What Are The Symptoms Of Parkinson’s Disease
The most noticeable symptoms of PD are movement-related, and the hallmark symptoms are: bradykinesia, resting tremor, and rigidity.
Bradykinesia refers to slowness of movement—especially slowness of the initiation of movement. PD patients will often have trouble getting their body to transition from a resting state to an active state. When they finally do get moving, their movement may be much slower than a healthy patient’s.
Resting tremor indicates a tremor that is worse when the patient is at rest. When the patient makes a voluntary movement, the intensity of the tremor often subsides. These tremors typically start in the hands or arms and then spread to the legs as the disease progresses.
Rigidity describes a state of generally elevated muscle tone where the patient displays inflexibility and resistance to movement .
Although these movement-related symptoms are the most familiar signs of PD, there are a number of other common symptoms that occur as well. For example, later in the disease, postural instability becomes common, making falls more likely. Some of the non-motor symptoms include constipation, deficits in the sense of smell, sleep abnormalities, mood disorders like depression and anxiety, cognitive impairment, and dementia.
Conclusions And Future Directions
Volumes of research have highlighted the unique contributions of the basal ganglia and medial temporal lobes to learning and memory. However, some of the resulting characterizations, such as assigning implicit and explicit learning and memory to these systems, have turned out to be oversimplified. Moreover, a focus on assigning unique attributes to these two systems has overlooked the many ways in which these brain regions jointly contribute to behavior. Converging evidence from electrophysiology, neuroimaging, computational modeling, and neuropsychology, and, moreover, communication between these fields, have advanced a more integrated view of basal ganglia function. Paradigms that translate across varied approaches have been key in developing the emerging view of basal ganglia function, and the study of learning in Parkinson’s disease patients has been integral to this progress. This integrative approach will help provide the next critical steps towards advancing our view of how the basal ganglia interact with the medial temporal lobes and other brain systems, as well as promote an understanding of the role of dopamine and other neuromodulators in multiple brain systems for learning and memory.
Parkinsons In The Brain
In the present study, a team led by researchers from the University of California San Diego in La Jolla wanted to contribute to this knowledge.
They conducted a study in mice to understand the relationship between neural circuits in the brain and some of the functions that are typically affected by Parkinsons disease, such as cognitive and motor abilities.
They looked in particular at the external globus pallidus in the brains of mice, which previous research has linked to the motor symptoms of Parkinsons.
The researchers used multiple methods to give a more detailed overview of this region of the mices brains, including electrophysiology, viral tracing, and behavioral experiments.
Don’t Miss: Parkinson’s Quality Of Life
Causes Of Parkinson’s Disease
Parkinson’s disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Degeneration Of Neurotransmitter Systems
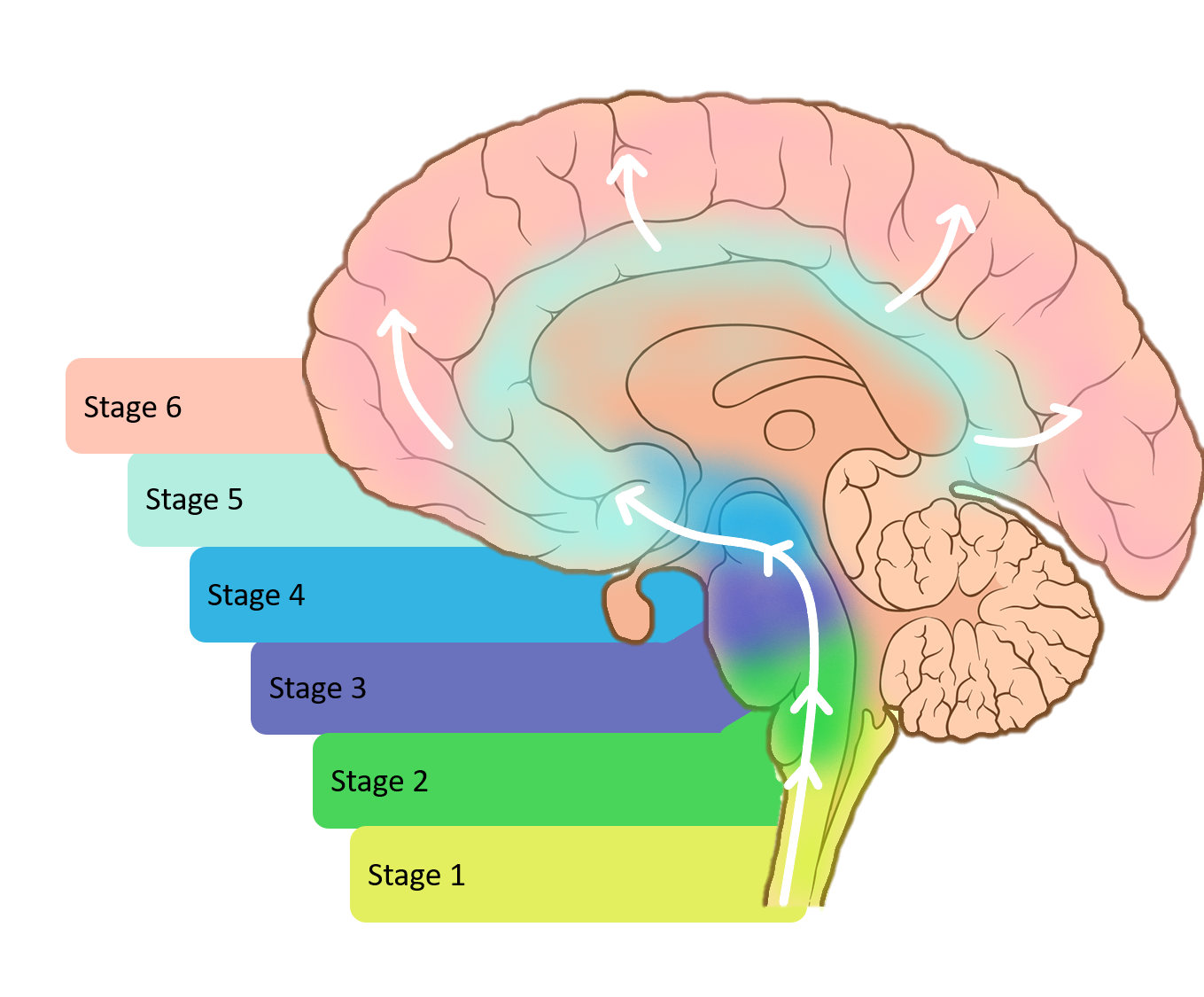
More widespread dopaminergic deficits in the brain
By definition, all patients with PD have a moderate-to-severe loss of dopaminergic neurons in the nigrostriatal projection pathway. More widespread degeneration of dopaminergic terminals in the striatum particularly denervation of dopaminergic terminals in the associative dorsal caudate nucleus occurs in those with PD-MCI than in those with PD without cognitive impairment . However, in patients with PD-MCI, there is relative preservation of other dopaminergic systems in the brain, whilst those with PDD have a considerable loss of the lateral dopaminergic system to frontal, parietal and temporal cortical regions . In healthy individuals, cortical dopamine modulation can boost working memory as well as visuospatial and attentional processing, and promotes cognitive effort,, suggesting a key role for dopamine in cognitive function.
Fig. 2: Neurotransmitter deficits associated with cognitive decline in PD and DLB.
Noradrenergic locus coeruleus and sympathetic systems
Basal forebrain cholinergic systems
Serotonergic dysfunction is not directly related to cognitive decline
You May Like: Does Parkinson’s Cause Swelling
What Causes Parkinsons Disease Dementia
A chemical messenger in the brain called dopamine helps control and coordinate muscle movement. Over time, Parkinsons disease destroys the nerve cells that make dopamine.
Without this chemical messenger, the nerve cells cant properly relay instructions to the body. This causes a loss of muscle function and coordination. Researchers dont know why these brain cells disappear.
Parkinsons disease also causes dramatic changes in a part of your brain that controls movement.
Those with Parkinsons disease often experience motor symptoms as a preliminary sign of the condition. Tremors are one of the most common first symptoms of Parkinsons disease.
As the disease progresses and spreads in your brain, it can affect the parts of your brain responsible for mental functions, memory, and judgment.
Over time, your brain may not be able to use these areas as efficiently as it once did. As a result, you may begin experiencing symptoms of Parkinsons disease dementia.
You have an increased risk of developing Parkinsons disease dementia if:
- youre a person with a penis
- youre older
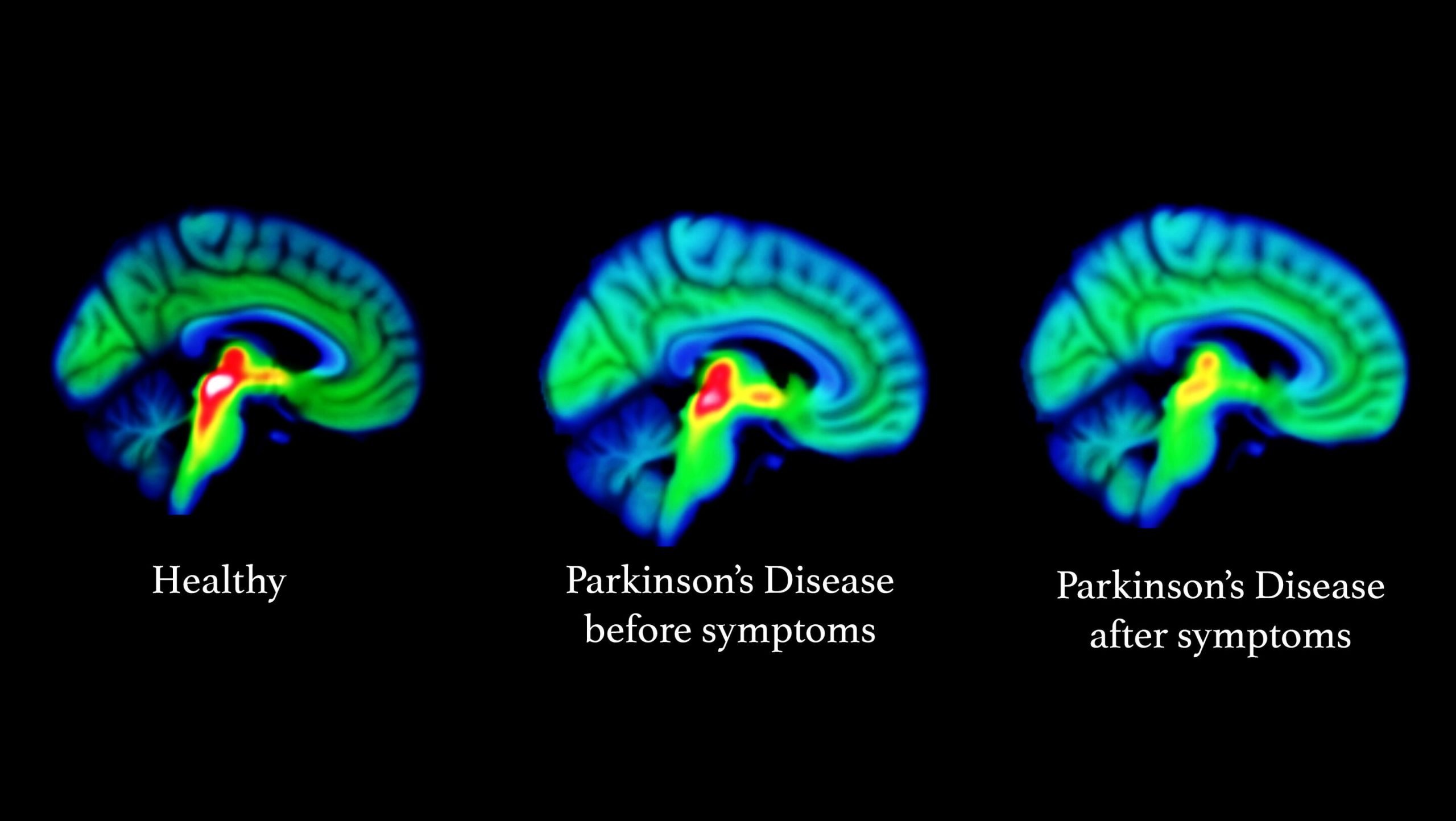
How Parkinsons Disease Affects The Brain
The Parkinson’s disease brain stops producing dopamine cells, which in turn causes problems with movement and coordination known as motor symptoms. We all have a basic understanding of how Parkinson’s disease affects the brain, but what really happens when someone has Parkinson’s disease? Let’s explore the facts surrounding the Parkinson’s disease brain and how it differs from a normal, “healthy” brain.
Also Check: How To Improve Walking With Parkinson’s
Relation Of The Neural Network Perspective To The Neuropathology Of Parkinsons Disease Dementia
At the neuropathological level the consensus from most studies to date is that the amount of Lewy-related pathology in neocortical and limbic areas is the most important factor in the development of PDD . However, the significance of Lewy-related pathology occurrence in particular cortical areas is debated, for example one retrospective autopsy study found that severity of cognitive decline in PDD correlated with Lewy-related pathology in the frontal and cingulate gyri , while another found no significant correlations in these regions but did find one in relation to temporal lobe Lewy-related pathology . Meanwhile some patients with Parkinsons disease with cortical Lewy-related pathology do not develop dementia at all . The significance of concurrent Alzheimer-type pathologies is hotly debated , although a recent study quantitatively assessing cortical Lewy-related pathology and Alzheimer-type pathologies found that a combination of both correlated most robustly with development of PDD . The relative contributions of other pathologies including microvascular disease, cerebral amyloid angiopathy, argyrophilic grains and TARDBP remain unclear .
Want To Learn More About The Latest Research In Parkinsons Disease Ask Your Questions In Our Research Forum
Cognitive impairment can occur due to stress, particularly if the patient feels they are a burden to their caregiver, are experiencing a decline in daily functioning, have a worsening quality of life, are dealing with rising medical costs, or are concerned about their mortality.
According to the National Parkinson Foundation, some of the common cognitive issues people living with Parkinsons disease face include:
- Slowness of thinking
- Struggling to find the right words in conversations
- Lack of reasoning skills
Some Parkinsons disease medications can help with areas such as motivation and concentration, but there are no medications that can improve memory function.
MORE:How does Parkinsons disease affect the brain?
Parkinsonss News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Read Also: Ultrasound Treatment For Parkinson’s Disease
Prognostic Factors For Development Of Parkinsons Disease Dementia
In the clinic the diagnosis of PDD is based upon the Movement Disorders Society Task Force criteria , which incorporates detection of the cognitive features described above. However, it is recognized that early identification of patients at risk of developing PDD is useful in order to monitor them more closely so that therapeutic and supportive strategies can be implemented at a stage of the disease when they are likely to have greatest efficacy. Detailed neuropsychological testing, although able to detect early subclinical deficits, is not widely available, and therefore identification of clinical features with high predictive value for PDD has pragmatic value for clinicians. Large longitudinal cohort studies have demonstrated that inability to copy the intersecting pentagons figure on the MMSE, impairments of semantic verbal fluency and recognition memory, and development of a postural instability and gait difficulty motor phenotype are significant predictors for PDD . Errors on the Pill Questionnaire and presence of REM sleep behavioural disorder are also associated with later development of PDD, although their positive predictive values are lower .
What Happens In Pdd
People with PDD may have trouble focusing, remembering things or making sound judgments. They may develop depression, anxiety or irritability. They may also hallucinate and see people, objects or animals that are not there. Sleep disturbances are common in PDD and can include difficulties with sleep/wake cycle or REM behavior disorder, which involves acting out dreams.
PDD is a disease that changes with time. A person with PDD can live many years with the disease. Research suggests that a person with PDD may live an average of 57 years with the disease, although this can vary from person to person.
Also Check: Parkinson’s Disease Research Paper
Care Partners: Burden Assessment And Support
Care partners or caregivers are an invaluable healthcare resource. When caregivers are present, patients are less likely to move to nursing homes. Caregivers also improve participation rates and retention of people with PD in research studies, which helps advance the path towards finding more effective therapeutics. Furthermore, many clinical trials for PDD require a caregiver in the study inclusion criteria.
Informal caregivers are providers who supervise or assist with instrumental and/or basic activities of daily living without pay to someone who cannot do these activities independently due to cognitive, physical, or psychological impairment. However, caregivers provide much more than this formal definition states. They often provide medical care including administration of medications, emotional and social support, and advice on medical decision-making. About 90% of men and 80% of women with PD have caregivers during their physician visits, and most caregivers are spouses.
Despite existing therapeutic support and resources for caregivers, there are several challenges to overcome. These include sex disparities in caregiving and the substantial financial strain that can be associated with caregiving. Caregivers are frequently at the forefront of providing medical history and administering complicated medication regimens without formalized education or support.
Management Of Parkinsons Disease Dementia
The relative importance of cholinergic network dysfunction in PDD is reflected in current treatment strategies, which focus on the use of AChEIs, such as rivastigmine, donepezil and galantamine, to boost cholinergic function. Two large placebo-controlled trials have shown that rivastigmine significantly improves deficits in orienting of attention, vigilance and cognitive fluctuation in patients with PDD , and indeed patients with more severe attentional deficits appear to respond best . These results serve to reinforce the cholinergic basis of attention deficits in PDD according to the neural network model. Benefits from AChEIs have also been demonstrated for executive deficits visuospatial tasks and hallucinations . Whether these improvements are due to amelioration of the cholinergic network deficits underlying these cognitive processes, or are secondary to an overall improvement in attention assisting other overlapping cognitive functions, or a combination of both, is unknown.
Don’t Miss: Why Does Parkinson’s Cause Hallucinations
What Are The Surgical Treatments For Parkinsons Disease
Most patients with Parkinsons disease can maintain a good quality of life with medications. However, as the disease worsens, medications may no longer be effective in some patients. In these patients, the effectiveness of medications becomes unpredictable reducing symptoms during on periods and no longer controlling symptoms during off periods, which usually occur when the medication is wearing off and just before the next dose is to be taken. Sometimes these variations can be managed with changes in medications. However, sometimes they cant. Based on the type and severity of your symptoms, the failure of adjustments in your medications, the decline in your quality of life and your overall health, your doctor may discuss some of the available surgical options.
Executive Dysfunction In Parkinsons
Executive functions in cognition are higher-order mental processes, including the ability to plan, organize, initiate and regulate behavior to meet goals. Executive functioning is present in activities such as multitasking, switching tasks, and solving problems. The prefrontal cortex of the brain and the dopamine system are responsible for executive function. As PD damages these areas, executive dysfunction occurs, and executive dysfunction is one of the most common cognitive impairments found in people with PD.3,4
Also Check: Parkinson’s Disease Causes Symptoms And Treatment
Behaviors Seen In Parkinsons Disease Dementia
As dementia progresses, managing disorientation, confusion, agitation, and impulsivity can be a key component of care.
Some patients experience hallucinations or delusions as a complication of Parkinsons disease. These may be frightening and debilitating. Approximately 50 percent of those with the disease may experience them.
The best thing to do when giving care to someone experiencing hallucinations or delusions from Parkinsons disease dementia is to keep them calm and reduce their stress.
Take note of their symptoms and what they were doing before they exhibited signs of hallucinating and then let their doctor know.
This element of the disease can be particularly challenging for caregivers. Patients may become unable to care for themselves or be left alone.
Some ways to make caregiving easier include:
- sticking to a normal routine whenever possible
- being extra comforting after any medical procedures
- limiting distractions
- using curtains, nightlights, and clocks to help stick to a regular sleep schedule
- remembering that the behaviors are a factor of the disease and not the person
Multiple Memory Systems: Understanding The Role Of The Basal Ganglia
Extensive converging evidence indicates that long-term memory is not unitary, but instead consists of multiple cognitive processes that rely on discrete neural systems and are governed by distinct learning rules and forms of plasticity . This concept, often referred to as the multiple memory systems framework, originated from neuropsychological research with patients with specific patterns of brain damage. As discovered with the famous case of patient H.M., damage to the hippocampus and surrounding medial temporal lobe cortices led to a severe impairment in declarative memory â that is, an inability to form new memories for facts and events . Notably, this devastating amnesia was selective: H.M. and other individuals with hippocampal damage remained able to learn new procedures and habits that were acquired gradually, such as playing the piano or developing diagnostic skills as a radiologist.
Also Check: Parkinson’s Age Of Onset
Executive Dysfunction Is Due To Disruption Of The Fronto
The prefrontal cortices are implicated in executive function , and distinct areas of prefrontal cortex have strong functional connections with the striatum via parallel dopamine-dependent cortico-striatal loops . Functional MRI imaging in patients with Parkinsons disease relates executive impairments on set shifting and working memory tasks to hypo-activation within the fronto-striatal loops connecting dorsolateral and ventrolateral prefrontal cortices, striatum and thalamus . However, such hypo-activation was only present during task phases that specifically required co-activation with the striatum in controls, indicating that striatal dysfunction was the determining factor in executive impairment in Parkinsons disease rather than frontal dysfunction. Both the globus pallidus internus and caudate are heavily affected by dopaminergic degeneration , and PET studies have specifically implicated dysfunction of these two structures in interruption of normal processing in the fronto-striatal network for example, patients with Parkinsons disease demonstrating executive impairments on tasks involving planning or random number generation show significantly altered outflow activity from the pallidum to the frontal cortices. In addition, other studies have shown strong correlations between dopamine depletion in the head of the caudate and deficits on executive tasks such as object alternation and the Stroop Test .
Cognitive Problems And Parkinsons
Many people with Parkinsons experience some mild memory loss and thinking problems. Symptoms vary widely and may fluctuate through the day. Research has shown that cognitive problems tend to be more severe in people with Parkinsons with more pronounced bradykinesia and rigidity, and less severe in those with more pronounced tremor.
If you are experiencing changes in your thinking and mental abilities, its natural to be concerned. You may worry you could go on to develop dementia however, this happens to comparatively few people. One study found that after ten years with Parkinsons, 80% of people with the condition experienced some cognitive difficulties, but less than 20% had developed dementia – known as Parkinsons disease dementia . The symptoms of PDD are very different from those of Alzheimers disease.
Some Parkinsons symptoms can make speech and facial communication difficult, and slowed thinking will often make things even harder. As the ability to remember words is affected, your vocabulary can become limited and humour may be less understood. It can also get harder to follow conversations, and this can result in you not making sense, or forgetting what you have said and repeating things.
Don’t Miss: Can You Be Tested For Parkinson’s