What Are Atypical Parkinsonian Disorders
Atypical Parkinsonian disorders are progressive diseases that present with some of the signs and symptoms of Parkinsons disease, but that generally do not respond well to drug treatment with levodopa. They are associated with abnormal protein buildup within brain cells.
The term refers to several conditions, each affecting particular parts of the brain and showing a characteristic course:
- Dementia with Lewy bodies, characterized by an abnormal accumulation of alpha-synuclein protein in brain cells
- Progressive supranuclear palsy, involving tau protein buildup affecting the frontal lobes, brainstem, cerebellum and substantia nigra
- Multiple system atrophy, another synucleinopathy that affects the autonomic nervous system , substantia nigra and at times the cerebellum
- Corticobasal syndrome, a rare tauopathy that typically affects one side of the body more than the other and makes it difficult for patients to see and navigate through space
Parkinsonism Vs Parkinsons: Whats The Difference
If you or a loved one are living with Parkinsons disease, youve likely heard the term parkinsonism but you may not know how it differs from Parkinsons. Getting very confused about the difference between Parkinsons and parkinsonism, wrote one MyParkinsonsTeam member.
Parkinsons disease is a brain condition that advances slowly over time in the majority of people. The condition involves the loss of brain cells in a part of the brain called the substantia nigra. The substantia nigra makes a chemical called dopamine, which plays a role in body functions including memory, movement, and pleasure. As these dopamine-producing neurons decrease in number, Parkinsons symptoms begin to appear.
Parkinsonism is a broad term referring to several neurological conditions with movement issues including Parkinsons disease. Types of parkinsonism other than Parkinsons disease are sometimes referred to as Parkinsons plus or atypical Parkinsons disease. Around 85 percent to 90 percent of diagnosed cases of parkinsonism are types other than Parkinsons disease.
Despite their differences, the various types of parkinsonism including Parkinsons disease share some common signs and symptoms. As a result, they sometimes can be misdiagnosed as a different type.
Postsynaptic Dopamine D2 Receptor
In drug-naïve PD patients compared to controls, binding potential for the G-protein-coupled dopamine D2 receptors measured using 11C-raclopride PET may appear normal or upregulated contralateral to the clinically affected side . Similarly, striatal dopamine D2 receptor upregulation was observed in drug-naïve PD patients using SPECT ligands probably suggesting compensatory changes secondary to nigrostriatal denervation, with higher upregulation detected in the posterior putamen . In medicated PD cases, postsynaptic D2 receptor binding was reduced or within the normal range compared to controls in PET and SPECT studies . Normal D2 binding potential was also observed in patients with DLB and essential tremor , while reductions were reported in atypical PS cases .
In PSP vs. controls, reduced D2 receptor binding was detected in PET and SPECT studies . Likewise, D2 binding reductions were noted in MSA patients compared to PD and controls correlating with striatal glucose hypometabolism . In CBS, studies typically show preservation of postsynaptic D2 receptors, although inconsistently, which is not surprising given the pathologic heterogeneity evident in this disorder .
Read Also: Psilocybin And Parkinson’s Disease
Whats The Difference Between Multiple System Atrophy And Parkinsons
Parkinsons and MSA both affect the movement control system and the involuntary autonomic control system and early symptoms can make a differential diagnosis a challenge. MSA, however, tends to progress faster than Parkinsons balance problems and a stooped posture happen earlier and get worse more quickly with MSA and autonomic functions such as blood pressure, heart rate, breathing, sweating, bladder function, and sexual problems are more severe in people with MSA.
For more information on multiple symptom atrophy, read this fact sheet.
Parkinsons Syndrome Vs Parkinsons Disease
In a recent poll of individuals with Parkinsons disease, more than one in four participants reported having been misdiagnosed. Obtaining an accurate diagnosis is fundamental to receiving appropriate and effective treatment however, many conditions can mimic Parkinsons disease.
Here is a quick breakdown of Parkinsons syndrome vs. Parkinsons disease.
Also Check: Parkinson’s Masked Face Images
Is Rls More Common In Pd
But what about the other possibility? Do patients with PD have an increased risk of RLS over the general population? Is it the same RLS as the person without PD has, or is it different? These questions have been difficult to answer. Of course, since PD affects about 1.5% of the elderly, and RLS in about 4-10% of the population, there will be some coincidental overlap. In addition to this however, patients with PD can have sensations that feel like RLS when their dose of dopamine medication is wearing off. These sensations are not truly RLS since they do not have the key features of RLS described above and fluctuate with medication timing, but they can be easily confused with RLS by the person with PD.
Studies of people with PD that assess for RLS and compare to a control group are hindered by the fact that the majority of patients with significant PD are under treatment with medications that affect RLS. Over the years, there have been multiple studies investigating whether RLS is more common in PD than in the general population. Different studies come to different conclusions. Studies conducted in which a group of people with PD are directly compared to a group of people without PD typically show that RLS is more common in PD than the general population.
About Paula Mcfeely Wiener Msw Lcsw
Paula is a licensed clinical social worker and senior information specialist with the Parkinsons Foundation. Since receiving her MSW in 1995, she has worked almost exclusively with the senior population. Her experience includes being a center coordinator for a Parkinsons Foundation Center of Excellence, leading a number of PD support groups, educating patients, families, and health care professionals about the disease, and answering questions on the Helpline for 12 years. Paula is passionate about improving understanding and care for people with Parkinsons disease and their family members. Paulas father was diagnosed with atypical parkinsonism which gave her a very personal understanding of what patients and families with this diagnosis go through.
Don’t Miss: What Are The Odds Of Getting Parkinson’s Disease
When Its Not Parkinsons Disease
In those cases where Levodopa doesn’t help with Parkinsons symptoms, its usually because the symptoms arent caused by neuron death in the brain but by external factors. These factors include any of the following:
- Medications prescribed for psychosis, psychiatric disorders, or nausea
- Exposure to environmental toxins
- Multiple instances of head trauma
- Fluid build up around the brain, or brain tumors or lesions
- Metabolic disorders, chronic liver failure, or Wilson’s disease
How Do Doctors Diagnose Parkinsonism
No single test exists for doctors to diagnose Parkinsonism.
A doctor will start by taking a persons health history and review their current symptoms. They will ask for a medication list to determine if any medicines could be causing the symptoms.
A doctor will likely also order blood testing to check for underlying potential causes, such as thyroid or liver problems. A doctor will also order imaging scans to examine the brain and body for other causes, such as a brain tumor.
Doctors can perform a test that tracks the movement of dopamine in the brain. This is known as the DaT-SPECT test.
The test uses radioactive markers designed to track dopamine in the brain. This allows a doctor to watch the release of dopamine in a persons brain and identify the areas of the brain that do or do not receive it.
Because Parkinsonism does not respond to typical treatments and can have a variety of symptoms, doctors can have difficulty coming to a quick diagnosis. It may take time for doctors to rule out other conditions and begin to make treatment recommendations.
You May Like: Healed From Parkinson’s Disease Naturally
Whats The Difference Between Dementia With Lewy Bodies And Parkinsons
In dementia with Lewy bodies, dementia always appears first. There can also be changes in alertness as well as visual hallucinations. However, because of the presence of Lewy bodies throughout the entire brain, characteristics of this disease not only include cognitive characteristics, but also physical, sleep, and behavioral changes. As the disease progresses, the motor symptoms common to Parkinsons such as tremor, slowness, stiffness, and walking and balance problems will appear.
For more information on dementia with Lewy bodies, visit www.lbda.org.
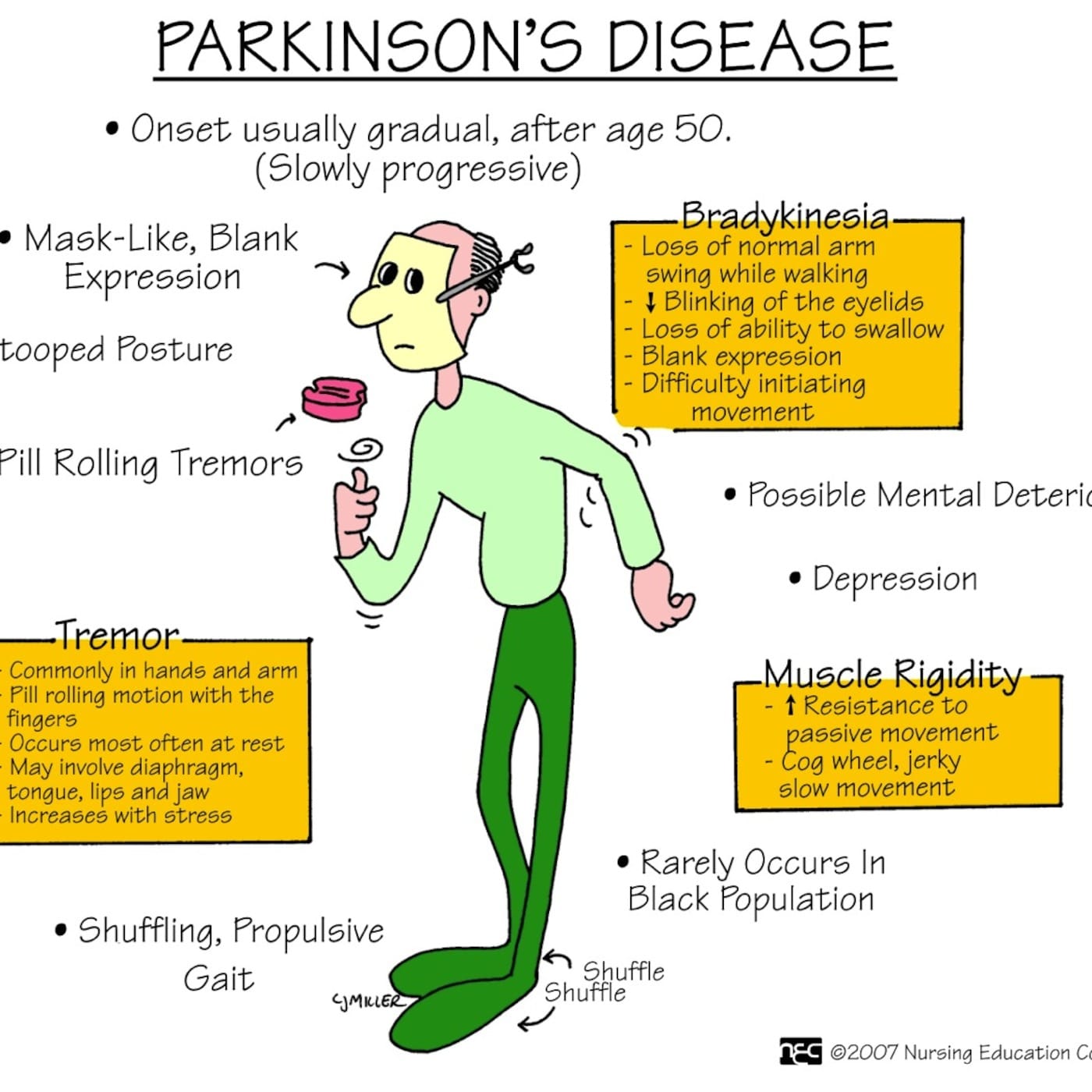
Symptoms Of Parkinsons Disease
Some symptoms of Parkinsons affect a persons ability to move. These symptoms are often called motor symptoms, and they include:
- Stiffness of muscles
- Tremor of an arm or leg while at rest
- Unstable posture
Other symptoms of Parkinsons dont affect a persons movement. These nonmotor symptoms may include:
- Digestive problems, such as constipation
- Cognitive changes, such as loss of attention, difficulty solving problems, memory loss, and trouble with language
Parkinsons symptoms may take several years to appear. A majority of people with Parkinsons live for many years with the condition.
Also Check: Motor Symptoms Of Parkinson’s Disease
Parkinson’s Disease And Movement Disorders Center
Our center provides compassionate and timely treatment to patients with movement disorders, such as dystonia, ataxia, essential tremor and similar conditions. But our mission goes beyond patient care excellence. By offering educational events and support groups, we empower patients and caregivers to become better partners in their health.
Environmental Factors And Exposures
Exposure to pesticides and a history of head injury have each been linked with PD, but the risks are modest. Never drinking caffeinated beverages is also associated with small increases in risk of developing PD.
Low concentrations of urate in the blood is associated with an increased risk of PD.
Drug-induced parkinsonism
Different medical drugs have been implicated in cases of parkinsonism. Drug-induced parkinsonism is normally reversible by stopping the offending agent. Drugs include:
Also Check: Best Parkinson’s Doctors In Usa
Motor Circuit In Parkinson Disease
The basal ganglia motor circuit modulates the cortical output necessary for normal movement .
Signals from the cerebral cortex are processed through the basal ganglia-thalamocortical motor circuit and return to the same area via a feedback pathway. Output from the motor circuit is directed through the internal segment of the globus pallidus and the substantia nigra pars reticulata . This inhibitory output is directed to the thalamocortical pathway and suppresses movement.
Two pathways exist within the basal ganglia circuit, the direct and indirect pathways, as follows:
-
In the direct pathway, outflow from the striatum directly inhibits the GPi and SNr striatal neurons containing D1 receptors constitute the direct pathway and project to the GPi/SNr
-
The indirect pathway contains inhibitory connections between the striatum and the external segment of the globus pallidus and between the GPe and the subthalamic nucleus striatal neurons with D2 receptors are part of the indirect pathway and project to the GPe
The STN exerts an excitatory influence on the GPi and SNr. The GPi/SNr sends inhibitory output to the ventral lateral nucleus of the thalamus. Dopamine is released from nigrostriatal neurons to activate the direct pathway and inhibit the indirect pathway. In Parkinson disease, decreased striatal dopamine causes increased inhibitory output from the GPi/SNr via both the direct and indirect pathways .
Pet Imaging Of Neuroinflammation In Parkinsonian Disorders
Microglia are the primary macrophages involved in the innate immune response of the central nervous system. It is suggested that microglia-mediated inflammatory processes can aggravate injury, leading to events that may result in neurodegeneration . A widely used PET ligand for imaging neuroinflammation has been 11C-PK11195, which binds to the 18 kDa translocator protein , located on the outer mitochondrial membrane in microglia. Upregulation of TSPO is suggestive of microglial activation in the central nervous system. However, there are several limitations of 11C-PK11195 , which has prompted the development of improved second-generation radiotracers, including 11C-PBR28 and 18F-FEPPA .
RBD is a significant risk factor for the development of -synucleinopathies . In polysomnography-confirmed cases with idiopathic RBD, elevated 11C-PK11195 binding was reported in the occipital lobe , as well as in the left SN, although no significant differences in 11C-PK11195 binding were noted in the putamen or caudate . Longitudinal studies are needed to identify biomarkers for those likely to convert earlier vs. later into an overt symptomatic synucleinopathy when presenting with RBD.
Summary of neuroimaging findings in -synucleinopathies and tauopathies are presented .
Table 5. Summary of neuroimaging findings in tauopathies.
Read Also: Best Place To Live With Parkinson’s Disease
How Is Parkinsonism Treated
The treatments for parkinsonism depend on the condition itself and what caused it. Most forms of parkinsonism are treatable, and some can stop entirely .
Some examples of treatable conditions include:
In general, your healthcare provider is the best person to provide more information about whether or not your condition is treatable or curable. That’s because so many different conditions fall under parkinsonism, many of which are very different from person to person. Your provider can tell you more about if your condition is treatable and what your treatment options are with your specific case and circumstances.
Recognizing Other Causes Of Parkinsonism
Although the symptoms and signs of Parkinsons disease are fairly specific, a significant fraction of patients with parkinsonism do not have PD.
In an epidemiologic study of patients with parkinsonism, Schrag et al found that
- 6% had atypical but non-specific features
- 2.5 % had progressive supranuclear palsy
- 2% had dementia with parkinsonism
- 1.7 % had multiple system atrophy
Identifyingpatients withatypical parkinsonism is important sincethese patients
- respond less reliably to dopaminergic agents,
- do not respond favorably to surgical treatments of PD, and
- develop additional clinical problems.
Atypical parkinsonism should be considered particularly
- in patients with poor dopamine responsiveness
- early loss of balance
Medication-induced Parkinsonism
Although tremor and postural instability may be less prominent, this condition may be indistinguishable from PD. Medications frequently associated with the development of parkinsonism include:
The parkinsonism usually resolves after some months after discontinuing the offending medication.
Progressive Supranuclear Palsy
Characteristic of PSP is the early onset of
- eye movement problems
There is no specific treatment for PSP. Dopaminergic treatment should be tried but often offers little benefit. Supportive measures such as speech therapy, physical therapy and antidepressants may help.
Corticobasal Degeneration
Dont Miss: Is Massage Good For Parkinsons
Also Check: Can You Drive A Car With Parkinson’s Disease
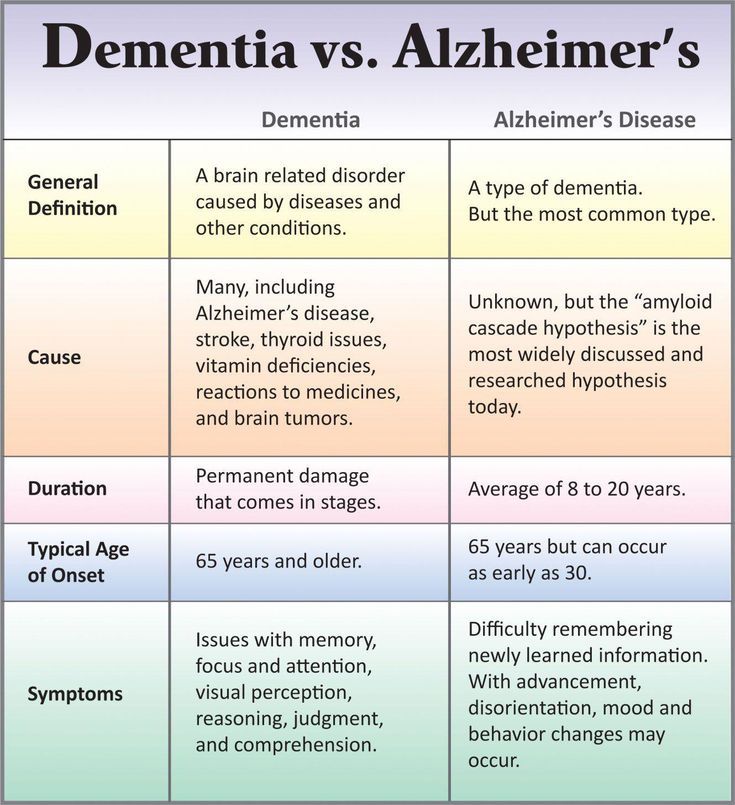
Whats The Difference Between Lewy Body Dementia Parkinsons Disease And Alzheimers Disease
Lewy body dementia is an umbrella term for two related clinical diagnoses: dementia with Lewy bodies and Parkinsons disease dementia. These disorders share the same underlying changes in the brain and very similar symptoms, but the symptoms appear in a different order depending on where the Lewy bodies first form.
Dementia with Lewy bodies is a type of dementia that causes problems with memory and thinking abilities that are severe enough to interfere with everyday activities. It specifically affects a persons ability to plan and solve problems, called executive function, and their ability to understand visual information. Dementia always appears first in DLB. The motor symptoms of Parkinsons such as tremor, slowness, stiffness and walking/balance/gait problems usually become more evident as the disease progresses. Visual hallucinations, REM sleep behavior disorder, fluctuating levels of alertness and attention, mood changes and autonomic dysfunction are also characteristic of DLB.
Finally, Alzheimers is characterized by different abnormal clumps called amyloid plaques, and jumbled fiber bundles called tau tangles. These microscopic structural changes in the brain were discovered by Dr. Alois Alzheimer in 1906. These plaques and tangles, together with loss of connections between nerve cells, contribute to loss of coherence and memory, as well as a progressive impairment in conducting normal activities of daily living.
Other Types Of Parkinsonism
Like Parkinsons, MSA can cause stiffness and slowness of movement in the early stages. However, people with MSA can also develop symptoms that are unusual in early Parkinsons, such as unsteadiness, falls, bladder problems and dizziness.
PSP affects eye movement, balance, mobility, speech and swallowing. Its sometimes called Steele-Richardson-Olszewski syndrome.
Normal pressure hydrocephalus mainly affects the lower half of the body. The common symptoms are walking difficulties, urinary incontinence and memory problems. Removing some cerebrospinal fluid through a needle in the lower back can help with these symptoms in the short term. If there is improvement after this procedure, an operation to divert the spinal fluid permanently can help in the long term.
While these are not parkinsonian disorders, you may be diagnosed with one of these conditions if tremor is your only symptom.
There are several other, much rarer, possible causes of parkinsonism. These include rare conditions like Wilsons disease, an inherited disorder where theres too much copper in your bodys skin and muscles.
Read Also: Is Memory Loss A Symptom Of Parkinson’s
Whats The Difference Between Corticobasal Degeneration And Parkinsons
The main difference between CBD and Parkinsons is that it usually starts on one side with the gradual loss of use of one hand or leg , and there may be little flicks of involuntary muscle jerks. Walking and balance difficulties usually occur later in CBD than in Parkinsons. Also, in CBD, a person may have trouble with purposeful movements, such as buttoning a shirt or cutting food.
For more information on corticobasal degeneration, read this information page.
Echogenicity In Substantia Nigra
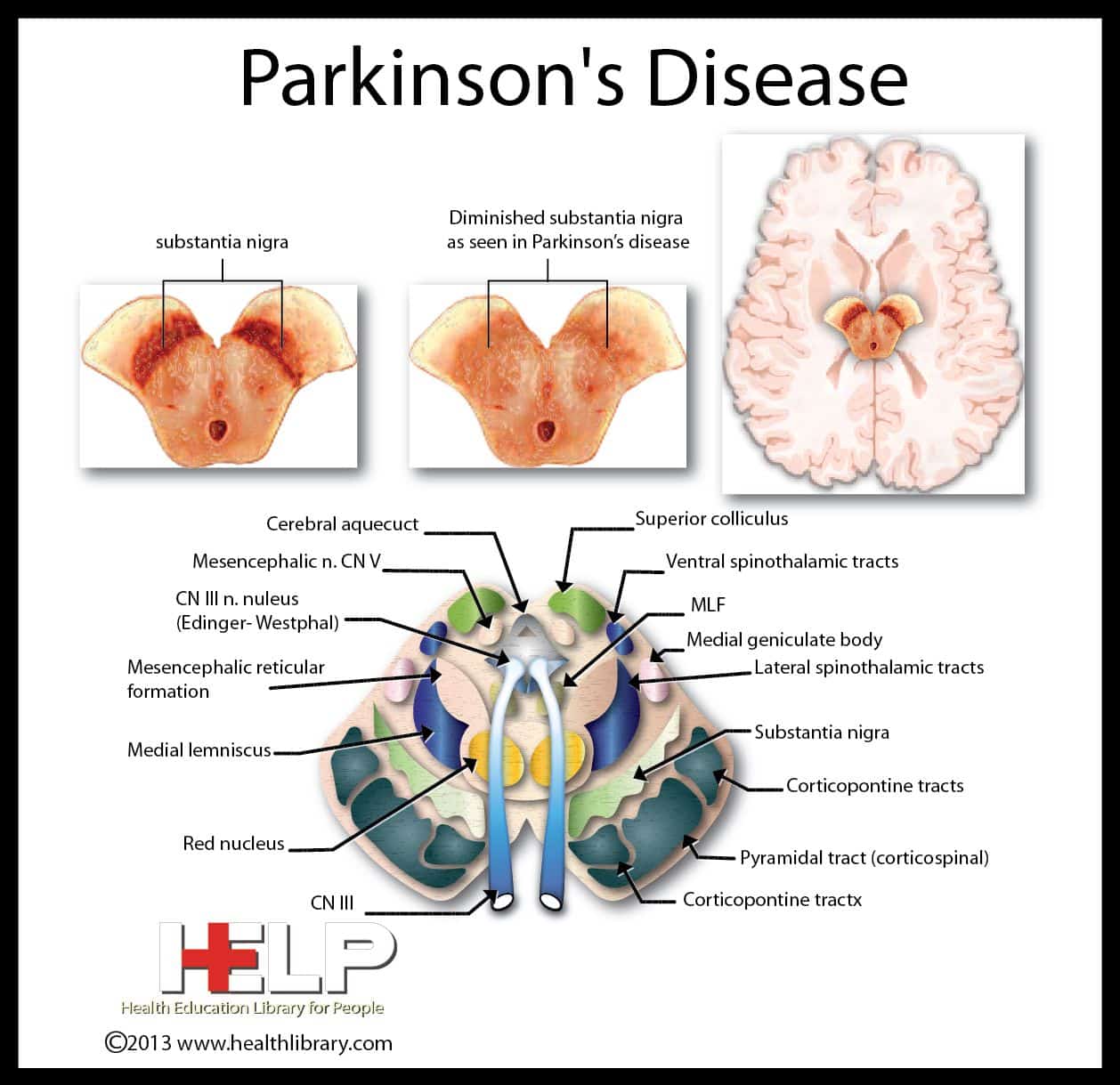
In PD, increased echogenicity of the SN is commonly observed, which can be visualized at the mesencephalic plane as an enlarged, lighter region within the darker mesencephalon . Similar to idiopathic PD, increased SN echogenicity is seen in PD patients carrying LRRK2 and GBA mutations . Although, the precise etiology of SN hyperechogenicity is under research, it is likely due to the known nigral pathology and associated accumulation of free iron within the SN.
Figure 7. Transcranial sonographic image outlining the butterfly-shaped midbrain at the mesencephalic plane. In , enlarged area of echogenicity at the anatomical site of substantia nigra is depicted, as may be seen in Parkinson’s disease patients. In addition, interrupted echogenic line of the raphe can be observed . In , normal midbrain echogenicity is shown. The aqueduct is indicated by an asterisk. Figure adapted from Richter et al. , under the Creative Commons Attribution License .
It is also important to note that ~10% of healthy controls, as well as ~16% of patients with essential tremor may show elevated echogenicity in the SN , thus limiting the utility of this echofeature as a standalone biomarker of PD. For example, in a 3 year longitudinal study, baseline SN hyperechogenicity was evident not only in PD, but also in patients with essential tremor, who subsequently developed parkinsonian symptoms during the follow-up period .
You May Like: Is Parkinson’s More Common In Males Or Females