Primary Motor Symptoms Of Parkinsons Include:
- Tremor: a rhythmic shaking in your arms, legs or chin. Most people with Parkinsons who experience tremor that is worse when relaxing and resting have rest tremor. Others experience active tremor, which means their shaking worsens when trying to do something, like drinking out of a cup of coffee or eating with a spoon.
- Rigidity: painful stiffness, often in the arms, legs, neck or back muscles.
- Akinesia, Bradykinesia, Hypokinesia:Akinesia and bradykinesia refer to the reduction of movement, slowness of movement, and sometimes even complete lack of movement that can be caused by Parkinsons. Hypokinesia refers to a loss of momentum or force in movement that can come with Parkinsons, usually in connection with akinesia, bradykinesia, or both. The small, cramped handwriting that some people with Parkinsons experience is thought to be some combination of akinesia and hypokinesia.
- Postural Instability: balance problems caused by a loss of reflexes that help you stay upright. This can cause challenges with general balance as well as walking . Sometimes postural instability brings the tendency to fall backward, called retropulsion.
Early motor symptoms can also include a mask-like face or loss of facial expression, small, cramped handwriting , and .
People often complain of a heaviness feeling, dragging of one side, or cramping in certain muscles. Speech can become softer and more difficult as Parkinsons progresses and swallowing can also be affected.
Support For People Living With Parkinsons Disease
While the progression of Parkinsons is usually slow, eventually a persons daily routines may be affected. Activities such as working, taking care of a home, and participating in social activities with friends may become challenging. Experiencing these changes can be difficult, but support groups can help people cope. These groups can provide information, advice, and connections to resources for those living with Parkinsons disease, their families, and caregivers. The organizations listed below can help people find local support groups and other resources in their communities.
If You Develop A Tremor
Urgent medical care isn’t needed if you’ve had a tremorshaking or tremblingfor some time. But you should discuss the tremor at your next doctor’s appointment.
If a tremor is affecting your daily activities or if it’s a new symptom, see your doctor sooner.
A written description will help your doctor make a correct diagnosis. In writing your description, consider the following questions:
- Did the tremor start suddenly or gradually?
- What makes it worse or better?
- What parts of your body are affected?
- Have there been any recent changes in the medicines you take or how much you take?
Recommended Reading: Signs Of Parkinson’s In Young Adults
Cold Weather And Parkinsons Symptoms
If you find your Parkinsons disease symptoms are worse in cold weather, youre not alone. Many members on MyParkinsonsTeam note greater stiffness, pain, and other symptoms during the winter months. Parkinsons disease impacts a persons ability to regulate body temperature, which makes some people with PD more sensitive to hot or cold temperatures.
Winter weather is extremely unpleasant for some members on MyParkinsonsTeam. This winter when the temperature dropped to , I experienced greater pain, stiffness, freezing, and slowness, one member posted. It was so overwhelming I could not find any remedies except five blankets. The pain was surprising.
Several other members mentioned that cold temperatures can cause or worsen pain related to Parkinsons disease. I get cold very easily and I shiver, a member wrote. Because I am stiff it actually hurts to be cold. Others agreed, My back and neck are excruciatingly painful, more so than usual.
Cold weather can also exacerbate Parkinsons tremors. One member commented, I have found that my shivering to stay warm makes my tremors worse. Another MyParkinsonsTeam member added, I also struggle with the cold now. It brings on my tremor, so I always have to stay warm.
Some MyParkinsonsTeam members didnt know about the impact of cold on PD until other members raised the issue. I thought I was alone with my symptoms, a member wrote in response to a question about cold weather.
Read Also: Asbestos And Parkinsons Disease
What Is A Parkinsons Tremor
Other health issues can also cause tremors, like multiple sclerosis or essential tremor. But Parkinsonâs tremors are different because theyâre usually:
- Resting. Parkinsonâs tremors happen when your muscles are still. They go away when you move. They also lessen while you sleep. For example, if youâre sitting in a chair with your arm relaxed, you may notice that your fingers twitch. But if youâre using your hand, like when you shake someone elseâs hand, the tremor eases or stops.
- Rhythmic. Parkinsonâs tremors are slow and continuous. They arenât random tics, jerks, or spasms.
- Asymmetric. They tend to start on one side of your body. But they can spread to both sides of the body.
You May Like: Living Alone With Parkinson’s
If You Have Parkinson’s Disease
If you have been diagnosed with Parkinson’s, call your doctor if:
- You notice any significant change in your symptoms, such as severe episodes of freezinga sudden loss of mobilitywhich may affect walking.
- Your response to your medicine changes.
- Any other symptoms occur, such as constipation, sexual problems, or incontinence.
- You have symptoms of depression, such as feeling sad or losing interest in daily activities.
- You or your family notice that you have problems with memory and thinking ability.
Living With Parkinson Disease
These measures can help you live well with Parkinson disease:
- An exercise routine can help keep muscles flexible and mobile. Exercise also releases natural brain chemicals that can improve emotional well-being.
- High protein meals can benefit your brain chemistry
- Physical, occupational, and speech therapy can help your ability to care for yourself and communicate with others
- If you or your family has questions about Parkinson disease, want information about treatment, or need to find support, you can contact the American Parkinson Disease Association.
Dont Miss: Dealing With Parkinsons Dementia
Read Also: Strange Behavior With Parkinson’s
What Can My Doctor Do To Treat Parkinson’s Disease
There is no cure for Parkinson’s, but your doctor can prescribe drugs to drastically reduce your symptoms. In the earliest stages of the disease, you may not need medications at all. As symptoms get a bit worse, your doctor may suggest selegiline, a drug that protects brain cells from damage. If used in the early stages of the disease, selegiline can delay the need for levodopa. And when prescribed in combination with levodopa, selegiline may slow the onset of disability. But eventually, all patients will need more serious medication to help them carry on their lives.
At some point, almost everyone with Parkinson’s will take levodopa — a drug seemingly capable of miracles. The brain converts levodopa into dopamine, thus replenishing the supply of this crucial compound as well as restoring, at least temporarily, long-lost physical abilities. You may remember levodopa from the movie “Awakenings,” which was based on a true story. With one shot of the drug, the character played by Robert DeNiro awoke from a long coma brought on by a Parkinson’s-like disease.
For Parkinson’s patients, the response to levodopa can be almost as dramatic. In some cases, the disease seems to disappear, at least temporarily. The drug can give a patient years of normal, productive living when they would have otherwise been disabled. Levodopa is especially useful for relieving slowness and stiffness, but it has a limited effect on tremors.
What Causes Parkinson’s Disease
There’s no doubt that damaged or dying nerve cells in a part of the brain known as the substantia nigra cause Parkinson’s disease, but nobody knows why this occurs. Certain genes seem to make these cells easier to harm, but what actually pulls the trigger? Some experts blame pesticides and other poisons, some point to viruses or oxidation damage in the brain, and some speculate that in some people the brain simply ages faster than usual. Many researchers believe that it takes a combination of these factors — plus genetics — to actually cause the disease, according to the National Institutes of Health.
Also Check: Wheelchair For Parkinson’s Patients
Reasons Your Parkinsons Symptoms May Be Worse After Exercise
Youve heard all the hype. Every Parkinsons healthcare professional, researcher and advocate is shouting from the rooftops how wonderful exercise is supposed to be to help you improve your symptoms and slow the progression of the disease.
But youve had a different experience.
When you exercise, you feel like your symptoms get worse instead of better.
Youre afraid youre the only one.
Youre worried that youre the outlier who cant reap the benefits of exercise.
Rest assured, its not just you.
As a Parkinsons physical therapist, I regularly talk to people who struggle to get on board with a regular exercise program because the side effects after the fact are frustrating and disruptive.
In this article, I want to walk you through four reasons why your Parkinsons symptoms may be getting worse after exercise, and how you can adapt your Parkinsons exercise program to minimize the side effects so you can reap the benefits.
Why Parkinsonian Symptoms Can Worsen During The Day
Parkinsonian symptoms can get worse at certain times, and many people have good days and bad days with Parkinson’s disease. While symptoms can fluctuate naturally, patients can also experience periods where their medication doesn’t work as effectively as usual, typically when they’ve been taking it for a long time. Some people with Parkinson’s disease find that their symptoms are worse due to the decreased effects of levodopa medication that occur over time. Lets look at why this happens and explore ways to treat daytime Parkinsonian symptoms.
You May Like: Cold Hands Parkinson’s Disease
What Are The Symptoms Of Parkinson’s
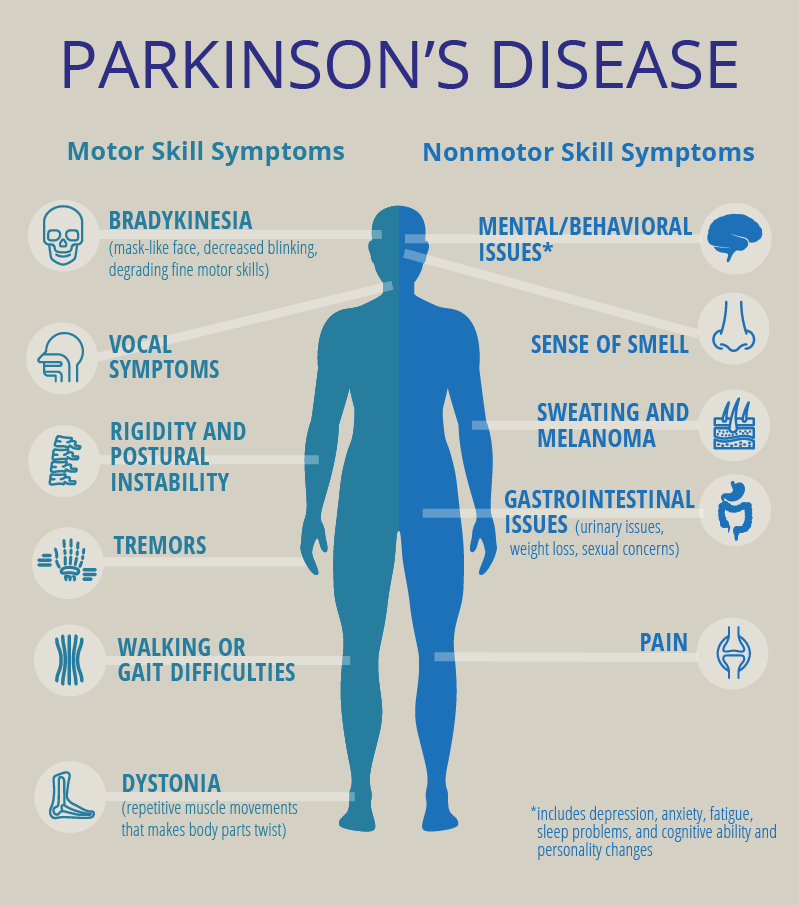
The main motor symptoms of Parkinsons are:
- slowness of movement
- problems with balance.
However, the condition does not only affect movement. People living with the condition can experience a range of non-motor symptoms that can often have a greater impact on their lives than movement difficulties.
Non-motor symptoms include:
- urinary urgency, frequency
These non-motor symptoms are present at all stages of the condition but they can become more severe in the later stages of Parkinsons and have a major impact on quality of life.
Parkinsons gets worse over time and it can be difficult to predict how quickly the condition will progress. For most people, it can take years for the condition to progress to a point where it can cause major problems. For others, Parkinsons may progress more quickly.
What Are The Symptoms Of Parkinson’s Towards The End Of Life

Parkinsons progresses in stages: diagnosis, maintenance, advanced and palliative. Professionals should have talk to people with Parkinsons about advance care planning in the earlier stages of the disease. This can allow them to express their wishes and preferences for their care in the later stages of the disease and make plans for the future.
Although the condition progresses differently and at a different speed for each person, the advanced stage can potentially cover a long period of time.
Problems that affect someone with advanced Parkinsons may include:
- medicines being less effective at managing symptoms than before
- having to take lots of medicines to manage symptoms and side effects
- more off periods when the effects of medication are reduced, and people experience movement fluctuations and involuntary movements
- increased mobility problems and falls
- swallowing difficulties
- less control of their Parkinsons symptoms, which become less predictable
Some of the more advanced symptoms can lead to increased disability and poor health, which can make someone more vulnerable to infection, such as pneumonia. People with Parkinsons most often die because of an infection or another condition, usually caused by Parkinsons.
You May Like: Is There A Medical Test For Parkinson’s Disease
Mayo Clinic Q And A: Rate Of Progression Of Parkinsons Disease Hard To Predict
DEAR MAYO CLINIC: My father is 64 and was diagnosed with Parkinsons last year. So far his symptoms are very mild, but Im wondering what the typical progression of the disease is like. I have read that deep brain stimulation is sometimes recommended. When is this type of treatment usually considered? Is it safe?
ANSWER: The symptoms of Parkinsons disease, or PD, tend to begin very gradually and then become progressively more severe. The rate of progression is hard to predict and is different from one person to another. Treatment for PD includes a variety of options, such as exercise, medication and surgery. Deep brain stimulation is one surgical possibility for treating PD, but its usually only considered in advanced cases when other treatments dont effectively control symptoms.
Parkinsons disease is a syndrome which typically has no known cause. The diagnosis is based on symptoms. Neurologists who specialize in movement disorders typically have the most experience with PD diagnosis and treatment. There are many symptoms of parkinsonism. The most common include excessive slowness and lack of movement, as well as shaking or tremor.
As in your fathers situation, symptoms are often mild at the outset. How quickly they get worse varies substantially, perhaps because there may be multiple underlying causes of the disease. In most cases, symptoms change slowly, with substantive progression taking place over the space of many months or years.
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinsons disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Recommended Reading: Parkinson’s And Seborrheic Dermatitis
Sidebar: Morris K Udall Centers Of Excellence For Parkinson’s Disease Research
The Morris K. Udall Parkinsons Disease Research Act of 1997 authorized the NIH to greatly accelerate and expand PD research efforts by launching the NINDS Udall Centers of Excellence, a network of research centers that provide a collaborative, interdisciplinary framework for PD research. Udall Center investigators, along with many other researchers funded by the NIH, have made substantial progress in understanding PD, including identifying disease-associated genes investigating the neurobiological mechanisms that contribute to PD, developing and improving PD research models, and discovering and testing potential therapeutic targets for developing novel treatment strategies.
The Udall Centers continue to conduct critical basic, translational, and clinical research on PD including: 1) identifying and characterizing candidate and disease-associated genes, 2) examining neurobiological mechanisms underlying the disease, and 3) developing and testing potential therapies. As part of the program, Udall Center investigators work with local communities of patients and caregivers to identify the challenges of living with PD and to translate scientific discoveries into patient care. The Centers also train the next generation of physicians and scientists who will advance our knowledge of and treatments for PD. See the full list of Udall Centers.
Treating The Symptoms Of Parkinsons Diseasehow Palliative Care Can Help
While there is no cure for Parkinsons disease, there are a growing number of treatments that can provide you with relief from its symptoms. People with Parkinsons disease are often prescribed a combination of levodopa and carbidopa, which helps replenish the brains shrinking supply of dopamine.
A new therapy uses electrodes surgically implanted inside the brain, and a small electrical device called a pulse generator to provide electrical deep brain stimulation . Parkinsons patients also benefit from the expertise of physical, occupational and speech therapists to help them manage practical issues in their daily lives.
Other symptoms of Parkinsons disease include a variety of motion-related issues, as well as sleep disturbances, fatigue , constipation and other gastrointestinal problems, and low blood pressure.
Another whole area of Parkinsons symptoms is called cognitive decline, whereby ravages of the disease affect thinking and other uses of the brain. These include troubling mood disorders like depression and anxiety, unclear thinking, difficulty concentrating on a task and the potential emergence of dementia.
Some people become more disabled and dependent over time despite the best treatments. They may come to need so much help with the routine tasks of living that they require 24-hour care. This care may be provided at home or in a setting like assisted living, where they get the personal care they need.
Recommended Reading: Magnetic Therapy For Parkinson’s Disease
Which Body Parts Do Parkinsons Tremors Affect
There are five main places youâll have Parkinsonâs tremors:
1. Hands. Parkinsonâs disease tremors often start in the fingers or hands with whatâs called a pill-rolling motion. Imagine holding a pill between your thumb and index finger and rolling it back and forth.
2. Foot. A Parkinsonâs foot tremor is more likely to happen while youâre sitting or lying down with your feet at rest. If the tremor moves into your thigh muscles. It could look like your whole leg is shaking.
Foot tremors disappear when you stand or walk because those are active movements. A foot or leg tremor while youâre standing may be another condition.
3. Jaw. This is common in people with Parkinsonâs. It may look like youâre shivering. It can become bothersome if the tremor makes your teeth chatter. If you wear dentures, it could make them shift or fall out.
Chewing eases the tremor, so gum might help.
4. Tongue. Itâs rare, but a tongue tremor can cause your entire head to shake.
5. Internal. Some people with Parkinsonâs say they can feel a shaking sensation in their chest or abdomen. But canât be seen from the outside.
Managing Anger And Irritability In Parkinsons As A Caregiver
Informal caregivers particularly family members often play a significant role in helping and caring for loved ones with Parkinsons. Research has shown that caregivers are especially affected by caring for someone dealing with cognitive and mental dysfunctions from Parkinsons. These caregivers report higher caregiver burden and lower overall well-being and quality of life than caregivers of people with PD without significant cognitive impairment. Many caretakers of people with Parkinsons experience anxiety and depression.
The stress of caregiving is a common topic of conversation on MyParkinsonsTeam. One member wrote, My wife has Parkinsons. It is hard to deal with all her ups and downs. We are both exhausted.
Another member wrote about her husband with Parkinsons: His dementia is hard. He is emotional at times, angry at times, and is not aware where he is at times. One member said, My husband has Parkinsons, dementia, diabetes, and a bad heart. It is getting more and more difficult to give him his medications, as he gets very angry and does not take them.
Its important to remember that anger and irritability in people with Parkinsons is often a part of the disease. It is not your fault.
Don’t Miss: Possible Causes Of Parkinson’s Disease