Cold Hands And Feet And Skin Mottling
Hands and feet may become colder and the skin may look blotchy and purplish . It happens because the heart is no longer able to pump blood as well. As a result, blood pressure goes down and the skin grows colder.
This mottling may slowly work its way up the arms and legs. The lips and nail beds can turn blue or purple too.
What Are The End Stages Of Parkinsons Disease
The final stages of Parkinsons disease occur when patients experience severe symptoms. Most of the time, medication only helps a little, and they can experience disabilities that can lead to the patients death.
Here are the Parkinsons death signs of the fourth and fifth stages:
For stage four of Parkinsons disease:
- Softer speaking voice
Adjusting Medications For Motor Symptoms
Over time, treatments for Parkinsons, such as levodopa, become less effective, and the risk of side effects increases. Problems with drug absorption in the gut and decreased sensitivity to levodopa can lead to a wearing off effect that causes worsening of symptoms before the next dose is given.
People can also experience off time when medication does not work and motor symptoms can increase. These effects can be minimized by changing your medication dosage or by adding on other medications. Breaking down levodopa doses into smaller doses given more frequently can help some people.
The addition of drugs such as the monoamine oxidase inhibitors rasagiline and amantadine or the dopamine agonist apomorphine can improve how levodopa works.
A class of drugs called catechol-O-methyltransferase inhibitors, such as entacapone and tolcapone , can slow the breakdown of levodopa in the body, allowing its effects to last longer.
Also Check: Is Parkinson’s A Prion Disease
What Are The Risks Of Not Receiving Any Dopaminergic Medication
There is the possibility of neuroleptic malignant-like syndrome , a life-threatening and distressing condition resulting in rigidity and fever, from withdrawal of therapy.31 This can also occur with sudden cessation of Deep Brain Stimulation .32,33,34 To reduce the risk of this, dopaminergic therapy at the end of life should be continued.27 It should also be noted that in a patient dying of another condition, whose PD is still responsive to dopaminergic medication, the cessation of this also risks aspiration pneumonia.35 Transdermal rotigotine can be used in patients in whom a NG tube may cause excessive distress or is not possible. The dose should be calculated with an accepted converter.36
Causes Of Parkinsons Disease
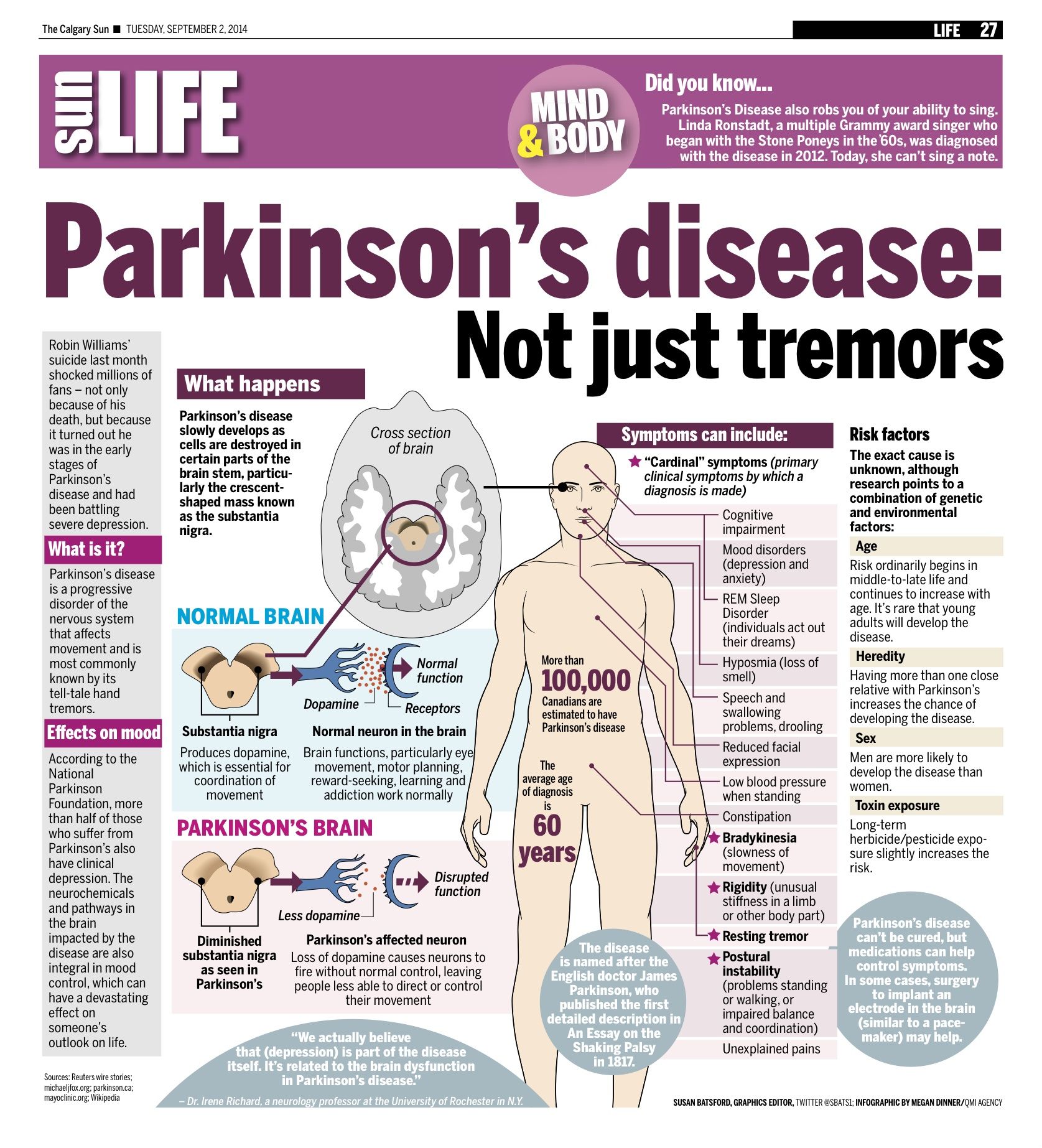
Parkinsons disease is caused by a loss of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in the brain.
Dopamine plays a vital role in regulating the movement of the body. A reduction in dopamine is responsible for many of the symptoms of Parkinsons disease.
Exactly what causes the loss of nerve cells is unclear. Most experts think that a combination of genetic and environmental factors is responsible.
Also Check: Ginkgo Biloba For Parkinson’s
My Parkinson’s Story: Advanced Parkinsons
This 10-minute video alternates between an interview with a man and his wife and his palliative care team, including a doctor, nurse, clerg and social worker. The man and his wife shares his experience with late stage Parkinson’s. The palliative care team explains that their job is to support the best physical, emotional and spiritual wellbeing of the immediate family as well as help the family make end of life decisions.
Managing Care In Late Stages
, March 3, 2017
What to expect in the late stages of Parkinsons disease and the challenges of caring with those difficulties and needs. Tips for helping someone overcome freezing, accomplishing activities of daily living as long as possible, managing medications and swallowing issues, and ways to minimize caregiver stress.
Don’t Miss: Parkinson Like Tremors In Dogs
What Is An Advance Decision To Refuse Treatment
During the course of an individuals advance care planning discussion they may indicate that they wish to make an advance decision to refuse certain treatments.
This is a separate document to that of the ACP and must be instigated by a professional who is competent in this process. They are required to follow the guidance available in the Code of Practice for the Mental Capacity Act on Advance Decision to Refuse Treatment in England, Wales and Northern Ireland. In Scotland professionals must follow guidance available in the Adults With Incapacity Act .
- An Advance Decision to Refuse Treatment allows the person who is 18 years of age or over to specify what treatments they would not want and would not consent to later in life. In Scotland the age of advanced directives is 16. They cannot demand certain treatments or refuse basic care, ie offers of food and water by mouth, warmth, shelter and hygiene. But clinically assisted nutrition and hydration given by intravenous, subcutaneous or gastroscopy are considered medical interventions and can be refused. These decisions can be withdrawn if the individual gains or retains capacity.
- All healthcare providers must respect the individuals advance decision and ensure it is incorporated into the person-centred care planning. They will also have discussed who is to be made aware of the ADRT and where they wish to store it in the home. A copy of the document should be stored in their healthcare notes and their GP made aware.
Parkinson’s Progression Palliative And End Of Life Issues
This 38-minute webinar provides an overview of Parkinson’s symptoms, and treatment challenges due to disease progression. 18-minutes in the topic turns to planning a good death, the euphemisms even doctors use to avoid discussing death, the most common cause of death in those with PD, putting your end-of-life preferences in writing. Palliative care can help families face these end-of-life issues.
Read Also: What Is Similar To Parkinson Disease
What To Do With Deep Brain Stimulation At The End Of Life
Deep brain stimulation uses an Implantable Pulse Generator, usually placed in the infraclavicular area, connected to leads within the brain. There is a remote programmer, and also a charging unit in the case of a rechargeable device, which are given to the patient and their carer. It improves dyskinesias and also has a levodopa sparing effect.37
Deactivation of DBS may lead to increased symptom burden as mentioned in the section above and so awareness of features of PHS should be considered if there is failure at the end of life. Supportive treatment should be given if possible,38 and anticipation of symptoms of distress from rigidity and fever.
After death, deactivation of the device with the patients handheld programmer is required before removing the pulse generator and battery in the case of a cremation.
What Are The Considerations For Pain Management In The Last Days Of Life In Pd
It is important to consider that pain can be a risk factor for, and associated with, many other symptoms which might be the presenting features in a patient with complex or advanced PD. These include a new or worsened confusion, hallucinations, agitation and symptoms of depression or apathy.
As well as being an underlying cause of another symptom, pain can also be the symptom of other features of PD, such as rigidity, dyskinesia, but also non-motor features, for example, depression and fatigue.
Identifying whether pain is at the root of the presenting complaint and what might be causing the pain is therefore the most important part of the initial history from the patient and the carer. Then using the clinical examination to confirm findings from the history and identify any features not already elicited such as abnormal posturing, or dystonia.
A recent review into the pathophysiology and treatment of pain in PD suggests simple analgesia with paracetamol and non-steroidal anti-inflammatory drugs but advises caution with opiate analgesia as constipation is a recognised problem in PD patients.25 The review mentions, however, the lack of evidence for many widely used analgesics specifically in PD.26
Recommended Reading: Beginning Of Parkinson’s Symptoms
Complications In Advanced Pd
While worsening of motor function and drug-induced motor complications represents a major challenge in patients with mid-stage to advanced disease, in the advanced stage of PD the most troublesome and distressful complications are usually nonmotor symptoms, including psychiatric and cognitive disorders, autonomic disturbances, and sleep disorders that significantly increase the need for supportive care. Unfortunately, these symptoms are frequently neglected in clinical practice due to limited consultation time, perception of the patient and caregivers that their symptoms are unrelated to the disease, or insufficient awareness of the clinicians, who generally focus on motor symptoms .
Proper supporting care becomes increasingly important in advanced PD. Rehabilitative and support services for patients and family become key interventions as the disease reaches its more debilitating stages and pharmacologic or surgical treatment becomes less relevant. Management of motor and nonmotor complications in advanced PD requires careful and ongoing assessment of whether symptoms are a side effect of medication or related to the progression of the disease .
Medication Issues
Also Check: On Off Phenomenon In Parkinsons Disease
Parkinsons Disease Diet And Nutrition
Maintaining Your Weight With Parkinsons Disease
Malnutrition and weight maintenance is often an issue for people with Parkinsons disease. Here are some tips to help you maintain a healthy weight.
- Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily.
- If you have an unexplained weight gain or loss , contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition.
- Avoid low-fat or low-calorie products. . Use whole milk, whole milk cheese, and yogurt.
Also Check: Is Blurred Vision A Symptom Of Parkinson’s
Planning For End Of Life
As difficult as it is to discuss, it is important for you and your loved one with PD to plan for and talk about end-of-life plans. Having your loved partake in these discussions can give them a sense of control in their life, even when it may feel like Parkinsons has taken the control.
Stages Of Parkinsons Disease
While there may be no cure, Parkinsons follows a predictable path. In the early stages, symptoms are mild and inconvenient by the end stages, symptoms are incapacitating.
- Stage One: Patients begin to experience tremors on one side of the body. One arm or leg will feel heavy, but not to the point it interferes with daily life. Symptoms may be so slight, they can be sometimes overlooked.
- Stage Two: Symptoms are clearly visible and affect both sides of the body. Patients become stooped as tremors grow more pronounced. Muscles are rigid, making it difficult to bend their trunk, arms, and legs facial muscles begin to freeze at this stage, creating an almost mask-like appearance. At this stage, however, balance is not yet impaired, so most patients continue to live independently.
- Stage Three: Balance becomes increasingly compromised, and reflexes and coordination deteriorate, elevating serious risks of falling. Muscles grow so stiff that patients can only take short, shuffling steps. Tremors become more serious, and yet most patients can still complete daily tasks, though it requires more time and greater effort.
- Stage 4: Patients can no longer live on their own. Balance is so weak that while it may be possible for them to stand, they will not be able to move without a walker. Some freeze periodically, unable to move for short periods of time.
- Stage 5: Patients cannot walk or stand without assistance and require round-the-clock care.
Also Check: Parkinson’s Disease Fun Facts
Talk With Others Who Understand
MyParkinsonsTeam is the social network for people with Parkinsons disease. On MyParkinsonsTeam, more than 89,000 members come together to ask questions, give advice, and share their stories with others who understand life with Parkinsons.
Are you or someone you care for living with Parkinsons disease? Share your experience in the comments below, or start a conversation by posting on your Activities page.
Hospice Care Late Stage Parkinsons
It is important to know your options for hospice care for late stage Parkinsons patients. Our article regarding in home health care for Parkinsons explains some of the basic facts and ideas to maintain quality of life once diagnosed. However, we offer specialized in home care from diagnosis through the final stages of the disease.
The Life of Parkinsons Crossing the bridges & facing forks in the road. Get the most out of life and adjust your lifestyle to make every day as good as possible.
Parkinsons disease is degenerative. Because the disease progresses with time there are basic stages that occur.
Recommended Reading: How To Feel Better With Parkinson’s
Study Designs And Descriptions Of Included Studies
The 42 studies were published until February 2020. The study designs were: retrospective cohort studies, prospective cohort and longitudinal studies, casecontrol studies and cross-sectional studies. Predictors of mortality included demographic and clinical markers, medical events, medication changes, disease-specific symptoms and patient and caregivers ratings of health-related quality of life. Eight studies described both predictors of mortality and causes of death.
Two Areas In Which Parkinsons Disease May Bring About Death
I. Falls
PD patients are at an increased risk of falling and bad falls can lead to death. This usually occurs as a complication of a fall that requires hospitalization, particularly if it involves surgery. While most people do not fracture their hips when they fall, some do, and hip surgery, while routine, is still major surgery. It carries the risk of infection, delirium related to pain medications and anesthesia, heart failure, pneumonia, blood clots in the legs that then go to the lungs, and general weakness from immobility. Hip fractures are probably the main cause for death for those who fall, but people can fracture other bones and require surgery. They may fracture their ribs, which leads to reduced coughing, because of the pain, and an increased risk of lung infections . It is surprisingly uncommon for Parkinsons Disease patients to die from brain injuries related to falls, but it still may occur.
II. Pneumonia
PD patients also may develop pneumonias completely unrelated to difficulties with swallowing, just like their non-PD friends and relatives.
You May Like: Parkinson’s Disease And Boxing Therapy
How Can Hospice Help Your Loved One In The Final Stages Of Parkinsons Disease
Hospice care is an extra layer of support to help you care for your loved one with end-stage Parkinsons disease. It is a special kind of care that provides comfort, support, and dignity at the end of life.
The comprehensive program focuses on physical, emotional, and spiritual quality of life through the help of a team of experts. The team includes a board-certified physician, nurse, social worker, certified home health aide , spiritual support counselor, and volunteer.
The nurse will explain the prognosis and what to expect in the upcoming days or weeks. They will also monitor pain and other symptoms. The CHHA helps with personal care needs like bathing and changing bed linens. The social worker helps address social, emotional and practical challenges including complex and inter-related needs. The spiritual support counselor helps explore spiritual concerns.
Most importantly, the hospice team will be there for you during this difficult time, bringing you peace of mind. The team is on call 24 hours a day even at 2:00 am.
Hospice is about making your final months and weeks as good as possible. This means focusing on what really matters to you.
Where Can You Get Palliative Care For Parkinsons
There are multiple providers that offer palliative care programs.
Often, agencies that offer home healthcare, hospice care, or senior living programs, also offer palliative care. Your doctor might be able to recommend a palliative care professional in your area.
You can also use this palliative care directory to find one in your area.
Also Check: Do Parkinson’s Tremors Come And Go
Pharmacologic Issues At End
As PD progresses there are fewer dopaminergic neurons in the substantia nigra as well as a progressively lower capacity to store exogenous levodopa and convert it to dopamine for storage and release in the remaining neurons. Additionally, as the dose requirements of levodopa increase, the patient’s functioning is inhibited before his next dose of medication . This usually takes place 24 hours after a levodopa dose and may appear as sensory , psychiatric or autonomic symptom, or progression of motor symptoms or dystonia . This is called end of dose wearing off. Wearing off has not been fully explored, but may be connected to pharmacokinetic changes, and shortening of striatal levodopa half-life resulting from progressive degeneration of nigrostriatal dopaminergic terminals . To treat motor symptoms it is necessary to deliver medication effectively. Patients with advanced PD often notice that protein-rich meals will diminish the effectiveness of levodopa doses . This can be alleviated by reducing protein intake during daytime and limiting protein intake at night to 40 grams . There are some strategies to Improve absorption of Levodopa include: advise patients to take levodopa before meals, on an empty stomach , advise patients to avoid protein-rich meals and bulk-forming foods , advise patients against lying down, and encourage them to move around, after ingesting a dose , and advise patients to mix levodopa, crushed into a powder, into sparkling liquid .
Management Of Social Care
When someone faces diagnosis and then the progression of a life limiting condition, many psychosocial issues will arise. These may include fears around diagnosis and an uncertainty about their future, with loss of independence and losing their role within the family. They may have anxieties about finances, about their independence and finally a fear of developing dementia.
Management of these changes both physical and mental will require early identification and an impeccable assessment with prompt referral to the appropriate team or professional.
The family and/or carers will require support from social services, carer support groups and Parkinsons support groups. Signposting to charities that provide support, education and guidance is also advisable.
Dont Miss: Symptoms Of Parkinson Disease Webmd
Also Check: Fda Approved Parkinson’s Drugs