Stage Two Of Parkinsons Disease
Stage two is still considered early disease in PD, and it is characterized by symptoms on both sides of the body or at the midline without impairment to balance. Stage two may develop months or years after stage one.
Symptoms of PD in stage two may include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities, soft voice, monotone voice, fading volume after starting to speak loudly, slurring speech, stiffness or rigidity of the muscles in the trunk that may result in neck or back pain, stooped posture, and general slowness in all activities of daily living. However, at this stage the individual is still able to perform tasks of daily living.
Diagnosis may be easy at this stage if the patient has a tremor however, if stage one was missed and the only symptoms of stage two are slowness or lack of spontaneous movement, PD could be misinterpreted as only advancing age.
Stage One Of Parkinsons Disease
In stage one, the earliest stage, the symptoms of PD are mild and only seen on one side of the body , and there is usually minimal or no functional impairment.
The symptoms of PD at stage one may be so mild that the person doesnt seek medical attention or the physician is unable to make a diagnosis. Symptoms at stage one may include tremor, such as intermittent tremor of one hand, rigidity, or one hand or leg may feel more clumsy than another, or one side of the face may be affected, impacting the expression.
This stage is very difficult to diagnose and a physician may wait to see if the symptoms get worse over time before making a formal diagnosis.
Is Parkinsons Disease Fatal
Parkinsons disease itself doesnt cause death. However, symptoms related to Parkinsons can be fatal. For example, injuries that occur because of a fall or problems associated with dementia can be fatal.
Some people with Parkinsons experience difficulty swallowing. This can lead to aspiration pneumonia. This condition is caused when foods, or other foreign objects, are inhaled into the lungs.
You May Like: Parkinson’s Double Vision
Cognitive And Psychiatric Symptoms
- depression and anxiety
- mild cognitive impairment slight memory problems and problems with activities that require planning and organisation
- dementia a group of symptoms, including more severe memory problems, personality changes, seeing things that are not there and believing things that are not true
What Is The Prognosis And Life Expectancy For Parkinson’s Disease
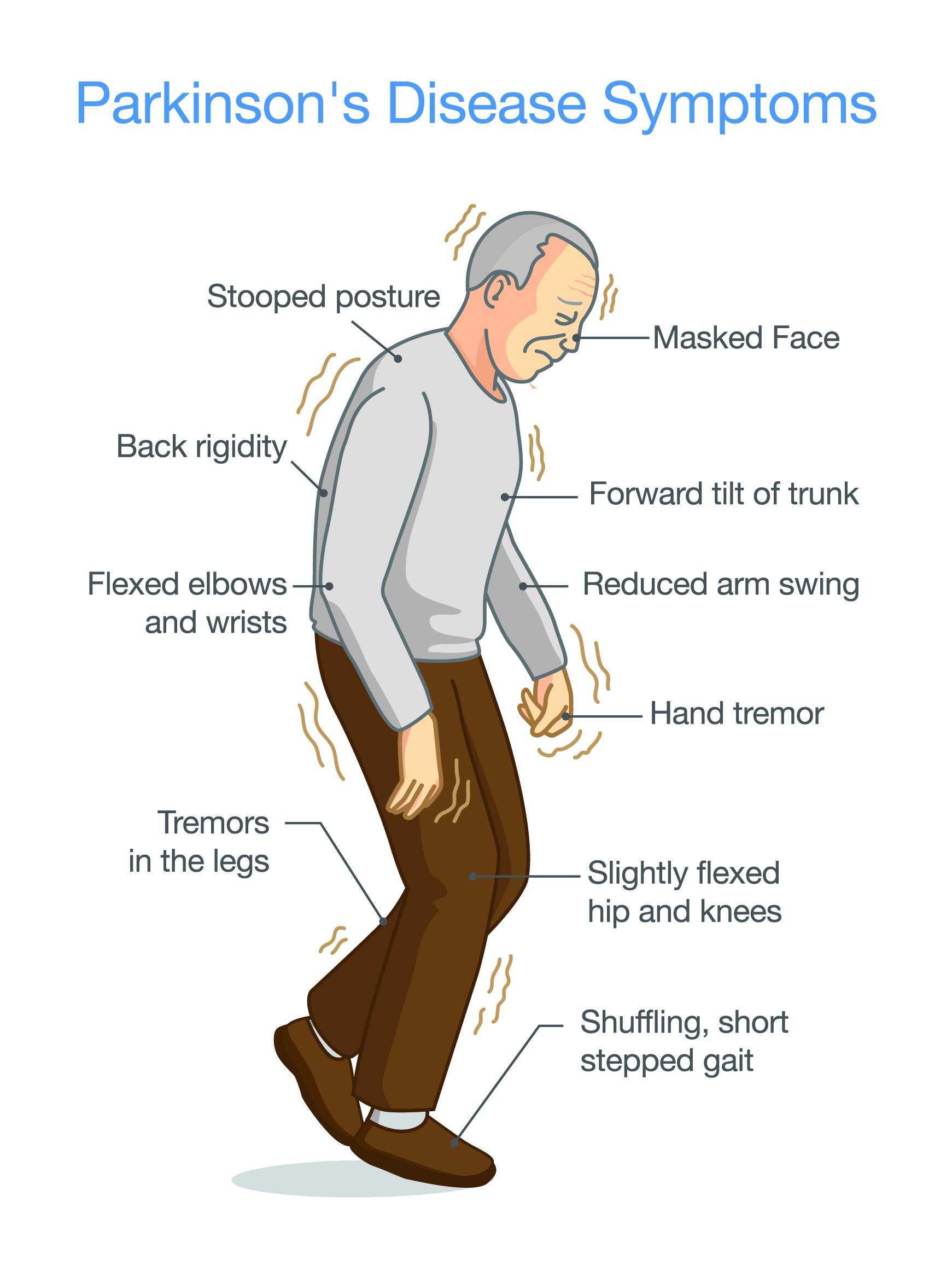
The severity of Parkinson’s disease symptoms and signs vary greatly from person to person, and it is not possible to predict how quickly the disease will progress.
- Parkinson’s disease itself is not a fatal disease, and the average life expectancy is similar to that of people without the disease.
- Secondary complications, such as pneumonia, falling-related injuries, and choking can lead to death.
- Many treatment options can reduce some of the symptoms and prolong the quality of life.
You May Like: Parkinson’s Bike Therapy
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
What Are The Symptoms Of End Stage Parkinsons Disease
End-stage Parkinsons disease dementia. The later stages of Parkinsons disease have more severe symptoms that may require help moving around, around-the-clock care, or a wheelchair. Quality of life can decline rapidly. Risks of infection, incontinence, pneumonia, falls, insomnia, and choking increase.
Also Check: Judy Woodruff Parkinson’s
How To Manage Symptoms At The End Of Life
At the end of life, good practice is to plan for any potential symptoms that may arise. The most common symptoms anticipated are pain, dyspnoea, nausea and vomiting, agitation, anxiety, delirium and noisy respiratory secretions.18 For patients with PD particular considerations should be given to the more commonly used medicines, specifically anticholinergics and antidopaminergics. These are usually prescribed for treatment of respiratory secretions and nausea and vomiting. Alternatives are available for respiratory secretions, and include glycopyrronium, in preference to hyoscine hydrobromide. Although this is an anticholinergic, only a small proportion crosses the blood brain barrier.
For nausea and vomiting, ondansetron,19 cyclizine, domperidone have all been suggested in PD.20 However, ondansetron has been shown to be inferior to domperidone in the pre-treatment of apomorphine.21 Cyclizine has anticholinergic properties and may exacerbate confusion, especially when comorbid psychosis or cognitive impairment are present. Levomepromazine, although it has antidopaminergic effects, has been shown to be effective for nausea with rotigotine in a case report.22
Agitation, dyspnoea and pain can all be managed with the same anticipatory medications as recommended.20 Specifically relating to PD, several case reports have supported the intraoperative use of midazolam, during sedation, for tremor and dyskinesias,23,24 as well as for agitation at the end of life.20
Caregiver Burden And Questionnaire Assessment
The mean ZBI score shows a tendency to be lower in LCIG group compared to CSAI or CU group, even if no statistically significant difference was found among groups . The boxplot of the ZBI Score showed that LCIG and CU populations have a very similar distribution . The CSAI ZBI boxplot distribution is slightly wider but not statistically different . The aggregated results on ZBI scores never/rarely vs. sometimes/quite frequently/nearly always did not show a significant difference between groups for each question, except for the question number 6, regarding the negative influence of the assistance on the relationship with other relatives or friends in this case, a difference was found between LCIG and CSAI . The following variables were correlated with the ZBI score: caregivers change in capability to perform family duties and leisure activities,caregivers change in work,need of professional assistance,patients judgment on QoL, and caregivers judgment on QoL.18 The analysis of the distribution of these significant associations is described in Figure 2A and B. The UPDRS-IV item 39 and the H& Y stage did not show any association with the ZBI score .
|
Figure 1 Frequency of symptoms reported by caregivers and kind of mood change in each group. |
|
Table 3 Aggregated Results for ZBI Scores in the Three Groups of Treatment. The Total Percentage in Each Group Were Computed Excluding the Missing Data |
Don’t Miss: Parkinson Bicycle Cleveland Clinic
When To Seek Hospice Care
When you or your loved one have a life expectancy of six months or less, you become eligible for hospice care a type of comfort care provided at the end of life for someone living with end-stage Parkinsons disease. Hospice provides extra support so your loved one can live as comfortably as possible.
If you have experienced a significant decline in your ability to move, speak, or participate in activities of daily living without caregiver assistance, its time to speak with a hospice professional.
Read more: What is hospice care?
Some of the things that determine whether your loved one with end-stage Parkinsons is eligible for hospice include: difficulty breathing, bed bound, unintelligible speech, inability to eat or drink sufficiently, and/or complications including pneumonia or sepsis.
If you live in South Jersey, our nurse care coordinator can answer your questions and decide if your loved one is ready for hospice care. Call us 24/7 at 229-8183.
How Is Parkinsons Disease Treated
There is no cure for Parkinsons disease. However, medications and other treatments can help relieve some of your symptoms. Exercise can help your Parkinsons symptoms significantly. In addition, physical therapy, occupational therapy and speech-language therapy can help with walking and balance problems, eating and swallowing challenges and speech problems. Surgery is an option for some patients.
Read Also: Does Vitamin B12 Help Parkinson’s
Delphi Criteria For Apd
Delphi criteria for APD were developed as a staging tool to help clinicians identify patients with APD using consistent characterization, which therefore will assist in optimizing patient treatment care . The Delphi versus physician judgment comparison was a pre-defined end point. Patients were first assessed by the investigator using their own physicians judgment and then assessed using the Delphi criteria. Independent assessments were not possible as the outcomes were determined by the same investigator. In this study, patients were assessed by movement disorder specialists using 11 indicators of suspected APD identified through a Delphi consensus methodology by an international movement disorder specialists expert group. Patients having any of the indicators were identified as having APD . As APD was determined by individual physician judgment, no comparison to other scales was conducted. Patients with ongoing DAT were not assessed using the Delphi criteria as the comparison was considered invalid as they would usually experience better clinical outcomes.
Table 1 Delphi criteria for APD
What Medications Are Used To Treat Parkinsons Disease
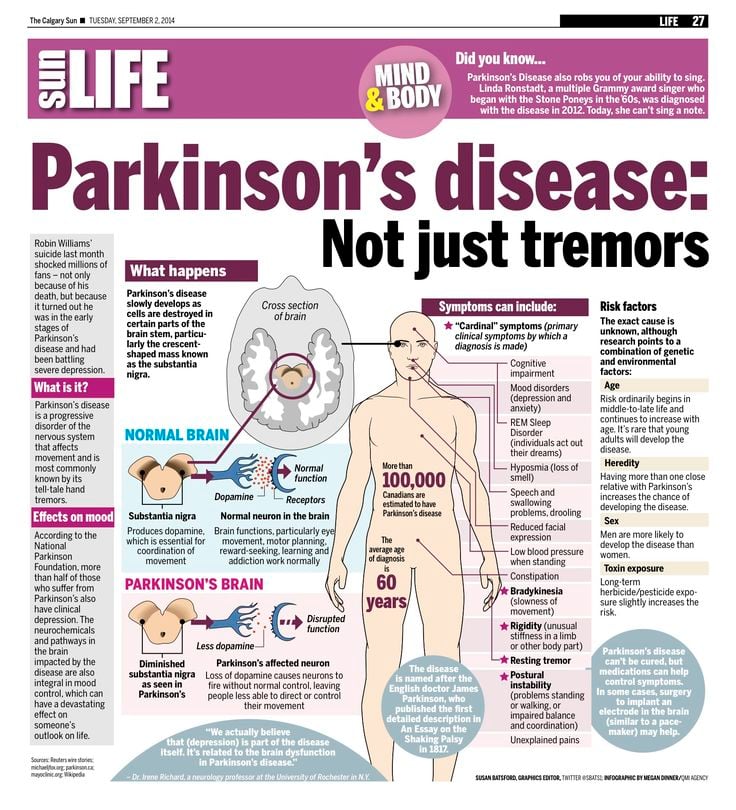
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
You May Like: Pfnca Wellness Programs
Living With Parkinsons Disease
Depending on severity, life can look very different for a person coping with Parkinsons Disease. As a loved one, your top priority will be their comfort, peace of mind and safety. Dr. Shprecher offered some advice, regardless of the diseases progression. Besides movement issues Parkinsons Disease can cause a wide variety of symptoms including drooling, constipation, low blood pressure when standing up, voice problems, depression, anxiety, sleep problems, hallucinations and dementia. Therefore, regular visits with a neurologist experienced with Parkinsons are important to make sure the diagnosis is on target, and the symptoms are monitored and addressed. Because changes in your other medications can affect your Parkinsons symptoms, you should remind each member of your healthcare team to send a copy of your clinic note after every appointment.
Dr. Shprecher also added that maintaining a healthy diet and getting regular exercise can help improve quality of life. Physical and speech therapists are welcome additions to any caregiving team.
Ethics Approval And Consent To Participate
To be included in the study, patients had to sign an authorization form to disclose personal health information and provided written informed consent. The study was approved by local ethics committees and performed according to the International Conference on Harmonization and Good Clinical Practice requirements, in accord with the principles of the Declaration of Helsinki. The local ethics committees that provided approval included those in Austria , in Belgium , in Canada , in Switzerland , in Germany , in Greece , in Ireland , in Israel , in Italy , in Turkey , in the Czech Republic , in Slovakia , in Russia , in Romania , in Hungary , in Slovenia , in Croatia , and Australia .
Don’t Miss: On Off Phenomenon
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
What Causes Parkinsons Disease
Parkinsons disease causes are still unknown. However, there is a vast amount of research directed at getting answers to its origin, treatment and prevention.
Parkinsons has been linked to declining levels of dopamine, an important brain chemical. Dopamine is a neurotransmitter. It plays a role in controlling movement and coordination. Parkinsons also causes the nerve endings to die on another neurotransmitter called norepinephrine. Norepinephrine controls automatic functions of the body, which contributes to Parkinsons symptoms such as fatigue, constipation and blood pressure changes .
Don’t Miss: Similar To Parkinsons
What Symptoms Can Be Expected In Advanced Pd
- Pain 86%
- Shortness of breath 54%
- Problems in swallowing 40%14
In an analysis of 339 death certificates and medical notes in the UK, pneumonia was found to be a terminal event in 45%.13
Caregiver distress with choking and the risk of choking to death is also mentioned in a separate study in to experiences regarding all stages of PD.4
In a survey of symptoms and their association with quality of life, in those patients with advanced disease, uncontrolled pain, anxiety and hallucinations were significantly associated with poor quality of life.9
Seizures are also noted in a description of the last phase of Parkinsonian syndromes,15 and in retrospective studies of PD patients overall.16,17
These above symptoms often occur on the background of weight loss, pain, and cognitive impairment. It is important therefore to note which medications given at the end of life may exacerbate these symptoms, and which should be considered in anticipation of them.
Depression And Parkinsons Disease
Depression is common in people with Parkinsons disease, occurring in about 40% to 50% of patients. Depression can worsen when the disease becomes more advanced and treatment becomes less effective. Mental health counseling and treatment options are available to help people living with APD. Seek help if you or a loved one is experiencing depression with their Parkinsons.
Recommended Reading: Foods To Avoid With Parkinson’s Disease
What Are The Primary Motor Symptoms Of Parkinsons Disease
There are four primary motor symptoms of Parkinsons disease: tremor, rigidity, bradykinesia and postural instability . Observing two or more of these symptoms is the main way that physicians diagnose Parkinsons.
It is important to know that not all of these symptoms must be present for a diagnosis of Parkinsons disease to be considered. In fact, younger people may only notice one or two of these motor symptoms, especially in the early stages of the disease. Not everyone with Parkinsons disease has a tremor, nor is a tremor proof of Parkinsons. If you suspect Parkinsons, see a neurologist or movement disorders specialist.
Tremors
Rigidity
Bradykinesia
Postural Instability
Walking or Gait Difficulties
Dystonia
Vocal Symptoms
What Are The Important Points Regarding Duodopa At The End Of Life
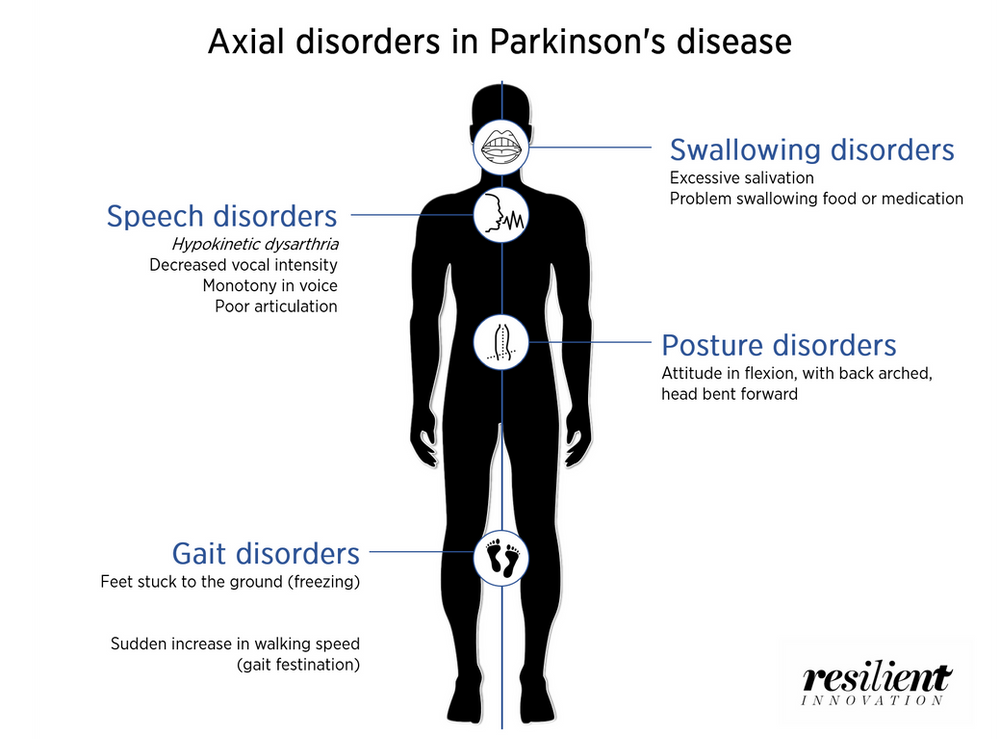
Duodopa is a continuous infusion of dopaminergic medication administered as a gel into the gut, pumped via a percutaneously inserted gastrostomy tube . There is a requirement for care of the stoma and PEG tube together with functioning of the pump by the patient or carer.41 It reduces the time in motor off periods in advanced PD and quality of life.42 There is evidence of effective treatment up until death from within a case series.43
Read Also: Sam Waterston Parkinson’s
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.