Side Effects Talk To Your Doctor Or Pharmacist
If you get side effects from your Parkinson’s medicines, tell your doctor or pharmacist. Common side effects include nausea , light-headedness, leg swelling and sleep problems. Also let them know if you think your medicines are causing confusion, hallucinations or involuntary movements. Some people have an unusual desire to gamble or engage in other obsessive behaviors. Your doctor may adjust the amount of medicine you take or you may be given another type. Do not stop taking your Parkinsons medicines until you are advised to do so.
Parkinsonism Vs Parkinsons Disease
Parkinsonism refers to a cluster of symptoms that mimic the movement problems caused by Parkinsons disease. Its sometimes referred to as atypical Parkinsons disease, secondary parkinsonism, or Parkinsons plus.
Parkinsons disease is a chronic, neurodegenerative brain disorder. In addition to problems with movement, Parkinsons disease causes non-motor symptoms that arent caused by drug-induced parkinsonism. They include:
- depression
- constipation
- anosmia
Another key difference between drug-induced parkinsonism and Parkinsons disease is symmetry. Drug-induced parkinsonism usually affects both sides of the body equally. Parkinsons disease affects one side of the body more than the other.
Parkinsonism can be caused by medications, repeated head trauma, and environmental toxins. It can also be caused by neurological disorders, including Parkinsons disease. Other neurological conditions that cause parkinsonism include:
- progressive supranuclear palsy
These medications dont cause resting tremors. Rather, they cause:
- Action tremors. These occur in a body part thats moving, not a body part thats resting.
- Postural tremors. These occur when a body part is forced to withstand gravity, such as when arms are outstretched or legs are raised.
Focused Ultrasound Therapy To Treat Tremor
Focused Ultrasound is used to treat Parkinsons patients experiencing tremor that does not respond to medication.
In medical terms this procedure is known as a non-invasive thalamotomy.
During the Focused Ultrasound procedure, the patient is awake. No general anaesthesia or surgical incisions are required.
A frame is placed on the patients head with local anaesthetic and the patient lies in a Magnetic Resonance Imaging scanner. If required some sedation can be given to help maximise comfort and relaxation during the procedure.
Doctors then use brain scans to direct ultrasound beams to the target location in the thalamus region of the brain.
The thalamus is a small structure within the brain located just above the brain stem. It has nerve connections with both cerebral cortex and the midbrain. The main function of the thalamus is to relay motor and sensory signals to the cerebral cortex.
The focused ultrasound sends 1024 individual ultrasound beams through the brain that intersect at a single target point in the thalamus to destroy the tremor-causing cells without damaging the surrounding normal tissue.
This is all monitored in real time on the MRI and by repeatedly checking the patient and until the tremor has been treated.
When the treatment is over there is an immediate and significant reduction in tremor.
In Australia, Focused Ultrasound therapy is administered by St Vincents Hospital where it is known as the Neuravive Procedure.
Also Check: My Dad Died From Parkinson’s
Dopamine Agonist Withdrawal Syndrome
Recent research has discovered dopamine agonist withdrawal syndrome, which can happen when someone very suddenly stops taking dopamine agonists, perhaps because they are experiencing impulsive and compulsive behaviour. It can lead to symptoms including depression, anxiety or pain . Any withdrawal from Parkinsons medications needs to be gradual, under the supervision of a health professional, to avoid the risk of this syndrome.
Injections of apomorphine are taken in a similar way to insulin for diabetes. There is a ready-to-use injection pen that works within 10 minutes and is often used as a rescue measure. This is very useful if you have a sudden off period.
Soreness or nodules can develop where the needle enters your skin. If this happens, do not stop the treatment and quickly seek advice from your specialist or Parkinsons nurse. It is important to change injection site to minimise scarring or infection. Simple massage, silicone gel patches or ultrasound can help to reduce any nodules that form.
How Anticholinergics Are Used
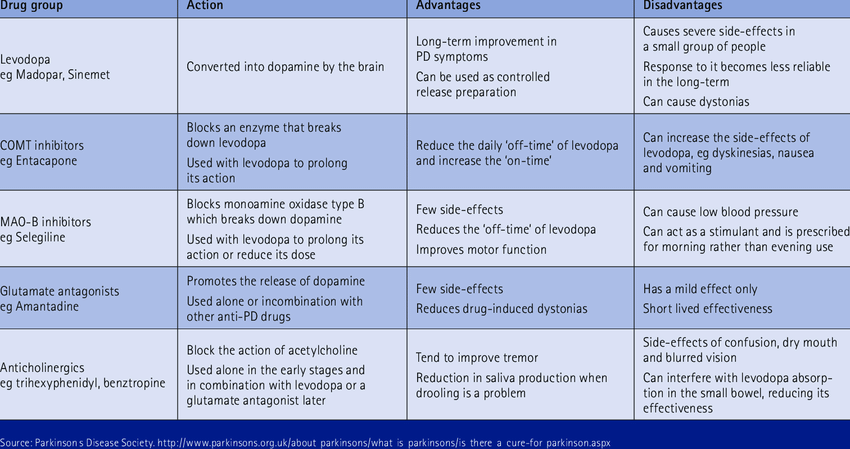
These medications are older and are not used very often for Parkinsons today. Sometimes they are prescribed for reducing tremor and muscle stiffness. They can be used on their own, especially in the early stages of your Parkinsons when symptoms are mild, before levodopa is prescribed.
Anticholinergics can also be used with levodopa or a glutamate antagonist. They are taken as tablets or as a liquid.
Don’t Miss: Parkinson’s Disease Causes Symptoms And Treatment
Withdrawal Syndrome With Levodopa
Research has shown that withdrawal symptoms can happen when someone very suddenly stops taking levodopa, perhaps because they are experiencing impulsive and compulsive behaviour. It can lead to symptoms such as depression, anxiety and pain. Any withdrawal from Parkinsons medications needs to be done gradually, under the supervision of a health professional, to avoid the risk of developing this syndrome.
Treating Parkinsons With Complementary Medicine
Complementary medicine incorporates many different practices that can be used alongside conventional medicine to try to ease PD symptoms. There is typically not as much rigorous data to support the use of complementary medicine techniques, as compared to conventional medicine, but many patients find them helpful. These include yoga and massage.
Also Check: Symptoms Of Parkinson Disease Webmd
What Should I Know About Parkinsons Disease And Medications
There have been rapid and remarkable changes over the past decade in treating Parkinsons disease . The development of new medicines and the understanding of how best to use them and the older drugs have significantly improved the quality of life for people with the disease.
There is currently no treatment that has been proven to affect the disease progression or development of medication that can slow the disease process. There are two general approaches to the treatment of PD improve the symptoms with medications and engage in physical therapy. Most patients with PD can be adequately treated with medicines that alleviate their symptoms. For the approximately 15% of patients for whom medicines are not sufficiently effective, new, highly effective, and safe surgical treatments are available.
Choices about medicines made early in the course of the disease have a strong impact on the long-term course of the illness. Therefore, you should seek the advice of doctors specially trained in treating PD even when the illness is only suspected. Movement disorders specialists are neurologists who have completed their training in neurology and have received special advanced training in treating PD and other related diseases.
Positive Results In Hand Abbvie Eyes Potential Approval For Parkinsons Treatment
AbbVies experimental subcutaneous Parkinsons disease drug ABBV-951 hit the mark in a 12-week Phase III study in patients with an advanced form of the disease. The company announced that patients who received daily doses of the drug showed statistically significant increases in On time without dyskinesia, the spasms associated with the disease.
AbbVies Phase III study compared ABBV-951 to oral treatment with levodopa/carbidopa. In addition to the increases in On time hours, AbbVie said the study also showed a significant reduction in Off time hours. People diagnosed with Parkinsons often deal with times classified as On and Off. The On time refers to when patients are responding to medication and symptoms are decreased. The Off periods are characterized by the re-emergence of Parkinsons symptoms. As the disease progresses, Off periods in patients can increase in frequency and severity.
With the positive Phase III data in hand, AbbVie is eying global regulatory submissions for ABBV-951, a solution of levodopa and carbidopa prodrugs for continuous subcutaneous infusion. Dr. Michael Severino, vice chairman and president of AbbVie, said the results of the Phase III study highlight the potential for ABBV-951 as a treatment for advanced Parkinsons disease patients.
AbbVie said full results from the Phase III study would be presented at a future medical meeting or submitted for publication in a peer-reviewed journal.
You May Like: Judy Woodruff Parkinson’s Disease
Treatment Of Late Stage Complications Of Parkinson’s Disease
Postural hypotension
Levodopa and dopamine agonists worsen postural hypotension and it may be necessary to lower the dose of levodopa or withdraw the agonist. Treatment is difficult, but patients should be advised to sleep with the head of the bed raised by one or two bricks and to add salt to their diet. Fludrocortisone can then be added at a dose of 0.1 mg in the morning, increasing if necessary up to 0.5 mg in the morning. If these measures are ineffective, the alpha agonist midodrine 10-20 mg four hourly can be useful but it is experimental and only available via the Special Access Scheme. Patients treated for postural hypotension need to have electrolytes, renal function and supine blood pressures closely monitored.
Parkinsonian psychosis, depression and dementia
Psychotic symptoms such as visual hallucinations and persecutory delusions occur most commonly in the setting of dementia, which may be mild and therefore easily missed. Most drugs for Parkinson’s disease make these symptoms worse. Depression is also common and requires treatment in its own right.
Finding The Right Medication
Finding the right medication to treat your Parkinson’s symptoms is a process that takes time and effort from you and your doctor. Parkinson’s medications work in different ways. Many are pills that you swallow, but some can be given through skin patches or intestinal infusions. It can sometimes feel like “trial and error” to figure out the best medication, dose and schedule to treat your symptoms. Over time, as symptoms progress or complications arise, your doctor may adjust your medications. This might mean changing your dose or how often you take a drug, or adding or switching medications. Staying in tune with your symptoms and which are most bothersome, and keeping track of how well medication is or is not working can help direct adjustments to your treatment regimen.
Here we describe the different categories of Parkinson’s medications how they work, their potential benefits and common side effects. We also give examples and highlight therapies that have been approved in the last few years with an asterisk.
Recommended Reading: Is Drooling A Sign Of Parkinson’s Disease
How Anticholinergics Work
These medications block the action of acetylcholine, a chemical messenger that is found in your body. Acetylcholine helps to send messages from your nerves to your muscles.
In the brain, there is normally a balance between the activity of dopamine and the activity of acetylcholine. But in Parkinsons a deficiency in the brain of the neurotransmitter dopamine causes over-activity of acetylcholine. Anticholinergics work by blocking acetylcholines activity to restore this balance and help reduce your Parkinsons symptoms.
What Are The Causes
Drug-induced parkinsonism is caused by medications that reduce dopamine levels in the brain. Dopamine is a neurotransmitter that works to control bodily movements.
Dopamine is also part of the brains reward system. It helps you feel pleasure and enjoyment, and it supports your ability to learn and focus.
Medications that bind to and block dopamine receptors are called dopamine antagonists. These medications arent used to treat Parkinsons disease. Rather, theyre used to treat other conditions that might seriously impact your quality of life.
If your doctor has prescribed a medication that causes unwanted side effects, you may have options. You may also decide that the side effects are worth it if the medication effectively treats your condition.
Some medications that cause drug-induced parkinsonism include:
Recommended Reading: Symptoms Of Parkinsons In Women
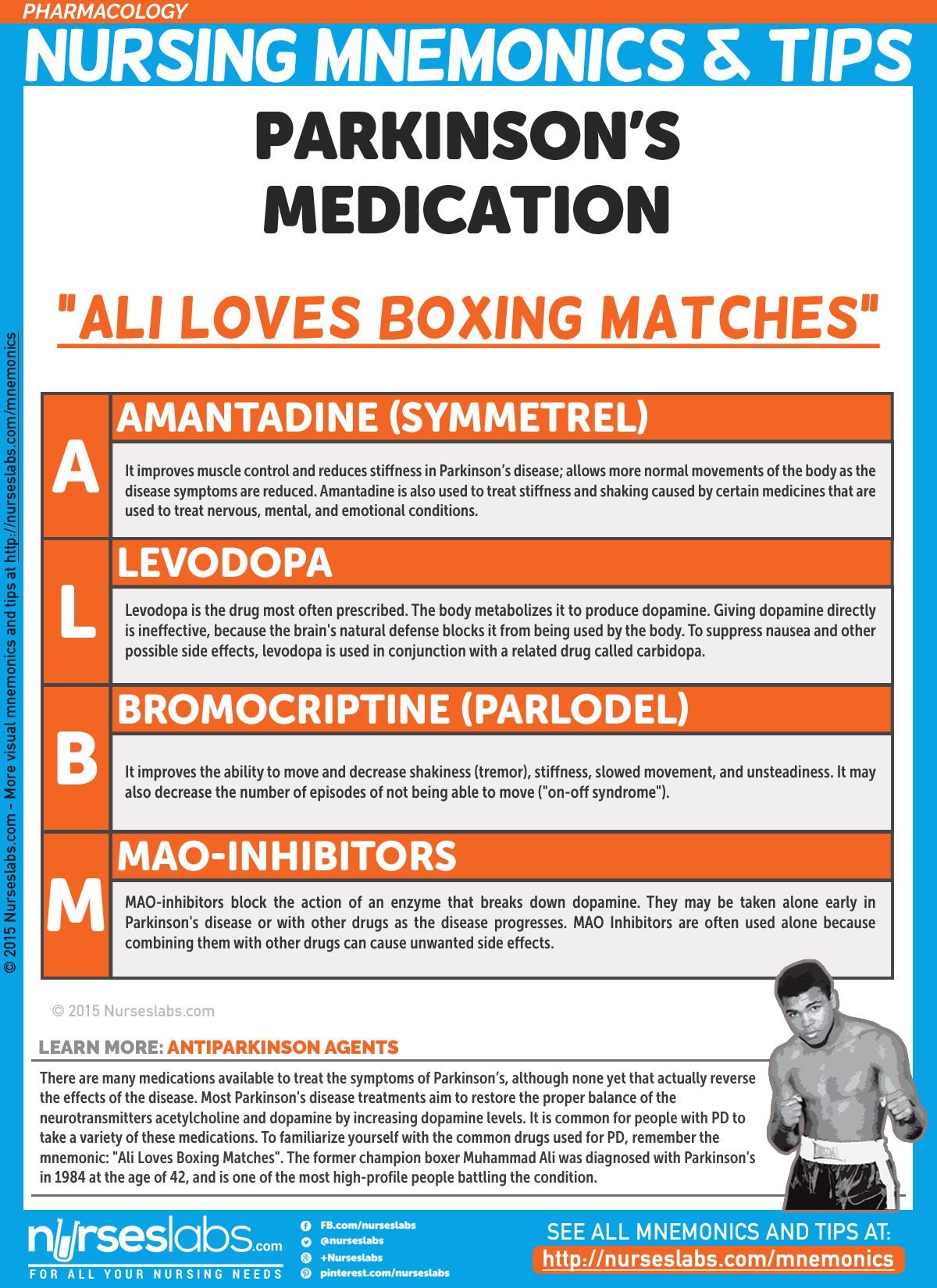
Common Drugs For Parkinson’s Disease
Levodopa and carbidopa . Levodopa is the most commonly prescribed medicine for Parkinsonâs. Itâs also the best at controlling the symptoms of the condition, particularly slow movements and stiff, rigid body parts.
Levodopa works when your brain cells change it into dopamine. Thatâs a chemical the brain uses to send signals that help you move your body. People with Parkinsonâs donât have enough dopamine in their brains to control their movements.
Sinemet is a mix of levodopa and another drug called carbidopa. Carbidopa makes the levodopa work better, so you can take less of it. That prevents many common side effects of levodopa, such as nausea, vomiting, and irregular heart rhythms.
Sinemet has the fewest short-term side effects, compared with other Parkinsonâs medications. But it does raise your odds for some long-term problems, such as involuntary movements. An inhalable powder form of levodopa and the tablet istradefylline have been approved for those experiencing OFF periods, OFF periods can happen when Parkinsonâs symptoms return during periods between scheduled doses of levodopa/carbidopa.
People who take levodopa for 3-5 years may eventually have restlessness, confusion, or unusual movements within a few hours of taking the medicine. Changes in the amount or timing of your dose will usually prevent these side effects.
Dopamine agonists. These drugs act like dopamine in the brain. They include pramipexole , rotigotine , and ropinirole , .
What Future Medications May Be Available For Parkinsons
There are numerous studies investigating new treatments for Parkinsons disease.
There has been new information about the role of autoimmunity and T-cells in the development of Parkinsons disease, possibly opening the door to a role for biologics.
Stem cells are also being investigated as a treatment option for Parkinsons disease.
Also Check: What Causes Pain In Parkinson’s Patients
Speech And Occupational Therapy
Parkinsons disease can lead to slurred speech and difficulty swallowing. A speech and language therapist can provide muscle training techniques that may help overcome some of these problems.
An occupational therapist can help identify everyday tasks that can be challenging and work with the person to find practical solutions.
This may include new strategies for dressing, preparing meals, performing household chores, and shopping. Adaptations to the home environment can also make daily living easier.
For people with Parkinsons disease, deep brain stimulation may help manage:
- tremor
- an electrode inside the part of the brain that controls movement
- a pacemaker-like device, or neurostimulator, under the skin in the upper chest
- a wire under the skin connecting the neurostimulator to the electrode
The neurostimulator sends electrical impulses along the wire and into the brain via the electrode. These impulses can prevent symptoms by interfering with the electrical signals that cause them.
There is a small risk of brain hemorrhage, infection, and headaches. Some people may see no improvement, or their symptoms may worsen. There may also be discomfort during stimulation.
Nevertheless, the AAN considers this treatment safe and effective for specific people and say any adverse effects are usually mild and reversible. Anyone considering this treatment should discuss the pros and cons with a healthcare professional.
Impulsive And Compulsive Behaviour
A small number of people taking levodopa have problems with impulsive or compulsive behaviour. This can also be called impulse control disorder. It affects a much smaller percentage of people taking levodopa than those taking dopamine agonists, but it is still a possible side effect. Further information is available at Compulsive and impulsive behaviour.
Another potential problem is dopamine dysregulation syndrome, where someone with Parkinsons might be tempted to take more of their Parkinsons medication than they are prescribed. If you think this is happening to you or the person you are caring for, tell your GP, specialist or Parkinsons nurse right away.
It is important that all people with Parkinsons are monitored for any potential risk of impulsive and compulsive behaviour while being treated with levodopa.
People with Parkinsons, their carers, friends and family members should work with healthcare professionals to monitor any changes in behaviour. If you start to experience these symptoms, you should discuss it with your specialist or Parkinsons nurse immediately. You should not stop taking the medication.
Recommended Reading: Microbiome Diet For Parkinson’s Disease
Antipsychotic Use In The Elderly
Antipsychotic agents are frequently used in facilities for the elderly and in general hospitals to treat older patients with behavioral problems, which are not uncommon. In nursing home facilities, behavioral disturbances are seen in as many as 40% to 95% of residents40% to 80% with dementia, 5% to 25% with depression, and 2% to 5% with schizophrenia. However, although approximately 50% to 75% of all nursing home residents take antipsychotic medications, only a relatively small proportion of residents actually see a mental health professional. In a study of the availability of mental health services in nursing homes, data indicated that 65% of nearly 2000 nursing home residents were found to have some type of mental disorder yet, the 1-month rate of contact with mental health professionals for this group was only 4.5%. Additionally, only 2% with a diagnosis of dementia and 17% of residents diagnosed with chronic schizophrenia had seen a mental health specialist.
Educational programs designed for primary care physicians and specialists such as nurses, psychologists, and social workers, as well as patients and their families, are clearly needed to achieve safer and more efficacious care for elderly patients. Learning to identify, distinguish, and manage drug-induced movement disorders associated with conventional, and sometimes atypical, antipsychotic agents can aid primary care physicians and others in achieving that end.
Mechanism Of Action Of Available Drugs
The major classes of drugs currently available for the treatment of idiopathic Parkinson’s disease are shown in Table 1. Many aim to increase dopamine in the brain, by increasing its production or altering its metabolism .
|
Table 1 |
Drugs with alter metabolism in boxed red italics
Levodopa
Levodopa is absorbed from the small intestine and transported into the brain where it is converted to dopamine. Levodopa has a short plasma half-life of about one hour. Early in Parkinson’s disease, levodopa has a long duration of action which is independent of plasma concentration, but as the disease progresses, the duration of the effect reduces. The short-duration effect is strongly linked to plasma concentration and lasts, at most, hours.
Slow-release preparations are gradually absorbed, resulting in more sustained plasma concentrations. They have reduced bioavailability higher doses are required to match the benefit of an equivalent strength of a standard preparation. Rapid release preparations are taken in liquid form to enhance passage through the stomach and absorption from the small intestine.
Dopamine agonists
Apomorphine is a potent emetic so patients must be pre-treated with domperidone 20 mg three times daily orally for at least 48 hours before the first injection. Domperidone should be continued for at least a few weeks once regular intermittent treatment has commenced. The dose can then be tapered slowly as tolerance to the emetic effects of apomorphine usually develops.
Don’t Miss: Young Onset Parkinson’s Symptoms