What Is The Prognosis And Life Expectancy For Parkinson’s Disease
The severity of Parkinson’s disease symptoms and signs vary greatly from person to peson, and it is not possible to predict how quickly the disease will progress. Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease. Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death. Many treatment options can reduce some of the symptoms and prolong the quality of life.
Parkinsons Disease Is A Progressive Disorder
Parkinsons Disease is a slowly progressive neurodegenerative disorder that primarily affects movement and, in some cases, cognition. Individuals with PD may have a slightly shorter life span compared to healthy individuals of the same age group. According to the Michael J. Fox Foundation for Parkinsons Research, patients usually begin developing Parkinsons symptoms around age 60. Many people with PD live between 10 and 20 years after being diagnosed. However, a patients age and general health status factor into the accuracy of this estimate.
While there is no cure for Parkinsons disease, many patients are only mildly affected and need no treatment for several years after their initial diagnosis. However, PD is both chronic, meaning it persists over a long period of time, and progressive, meaning its symptoms grow worse over time. This progression occurs more quickly in some people than in others.
Pharmaceutical and surgical interventions can help manage some of the symptoms, like bradykinesia , rigidity or tremor , but not much can be done to slow the overall progression of the disease. Over time, shaking, which affects most PD patients, may begin to interfere with daily activities and ones quality of life.
What Is Parkinsons Disease
Parkinsons disease is a progressive brain disorder that affects mobility and mental ability. If you or a loved one has been diagnosed with Parkinsons, you may be wondering about life expectancy.
According to some research, on average, people with Parkinsons can expect to live almost as long as those who dont have the condition.
Don’t Miss: What Benefits Can You Claim For Parkinson’s Disease
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38 and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patients handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
You May Like: Pump For Parkinson’s Disease
Myth : Parkinsons Is Only A Motor Condition
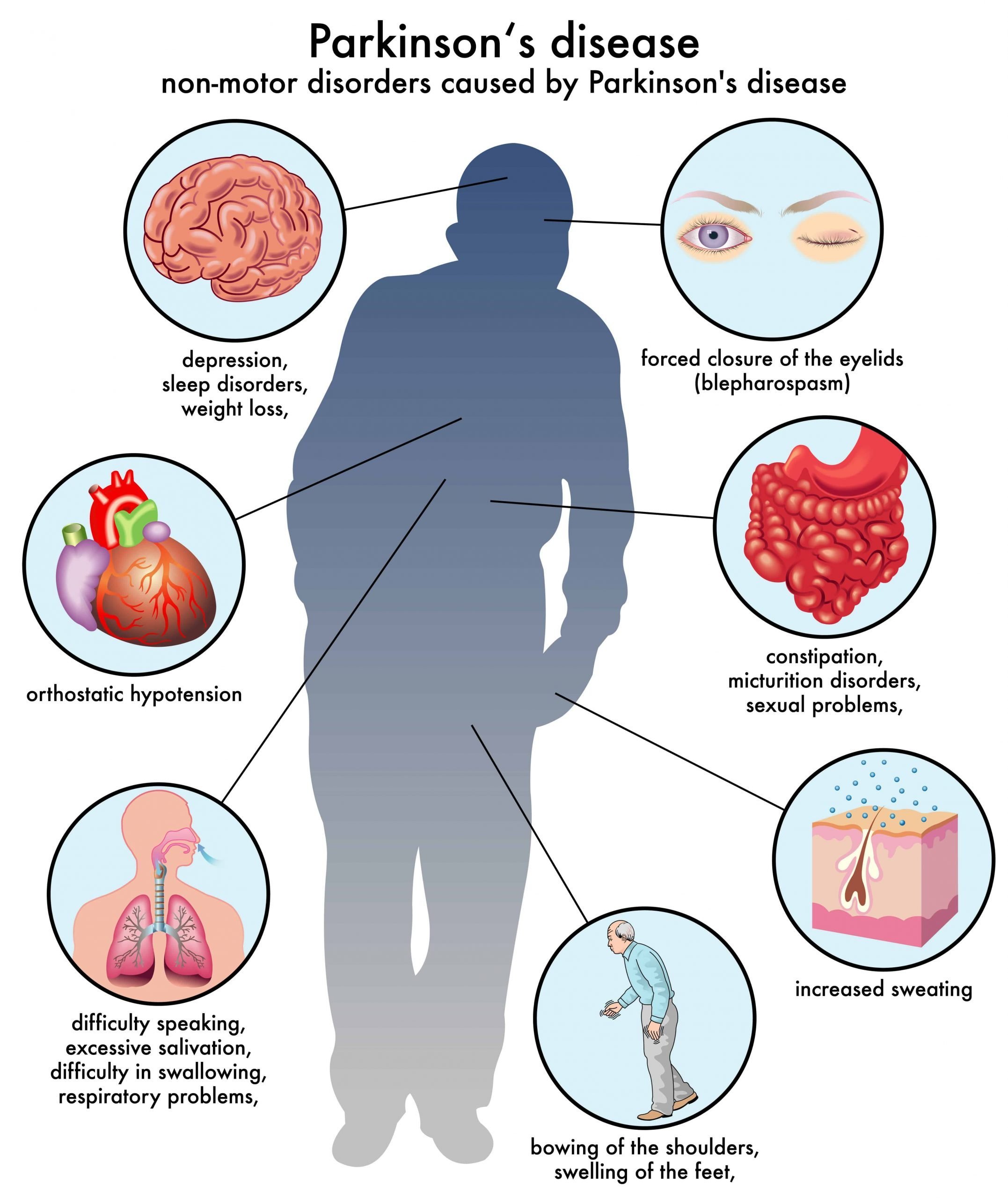
Fact: While its true that Parkinsons disease symptoms include shaking and tremor, rigid muscles, slowness of movement, and a frozen or flat expression, its a lot more than that.
Nonmotor symptoms deserve and are getting more attention from doctors and researchers. These symptoms include cognitive impairment or dementia , anxiety and depression, fatigue, sleep problems and more.
For some patients, nonmotor symptoms are more disabling than motor symptoms, which are the focus of treatment. Be sure to talk to your doctor about other issues so you can get all of your symptoms addressed.
Myth : Parkinsons Disease Is Fatal
Fact: Although a diagnosis of Parkinsons is devastating, it is not as some people may still believe a death sentence. Parkinsons disease is not a direct killer, like stroke or heart attack. That said, much depends on the quality of your care, both from your medical team and yourself.
As the disease progresses, you may become more vulnerable to falls, which can be dangerous. Thats why exercise and physical therapy are so important.
Infection is another problem. In later stages of Parkinsons, people often miss those signals and may not notice somethings up until its too late. That can be, literally, a killer so be sure to stay up to date with checkups.
Don’t Miss: Does Parkinson’s Cause Tinnitus
Ascertainment Of Vital Status
In January 2012, we confirmed the status of all patients. For those who had died, death certificates were obtained from the database of the Shanghai Municipal Center for Disease Control and Prevention, China. Diagnoses on the death certificate were registered using the international Classification of Disease ninth and tenth revision . The primary causes of death were grouped into five different categories based on the ICD-9 classifications.17
What Causes Parkinson Disease
Parkinson disease arises from decreased dopamine production in the brain. The absence of dopamine makes it hard for the brain to coordinate muscle movements. Low dopamine also contributes to mood and cognitive problems later in the course of the disease. Experts don’t know what triggers the development of Parkinson disease most of the time. Early onset Parkinson disease is often inherited and is the result of certain gene defects.
Don’t Miss: Are There Stages Of Parkinson’s Disease
Causes Of Parkinsons Disease
Parkinsons disease is a progressive neurodegenerative disorder best known for its movement-related symptoms. However, it also causes cognitive changes.
Parkinsons underlying cause is the death of dopamine-producing neurons, or nerve cells, in a brain region called the substantia nigra.
Dopamine is a neurotransmitter, which is a molecule produced by the body to send messages between nerve cells. It is involved in a range of behaviors, including control of body movements, learning and memory, the sleep-wake cycle, and moods, such as depression and mania.
Both genetic and environmental factors appear to influence a persons risk of developing Parkinsons. Thats why the disorder is thought to be a product of a combination of these factors. Genetics loads the gun and environment pulls the trigger, is one way Parkinsons has been described.
Availability Of Data And Materials
Pseudonymised outcome data were supplied by NHS Digital under a data sharing agreement subject to there being no risk of identifying any individual in the publication. However, as our cohort data contains detailed information on each workers job-history and health outcomes, identification of an individual is a possibility if raw data would be freely available. Derived data from this cohort is available in our repository by writing to the corresponding author, but researchers who would like to use the data will need to obtain agreement from NHS Digital.
Also Check: How To Support Someone With Parkinson’s Disease
Associated Factors As Predictor Of Death
The present study shows that low MMSE score at baseline was related to an increased risk of death among PD patients . The results are in accordance with the previous observations, which indicated that PD patients with cognitive impairment have a particularly high risk of mortalityReference Auyeung, Tsoi and Mok3,Reference Posada, Benito-Leon and Louis7,Reference Hughes, Ross, Mindham and Spokes9 and cognitive impairment is an independent predictor of decreased survival in PD.Reference de Lau, Verbaan, Marinus and van Hilten24,Reference Xu, Gong, Man and Fan25 It is well-known that cognitive impairment, especially Parkinsons disease dementia , occurs in 24% to 31% of PD patients,Reference Aarsland, Zaccai and Brayne26 and both reduced cholinergic activity in the cortex and the spread of fibrillar -synuclein pathology are thought to be the crucial mechanisms responsible for the development of PDD.Reference Chen, Xu, Wang and Chen23,Reference Irwin, Lee and Trojanowski27 Furthermore, the neocortical -synuclein pathology may confer a worse prognosis. Our results support the common hypothesis for PD with cognitive impairment as a predictor of death. The molecular pathological mechanism needs to be addressed in more detail in the future.
Smr And Cause Of Death
Although some studies report survival time, SMRs allow comparison between population groups with different demographics and life expectancies.Reference Ishihara, Cheesbrough, Brayne and Schrag11 The SMR of this cohort was 0.62 , implying that the five year mortality ratio of the patients with PD was not significantly higher than the ratio of the general urban Chinese population. The SMR in the present study is consistent with the survival data from the highly selected subjects in the DATATOP study 12 and an Austrian study carried out by Diem-Zangerl and his co-workers ,Reference Diem-Zangerl, Seppi and Wenning4 and very close to the previous investigation from Hong Kong .Reference Auyeung, Tsoi and Mok3
Also Check: Parkinson’s Education For Nurses
How Is Parkinson Disease Treated
Parkinson disease can’t be cured. But there are different therapies that can help control symptoms. Many of the medicines used to treat Parkinson disease help to offset the loss of the chemical dopamine in the brain. Most of these medicines help manage symptoms quite successfully.
A procedure called deep brain stimulation may also be used to treat Parkinson disease. It sends electrical impulses into the brain to help control tremors and twitching movements. Some people may need surgery to manage Parkinson disease symptoms. Surgery may involve destroying small areas of brain tissue responsible for the symptoms. However, these surgeries are rarely done since deep brain stimulation is now available.
What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Recommended Reading: Parkinson’s Disease Brain Changes
New Clues On Why Some People With Parkinsons Die Sooner
The American Academy of Neurology, an association of more than 22,000 neurologists and neuroscience professionals, is dedicated to promoting the highest quality patient-centered neurologic care. A neurologist is a doctor with specialized training in diagnosing, treating and managing disorders of the brain and nervous system such as epilepsy, dystonia, migraine, Huntingtons disease, and dementia.For more information about the American Academy of Neurology, visit http://www.aan.com.
Myth : Parkinsons Research Is Stalled
Fact: It may feel as though theres nothing dramatic going on in the Parkinsons disease field, but there are several recent and very exciting breakthroughs regarding our understanding of the underlying pathology and disease mechanism. This will translate into actual clinical results in the next few years.
Recommended Reading: Green Tea For Parkinson’s
How Did They Do This
Dr. Backstrom works at Umea University, in Sweden. He and his colleagues work in an area in northern Sweden where approximately 142,000 people live. Umea University is the main medical center in this region, and most of the people who live there are referred to Umea University. In order to better understand the connection between PD and early death, Dr. Backstrom enrolled only people who had early PD and who were not yet taking medication for this. People were enrolled between January 1, 2004, and April 30, 2009, and were followed until August 31, 2017. Dr. Backstrom identified 182 people with symptoms of early PD.
In the study, many tests were done . All of the participants had neurologic examinations, filled out questionnaires, and had neuropsychological testing. Not everybody had the other tests . The first test was a detailed neurologic examination in order to confirm and firmly establish the diagnosis of PD. This is essential because there are several illnesses that are very similar to PD, and Dr. Backstrom wanted to be sure that the diagnosis was as precise as possible. Of the 182 patients, Dr. Backstrom found that 143 had classic PD, 13 had a similar disease called multiple system atrophy , and 18 had progressive supranuclear palsy . The other 8 had an unclear diagnosis or simply did not have PD.
Tests performed
The study was designed to look at the association of mortality with PD. During the study, 109 people died. For 98 of these , a cause of death was known.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Don’t Miss: Anxiety And Parkinson’s Disease
What Are The Complications Of Parkinson Disease
Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may arise later. As the disease gets worse with time, many people develop dementia. This can cause profound memory loss and makes it hard to maintain relationships.
Parkinson disease dementia can cause problems with:
- Speaking and communicating with others
- Problem solving
- Forgetfulness
- Paying attention
If you have Parkinson disease and dementia, in time, you likely won’t be able to live by yourself. Dementia affects your ability to care of yourself, even if you can still physically do daily tasks.
Experts don’t understand how or why dementia often occurs with Parkinson disease. Its clear, though, that dementia and problems with cognitive function are linked to changes in the brain that cause problems with movement. As with Parkinson disease, dementia occurs when nerve cells degenerate, leading to chemical changes in the brain. Parkinson disease dementia may be treated with medicines also used to treat Alzheimer’s disease, another type of dementia.
What Are The Considerations For Pain Management In The Last Days Of Life In Pd
It is important to consider that pain can be a risk factor for, and associated with, many other symptoms which might be the presenting features in a patient with complex or advanced PD. These include a new or worsened confusion, hallucinations, agitation and symptoms of depression or apathy.
As well as being an underlying cause of another symptom, pain can also be the symptom of other features of PD, such as rigidity, dyskinesia, but also non-motor features, for example, depression and fatigue.
Identifying whether pain is at the root of the presenting complaint and what might be causing the pain is therefore the most important part of the initial history from the patient and the carer. Then using the clinical examination to confirm findings from the history and identify any features not already elicited such as abnormal posturing, or dystonia.
A recent review into the pathophysiology and treatment of pain in PD suggests simple analgesia with paracetamol and non-steroidal anti-inflammatory drugs but advises caution with opiate analgesia as constipation is a recognised problem in PD patients.25 The review mentions, however, the lack of evidence for many widely used analgesics specifically in PD.26
Read Also: Stem Cells For Parkinson’s Disease Therapy