Common Signs Of Young Onset Parkinsons
Symptoms of Young Onset Parkinsons are often different from Parkinsons that develops later in life. In young onset Parkinsons the first symptom is often dystonia: involuntary muscle contractions that may cause stiffness, twisting and repetitive motions in the limbs. Leg or foot dystonia is particularly common affecting up to 50 percent of diagnosed young people.
Many of the more common signs of Parkinsons in the elderly are less common early on in young onset Parkinsons disease, such as tremors, cognitive problems including memory loss and dementia, and loss of balance and coordination.
If Its Not Parkinsons Disease What Else Could It Be
There are several other conditions that might produce symptoms that can be mistaken for Parkinsons disease. Here are some possibilities:
- Medication side effects: Certain drugs can produce or exacerbate symptoms.
- Essential, or familial, tremor: This is a relatively common and benign cause of recurrent tremor and is often confused with the tremor of idiopathic Parkinsons. A general neurologist or movement disorder specialist is the best physician to help differentiate between these two conditions.
- A Parkinsonian syndrome: The symptoms of several neurologic conditions are similar to those of idiopathic Parkinsons, but they are often managed differently and often do not respond to the typical medications.
Remember: Only a general neurologist or movement disorder specialist can tell you with reasonable certainty if you have idiopathic Parkinsons. If for some reason you are not comfortable with the results of your first physician visit, getting a second opinion from another general neurologist or movement disorder specialist is always an option. It is important that you feel comfortable with your physician to ensure the best possible outcome for you.
Once you or your loved one has a diagnosis of Parkinsons disease, it is time to discuss treatment options with your physician.
What Research Has Been Done And The Need To Improve:
CANTAB Connect for Parkinsons disease is a rapid, reliable, and highly sensitive system for academic research or clinical trials. The CANTAB battery has demonstrated potential advantages when compared to other neuropsychological tests, such as for detecting cognitive impairment in Parkinsons disease7 and also avoiding floor and ceiling effects. It is highly sensitive to disease progression, can discriminate cognitive impairment due to comorbid depression, and detects untoward effects of medications on cognition11-14. It has also been shown to predict conversion to dementia in patients with Parkinsons disease15. The use of CANTAB in research of Parkinsons disease is clinically relevant: cognitive decline measured by the battery correlates with loss of day-to-day functioning in patients with Parkinsons disease16.
Furthermore, CANTAB maximises scope for sample enrichment, and for demonstrating disease modifying capability of interventions.
There are currently over 125 peer-reviewed publications supporting the application of CANTAB in research of Parkinsons disease. To find out more, .
Read Also: Best Parkinson’s Doctors In Houston
How Soon After Treatment Will I Feel Better And How Long Will It Take To Recover
The time it takes to recover and see the effects of Parkinson’s disease treatments depends strongly on the type of treatments, the severity of the condition and other factors. Your healthcare provider is the best person to offer more information about what you can expect from treatment. The information they give you can consider any unique factors that might affect what you experience.
Imaging And Lab Tests

Your doctor may order some imaging tests and laboratory tests. Imaging tests can include computed tomography scans and magnetic resonance imaging scans. Laboratory tests can include blood tests and urine tests.
While these tests and scans will not help diagnose Parkinsons disease, they can help rule out other conditions that have similar symptoms.
Your doctor may also suggest that you get a dopamine transporter scan . This scan requires a single-photon emission computed tomography scanner. It involves an injection of a small amount of a radioactive drug so that your doctor can study the dopamine systems in your brain .
While a DaTscan cannot conclusively prove that you have Parkinsons, it can help confirm your doctors diagnosis and eliminate other conditions.
Don’t Miss: Acupuncture And Parkinson’s Tremors
What Is The Pattern Of Disease In Pd
The onset of PD usually occurs in patients in their sixties, and the disease progresses slowly. Although PD eventually results in severe disability and often dementia, life expectancy is not significantly shortened. Death is often due to secondary problems associated with the disease such as falls, pneumonia, aspiration, and immobility.
Figure 2. The onset of Parkinsons disease usually occurs in patients older than 60 and the disease progresses slowly.
Also Check: What Is The Difference Between Parkinsons And Alzheimers
Why Is Expert Care Important
Early expert care can help reduce PD complications. Findings show that 60 percent of people with Parkinsons fall short of getting the expert care they need. The National Parkinson Foundation has estimated that about 6,400 people with Parkinsons die unnecessarily each year due to poor care.
Trained neurologists will help you recognize, treat and manage the disease. Common approaches include medication, surgical treatment, lifestyle modifications , physical therapy, support groups, occupational therapy and speech therapy. The best approach is interdisciplinary care, where you are seen by multiple specialists on a regular basis and all of the specialists talk and arrange the best possible coordinated care. This is what is referred to as a patient-centric approach to Parkinsons care.
Read Also: What Kills A Person With Parkinsons Disease
Also Check: Very Early Signs Of Parkinson’s Disease
Surgery For People With Parkinsons Disease
Deep brain stimulation surgery is an option to treat Parkinsons disease symptoms, but it is not suitable for everyone. There are strict criteria and guidelines on who can be a candidate for surgery, and this is something that only your doctor and you can decide. Surgery may be considered early or late in the progression of Parkinsons. When performing deep-brain stimulation surgery, the surgeon places an electrode in the part of the brain most effected by Parkinsons disease. Electrical impulses are introduced to the brain, which has the effect of normalising the brains electrical activity reducing the symptoms of Parkinsons disease. The electrical impulse is introduced using a pacemaker-like device called a stimulator. Thalamotomy and pallidotomy are operations where the surgeon makes an incision on part of the brain. These surgeries aim to alleviate some forms of tremor or unusual movement, but they are rarely performed now.
Is There Anything I Can Do To Slow The Progression Of Parkinsons Symptoms
Treatment for Parkinsons can help you manage your symptoms. Currently, theres no way to cure or stop the progression of Parkinsons. However, medical professionals have found ways to slow the progression of symptoms with therapies such as medications and deep brain therapy.
Diet and exercise are also known to slow down Parkinsons. Studies have shown that eating a nutritious diet, such as the Mediterranean diet, can help slow down the progression of Parkinsons disease.
Additionally, getting regular exercise has been shown to slow down symptom progression. People with Parkinsons should try to get at least 2.5 hours of exercise each week. A physical therapist or another medical professional can help you develop an exercise routine that meets your needs.
Don’t Miss: Wolff Parkinson White Syndrome Causes
Medications For People With Parkinsons Disease
Symptoms of Parkinsons disease result from the progressive degeneration of nerve cells in the brain and other organs such as the gut, which produce a neurotransmitter called dopamine. This causes a deficiency in the availability of dopamine, which is necessary for smooth and controlled movements. Medication therapy focuses on maximising the availability of dopamine in the brain. Medication regimes are individually tailored to your specific need. Parkinsons medications fit into one of the following broad categories:
- levodopa dopamine replacement therapy
- dopamine agonists mimic the action of dopamine
- COMT inhibitors used along with levodopa. This medication blocks an enzyme known as COMT to prevent levodopa breaking down in the intestine, allowing more of it to reach the brain
- anticholinergics block the effect of another brain chemical to rebalance its levels with dopamine
- amantadine has anticholinergic properties and improves dopamine transmission
- MAO type B inhibitors prevent the metabolism of dopamine within the brain.
How Parkinsons Disease Is Diagnosed
Diagnosing Parkinsons disease can be complicated because there isnt a specific blood test or screening test that can determine whether or not you have it.
Instead, Parkinsons is diagnosed clinically, which means a doctor will examine you, review your symptoms and medical history, and diagnose accordingly.
Parkinsons disease is a neurological condition that can make movement difficult. If your general practitioner thinks you might have Parkinsons, they may refer you to a neurologist who specializes in movement disorders for a diagnosis.
It can be challenging to catch Parkinsons in the early stages because the symptoms may be too mild to notice or meet the diagnostic criteria. Also, early Parkinsons symptoms are often mistaken for typical signs of aging.
The symptoms of Parkinsons disease are also similar to those of other health conditions, which may be misdiagnosed as Parkinsons at first. Your doctor may suggest specific tests and scans to help eliminate other conditions that can mimic the symptoms of Parkinsons disease.
Don’t Miss: Does Parkinson’s Cause Dry Mouth
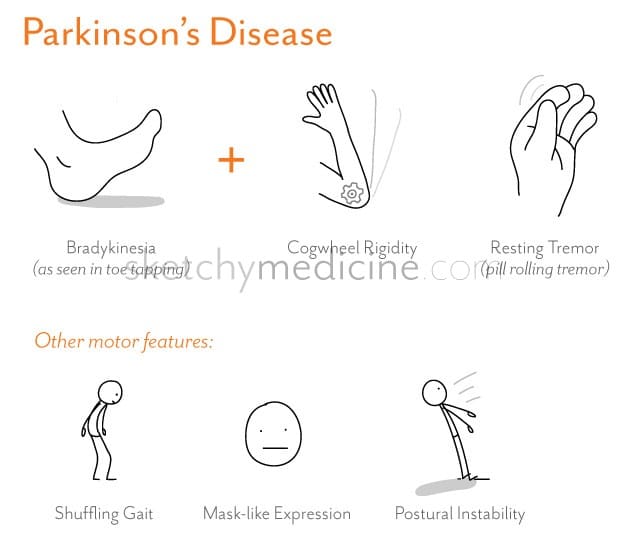
Diagnosis Of Parkinson Disease: Motor Symptoms
The clinical diagnosis of Parkinson’s disease is based on the presence of characteristic motor symptoms: bradykinesia, rigidity, postural instability, and resting tremor but neuropathology is still considered the gold standard for definite diagnosis. Differentiating PD from other movement disorders can be challenging throughout the disease course, because signs and symptoms often overlap. Indeed, neuropathology studies reveal that clinical diagnosis of PD can be confirmed with an accuracy of about 75%. Good response to levodopa is often used to support the diagnosis of PD. However, cases of pathologically proven PD with poor response to levodopa have also been reported.
Misdiagnosis of PD can occur for several reasons. In a community-based study of patients taking antiparkinsonian medication, the most common misdiagnosis were essential tremor, Alzheimer’s disease, and vascular parkinsonism. In addition, many of the prominent features of PD may also occur as a result of normal aging or from comorbid and multifactorial medical conditions .
R. Savica, … G. Logroscino, in, 2016
I Have Pd And Several Symptoms Should I Get A Datscan
Likely no. There is no need for DaTscan when your history and exam suggest Parkinsons disease and you meet the diagnostic criteria. Occasionally, if signs and symptoms are mild or you dont meet the diagnostic criteria, your doctor will refer you for a DaT scan. Keep in mind that ultimately the diagnosis is based on your history and physical exam. The DaT scan is most commonly used to complete the picture and is not a test for a diagnosis.
Read Also: Tao Patch For Parkinson’s
Symptoms Of Parkinsons Disease
Parkinsons has four main symptoms:
- Tremor in hands, arms, legs, jaw, or head
- Muscle stiffness, where muscle remains contracted for a long time
- Slowness of movement
- Impaired balance and coordination, sometimes leading to falls
Other symptoms may include:
The symptoms of Parkinsons and the rate of progression differ among individuals. Early symptoms of this disease are subtle and occur gradually. For example, people may feel mild tremors or have difficulty getting out of a chair. They may notice that they speak too softly, or that their handwriting is slow and looks cramped or small. Friends or family members may be the first to notice changes in someone with early Parkinsons. They may see that the persons face lacks expression and animation, or that the person does not move an arm or leg normally.
People with Parkinson’s disease often develop a parkinsonian gait that includes a tendency to lean forward take small, quick steps and reduce swinging their arms. They also may have trouble initiating or continuing movement.
Symptoms often begin on one side of the body or even in one limb on one side of the body. As the disease progresses, it eventually affects both sides. However, the symptoms may still be more severe on one side than on the other.
What Is A Datscan
A DaTscan is an imaging drug, also called Ioflupane I 123 or phenyltropane, that acts as a radioactive tracer for dopamine transporters within the brain. This drug was approved by the FDA in 2011. It may help distinguish the diagnosis of essential tremor from Parkinsons syndromes, like Parkinsons disease or Parkinsons disease dementia.
The drug is administered during the SPECT scan. This scanning technique gathers images of a particular area in the brain called the striatum, a cluster of neurons in the subcortical basal ganglia of the forebrain. The striatum helps facilitate the transportation of dopamine.
DaTscan is injected into the patients bloodstream and eventually circulates to the brain. The tracer attaches itself to a molecule found on dopamine neurons in the striatum called the dopamine transporter . The patient then undergoes a SPECT scan which will produce an image of the dopaminergic neuron terminals that remain available in the striatum.
In patients with a diagnosis of Parkinsons disease, or parkinsonism , this area of the brain will show dark. This indicates the loss of dopamine-containing nerve cells within the brain, a hallmark of the disease.
You May Like: Judy Woodruff Parkinsons
Don’t Miss: Can Vyvanse Cause Parkinson’s
Woman Who Can Smell Parkinsons Disease Helps Scientists Develop 3
Scientists in the UK have harnessed one womans extraordinary sense of smell to develop a test that could determine in just three minutes whether people have Parkinsons disease.
Researchers at the University of Manchester were helped by Joy Milne, a Scottish grandmother who discovered she could detect the neurodegenerative illness in people from their distinct body odour.
British media report that the 72-year-old, who has hereditary hyperosmia a heightened sensitivity to smells noticed that her late husband developed a different odour more than a decade before he was diagnosed with Parkinsons.
She described a musky aroma, different from his normal scent.
The team in Manchester investigated her observation and discovered that Parkinsons disease indeed has a particular odour. They found the smell is strongest on patients upper backs, where sebum, an oily substance produced by the skin, tends to amass.
The researchers have since designed a test that can identify people with Parkinsons using a simple cotton swab run along the back of their neck.
We are tremendously excited by these results which take us closer to making a diagnostic test for Parkinson’s disease that could be used in clinic, Professor Perdita Barran, who led the research, said in a statement.
‘it Has To Be Detected Far Earlier’
Mrs Milne said that it was “not acceptable” that people with Parkinson’s had such high degrees of neurological damage at the time of diagnosis, adding: “I think it has to be detected far earlier – the same as cancer and diabetes – earlier diagnosis means far more efficient treatment and a better lifestyle for people.
“It has been found that exercise and change of diet can make a phenomenal difference.”
She said her husband, a former doctor, was “determined” to find the right researcher to examine the link between odour and Parkinson’s, and they sought out Dr Tilo Kunath at the University of Edinburgh in 2012.
Dr Kunath paired up with Professor Perdita Barran to examine Mrs Milne’s sense of smell.
The scientists believed that the scent may be caused by a chemical change in skin oil, known as sebum, that is triggered by the disease.
Researchers hoped the finding could lead to a test being developed to detect Parkinson’s, working under the assumption that if they were able to identify a unique chemical signature in the skin linked to it, they may eventually be able to diagnose the condition from simple skin swabs.
In 2019, researchers at the University of Manchester, led by Prof Barran, announced that they had identified molecules linked to the disease found in skin swabs and now the scientists have developed a test using this information.
The tests have been successfully conducted in research labs, and scientists are assessing whether they can be used in hospital settings.
Read Also: Why Parkinson’s Disease Occurs
New Test For Parkinsons Developed After Woman Sniffed Out The Disease
A new Parkinsons test has been developed after scientists were able to harness the power of a woman who can sniff out the disease.
The test has been years in the making after researchers at Manchester University realised that Joy Milne of Perth, Scotland, could smell the condition.
The academics first began to believe Parkinson’s might have a discernible odour when Mrs Milne claimed she detected a change in the odour of her husband, Les, six years before he was diagnosed with the condition.
Mrs Milne, 72, said that her husbands smell changed subtly to a “musky” aroma years before any difficulty with movement started to emerge. Mr Milne died in 2015 aged 65.
When researchers conducted tests with Mrs Milne, they found she was able to identify people living with Parkinson’s from people without the condition just by smelling the t-shirts they had worn.
In preliminary lab work, she was also able to identify that one t-shirt from the group of people without the condition smelled like the disease, and eight months later the individual wearing it was diagnosed with Parkinson’s.
Now, the academics at the University of Manchester have made a breakthrough by developing a test which can identify people with the condition by using a simple cotton bud run along the back of the neck.
Researchers can examine the sample to identify molecules linked to the condition to help diagnose whether someone has the disease.