Nocturnal Leg Cramps Take Their Toll
Most nights I awake about 2 a.m. writhing in pain, drenched in sweat, and yelling for help. One of my legs is spasming out of control and the muscles feel hard to the touch. I try to move my leg, to forcefully extend it outside of the curled up ball that is now me, but it is too rigid to change position.
Tony, I cant move, I call to my husband, trying to tone down the panic Im feeling. Im paralyzed.
No, youre not, he responds as he sits down beside me on our bed, massages my limbs, and calmly reassures me that my cramping will relax in 10 minutes and we will go to the kitchen to have a snack, just like we always do. Thankfully, he is right.
The first I heard of nocturnal leg cramps was about two years ago when I started experiencing them myself. Gaining in frequency and intensity over time, the cramping has risen to the number 1 spot on my personal list of favorite PD symptoms, dropping incontinence to number 2. Imagine how painful leg cramps are that they beat out incontinence and the inconvenience and embarrassment that accompanies it.
- Narrowing of the arteries that deliver blood to the legs.
- Compression of the nerves in your spine.
- Too little potassium, calcium, and magnesium.
Muscle cramps and dystonia occur when muscles tighten or shorten involuntarily. Parkinsons muscle cramps are generally caused by muscular rigidity and reduced movement rather than by muscles contracting.
Second Type Of Leg Pain Is Caused By Dystonia
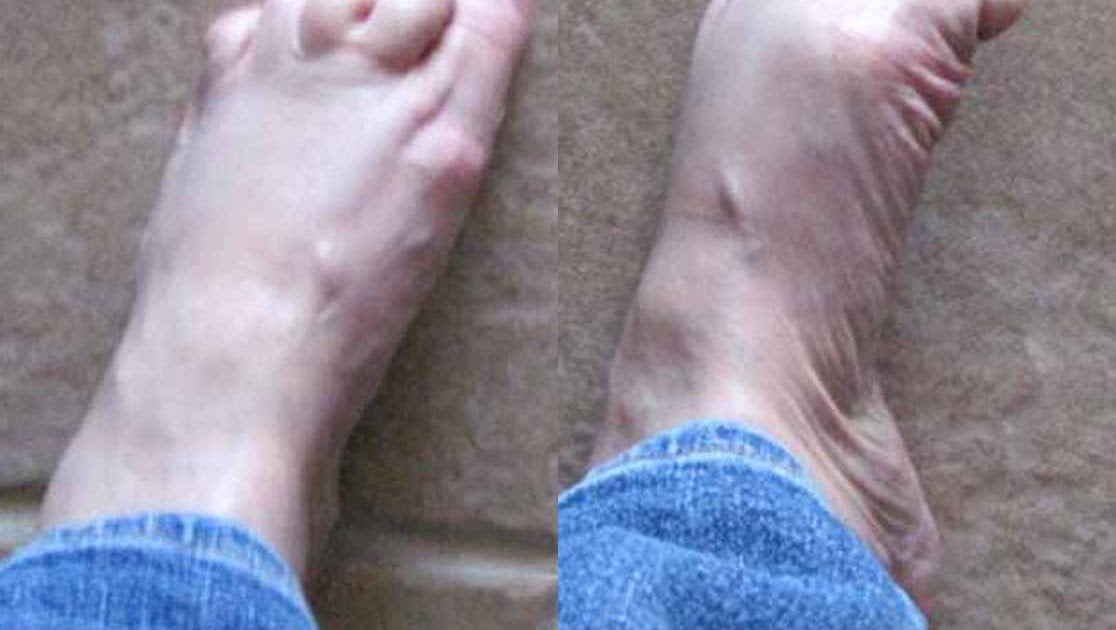
When related to levodopa, it usually occurs as a wearing off but can also occur at peak dose. In most cases this leg pain is unilateral and has direct correlation to medication intake. When pain is due to dystonia, it is more common in early morning. This type of leg pain is usually accompanied by toes curling and foot abnormally posturing.
Urinary Issues In Advanced Parkinsons Disease
Urinary dysfunction and symptoms in PD are most commonly caused by overactivity of the detrusor muscle, or the muscle of the bladder, which contracts excessively despite the fact that it is not filled with urine. This causes an increased urge to urinate and/or an increased frequency of urination, which can be especially prominent at night. In advanced PD, this could culminate in urinary incontinence, or involuntary release of urine. Mobility issues which make getting to the bathroom slower and more cumbersome, compound the problem.
Always remember that people with advanced PD may have other medical problems that affect their urination such as an enlarged prostate. Make sure to have a complete evaluation before assuming that the problem is only related to PD. It is also essential to keep in mind that if changes in urination occur suddenly, there could be a urinary tract infection present.
Once other medical issues and urinary tract infection are ruled out, there are a number of approaches to the issue of urinary incontinence in a person with advanced PD:
Unfortunately, for some, the above available options may not be sufficient to effectively treat urinary incontinence in advanced PD. If this is the reality, it becomes extremely important to keep the skin dry with frequent changes of incontinence products to prevent skin breakdown and the potential development of skin infection.
Also Check: Can Essential Tremor Become Parkinson’s
First Type Of Leg Pain Is Central Pain
This pain is described as constant burning sensation with occasional burst of sharp pain. As it was in my case, this pain is commonly exacerbated by cold and by light touch. I could not stand the sheets to touch my skin and being in a cold room sent my pain through the roof. This type is usually bilateral but it may start on the side where other Parkinsons symptoms begin. For me, it was the leg where my rest tremor began.
Identify The Cause Of The Pain
The first step in treating pain is to try to identify the cause. As I noted in the last essay, there are many different causes of pain for people with PD. If we look at the most common pain problems, low back and neck pain, we can see that there are many different causes for each. Many doctors order x-rays of the spine for these conditions, and they may be needed. The main problem with x-rays of the spine is that they always show arthritis, which is because virtually everyone over the age of 60 has arthritis in the spine. Whether thats the cause of the pain or not is usually not clear.
However, x-rays will show if theres a compression fracture , or a tumor. Since older women frequently develop compression fractures even without a fall, this can be important because we know then that the pain is likely severe, but time limited, and will resolve in a month or two. This makes it easier to treat with strong medication, like narcotics, because there is less concern for addiction. X-rays do not show discs, but disc herniation is much less common in older people so its of less concern.
Physical Therapy
Alternative treatments
Chiropractors focus entirely on spine pain and may be very helpful. Since many medical doctors are not very familiar with PD, I assume that many chiropractors probably arent either. Therefore it will be helpful to find one who is familiar with PD. Probably the best way to do this is through a Parkinsons Disease support group in your area.
You May Like: Can A Blood Test Detect Parkinson’s
Pain In Parkinsons Disease: A Spotlight On Women
This 2-page interview with neurologist, Dr. Jori E. Fleisher, discusses pain in Parkinsons disease with some interesting statistics about women and pain. Dr. Fleisher outlines the 4 primary types of pain in PD, how depression interferes with pain management, the role of exercise and medications in pain management as well as alternative therapies.
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Also Check: How Do You Get Parkinson’s
What Does Dystonia Feel Like
For some people, dystonia feels like a Charlie horse, which can be so painful that it wakes you up at night. For some, it feels like opposing muscles, muscles that work in pairs, are competing with each other. For example, when your bicep muscle contracts, your tricep muscle relaxes or elongates. In dystonia, both muscles want to contract at the same time, and it feels like theyre fighting. For some people living with Parkinsons, dystonia is the most distressing symptom they experience.
Want More Practical Articles Like This
Much more can be found in our Every Victory Counts® manual. Its packed with up-to-date information about everything Parkinsons, plus an expanded worksheets and resources section to help you put what youve learned into action. Request your copy of the Every Victory Counts manual by clicking the button below.
Thank you to our 2020 Peak Partners, Amneal and Kyowa Kirin, with special support from Adamas, for helping us make printing, distributing, and shipping the Every Victory Counts manual for free possible.
Read Also: Deep Brain Stimulation For Parkinson’s Disease Success Rate
Talking To Your Doctor
How do you know if your neck pain is potentially related to early signs of Parkinson’s disease?
You can’t know for sure, but you and your doctor can explore the issue. If your neck pain is accompanied by any of the other early warning signs of the condition, such as stiff shoulder, small handwriting, hand tremor, reduced arm swing, and shuffling gait, then it becomes more likely that you may have Parkinson’s disease.
If you have one or more of these symptoms, you should speak to a neurologist about them. Early identification may allow doctors to slow the progression of the disease, if, in fact, you do have the disease.
Impaired Posture And Balance
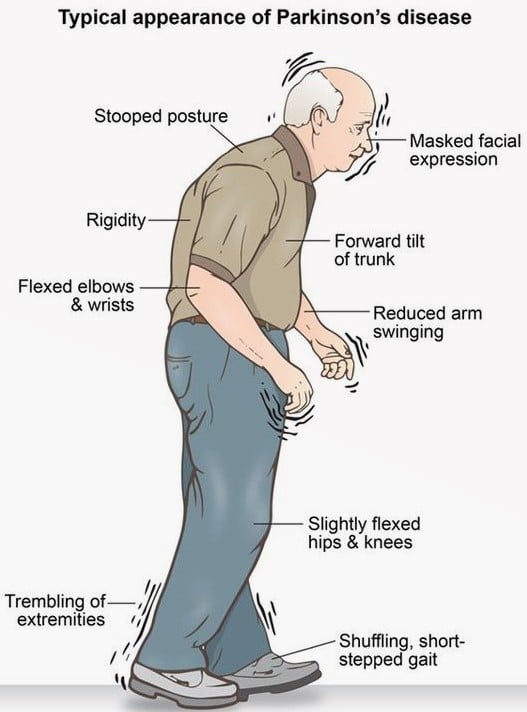
Postural instability is the most difficult Parkinsons symptom to treat, and one of the most important criteria for diagnosing Parkinsons.
Postural instability is the inability to balance due to loss of postural reflexes and often leads to falls. Patients with impaired posture and balance might revert to a stooped posture and have a shuffling gait.
You May Like: Using Cbd For Parkinson’s Disease
What Causes Numbness And Tingling In The Face
A stroke occurs when blood and oxygen to the brain are cut off, and causes numbness, confusion, and more. Transient ischemic attacks cause headache, numbness, tingling, or weakness in the face, arm, or leg, and more. Wernickes encephalopathy can cause confusion, lack of muscle coordination, and vision problems.
Pain In Parkinsons Disease

Parkinsons patients suffer from the same pain other people have, often amplified by the motor dysfunction, but they also have additional pain problems unique to PD. Lower back pain and back of he neck pain are most common. Strengthening exercises or stretching may be helpful. Identifying the cause of the pain is essential in treating the pain. Treatments include physical therapy, medications, and alternative therapies like Reiki, acupuncture and massage.
You May Like: What Is The Difference Between Parkinson’s And Alzheimer’s
Opening The Medicine Box In The Mind: The Psychology Of Pain
In this 50-minute lecture, Beth Darnall, PhD explains how our experience of pain goes beyond the physical sensation of pain. It has emotional and psychological components that affect our ability to treat pain. She cites research to demonstrate that and shares 13 specific tips to reduce the experience of pain and increase treatment effectiveness. Audience questions follow the lecture.
Leg Pain And Parkinson’s
Interestingly enough, one of my early symptoms of the disease was deep searing pain in my left leg, the type of pain my grandma had complained about many times. Initially this type of pain was worst in the morning as well as at night, making me think is was some sort of fasciitis. However not only did typical anti-inflammatories and muscle relaxants not alleviate my pain but pain worsened over time to a constant burning pain that felt as if someone was tearing the muscle and pouring hot oil on it. The pain was so excruciating it was permeating into all aspects of my life. I was constantly in need of deep tissue massage asking my husband to massage my legs just as my grandmother had asked of us time and time again. This helped only temporarily.
Which brings me to the four types of leg pain in PD.
You May Like: Movie Stars With Parkinson’s Disease
How To Deal With The 6 Common Causes Of Leg Pain In Pd
Severe leg pain is a common complaint from people with PD. Lately, it is understood that central pain is common to Parkinsons disease, and can even be the first sign of PD, usually bilaterally. This blog post lists six causes of lower limb pain, and the importance of treating it. Treatments depend on properly identifying the source of pain. Some treatment suggestions are included.
Tips For Dealing With Chronic Pain
Chronic pain is one that last more than 3-6 months , or pain that extends behind the expected period of healing. This blog post explains the different types of pain caused by Parkinsons disease and how to address pain brought on by the disease, by medications, or by comorbid disease. It is always best to treat pain before it becomes chronic.
Read Also: Stem Cells For Parkinson’s Disease Therapy
Low Blood Pressure When Standing
Orthostatic hypotension refers to a persistent drop in blood pressure that occurs when you move from sitting to standing, or from lying down to sitting up or standing. It can cause:
- dizziness
- headache
- feeling faint
OH is defined as a blood pressure drop of 20 millimeters of mercury in systolic blood pressure, or a drop of 10 millimeters in diastolic blood pressure.
Exercise Stretch And Strengthen
- Even if you dont feel like it, exercising every day can increase flexibility in your muscles and joints, reduce pain and discomfort, and improve circulation. Exercise can increase the secretion of your happy hormones, improve your mood, and decrease anxiety and depression.
- If you have discomfort in your calves, ankles, feet, or toes, and try the eight exercises physical therapist Sarah King recommends.
Read Also: Does Parkinson’s Cause Weight Gain
Cognitive And Psychiatric Symptoms
- depression and anxiety
- mild cognitive impairment slight memory problems and problems with activities that require planning and organisation
- dementia a group of symptoms, including more severe memory problems, personality changes, seeing things that are not there and believing things that are not true
What Causes Numbness And Tingling In The Arms And Legs
Diabetic neuropathy is a nerve condition of the extremities causing numbness, tingling, and pain. Wernickes encephalopathy can cause confusion, lack of muscle coordination, and vision problems. Cold exposure symptoms include color changes on the skin, numbness, stinging, redness, blisters, and more.
There is no need for treatment other than patience. Its worthwhile to note that carpal tunnel syndrome can also cause numbness in the middle fingertip . However, there will be other symptoms with carpal tunnel syndrome.
Also Check: Glutathione Injections For Parkinson’s
Increased Urination Urgency And Frequency
Bladder problems are a common occurrence in people with Parkinsons, occurring in 30-40 percent of people with the disease. The most common urinary symptom is a frequent and urgent need to urinate even when the bladder is empty, as well as trouble delaying urination.
Trouble emptying the bladder is a less common feature of Parkinsons urinary dysfunction. It may be caused by difficulty in relaxing the urethral sphincter muscles that allow the bladder to empty.
Pain Is An Unfortunately Common Problem In Parkinsons Disease
Of course, pain is common in the general population, especially among older people. A recent American study found that pain affected about twice as many people with Parkinsons Disease than those of the same age and gender without PD. About 50% of Parkinsons Disease patients in that study suffered from painful disorders. Men and women seem to be about equally affected. A very well described scenario is the patient who is followed for a painful frozen shoulder for a year or so before a tremor develops leading to a diagnosis of PD. Pain clearly plays a major role in quality of life. Everyone with chronic pain enjoys life less, leading to a vicious cycle in which pain causes depression or isolation which in turn leads to more pain.
Parkinson patients suffer from the same pain problems that other people have, often amplified by the motor dysfunction, but they also have additional pain problems which are unique to PD.
One recent review classified the types of pain Parkinsons Disease patients have into: musculoskeletal, in which the pain results from problems with the muscles , bones or joints dystonic, which is due to abnormal muscle contractions caused by the Parkinsons Disease or the medications used to treat it radicular pain, which is feels like the pain caused by pinched nerves central pain, which is presumed due to abnormalities in the brain, and is a continuously present pain that cannot be explained otherwise and discomfort related to an unpleasant urge to move.
Recommended Reading: Cialis And Parkinson’s Disease
Negative Impact Of Severity Of Pain On Mood Social Life And General Activity In Parkinson’s Disease
This case control study designed for clinicians and rehabilitation specialists to effectively identify pain from the patient’s point of view determined that PD patients had significantly higher pain severity scores compared to controls. PD patients with depressive symptoms had significantly higher pain severity and pain interference scores than controls without depressive symptoms. PD patients reported greater scores on Global BPI pain interference and all components of the pain interference subscale. Therefore, PD and depression seem to be correlated with higher perceived pain, severity and interference. A report on this study, by Jose Marques Lopes, PhD., was published in Parkinson’s News Today, September 21, 2018.
Pain Is A Common But Overlooked Problem In Parkinsons Disease
Pain is an often overlooked non-motor symptom of Parkinsons disease . Studies show that between 40-80% of people with PD report pain, which is likely why it is often suggested as a topic for this blog.
One of the reasons why the topic of pain and PD is difficult to address is that it is sometimes tough to discern whether a particular pain is due to PD or not. Chronic pain is such a common symptom among the general population, and people with PD are not immune to common problems as well. However, there are aspects of PD that may exacerbate the pain experienced from a common problem. In addition, there are particular types of pain that may be unique to people with PD.
Also Check: What Age Parkinson’s Disease
When Can Dystonia Occur
Each persons experience with Parkinsons and dystonia is unique. Dystonia can occur unexpectedly or during repetitive actions, such as writing or golfing. It can be brief or prolonged. It can occur as a response to your levodopa therapy, even if your medication is working optimally. And, it can occur at different times throughout the day or can be cyclical.
Stages Of Parkinsons Symptoms
Parkinsons symptoms can be divided into three categories or phases: pre-motor, motor, and cognitive. These phases dont necessarily happen in chronological order, and not all Parkinsons patients will experience all symptoms.
The premotor phase is the phase of Parkinsons in which non-motor symptoms are present. These symptoms include:
- loss of smell
- torso
- legs
There are two main categories of tremor: resting tremor, and action tremor. Resting tremor occurs when muscles are relaxed, like when your hands are sitting in your lap, and lessen during sleep or when the body part is in use. Action tremors occur with the voluntary movements of a muscle.
Tremors typically affect only one side of the body but may affect both sides as the disease progresses. Fatigue, stress, and intense emotion may worsen tremors.
Read Also: Idiopathic Parkinson’s Disease Life Expectancy