Common Physical Therapy Goals
As a physical therapy patient, you will work with a physical therapist to set and achieve realistic goals. A physical therapist will create a tailored, research-based exercise routine for you. They will first evaluate your current abilities and consider the areas you want to improve. The therapist will then design an exercise program to target those areas. Typically, physical therapy involves small achievements that build to a bigger goal.
Although your physical therapist will create an exercise plan based on your unique needs, shared goals for patients with Parkinson’s disease include:
Who Can Benefit From Pd Warrior
PD Warrior® was developed by specialist neurological physiotherapists and is designed specifically for people newly diagnosed with Parkinsons disease. For those further along in their journey, the program will still be of enormous benefit to you. Your specially trained physiotherapist and exercise physiologist will modify and personalise the program to suit your needs.
What Is Physical Therapy
Physical therapy is a specialized form of health care that involves evaluating and treating a person with limited mobility. It is used to treat many conditions, including arthritis, amputations, injuries and Parkinson’s disease. Physical therapists are licensed professionals trained to apply individualized techniques to help patients regain mobility.
You May Like: Parkinson’s Disease Exercise Program
Specialized Treatments To Manage The Symptoms Of Parkinson’s & Movement Disorders
Take control of you! Use it and improve it!
The Helen Hayes Hospital Outpatient Neurology Center offers innovative treatment programs for patients diagnosed with Parkinsons Disease and Atypical Parkinsonism. Our Outpatient Parkinsons Disease treatment program addresses both motor and non-motor symptoms, including slowness and smallness of movement, rigidity, tremors, impaired balance and coordination, sleep disturbances, cognitive changes, and pain.
Our Program Is Specifically Designed To Strengthen Muscles Affected By Parkinsons
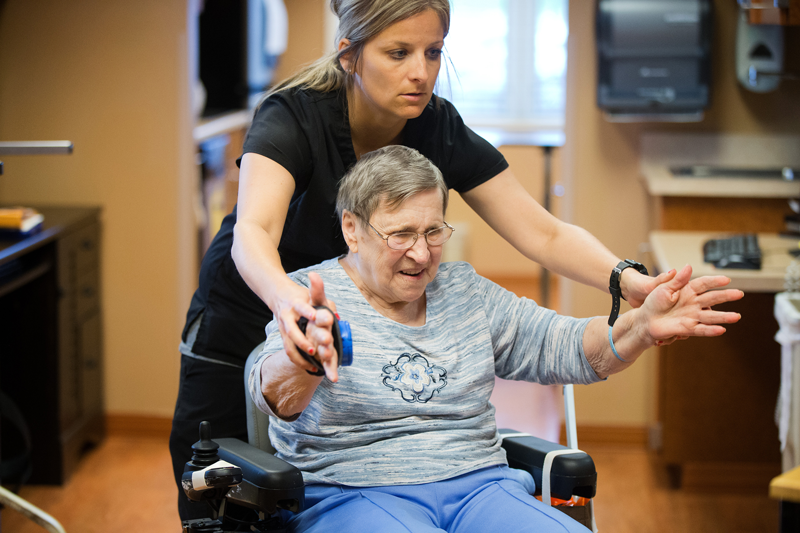
The goal of this program is to deliver specific exercises for clients with Parkinsons Disease . The programs include a combination of machine based Pilates, strength training and gross motor movements designed to enhance functional strength and co-ordination. The goal is to strengthen the muscles that have become weak and are affected by PD.
About Us
ProActive Rehabilitation and Health is a practice ran by Exercise Physiologists, who provide Exercise Based Rehabilitation Programs for a multitude of injuries and health conditions.
Our philosophy is through the education of Based and appropriate movement we can improve the quality of a persons life, and we do this through specialised exercise programming.
Useful Links
Recommended Reading: How Is Parkinson’s Disease Associated With Headaches
What Is Pd Warrior
Royal Rehab Private Hospital is proudly licensed to offer exercise program PD Warrior®, as part of its multidisciplinary rehab program in Sydney.
This internationally renowned group-based program helps both the physical and cognitive symptoms that occur with Parkinsons disease, in a fun and social way.
The PD Warrior® program uses a unique combination of physical and cognitive activities, to drive your brains natural ability to re-wire itself through neuroplastic change. This helps to improve bodily movement and to delay the onset of severe symptoms of the disease. Expect success with PD Warrior® your new exercise regime, support network and motivational coach all in one.
Clinical Motor Cardinal Signs
A-/hypo-/bradykinesia: These terms are defined, collectively, as slowed voluntary movement. Separately, akinesia indicates the absence of voluntary movement, while hypokinesia means smaller movements, and bradykinesia refers to slowness of movement. They usually determine any impairment in fine motor movements, facial expression , monotonic and hypophonic speech with a reduction of speed, and general motion amplitude. This can have an important impact in functional skills like arm swinging when walking, raising from a chair, handwriting, and general gesturing .
This cardinal sign is one of the best that emerges from its origin of dysfunction, which is cited in this chapter . It has been determined especially by a characteristic involving the movement programming of the cerebral cortex, in particular the supplementary motor area .
2. Rest tremor : this sign is usually asymmetric, consisting of alternate contractions of agonist and antagonist muscles, including flexors, extensors, pronators, and supinators of the wrists and arms, resulting in the pill rolling movement of the hand. It has a medium frequency and tends to disappear with action. The legs, lower jaw, or head may also be involved, resulting in an adduction-abduction movement of the lower limbs and yes-yes or no-no motion in the head .
You May Like: Loss Of Smell And Parkinson’s
What To Expect When You Are Referred To Epworth Rehabilitation
Depending on your individual needs and goals, your rehabilitation might be as an inpatient, staying in hospital or, as an outpatient, coming to hospital for a few hours over a period of time..Everyone’s experience of living with Parkinson’s disease may vary. When you are referred to our program, you will meet with a rehabilitation doctor, followed by the allied health team to develop an appropriate program to meet your specific goals, needs and concerns.
Parkinsons Clinical Signs Diagnosis And Rating Scales
The three clinical motor cardinal signs of PD, a-/hypo-/bradykinesia, rest tremor, and rigidity, are directly related to the degeneration of dopaminergic neurons. However, other motor symptoms and signs, secondary to degeneration of nondopaminergic pathways, can be described such as loss of postural control, postural stability/balance, and gait disturbance. In addition, the most well-known nonmotor characteristic motor symptoms have also been described. There can be additional psychiatric and autonomic features found, as well as cognitive impairment, sleep disorders, olfactory dysfunction, and pain.
Don’t Miss: Home Exercise For Parkinson Disease
Reach Out For Support
It can be challenging living with Parkinson’s disease, but you do not have to manage the symptoms alone. If you find yourself feeling discouraged or frustrated, share your feelings with others. Spend time with supportive friends and family members, or consider joining a support group. You might also speak with a counselor to address depression, anxiety or any other mental health issues you experience. By taking care of your mental and emotional health, you will be better positioned to reach your physical health goals.
Study Design And Sample
This is a retrospective, observational study, in which 24 PwPD accessed the NeuroRehabilitation Unit of the S. Maria Nascente Center, IRCCS Fondazione Don Carlo Gnocchi ONLUS in Milan, were included.
The study was performed in accordance with the principles of the Helsinki Declaration and by previous approval from the IRCSS Fondazione Don Carlo Gnocchi ONLUS Ethics Committee.
All medical records and data extracted and included in the present study concerned patients with the following characteristics: diagnosis of PD according to the United Kingdom Parkinson’s Disease Society Brain Bank involvement in an inpatient personalized and multidimensional rehabilitation program during the period of hospitalization in our NeuroRehabilitation Unit the presence of an initial evaluation and a final assessment regarding the rehabilitation treatment carried out in particular, in admission and in discharge, they had to be present and filled in: a functional evaluation , a cognitive assessment , and an evaluation of common geriatric aspects signature of a written informed consent that allows the use of clinicalmedical data for research purposes.
Don’t Miss: Music Therapy For Parkinson’s
Make It To Your Appointments
The number of physical therapy appointments you need depends on your condition and goals. Generally, your first appointment will include an evaluation and exercise recommendations. In following appointments, your physical therapist will check your progress and add or modify exercises according to your needs. Make sure you attend all of your appointments to stay on track.
Physical Therapy In Pd

As every individual with Parkinsons has a different set of problems, a qualified physical therapist would need to individualize the treatment focused mostly on:
- Improve posture, gait, and rigidity, through stretching and neuromuscular re-education, to walk better, work effectively.
- Muscle strengthening exercises to improve movements.
- Teach strategies to manage the day to day tasks.
- Provide mobility aids to keep a person active and independent.
- Prescribe special exercises to improve balance and stability.
- Reduce the risk of trauma or fall by teaching specific techniques
- Helping manage fatigue
Don’t Miss: Stage 2 Parkinson’s Disease
What Are The Symptoms Of Parkinsons Disease
The four diagnostic symptoms are: tremor, bradykinesia , muscle rigidity and postural instability. Other symptoms may include loss of smell, constipation, slowness in thinking, depression, fatigue, changes in speech fluency, micrographia , decrease in speech volume, sleep disturbances and swallowing changes.
Parkinson Voice Project Speak Out Program
Methodist is a proud provider of Speak Out!®, a highly effective speech therapy program developed by Parkinson Voice Project. Our certified speech therapists at Methodist Hospital, Methodist Jennie Edmundson Hospital and Methodist Fremont Health Hospital will work with you during this month-long program to help you:
- Improve your vocal volume
- Strengthen muscles for improved swallowing
Don’t Miss: Do You Get Pain With Parkinson’s
Parkinson’s Evaluation & Treatment
Patients are evaluated by a physical, occupational, and speech therapist based on need. An individualized treatment plan, including but not limited to functional mobility training, functional Activities of Daily Living training, balance training, cognitive retraining, vocal retraining, breath support training, visual retraining, and caregiver training will be implemented.
Helen Hayes Hospital offers an innovative, disease-specific treatment program for patients with PD. The program incorporates LSVT BIGTM and LSVT LOUDTM, which are research-based therapy protocols that address two of the main symptoms associated with PD: functional mobility and speech output. These treatments are provided by the Hospitals LSVT® certified occupational, physical, and speech therapists. They also incorporate neuroplasticity-principled programming , driven by Parkinson Exercise Experts. These experts have been trained to implement treatment plans or community programming that adhere to research-based Exercise4BrainChange® techniques, which are shown to optimize learning, brain health, and function.
LSVT LOUD is an effective speech treatment that improves vocal loudness, intonation, and voice quality. The therapy is also effective in managing disordered articulation, diminished facial expression and impaired swallowing. It uses enhancement of sound and articulation to bring the voice to an improved, healthy vocal loudness with no strain.
Physical Therapy For Parkinsons Disease
Its well-known that exercise of all kinds is beneficial for patients with Parkinsons disease. But physical therapy, in particular, is key. Why? A professional can guide you through the right moves to increase mobility, strength and balance, and help you remain independent, says Denise Padilla-Davidson, a Johns Hopkins physical therapist who works with patients who have Parkinsons. Here are things a therapist may work on:
Note: Please discuss any exercise program with your physician/neurologist and get a referral to a physical therapist or trainer with expertise in Parkinsons disease before starting any specific program.
Read Also: What Kills A Person With Parkinson’s Disease
The Right Program For You
PD Warrior® is not the same as working out in the gym, going for a walk or going for a swim. Although these are all examples of good exercise for general fitness, those with Parkinsons disease need tailored and specific exercises to ultimately see results in physical mobility and functionality.
PD Warrior® incorporates the most current evidence into its program to ensure that you get success and drive the brains natural ability to re-wire itself. Find out more today so you can move better, think better, look better, build your confidence and regain control.
Benefit from our multidisciplinary approach
Royal Rehab Private Hospital is licensed to offer PD Warrior® as part of the Day Rehab program across Sydney. The Day Rehabilitation program is a multidisciplinary approach to physical rehabilitation that includes a minimum of two disciplines personalised to suit your needs. Other services offered by Royal Rehab Private Hospital include LSVT BIG and LSVT LOUD, , Exercise Physiology, physiotherapy, hydrotherapy, Speech Pathology, Occupational Therapy and dietetics.
Each of our Day Rehabilitation programs run for a minimum of 1.5 hours or up to 3 hours .
Referrals and Funding
How Can Physical Therapy Help Parkinson’s Disease
Physical therapy is an important part of a treatment plan for Parkinson’s disease. It aims to help individuals with Parkinson’s disease remain active and independent as long as possible. According to a recent meta-analysis, physical therapy significantly improves symptoms related to motor skills. The Parkinson’s Foundation states that increasing physical activity to 2.5 hours a week or more can help people with Parkinson’s disease maintain their quality of life.
Overall, physical therapy can help with the following:
- Increasing endurance
- Reducing pain
Because physical therapy improves motor skills and decreases pain, you can expect it to help with many of your regular activities, such as getting up from a chair, climbing stairs and getting into and out of a car.
Physical therapy can also improve other symptoms associated with Parkinson’s disease, such as depression, anxiety and fatigue. Lastly, it can help with other health issues that impair mobility, like joint pain.
Doctors recommend beginning an evidence-based physical therapy program as soon as possible. Exercise can induce neuroplasticity, or the brain’s ability to change in response to behavioral changes. When you begin physical therapy, your brain learns new ways to move and think. Exercise also helps brain cells stay healthy. In other words, physical therapy may slow the progression of Parkinson’s disease.
You May Like: How Do You Treat Parkinson’s Disease Naturally
Choose Activities You Enjoy
Make sure you choose exercises that are fun and challenging but not too difficult. For example, if you enjoy walking in nature, make that part of your exercise routine. It is important to enjoy appointments with your physical therapist, too. If your physical therapy program is not working for you, talk with your physical therapist so they can change your routine.
If you choose activities you like, you are more likely to stick to your plan and reach your goals.
Family Support Of Therapy For Parkinsons Disease

For caregivers and family members, its important to be involved in a Parkinson patients treatment. Family involvement ensures that even when patients are at home, they can have someone to depend on who understands their challenges and is willing to help monitor and encourage their daily exercises.
For inpatient therapy for Parkinsons disease, .For outpatient therapy for Parkinsons disease, .
Recommended Reading: How Does Occupational Therapy Help Parkinson Disease
Rehabilitation For Parkinsons Disease
NYU Langones Rusk Rehabilitation has a long history of treating people with Parkinson’s disease. The professionals in our Parkinsons disease rehabilitation program have specialized training that allows them to provide the medical, nursing, and therapeutic care people with the condition need. The goal is to maximize a persons ability to function and to maintain quality of life.
At Rusk Rehabilitation, rehabilitation doctors, called physiatrists, specialize in treating people with Parkinsons disease. Physiatrists evaluate the medical needs and treatment goals of people with Parkinsons disease, as well as the needs and concerns of their families. The physiatrist and rehabilitation team then create a customized treatment plan to help each person achieve the best possible outcome.
Vocal Quality And Volume
The most prominent vocal symptom related to Parkinson’s is a reduction in volume. Because this change occurs gradually over a period of years, you are often the last one to recognize it as a communication problem. If family and friends are often asking for a repetition, it may indicate the need to have a voice evaluation.
Parkinsons can also affect vocal quality. People often describe changes such as a raspy, hoarse or breathy quality. These symptoms often clear quickly after the first couple of weeks of LOUD therapy.
Don’t Miss: Drugs Prescribed For Parkinson’s Disease
Treating Parkinson’s Disease With Rehabilitation
Maintaining physical activity is a very important component in the management of Parkinson’s disease and parkinsonism.
The University of Maryland Parkinson’s Disease and Movement Disorders Center is at the forefront of research to increase our understanding of the effects of physical and cognitive training in Parkinson’s disease and developing recommendations for our patients.
Outpatient rehabilitation therapy enhances the lives of people with Parkinson’s disease. A program of physical therapy and occupational therapy can help people learn movement strategies:
- How to roll over and get out of bed more easily
- How to rise from a chair or get out of a car
Therapists sometimes suggest simple devices to assist with daily activities, such as:
- Shower grab bars
- Shower stools
- Elevated toilet seats
Occupational therapists and physical therapists have experience finding ways to help people button shirts, cook and generally keep their lives going. They know about special kinds of utensils that help keep food on a spoon or a fork. Even people with serious tremor, slowness or rigidity can use these utensils to feed themselves without making a mess.
In addition to allowing people to enjoy their meals, this kind of therapy helps people maintain their independence and self-respect. Certain forms of speech therapy can also be valuable in improving voice problems.
In This Section:
Types Of Physical Therapy For Parkinson’s Disease
Parkinson’s disease is a nervous system disorder that affects over 1 million Americans. This disease involves the part of the brain that controls movement. The main symptoms include tremors, muscle rigidity and difficulty with coordination, balance and walking.
Although there is no cure for Parkinson’s disease, various treatments can relieve symptoms and help patients maintain their quality of life. Physical therapy is one form of treatment known to help individuals with Parkinson’s disease increase mobility, strengthen their muscles, improve coordination and balance, and ultimately, remain independent. This post explores the different types of physical therapy and how to make the most of a rehabilitation program.
Also Check: Parkinson’s And Marriage Breakdown
Information And Variables Collected
The main data and variables extracted from the medical records were the Barthel Index as a measure of PwPD’s functional disability in daily life the Mini-Mental State Examination , Token test , Phonemic and Semantic Fluency , Copy and Recall Rey’s Figure , Raven’s Colored Progressive Matrices as measures of PwPD’s cognitive functioning and measures of common geriatric aspects: Numeric Rating Scale to detect the presence and severity of pain, Norton Scale to take over the risk of contracting pressure ulcers, and Conley Scale to assess the fall risk.
The Movement Disorders Society Unified Parkinson’s Disease Rating Scale Part III-Motor Examination Part III was filled out at baseline.