If You Notice Oily Skin On Your Scalp You May Want To Get Checked For Parkinson’s
Many people with Parkinson’s experience a surprising symptom with no obvious connection to the condition: having oily skin on their scalp. This occurs thanks to an increase in sebum, an oily substance produced by the body’s sebaceous glands. This can cause the scalp and hair to appear greasy and shiny. “Some people may only have minor issues, while others may have more severe problems that can affect daily life and cause them discomfort or embarrassment,” explains health organization Parkinson’s UK.
This increase in sebum can also cause a distinct smell associated with PD, according to the Michael J. Fox Foundation, and researchers say this symptom may someday prove diagnostically useful. “If we can define what is behind this Parkinson’s scent, perhaps we can develop objective tests to diagnose the disease earlier,” said Perdita Barran, BSc, PhD, a researcher studying sebum characteristics in PD patients. “Measuring Parkinson’s disease with such an easy-to-obtain sample, a swab of skin secretions, would also allow for more widespread screening,” she said.
Identification Of Malassezia Yeasts
Seven lipophylic Malassezia species were identified: M. globosa, M. furfur, M. slooffiae M. sympodialis, M. restricta, M. obtusa and M. japonic based on microscopic characteristics, presence of catalase and the ability of each isolate to utilize different Tweens . The presence of catalase was determined by applying a drop of 10% hydrogen peroxide on a culture smeared on a glass slide. The production of gas bubbles indicated a positive reaction. The ability to utilize different Tween substrate was assessed on the agar plates, by spreading fresh yeast suspension onto plates. Tween 20, 40, 60 and 80 were added in 4 wells in each plate. The plates were incubated at 32°C for one week and the growth of yeast around individual wells contain different Tween was recorded and Malassezia were identified .
Abbreviations: HC, Healthy controls SD, Seborrheic dermatitis SDN, Seborrheic dermatitis in patients without Parkinson disease SDP, Seborrheic dermatitis in patients with Parkinson disease M, Male F, Female *p< 0.05.
When To See A Doctor
It is recommended to visit a doctor if you develop symptoms of eczema or dermatitis, especially if:
- The skin irritation is hampering your daily activities.
- You have constant pain.
- You have symptoms of a skin infection.
- Home remedies and self-care are unable to improve the infection.
- What can I do at home to help improve my condition?
- Am I allergic or sensitive to anything?
- What treatment do I need and how long will it take to work?
- How can I prevent the condition from flaring up?
- When and what symptoms did you first experience?
- Are you on any topical or oral medications?
- Have you identified any triggering factors?
- Does anyone else in your family has/had asthma or allergies?
Dont Miss: Beginning Signs Of Parkinsons
You May Like: Does Sam Waterston Have Parkinsons
Aids And Cd4+ T Cells
AIDS patients are at increased risk of parkinsonism : about 515% are affected . AIDS-induced parkinsonism differs from sporadic PD in several respects: bradykinesia and rigidity are usually symmetrical, postural instability and gait abnormalities occur earlier, and onset can occur at a much younger age .
A small post-mortem study reported a higher fraction of pigmented cells in the pars compacta of the substantia nigra in AIDS patients . It also reported lower neuronal density in AIDS patients, suggesting neuronal loss . Another small post-mortem study reported lower dopamine levels in the caudate nucleus tissue in AIDS patients , which was attributed to the loss of nigrostriatal dopamine neurons.
AIDS-induced parkinsonism usually occurs when CD4+ T cell counts are very low . Interestingly, peripheral blood CD4+ T cell counts in sporadic PD are also depressed , though not as much as in AIDS. This suggests CD4+ T cells are protective in PD, and prevent or slow dopamine neuron loss. Age-related CD4+ T cell immunosenescence could thus partly explain why PD risk increases with age.
Parkinsons Disease And Its Relationship To Sd

The exact mechanism underlying the association of PD and SD is not fully clear. An increasing amount of evidence indicates direct involvement of Malassezia in the pathogenesis of PD . This yeast species is also recognized as a factor in SD development, thereby constituting a common denominator in the pathogenesis of both SD and PD. Other possibilities for the strong association between SD and PD include gene polymorphisms GBA, LRRK2 and PINK1, which both play a role in lipid regulation and have been shown to confer an increased risk for PD development . In particular, LRRK2 promotes formation of large lipid droplets while PINK1 increases their number and size . Additionally, a variant of the SNCA gene, which encodes for -synuclein, is dysregulated in PD and leads to the abnormal coating of lipid droplets, making them more susceptible to lipases . This is of clinical importance as Malassezia is known to secrete lipases and it has been suggested that SNCA variants facilitate easier access to essential nutrients, allowing the fungus to infiltrate host tissue . Further research is needed to elucidate Malassezias potential direct contribution to the pathogenesis of both SD and PD, but it may help explain the increased prevalence of SD among PD patients.
Recommended Reading: Judy Woodruff Parkinson’s
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Garlic Most Common Seborrheic Dermatitis Herbal Treatment
Garlic is also an effective natural treatment for seborrheic dermatitis. Its very effective in killing yeast and can prevent seborrheic dermatitis flare-ups by preventing the excessive production of yeast on your skin. If you want to use garlic for treating your condition, you can combine garlic juice with a cup of water and apply it to the affected area. Leave it for a while, and then rinse it off thoroughly.
You May Like: Parkinson Bicycle Cleveland Clinic
Examining The Association Nature Of Skin Disorders In Parkinson Disease
Although Parkinson disease is often characterized as a motor disorder, the presence of nonmotor symptoms, such as skin disorders, is common and may provide insights into the pathophysiological mechanisms underlying PD.
Although Parkinson disease is often characterized as a motor disorder, the presence of nonmotor symptoms, such as skin disorders, are common and may provide insights into the pathophysiological mechanisms underlying PD, said Nicki Niemann, MD, neurologist at the Muhammad Ali Parkinson Center and an assistant professor of neurology at Barrow Neurological Institute.
Transcript
AJMC®: Hello, I’m Matthew Gavidia. Today on the MJH Life Sciences Medical World News, The American Journal of Managed Care® is pleased to welcome Dr Nicki Niemann, neurologist at the Muhammad Ali Parkinson Center and an assistant professor of neurology at Barrow Neurological Institute. Dr Niemann additionally served as a co-author of a review article titled Parkinson’s Disease and Skin.
Great to have you on, Nicki. Can you just introduce yourself and tell us a little bit about your work?
Dr Niemann: So, I’m a neurologist by training. I did my training at Baylor College of Medicine in Houston, Texas, and then I did my mood disorders fellowship with the same institution under the mentorship of Dr Joseph Jankovic, who’s one of the co-authors on the review article that we’re talking about today.
Scales Formation On Oily Parts Of The Skin
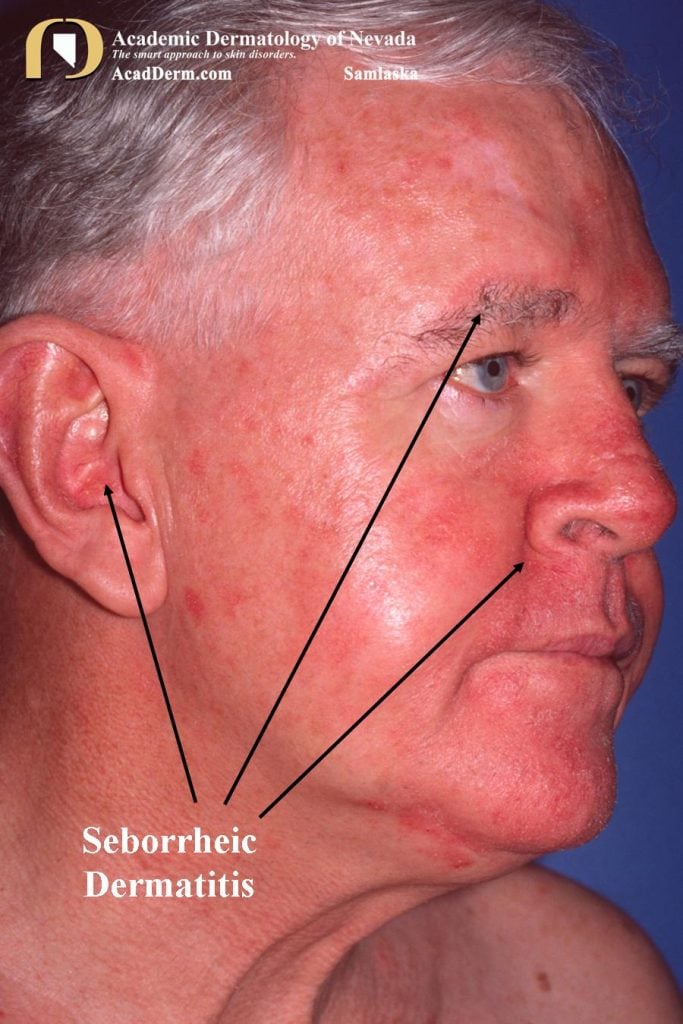
There is formation of white or yellow scales on the oily parts of skin in patients with parkinsons disease. Although seborrheic dermatitis is a common skin issues in general population but is more frequently present in Parkinsons disease patients. There is formation of scaly patches, dandruff, and redness of skin mainly on the oily parts of the face like on the sides of the nose or on the scalp.
You May Like: Prayers For Parkinson’s Disease
Malassezia Are A Necessary Factor In Crohn’s Disease And Spondyloarthritides
Spondyloarthritides are a group chronic immune-mediated diseases mainly driven by alpha beta T cells recognizing intracellular peptides through HLA-B*27 presentation . Affected organs include the spine, joints, skin, eyes, gut, and prostate . Historically, isolated inflammation of the eyes, gut, and skinrespectively acute anterior uveitis, inflammatory bowel disease and psoriasiswere considered separate diseases unrelated to SpA. However, SpA, acute anterior uveitis, inflammatory bowel disease and psoriasis run together in families , and share many polymorphisms in genes controlling T cell activation , strongly suggesting that they are the same immunological pathology . In particular, the fact that HLA-B*27 increases the risk of each disease strongly suggests the same antigens are being targeted . Varied lines of evidence support the presence of an elusive necessary intracellular fungal infection in each affected organ, which is efficiently detected by HLA-B*27 and CARD9 . CARD9 is an essential signaling protein for fungal immunity: homozygous loss-of-function CARD9 mutations cause severe mycoses . CARD9 polymorphisms are associated with inflammatory bowel disease and SpA . Oral antifungal drugs are effective in psoriasis , psoriatic arthritis , and likely in Crohn’s disease as well .
What Do The Ecz
Seborrheic dermatitis isnt contagious and is not an allergy, although some allergies can mimic it, said Dr. Peter Lio, clinical assistant professor of dermatology and pediatrics at Northwestern Universitys Feinberg School of Medicine. A correct diagnosis, he added, requires careful evaluation by a dermatologist.
Seborrheic dermatitis can also overlap with atopic dermatitis, especially in infants. We see this overlap in young adults, as well, usually in those with more severe atopic dermatitis, Lio said. They can develop a condition that some call head and neck dermatitis that seems to be very closely related to seborrheic dermatitis and is treated similarly.
- National Eczema Association | 505 San Marin Drive, #B300 | Novato, CA 94945
- 415-499-3474 or 800-818-7546
Read Also: Voice Amplifiers For Parkinson’s
How To Manage Seborrhoeic Dermatitis
There is no cure for seborrhoeic dermatitis but there are treatments that can control it. Be aware that if you stop the treatments the condition may come back. It can also flare up when you are stressed.
Try to avoid cosmetics that contain alcohol, and soaps and shaving creams that irritate your skin. You should also switch to using non-greasy special moisturising creams and emollient soap substitutes. Some people may find certain foods make the condition worse, so you could try keeping a diary to see if anything in your diet is causing problems.
The following treatments are recommended for the scalp and beard.
- Loosen any crusts or scales on the scalp by rubbing on olive or mineral oil several hours before washing your hair. Or you can also use a de-scaling agent containing coal tar or salicylic acid these can be brought over the counter in your local pharmacy.
- Wash your hair and your beard, if you have one, with a medicated shampoo, or those containing coal tar or salicylic acid, which you can buy over the counter. Alternatively, your GP can prescribe shampoos containing ketoconazole and selenium sulphide.
- If you have severe itching on your scalp, your GP can prescribe a steroid-based cream or ointment, for you to use as a short-term solution.
- Use shampoos that contain tea tree oil.
The following treatments are recommended for the face and body.
Sweating excessively can also happen in the on state especially if you have dyskinesia .
How Is Seborrheic Dermatitis Treated
Following a skincare routine can help keep symptoms under control. Wash affected areas daily with a gentle, zinc-containing cleanser and follow up with a moisturizer. Healthy lifestyle habits, like managing stress and getting plenty of sleep, can also improve skin.
Treatment for seborrheic dermatitis is aimed at removing scales, reducing itch and calming the inflammation thats causing redness and swelling.
In infants, using an emollient such as mineral oil or petroleum jelly to gently loosen scales is usually all thats needed. Care can be more complicated for adults, who often need ongoing treatment and self-care to help prevent flare-ups.
Dermatologists usually begin treating mild cases with a topical antifungal cream or medicated shampoo, such as a prescription anti-fungal shampoo or over-the-counter dandruff product.
If the condition is more severe, intermittent use of a topical corticosteroid or calcineurin inhibitor may be required.
Read Also: Parkinson’s Bike Therapy
Patients Demographic Data And Determination Of Sd Severity
Most SD patients were male and intensity of SD was dominantly in severe or moderate form . Taking into account SD categories, there was no statistically significant difference between SDP and SDN groups in terms of SD severity: mild moderate severe . However, when SD was measured by scale there was a significant difference between SDP and SDN patients .
Table 1 Demographics and description of SD
What Is The Treatment For Seborrhoeic Dermatitis
Treatment of seborrhoeic dermatitis often involves several of the following options.
- Keratolytics can be used to remove scale when necessary, eg salicylic acid, lactic acid, urea, propylene glycol
- Topical antifungal agents are applied to reduce malassezia eg ketoconazole, or ciclopirox shampoo and/or cream. Note, some strains of malassezia are resistant to azole antifungals. Try zinc pyrithione or selenium sulphide
- Mild topical corticosteroids are prescribed for 13 weeks to reduce the inflammation of an acute flare
- Topical calcineurin inhibitors are indicated if topical corticosteroids are often needed, as they have fewer adverse effects on facial skin.
In resistant cases in adults, oral itraconazole, tetracycline antibiotics or may be recommended. Low dose oral isotretinoin has also been shown to be effective for severe or moderate seborrhoeic dermatitis.
Also Check: Idiopathic Parkinsons Disease Life Expectancy
You May Like: On And Off Phenomenon
Treatment Of Severe Seborrhea
An occasional patient with severe seborrhea that is unresponsive to the usual topical therapy may be a candidate for isotretinoin therapy.14 Isotretinoin can induce up to a 90 percent reduction in sebaceous gland size, with a corresponding reduction in the production of sebum. Isotretinoin also has anti-inflammatory properties. Treatment with daily doses of isotretinoin as low as 0.1 to 0.3 mg per kg may result in improvement in severe seborrhea after four weeks of therapy. Thereafter, a dose as low as 5 to 10 mg per day may be effective as maintenance therapy over several years. However, isotretinoin has potentially serious side effects and few patients with seborrhea are appropriate candidates for therapy. The most devastating side effect is teratogenicity, but other serious side effects include hyperlipidemia, neutropenia, anemia and hepatitis. Mucocutaneous adverse effects include cheilitis, xerosis, conjunctivitis, urethritis and hair loss. Long-term use has been associated with the development of diffuse idiopathic skeletal hyperostosis . This agent must be used cautiously and only by physicians who are well versed in all of its adverse effects.
Safety And Tolerability Of Cannabinoids
While the use of oral cannabinoids is promising, limited safety profile data exist. However, recent studies have illustrated that CBD has a favorable safety profile. In one study, PD patients treated with oral CBD experienced an improvement in quality of life as assessed by the Parkinsons Disease Questionnaire PDQ-39, a questionnaire which assesses PD-specific effects on dimensions of functioning and well-being no adverse side effects were reported . Currently, there is an ongoing phase 2 clinical trial assessing tolerability, safety and efficacy of oral cannabinoid in the treatment of dermatomyositis .
Due to variation in quality and processing of cannabinoid products, certain products may contain different active agents with various potencies such as synthetic cannabinoids, which have been shown to cause abdominal pain, hyperemesis syndrome, cannabinoid sensitization and/or allergy, and acute kidney injury . While cannabinoids have antineoplastic effects, an in vivo study has demonstrated that tumor growth may occur during early stages following exposure to CBD . Despite the conflicting data on potential adverse effects, it is important to understand the pharmacokinetics of cannabinoids and how drug-drug interaction can be of clinical concern.
Also Check: Adaptive Silverware For Parkinson’s
Determination Of Sd Severity
A clinical assessment of SD was carried out and scored. The overall SD score was calculated by scoring the severity of SD and the facial skin area affected . The severity of SD was evaluated according to the presence of: erythema, scale, infiltration and pustule. A four-point score was used for each parameter . The second scale was based on the percentage of the affected skin area: less than 10% , 10-30% , 30-50% , 50-70% and over 70% . The result was obtained by multiplying the scores of both scales giving an overall score: mild SD moderate SD and severe SD . Severity of SD has been described as: mild moderate and severe .
Pd Genetics And Lipids
Malassezia are lipid-dependent fungi which consume host lipids by secreting extracellular lipases . On the skin, they consume extracellular lipids in sebum , though they can also utilize intracellular lipids by invading keratinocytes . The best documented cases of Malassezia inside the body were reported following lipid-rich parenteral nutrition . In these cases, Malassezia were mainly found within the wall of arteries which contained lipid deposits, suggesting high lipid concentrations are required to sustain Malassezia in tissue .
Interestingly, four LRRK2 risk alleles in PD also increase the risk of CD . CD is likely caused by a T cell-mediated immune response against Malassezia in the gut . It is important to note that only LRRK2 PD risk allele Y1699C has been tested for lipid-droplet formation, and that LRRK2 alleles associated with both CD and PD have not been tested for excess lipid-droplet formation. It is also important to note that the most important LRRK2 PD risk allele G2019S did not reach statistical significance in one of the CD studies : The LRRK2 N2081D CD risk allele is located in the same kinase domain as G2019S, a mutation that is the major genetic cause of familial and sporadic PD . Notably, G2019S did not have nominally significant CD association , likely because of subtle stochastic fluctuations in allele frequencies during imputation. However, it amply reached statistical significance in the other CD study .
Read Also: Sam Waterston Parkinson’s