How Is Parkinsons Disease Treated
There is no cure for Parkinsons disease. However, medications and other treatments can help relieve some of your symptoms. Exercise can help your Parkinsons symptoms significantly. In addition, physical therapy, occupational therapy and speech-language therapy can help with walking and balance problems, eating and swallowing challenges and speech problems. Surgery is an option for some patients.
Treatment Of Late Stage Complications Of Parkinsons Disease
Postural hypotension
Levodopa and dopamine agonists worsen postural hypotension and it may be necessary to lower the dose of levodopa or withdraw the agonist. Treatment is difficult, but patients should be advised to sleep with the head of the bed raised by one or two bricks and to add salt to their diet. Fludrocortisone can then be added at a dose of 0.1 mg in the morning, increasing if necessary up to 0.5 mg in the morning. If these measures are ineffective, the alpha agonist midodrine 10-20 mg four hourly can be useful but it is experimental and only available via the Special Access Scheme. Patients treated for postural hypotension need to have electrolytes, renal function and supine blood pressures closely monitored.
Parkinsonian psychosis, depression and dementia
Psychotic symptoms such as visual hallucinations and persecutory delusions occur most commonly in the setting of dementia, which may be mild and therefore easily missed. Most drugs for Parkinsons disease make these symptoms worse. Depression is also common and requires treatment in its own right.
Levodopa: The Most Effective Drug For Treating Parkinsons
Levodopa, also known as L-DOPA, has long been, and continues to be, the most effective drug in treating Parkinsons disease symptoms. Most people with Parkinsons disease will take this drug at some point. There are side effects that can occur with Levodopa including nausea, fatigue and orthostatic hypotension. Often these side effects can be successfully treated so that Levodopa can be tolerated better. In addition, as the disease progresses and the brain has less ability to produce and process dopamine, dyskinesias, or involuntary movements can develop from Levodopa.
You May Like: Does Nick Nolte Have Parkinson’s Disease
How Anticholinergics Are Used
These medications are older and are not used very often for Parkinsons today. Sometimes they are prescribed for reducing tremor and muscle stiffness. They can be used on their own, especially in the early stages of your Parkinsons when symptoms are mild, before levodopa is prescribed.
Anticholinergics can also be used with levodopa or a glutamate antagonist. They are taken as tablets or as a liquid.
Treatments And Outcomes Of Dip
DIP is generally treated by cessation of the offending drugs. Patients who cannot stop taking antipsychotic drugs because of their psychiatric diseases, such as those with schizophrenia or major depressive disorders, may be switched to atypical antipsychotics that have a lower risk of EPS. People who are prescribed dopamine antagonists due to simple GI disturbance, headache, dizziness, or insomnia should stop taking the offending drugs as soon as possible. Anticholinergics including trihexyphenidyl, benztropine, amantadine, and levodopa have been empirically tested for their ability to relieve symptoms of DIP, but this has produced no clear evidence of their effects in DIP patients.,,,,
Dont Miss: What Classes Of Drugs Are Used To Treat Parkinsons Disease
You May Like: Can Parkinson’s Psychosis Be Reversed
Dopamine Agonist Withdrawal Syndrome
If you suddenly stop taking dopamine agonists, this can lead to dopamine agonist withdrawal syndrome, which can cause symptoms such as depression, anxiety or pain.
Any withdrawal from Parkinsons drugs needs to be done in a tapered way, under the supervision of a health professional.
Speak to your specialist for advice.
You May Like: How To Support Someone With Parkinsons Disease
Types Of Dopamine Agonist Drugs
Below are the types of dopamine agonist drugs. The generic names are written in bold and the brand names are written underneath in bullet points.
Pramipexole
- Apo-go pre-filled pen for Intermittent injection
- Dacepton cartridge for Intermittent injection
- Apo-go pre-filled syringe for infusion
- Dacepton Vial
Recommended Reading: How Do You Spell Parkinson’s
What Future Medications May Be Available For Parkinsons
There are numerous studies investigating new treatments for Parkinsons disease.
There has been new information about the role of autoimmunity and T-cells in the development of Parkinsons disease, possibly opening the door to a role for biologics.
Stem cells are also being investigated as a treatment option for Parkinsons disease.
Recommended Reading: Can Essential Tremor Become Parkinsons
Mechanism Of Action Of Available Drugs
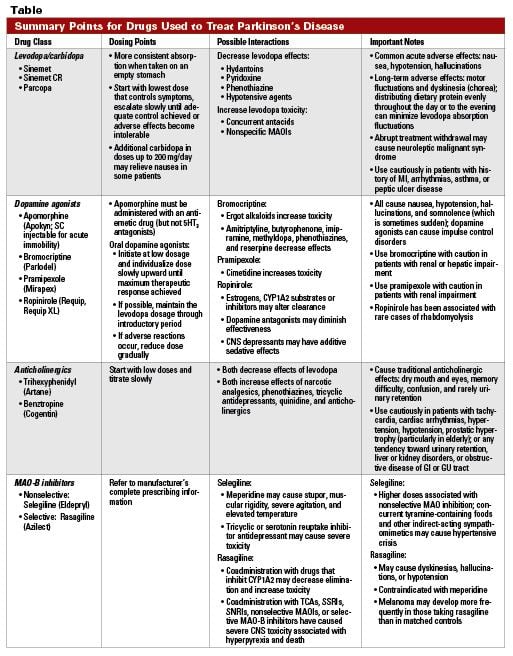
The major classes of drugs currently available for the treatment of idiopathic Parkinson’s disease are shown in Table 1. Many aim to increase dopamine in the brain, by increasing its production or altering its metabolism .
|
Table 1 |
Drugs with alter metabolism in boxed red italics
Levodopa
Levodopa is absorbed from the small intestine and transported into the brain where it is converted to dopamine. Levodopa has a short plasma half-life of about one hour. Early in Parkinson’s disease, levodopa has a long duration of action which is independent of plasma concentration, but as the disease progresses, the duration of the effect reduces. The short-duration effect is strongly linked to plasma concentration and lasts, at most, hours.
Slow-release preparations are gradually absorbed, resulting in more sustained plasma concentrations. They have reduced bioavailability higher doses are required to match the benefit of an equivalent strength of a standard preparation. Rapid release preparations are taken in liquid form to enhance passage through the stomach and absorption from the small intestine.
Dopamine agonists
Apomorphine is a potent emetic so patients must be pre-treated with domperidone 20 mg three times daily orally for at least 48 hours before the first injection. Domperidone should be continued for at least a few weeks once regular intermittent treatment has commenced. The dose can then be tapered slowly as tolerance to the emetic effects of apomorphine usually develops.
You May Like: Stage 1 Parkinson’s Treatment
Medication Tips For Treating Parkinsons Disease
Your doctor will determine the best combination of Parkinsons disease medications for you, as well as how and when to take them. There are also some general guidelines to consider:
- Keep a Parkinsons disease medication list and note down how and when you should take each drug. This can be helpful if memory problems crop up and someone else has to administer medications for you.
- Always take your medications as your doctor prescribes. Write it down or bring a family member to your appointment if you think youll forget.
- Store your medications in a dry, safe place, unless your doctor advises you to keep them in the fridge.
- Throw away expired medications.
- Remember to order your prescriptions in advance.
- Always take extra medication with you when you travel.
- Dont change your dose or stop taking your medication unless your doctor tells you to.
- Take your medication at the same time every day. Keep them in a pill case and set an alarm to remind yourself to take them, especially if you live alone.
- Physical exercise can help the body absorb medication, so try to move as much as possible.
If you have any questions about this Parkinsons disease medication list, consult your doctor. He or she will be able to answer your questions and advise you on how and when to take your medication. You should also seek medical advice if youre struggling with the side-effects of a particular drug or you want to try something different.
See Also:
Treatment Of Neurobehavioral Features
Treatment of cognitive deficits associated with PD is as challenging as the treatment of Alzheimers disease and other dementias. While the general assumption has been that cognitive deficits are a feature of late-stage PD, clinically inapparent cognitive changes on neuropsychiatric testing may be found . With the introduction of cholinesterase inhibitors such as donepezil , rivastigmine , and galantamine and the NDMA antagonist memantine , it is possible that cognition, orientation and language function will improve, and that such improvement will lead to a meaningful improvement in function. Both donepezil and rivastigmine improve cognition to the same effect, but donepezil is better tolerated . The largest and best-designed study of rivastigmine in dementia associated with PD involved 541 patients enrolled in a 24-week randomized, multicenter, double-blind clinical trial . The patients had a relatively mild dementia , with onset of dementia about 2 years after onset of PD symptoms. The mean ADAS-cog score, the primary efficacy variable, improved by 2.1 points in the rivastigmine group, compared to 0.7 in the placebo group , and the MMSE improved by 0.8 in the rivastigmine group and worsened by 0.2 in the placebo group . At the end of the study, 55.5% were receiving 9 to 12 mg. The adverse effects that were significantly more frequent in the rivastigmine group were nausea, vomiting, dizziness, and tremor.
Recommended Reading: Parkinsonism Is Characterized By The Loss Of
Recommended Reading: Using Cbd For Parkinson’s Disease
What Should I Know About Storage And Disposal Of This Medication
Keep this medication in the container it came in, tightly closed, and out of reach of children. Store it at room temperature and away from excess heat and moisture .
Store cassettes containing levodopa and carbidopa enteral suspension in the refrigerator in their original carton, protected from light. Do not freeze the suspension.
Unneeded medications should be disposed of in special ways to ensure that pets, children, and other people cannot consume them. However, you should not flush this medication down the toilet. Instead, the best way to dispose of your medication is through a medicine take-back program. Talk to your pharmacist or contact your local garbage/recycling department to learn about take-back programs in your community. See the FDAs Safe Disposal of Medicines website for more information if you do not have access to a take-back program.
It is important to keep all medication out of sight and reach of children as many containers are not child-resistant and young children can open them easily. To protect young children from poisoning, always lock safety caps and immediately place the medication in a safe location â one that is up and away and out of their sight and reach.
You May Like: Is Rigidity A Symptom Of Parkinsons
Side Effects And Problems With Dopamine Agonists
Common side effects of dopamine agonists include:
- Nausea and vomiting
- Hallucinations or delusions and confusion
- Existing dyskinesias becoming more troublesome initially
If you are taking Cabergoline , Pergolide or Bromocriptine your neurologist or GP will have to arrange a chest CT scan or ultrasound of your heart yearly as over time these medications may affect heart or lung tissue.
This precaution does not apply to the other dopamine agonists available in Australia.
Don’t Miss: What Makes Parkinson’s Tremors Worse
Medication Guidelines For Parkinson’s Disease
There is no one best mix of Parkinsonâs medicines. You and your doctor will have to try a few treatment approaches to figure out the best one for you.
But there are some general guidelines for taking your medication. Be sure to ask your doctor or pharmacist for any specific tips for your treatment.
Adjust Your Drug Dose
Side effects like dyskinesia might be due to the amount of levodopa youre taking. Ask your doctor whether you can lower your dose enough to prevent side effects while still managing your Parkinsons symptoms. It might take some trial and error to get the dose just right.
Another option is to switch to an extended-release form of dopamine. Because the drug releases more slowly into your blood, it prevents the dopamine spikes and valleys that can trigger dyskinesia.
You might also need to add more of a drug. For example, adding extra carbidopa to levodopa can cut down on nausea.
Read Also: Symptoms Of Parkinsons In Women
An Approach To The Treatment Of Parkinsons Disease
No treatment can arrest or slow neurodegeneration in Parkinsons disease. The aim is to relieve symptoms and avoid the complications of therapy.
Early Parkinsons disease
Many studies have shown that early treatment with dopamine agonists reduces the incidence of dyskinesia.1Fewer motor fluctuations were shown in some but not all of the studies. We recommend a dopamine agonist as the first treatment in younger patients who have mild disease and no cognitive deficit. It is necessary to add levodopa within 1-5 years in most patients. In more severe disease, treatment begins with levodopa but a dopamine agonist may be added to keep the daily dose of levodopa in the lower range if there is no cognitive deficit. Dopamine agonists are used infrequently and with caution in patients more than 70 years old because of the risk of neuropsychiatric adverse effects and postural hypotension. They are contraindicated in the presence of dementia.
Isolated resting tremor is rarely disabling, but if it interferes with function it can usually be managed with levodopa. When this is ineffective at low to moderate doses, the addition of an anticholinergic can sometimes be useful.
Patients with motor fluctuations
Role of physical therapy and surgery
How Is Parkinsons Treated In The Early Stages
Three main groups of medication are used to treat Parkinsons in the early stages:
- Levodopa : is converted into dopamine in the brain.
- Dopamine agonists: stimulate the nerve receptors responsible for the uptake of dopamine.
- MAO-B inhibitors : block the breakdown of dopamine in the brain.
The medications are usually taken in tablet form. Some dopamine agonists are also available as patches.
In the early stages, some people with mild symptoms cope just fine without medication. If at some stage the symptoms become too much of a problem, levodopa and dopamine agonists are the main medication options. They work slightly differently to each other, and some products may cause side effects more often or have worse side effects than others. But both are very effective in the early stages of the illness. That helps many people with Parkinsons to live a fairly symptom-free life for at least a few years.
Also Check: Parkinson’s Freezing Of Gait Treatment
Stay Safe With Your Medicines
Read all labels carefully.
- Tell all your health care providers about all the medicines and supplements you take.
- Know all the medicines and foods youâre allergic to.
- Review any side effects your medicines can cause. Most reactions will happen when you start taking something, but thatâs not always the case. Some reactions may be delayed or may happen when you add a drug to your treatment. Call your doctor right away about anything unusual.
- Use one pharmacy if possible. Try to fill all your prescriptions at the same location, so the pharmacist can watch for drugs that might interact with each other.
- You can use online tools to see if any of your medicines wonât work well together.
You have the right and responsibility to know what medications your doctor prescribes. The more you know about them and how they work, the easier it will be for you to control your symptoms. You and your doctor can work together to create and change a medication plan. Make sure that you understand and share the same treatment goals. Talk about what you should expect from medications so that you can know if your treatment plan is working.
Show Sources
Editorial Sources And Fact
- Parkinsons Disease: Diagnosis & Treatment. Mayo Clinic. December 8, 2020.
- Pringsheim T, Day GS, Smith DB, et al. Dopaminergic Therapy for Motor Symptoms in Early Parkinson Disease Practice Guideline Summary: A Report of the AAN Guideline Subcommittee. Neurology. November 15, 2021.
- Levodopa and Carbidopa. MedlinePlus. June 15, 2018.
Read Also: Does Senator Susan Collins Have Parkinson’s Disease
Delayed Administration And Contraindicated Drugs Place Hospitalized Parkinsons Disease Patients At Risk
Problem: One-third of all patients with Parkinsons disease visit an emergency department or hospital each year, making it a surprisingly common occurrence.1 The disease affects about 1 million people and is currently the fourteenth leading cause of death in the US. Hospitalization can be risky for patients with Parkinsons disease when viewed from the perspective of pharmacological management.
Patients with Parkinsons disease require strict adherence to an individualized, timed medication regimen of antiparkinsonian agents. Dosing intervals are specific to each individual patient because of the complexity of the disease. It is not unusual for patients being treated with carbidopa/levodopa to require a dose every 1 to 2 hours. When medications are not administered on time, according to the patients unique schedule, patients may experience an immediate increase in symptoms.2,3 Delaying medications by more than 1 hour, for example, can cause patients with Parkinsons disease to experience worsening tremors, increased rigidity, loss of balance, confusion, agitation, and difficulty communicating.2 Studies show that three out of four hospitalized patients with Parkinsons disease do not receive their medications on time, or have had doses entirely omitted.4 According to the National Parkinson Foundation, 70% of neurologists report that their patients do not get the medications they need when hospitalized.2
Two case examples
References
Side Effects And Problems Of Anticholinergics
Another reason these drugs are not a first choice for treating Parkinsons are their side effects. Some people may experience confusion, a dry mouth, constipation and blurred vision when taking anticholinergics.
Anticholinergics may interfere with levodopa absorption in the small bowel, which reduces the effectiveness of Madopar or Sinemet, forms of the drug levodopa.
Anticholinergics are not usually prescribed to older people with Parkinsons because there is an increased risk of memory loss and, in men, problems urinating.
Read Also: Is Zinc Good For Parkinson’s
Medications To Avoid Or Use With Caution
Sign up for our email list and receive our publication on medications with potential complications you should be aware of.
Before making any decisions about treatment of Parkinsons disease, you will want to learn about the different types of medications available for Parkinsons disease and discuss the pros and cons of each with your physician. It may help to know that there is no right answer, and if you try something that doesnt work for you, you can always adjust your plan.
To learn more about adjusting medication plans, view our webinar on What to Do When Your Medications Stop Working.