early in the illness can affect the long-term success of the treatment.
You May Like: Mucuna Plants For Parkinson’s Disease
What Is Parkinsons Disease
Parkinsons disease is a progressive brain disorder that affects mobility and mental ability. If you or a loved one has been diagnosed with Parkinsons, you may be wondering about life expectancy.
According to some research, on average, people with Parkinsons can expect to live almost as long as those who dont have the condition.
Palliative Care As An Option
If your loved one is not eligible for hospice, the good news is that they can still receive palliative care. This type of care focuses on alleviating symptoms, discomfort, and stress associated with any illness, including PD.
The main difference between palliative care and hospice is that palliative care can be given along with standard treatments, including therapies intended to prolong life.
Read Also: What Causes Tremors Besides Parkinson’s
Why Is This Important
This study reveals unmet needs among those in the late stages of Parkinsons and their families. These issues are likely to apply in other chronic progressive neurological disorders such as dementia.
The shift from hospital care to community services is complicated in England by the separation in social care and healthcare funding, and the separation in organisation of different service providers. This research underlines problems with this model.
The research demonstrates the importance of Parkinsons Disease Nurse Specialists in caring for patients in their homes by expertly managing symptoms, providing personalised information and a link to hospital services, and offering emotional support. It highlights the importance of finding better ways of managing and living with deterioration and eventually planning end of life care. In parallel, informal caregivers could be better supported to help people with late-stage Parkinsons retain their sense of self, maintain day-to-day life, and allow them to stay in their own homes for longer.
Can Parkinsons Disease Be Prevented

Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Recommended Reading: Utensils For Parkinson’s Patients
What Is Your Advice For People With Parkinsons Who Are Preparing For End Of Life
It is very important for people with Parkinsons disease and their families to be informed. They must recognise the personal needs that need to be managed, and consider incorporating palliative care.
For the best care, trustworthy multidisciplinary support can be very helpful particularly from healthcare professionals who specialise in solving broad-based problems. This might include a movement disorder physician, nurse, physiotherapist, occupational therapist, speech therapist or, importantly, a psychologist or chaplain to help manage psychosocial and spiritual problems, taking into consideration cultural and social specificities.
How To Manage Symptoms At The End Of Life
At the end of life, good practice is to plan for any potential symptoms that may arise. The most common symptoms anticipated are pain, dyspnoea, nausea and vomiting, agitation, anxiety, delirium and noisy respiratory secretions.18 For patients with PD particular considerations should be given to the more commonly used medicines, specifically anticholinergics and antidopaminergics. These are usually prescribed for treatment of respiratory secretions and nausea and vomiting. Alternatives are available for respiratory secretions, and include glycopyrronium, in preference to hyoscine hydrobromide. Although this is an anticholinergic, only a small proportion crosses the blood brain barrier.
For nausea and vomiting, ondansetron,19 cyclizine, domperidone have all been suggested in PD.20 However, ondansetron has been shown to be inferior to domperidone in the pre-treatment of apomorphine.21 Cyclizine has anticholinergic properties and may exacerbate confusion, especially when comorbid psychosis or cognitive impairment are present. Levomepromazine, although it has antidopaminergic effects, has been shown to be effective for nausea with rotigotine in a case report.22
Agitation, dyspnoea and pain can all be managed with the same anticipatory medications as recommended.20 Specifically relating to PD, several case reports have supported the intraoperative use of midazolam, during sedation, for tremor and dyskinesias,23,24 as well as for agitation at the end of life.20
Read Also: Grants For Parkinson’s Patients
Managing The Terminal Phase
When the terminal phase can be anticipated by an acceleration in the patient’s global deterioration, a decision may have been taken with the patient and family not to treat further episodes of infection. A careful check for specific symptoms should be sought from the patient directly or from observing the patient for any signs of distress. Close family members will often recognise signs of unspoken distress. The views of experienced clinical staff may determine if the patient is frightened, in pain or has different nursing requirements.
For patients unable to swallow in the terminal stage, medication can be administered subcutaneously as needed or continuously using a syringe driver. Medication can be given, if necessary, to relieve specific symptoms as follows:
-
midazolam for fear or agitation
-
hyoscine butylbromide for drooling or chesty secretions
-
morphine for pain
If pain is present, a sufficient dose of morphine should be used to relieve it but without causing undesirable opioid side effects.