What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Who Develops Parkinson’s Disease
PD mainly develops in people over the age of 50. It becomes more common with increasing age. About 5 in 1,000 people in their 60s and about 40 in 1,000 people in their 80s have PD. It affects men and women but is a little more common in men. Rarely, it develops in people under the age of 50.
PD is not usually inherited and it can affect anyone. However, one type of PD, which appears in the small number of people who develop it before the age of 50, may be linked to inherited factors. Several family members may be affected.
Discuss With Your Physician
Non-motor symptoms can sometimes be difficult to recognize. Therefore, it is important to make your doctor aware of them.
One useful resource is the PD NMS Questionnaire. You can use this to record your symptoms and discuss them with your doctor.
Dr. Ron Postuma, whose research was funded by donations to the Parkinson Canada Research Program, has also developed tools to help people with Parkinsons and their physicians identify and manage non-motor symptoms.
Read Also: Weighted Silverware For Parkinson’s
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinsons disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinsons. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinsons disease. Electrical impulses are introduced to the brain, which has the effect of normalising the brains electrical activity reducing the symptoms of Parkinsons disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
What Are The Treatments For Parkinson’s Disease
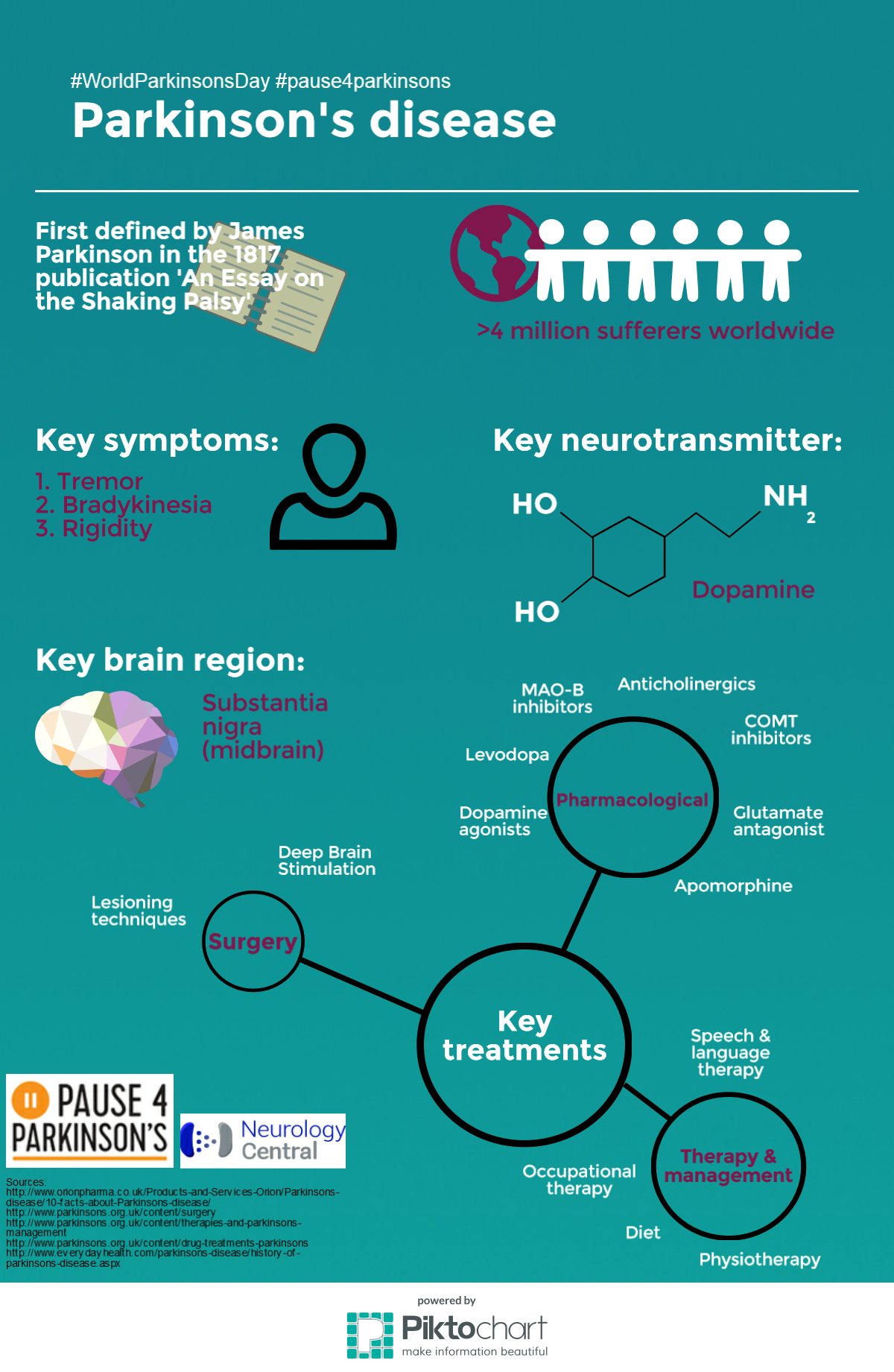
There is no cure for PD, and no treatment prevents the disease from progressing. However, treatments can usually ease symptoms.
- At first, you may not need any treatment when the symptoms are mild. A specialist may simply see you every now and then to monitor how the disease is progressing.
- A medicine that eases symptoms is usually started when symptoms become troublesome.
- Therapies such as physiotherapy, occupational therapy and speech therapy may also be useful as the disease progresses.
- Surgery may be an option for severe cases.
You May Like: Parkinson’s Support Group Long Island
When I Am In The Hospital Why Don’t I Always Get My Medications On Time
Hospitals and hospital pharmacies have their own dosing schedules. A medication written for “TID ” may be given at 7 AM – 3 PM – 11 PM or some other standard schedule. Many hospitals may have a policy that permits nurses to give medications at times different from the scheduled time. This policy is a practical compromise because nursing staffs are busy and each nurse cares for multiple patients. Such a policy provides nurses time to complete their scheduled duties and allows flexibility in case of emergencies on the ward. As a result, it may seem that patients with Parkinson’s disease receive their medications at random times.
How can such a situation be remedied? First, make sure that the drug schedule, with specific times, is written into the doctor’s orders. Check that the physician knows when it should be given. Bring with you the complete list of your medications with the correct dosage. Talk with your nurse about the importance of receiving your medications on time. Explain that, without the medications, you can be immobile or uncomfortable and that the medications allow you to move around independently. You may know more about Parkinson disease than the doctor and the staff, so it is your responsibility to help them understand your situation. While you will still need to be somewhat flexible, sharing your knowledge can alleviate many problems. The staff wants patients to be well cared for during their stay.
Support For People With Parkinsons Disease
Early access to a multidisciplinary support team is important. These teams may include doctors, physiotherapists, occupational therapists, speech therapists, dietitians, social workers and specialist nurses. Members of the team assess the person with Parkinsons disease and identify potential difficulties and possible solutions.There are a limited number of multidisciplinary teams in Victoria that specialise in Parkinsons disease management. But generalist teams are becoming more aware of how to help people with Parkinsons disease.
Read Also: Who Discovered Parkinson’s Disease
Complex Parkinson’s Disease And Palliative Care
Complex Parkinson’s disease is defined as the stage when treatment is unable to consistently control symptoms, or the person has developed uncontrollable jerky movements .
These problems can still be helped by adjustment or addition of some of the medications used to treat Parkinson’s disease, under the supervision of a doctor with a specialist interest in Parkinson’s disease.
As Parkinson’s disease progresses, you’ll be invited to discuss the care you want with your healthcare team as you near the end of your life. This is known as palliative care.
When there’s no cure for an illness, palliative care tries to alleviate symptoms, and is also aimed at making the end of a person’s life as comfortable as possible.
This is done by attempting to relieve pain and other distressing symptoms, while providing psychological, social and spiritual support for you and your family.
Palliative care can be provided at home or in a hospice, residential home or hospital.
You may want to consider talking to your family and care team in advance about where you’d like to be treated and what care you wish to receive.
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms
Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
Recommended Reading: Parkinson’s Disease And Brain Function
What Is The History Of The Discovery Of Levodopa
There were several seminal discoveries that led to the development of levodopa as a therapy for Parkinsons disease:
- 1911 First synthesis of its D,L racemate and the isolation of its L-isomer from the seedling of Vicia faba beans
- 1913 Isolation from legumes
- 1930 L-Dopa was shown to have an effect on Rabbit glucose metabolism
- 1938 L-dopa decarboxylase described and enzymatic conversion to dopamine demonstrated
- 1940 Studies on the effects of L-Dopa on blood vessels
- 1950 Studies began to consider the use of dopamine on the brain
- 1960 Consideration was given to Parkinsons disease treatment which was found to be related to dopamine
- 1967 High dose levodopa was verified for treatment of patients suffering with Parkinsons disease
- 1970s Dopamine decarboxylase was added to the regimen to improve the side effect profile and absorption
Many scientists have worked on the development of levodopa and levodopa therapy and the list of their names is too long for a short book such as this. Arvid Carlsson from Sweden won the Nobel Prize in 2000 for his work on the administration of levodopa to animals , and Oliver Sacks .
The Facts About Parkinsons Disease
Parkinson’s disease is a progressive neurogenerative disease that causes nerve cells in the area of the brain that controls movement to weaken and/or die. While healthy neurons produce a chemical called dopamine, which the brain needs a certain amount of in order to regulate movement, weakened neurons produce lower levels of dopamine. What causes these neurons to weaken is currently unknown.
Some patients with Parkinson’s disease also suffer from a decline in norepinephrine, a chemical that transmits signals across nerve endings and controls various functions, such as blood pressure and heart rate.
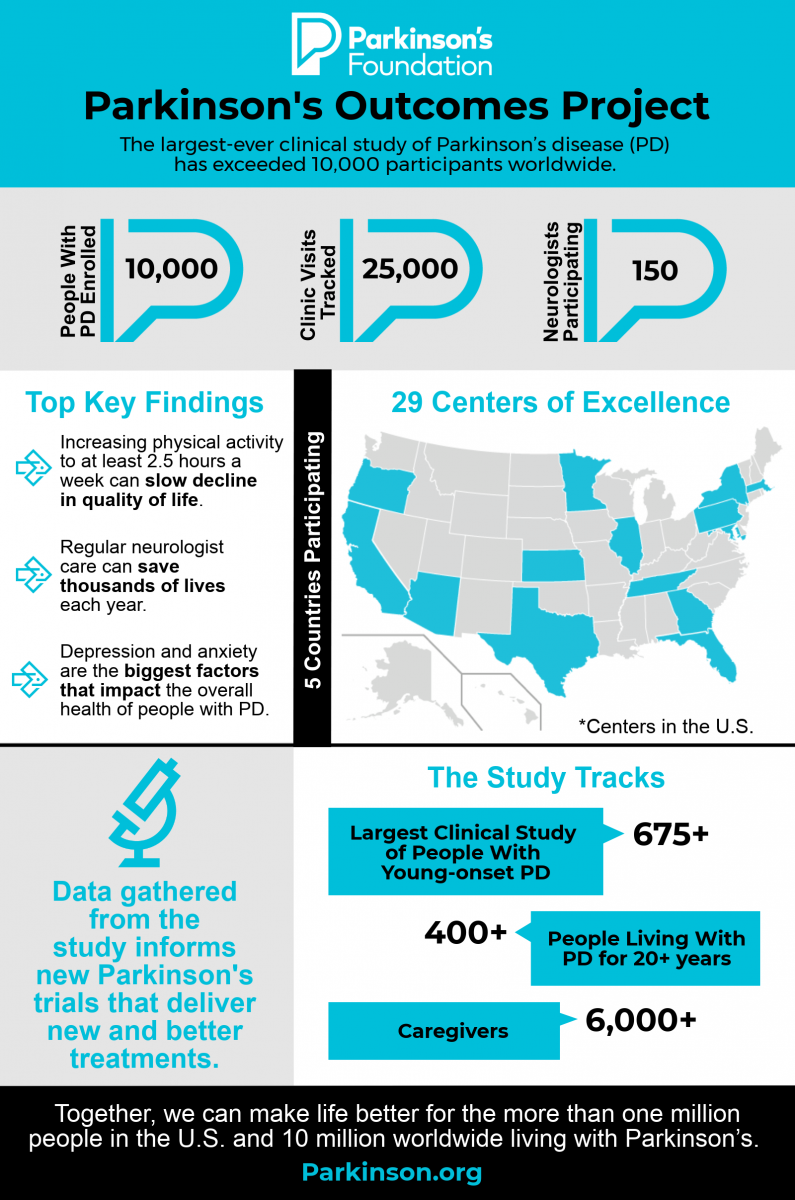
More than 10 million people worldwide are currently living with Parkinson’s disease and nearly one million will be living with the disease in the United States this year, according to the Parkinson’s Foundation.
Recommended Reading: How Do You Stop Parkinson’s Tremors
Does Parkinson’s Disease Cause Dementia
The cells in the brain affected in PD are not in the ‘thinking’ parts of the brain and dementia is not a typical early feature of PD. However, if you have PD you have an increased risk of developing dementia. About half of people with PD develop dementia at some stage. If dementia occurs, it tends to develop in older people with PD . Early dementia in younger people with PD virtually never develops. It is thought that PD alone does not cause dementia however, other age-related factors in addition to PD may increase the risk of dementia developing.
Who Gets Parkinsons Disease
Parkinsonâs disease, documented in 1817 by physician James Parkinson, is the second most common neurodegenerative disease after Alzheimerâs disease. Estimates regarding the number of people in the United States with Parkinsonâs range from 500,000 to 1,500,000, with 50,000 to 60,000 new cases reported annually. No objective test for Parkinsonâs disease exists, so the misdiagnosis rate can be high, especially when a professional who doesnât regularly work with the disease makes the diagnosis.
You May Like: Parkinson’s Fight Club The Villages Fl
Give Yourself Time To Adjust
Over time, youll likely become an expert in Parkinsons disease but right now, youre a newbie. Give yourself time for the diagnosis and all it might mean to sink in. Then, get educated: Ask your doctor for information you can take home and read, find other people with Parkinsons in your community or online to talk to, and browse sites like the National Parkinson Foundation and the Michael J. Fox Foundation for Parkinson’s Research.
Exercise And Healthy Eating
Regular exercise is particularly important in helping relieve muscle stiffness, improving your mood and relieving stress.
There are many activities you can do to help keep yourself fit, ranging from more active sports like tennis and cycling, to less strenuous activities such as walking, gardening and yoga.
You should also try to eat a balanced diet containing all the food groups to give your body the nutrition it needs to stay healthy.
You May Like: Can Parkinson’s Cause Congestive Heart Failure
Resources For Specialized Populations
For Care Partners
When one person in a couple or family is affected by Parkinsons disease, the other family members live with it as well. To keep your care partnering relationship healthy and balanced, its important that the care partner finds time to take a break from caregiver duties, has some outside interests, and has others they can turn to for support and resource information.
Young Onset Parkinsons Disease
For those who have been diagnosed under the age of 50, APDA provides resources and information to help younger people with Parkinsons Disease live active and productive lives. Our Early/Young Onset section offers a wide range of resource links and discusses issues that are particularly relevant to people with young onset Parkinsons disease, such as ongoing employment, parenting, and planning for the near and distant future.
Veterans with PD
In 2017, APDA published Helping Those Who Serve: Parkinsons Disease Information for Veterans Community. This manual offers general information about Parkinsons diagnosis, symptoms and treatment, tips for coping with disease progression and support for care partners. It also provides step by step directions on how to access the Veterans Affairs system and receive care from the VA PADRECC and consortium centers across the country. The manual is accessible on the page linked below, and in print.
Email:
What Causes Parkinsons Movement Symptoms
Dopamine is a chemical messenger that is primarily responsible for controlling movement, emotional responses and the ability to feel pleasure and pain. In people with Parkinsons, the cells that make dopamine are impaired. As Parkinsons progresses, more dopamine-producing brain cells die. Your brain eventually reaches a point where it stops producing dopamine in any significant amount. This causes increasing problems with movement.
Page reviewed by Dr. Chauncey Spears, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
Recommended Reading: Do You Get Pain With Parkinson’s
Causes Of Parkinsons Disease
At present, we do not know the cause of Parkinsons disease. In most people there is no family history of Parkinsons Researchers worldwide are investigating possible causes, including:
- environmental triggers, pesticides, toxins, chemicals
- genetic factors
- combinations of environment and genetic factors
- head trauma.
Factors That May Make Your Symptoms Worse:
- Failure to get medications at specific times and coordinated with meals.
- Certain dopamine blocking drugs can worsen symptoms. If absolutely necessary because of hallucinations or behavior, only quetiapine or clozapine should be used.
- Anxiety, stress, and sleep deprivation
- Urinary tract, lung, or other infections
- Provide Advance Directives: Power of attorney for health care and living will. Choose an advocate who can ask questions and act as your spokesperson. Make sure this person is aware of your medical wishes so he or she can assist in speaking for you if needed.
Also Check: Parkinson’s Coughing At Night
What Can You Do If You Have Pd
- Work with your doctor to create a plan to stay healthy. This might include the following:
- A referral to a neurologist, a doctor who specializes in the brain
- Care from an occupational therapist, physical therapist or speech therapist
- Meeting with a medical social worker to talk about how Parkinson’s will affect your life
For more information, visit our Treatment page.
Page reviewed by Dr. Chauncey Spears, Movement Disorders Fellow at the University of Florida, a Parkinsons Foundation Center of Excellence.
Incidence Of Parkinsons Disease

Its estimated that approximately four people per 1,000 in Australia have Parkinsons disease, with the incidence increasing to one in 100 over the age of 60. In Australia, there are approximately 80,000 people living with Parkinsons disease, with one in five of these people being diagnosed before the age of 50. In Victoria, more than 2,225 people are newly diagnosed with Parkinsons every year.
Also Check: Anxiety And Parkinson’s Disease
When Does Parkinson Disease Really Start
This is one of the million dollar questions in Parkinsons disease research. We actually dont know the answer. From the clinical trial or research perspective, we arbitrarily base the answer on either the occurrence of the first symptom or alternatively the date of diagnosis. The date of diagnosis is however biased, and largely based on obvious motor symptoms such as tremor, stiffness, or slowness. We know that this estimate therefore is grossly inaccurate. In fact, by the time a Parkinsons disease patient manifests the first symptom , significant degeneration of the dopaminergic neurons in the brain has already occurred.
We now know that the loss of the sense of smell, constipation, depression, personality changes, sleep problems, and even anxiety may long precede the motor symptoms of Parkinsons disease. The problem with using these symptoms as diagnostic markers however, is that they commonly occur in the general population, making it very difficult to judge what is part of Parkinsons disease, and what is not.
Complicating the picture as to the onset of Parkinsons disease has been the discovery that many patients may have rapid eye movement sleep disorders many years prior to the onset of motor symptoms. Additionally, Braak and colleagues have recently proposed that the degeneration in Parkinsons disease actually starts well before dopaminergic cells in the midbrain begin to die. The cells that die in Parkinsons disease are deep in an area called the brainstem.