Treatment Of Vascular Parkinsonism
The most commonly used medications for vascular Parkinsonism are L-dopa and amantadine. However, some people with Parkinsonism do not experience significant improvement with medication. Some stroke survivors who have vascular Parkinsonism can experience better muscle control with physical therapy. Often, safety measures need to be taken to avoid falls.
If you have already had recurrent strokes resulting in vascular Parkinsonism, you may be at risk of experiencing more strokes over the coming years if no action is taken to reduce your risk. Therefore, if you have been diagnosed with vascular Parkinsonism, it is particularly important to follow up with your doctor in order to prevent additional strokes. You should expect to have testing for stroke risk factors and medical treatment to reduce your risk of stroke.
There are also a number of lifestyle factors that can help reduce stroke risk, such as getting regular moderate exercise and quitting smoking if you smoke. Eating a healthy diet is also important.
Pd And Its Heterogeneity
Traditionally, sporadic PD has been recognized as a unique clinical entity, characterized by the presence of classical clinical signs, and by the typical pathology. The pathological hallmark of PD, the presence of LBs, was described by Friedrich Heinrich Lewy in his chapter of Max Lewandovskys neurology textbook, issued in Berlin in 1912. The disease-specific involvement of substantia nigra was then described by Tretiakoff in 1919, who also confirmed the existence of LBs . The fact, that LBs are formed predominantly by pathological alpha-synuclein was revealed by Spillantini and colleagues only 80 years later,. The presence of this alpha-synucleinopathy was listed as the typical pathological feature of PD, either sporadic or hereditary.
Table 1 Genes and cytogenetic locations in hereditary forms of Parkinsons disease their clinical phenotypes and neuropathological findings.
The fact that the same genetic variation may cause disparate clinical manifestations and pathological findings demonstrate a complex interplay of genetic, environment, and exposures. On the other side, there is a broad spectrum of clinical manifestations of typical Lewy-related brain pathology associated with various rare genetic abnormalities,,, where a similar combination of factors can be assumed.
What Does Lewy Body Dementia Look Like
Lewy body dementia affects a persons ability to think and process information and it can negatively impact memory and alter personality. Though it shares aspects of other forms of dementia, there are distinct hallmarks of LBD. Lewy body dementia symptoms include:
- Fluctuating attention/alertness: These shifts can last hours or go on for days. The person may stare into space, appear lethargic or drowsy, and have hard-to-understand speech, appearing a lot like delirium. At other times, the person may have much more clarity of thought.
- Visual hallucinations: Often, these are very detailed hallucinations and visions of people or animals, and they can recur.
- Movement disorders: Parkinsons-like movement issues, such as muscle rigidity, tremors, falls, or a shuffling gait or way of walking, may occur.
Read Also: What Is The Difference Between Parkinson’s And Huntington’s Disease
How Is Lewy Body Dementia Diagnosed
There are no medical tests that can diagnose Lewy body dementia with 100% accuracy. Specialists, including neurologists, geriatric psychiatrists, neuropsychologists and geriatricians, make the diagnosis of probable LBD based on the combined results of tests and patient symptoms.
Your healthcare provider will perform a thorough neurological and physical examination. You or your loved one will also complete mental status and neuropsychological tests. These tests check thinking abilities, including memory, word-finding, attention and visual-spatial skills. Your doctor will ask you and your family about your mental status and the history of your symptoms. Be sure to tell your healthcare provider of any physical, cognitive, memory, emotional, behavioral, movement, sleep or physical changes you or your loved one is having. Also, tell your healthcare provider about any of your current medications, supplements, vitamins, herbal products and frequently used over-the-counter products. These will be reviewed to see if they might be a cause of your or your loved ones symptoms.
Depending on your symptoms, your doctor may also test your blood. If your doctor needs more information, brain imaging studies may be performed.
If you have cognitive deficiency severe enough to impair daily life in the presence of any following clinical features, your doctor may suspect diagnosis of LBD:
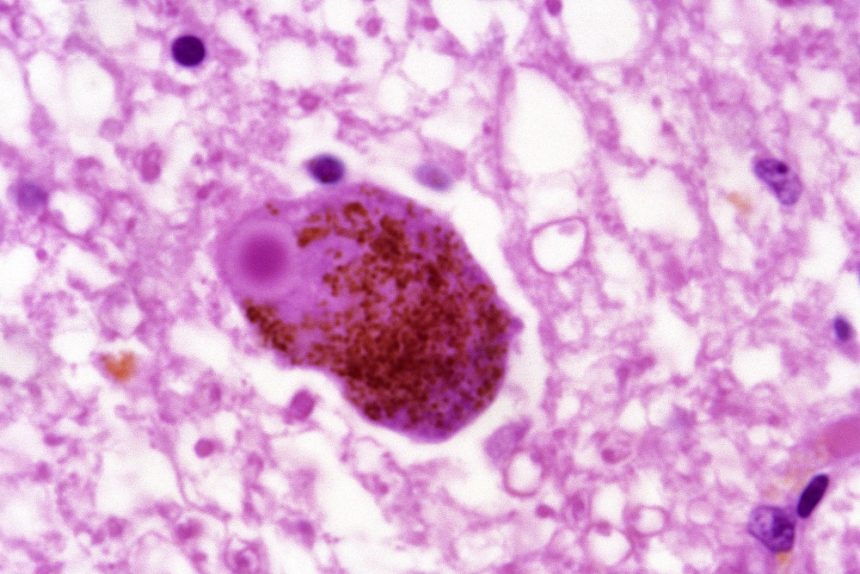
The Presence Of Lewy Bodies
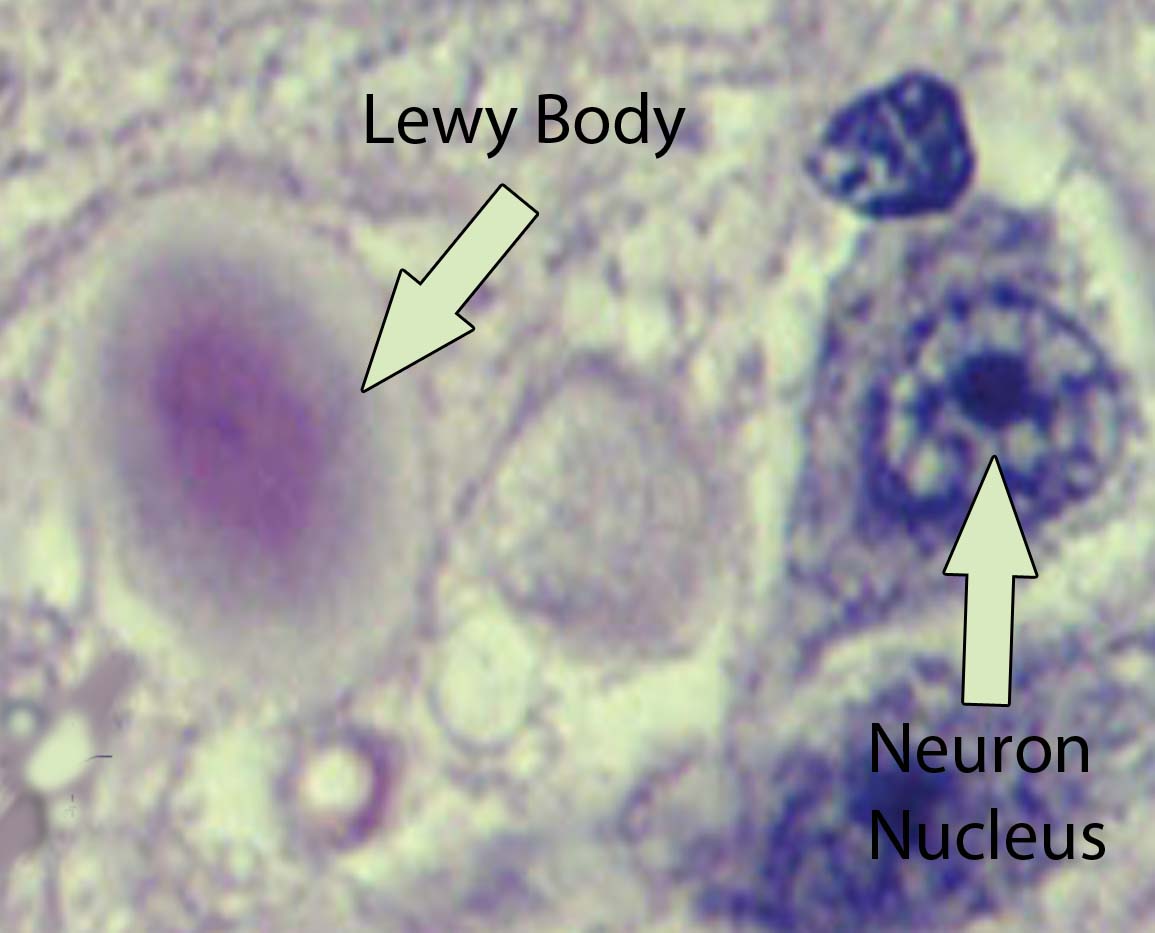
LBD is characterized by the presence of Lewy bodies in the nerve cells of the brain, meaning that LBD patients have Lewy bodies in the brain. However, Lewy bodies are also common with other conditions, such as Alzheimer’s and Parkinsons disease.2
In fact, most people with PD also have Lewy bodies in their brain. However, even if they have Lewy bodies, not all Parkinsons patients will also develop LBD.2
Don’t Miss: Ed Begley Jr Parkinson’s
The Link To Parkinsons Disease
Most people with Parkinsons disease have Lewy bodies in their brains. Its these clusters that cause some or all of the motor symptoms of Parkinsons disease, as well as memory or cognitive problems, visual hallucinations, and problems with alertness.
We rarely know if a living patient has Lewy bodies with certainty, however. Its not until an autopsy that they can be seen, says Liana Rosenthal, M.D., assistant professor of neurology at the Johns Hopkins University School of Medicine. If we see Lewy bodies in someones brain during an autopsy, thats considered a pathologic certainty of Parkinsons disease, she says.
As with Parkinsons, Lewy body dementia is associated with a depletion of certain neurotransmitters in the brain. These are:
- Dopamine: This neurotransmitter helps transmit signals that control muscle movement. When the accumulation of Lewy bodies blocks dopamines production and transmission, the result is the hallmark movement issues of Parkinsons disease.
- Acetylcholine: This neurotransmitter does its work in the parts of the brain responsible for memory, thinking and processing. When Lewy bodies build up in these areas, they interfere with acetylcholine, causing symptoms of dementia.
Dementia With Lewy Bodies Without Parkinsonism
I agree with the proposal of new criteria for the diagnosis and management of dementia with Lewy bodies . Previous criteria did not adequately differentiate DLB from Parkinson disease with dementia as outlined in the articles accompanying editorial.
Lewy body disease includes PD and DLB, thus there should be DLB without parkinsonism as well as PDD. The new criteria outlined four core clinical features: fluctuating cognition with pronounced variations in attention and alertness detailed, recurrent visual hallucinations REM sleep behavior disorder, which may precede cognitive decline and one or more spontaneous cardinal features of parkinsonism including bradykinesia, rest tremor, or rigidity. According to this criteria, a patient who has the first three clinical features but does not have parkinsonism may be diagnosed as DLB.
Braak et al. proposed that brainstem synucleinopathy progresses rostrally to affect the substantia nigra, which may cause parkinsonism. . However, these described patterns of synucleinopathy are not often observed in DLB, especially when synucleinopathy occurs in the absence of parkinsonism. Braak et al.s hypothesis would indicate that visual hallucinations are a result of occipital dysfunction. Meanwhile, attention and alertness are due to frontal dysfunction, which does not necessarily follow Braaks hypothesis. In addition, DLB patients with predominantly frontal dysfunction may not have parkinsonism.
Recommended Reading: What Are The Beginning Signs Of Parkinson’s Disease
Movement Problems And Lewy Body Dementia
Some people with LBD may not experience significant movement problems for several years. Others may have them early on. At first, movement symptoms, such as a change in handwriting, may be very mild and easily overlooked. Movement problems may include:
- Muscle rigidity or stiffness
How Is Lewy Body Disease Diagnosed
This type of dementia is diagnosed by taking a careful history of the pattern of symptoms, and by excluding other possible causes such as Vascular dementia and Alzheimers disease. A brain scan may reveal brain degeneration, but the Lewy bodies can only be identified by examination of brain tissue after death.
Lewy body disease is similar to Alzheimers disease in many ways, and in the past it has sometimes been difficult to distinguish the two. It has only recently been accepted as a disease in its own right. It can occur by itself or together with Alzheimers disease and/or Vascular dementia. It may be hard to distinguish Lewy body disease from Parkinsons disease, and some people with Parkinsons disease develop a dementia which is similar to that seen in Lewy body disease.
Read Also: Physical Therapy For Parkinson Disease Patients
Management Of Patients With Pdd
Non-pharmacological measures include education of the family about disease symptoms and appropriate care psychopharmacological medication), providing and promoting sufficient mental and physical activities. Before initiating pharmacological treatment conditions including systemic diseases, depression and adverse events of medication should be considered and managed appropriately. In particular, treatments with anticholinergics, tricyclic antidepressants, and benzodiazepines should be minimized and ideally discontinued where possible. The need for pharmacological intervention should be determined based on symptom frequency, severity, and burden.
Memantine, a partial NMDA receptor antagonist used in the treatment of AD, was tested in patients with DLB or PDD in two randomized controlled trials. In one, there was a significant difference in favor of memantine only in the global outcome scale, where patients with PDD had more benefits as compared to those with DLB.95 In the larger study the global outcome scale and behavioural scores were significantly better with memantine in the DLB group, whereas there were no significant differences in the PDD population.166 These results suggest that memantine may have mild beneficial effects in patients with Lewy body-related dementias, possibly more so in the DLB population, in global status and for behavioural symptoms.
Medications For Other Symptoms Of Dementia
People with LBD may often experience a sleep disorder called rapid eye movement sleep behavior disorder. This can sometimes be treated with sedatives like clonazepam or with melatonin . Other more severe symptoms of LBD including fluctuating levels of alertness , hallucinations, agitation, severe confusion, and delirium can be challenging to treat. Doctors must first rule out underlying causes like infection or other medications that can be triggering these symptoms. If unable to find a treatable cause, doctors may use a low dose of the atypical antipsychotic medication quetiapine to treat these symptoms. However, people with LBD must not be given typical antipsychotics or high-potency atypical antipsychotics , as people with LBD are very sensitive to these medications and may develop neuroleptic malignant syndrome if they take them. This is a life-threatening condition that causes fever, muscle stiffness, and racing heart, and can lead to heart and kidney failure. Talk with your doctor about medication options.
Read Also: Apda Parkinson’s Disease Handbook
Acknowledgments And Conflict Of Interest Disclosure
Data in this manuscript are original and were generated for the purpose of this study. Photomicrographs were taken from tissue provided by the Newcastle Brain Tissue Resource, which is funded in part by a grant from the UK Medical Research Council , by Brains for Dementia research, a joint venture between Alzheimers Society and Alzheimers Research UK and by the NIHR Newcastle Biomedical Research Centre awarded to the Newcastle upon Tyne Hospitals NHS Foundation Trust and Newcastle University. DLB research is supported by NIHR Newcastle Biomedical Research Centre in Ageing and Long-Term Conditions. LW is funded by the Alzheimers Society. The authors have no conflicts of interest to declare.
You May Like: Motor And Non Motor Symptoms Of Parkinsons Disease
What Causes Parkinsons Disease
The most prominent signs and symptoms of Parkinsons disease occur when nerve cells in the basal ganglia, an area of the brain that controls movement, become impaired and/or die. Normally, these nerve cells, or neurons, produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems associated with the disease. Scientists still do not know what causes the neurons to die.
People with Parkinsons disease also lose the nerve endings that produce norepinephrine, the main chemical messenger of the sympathetic nervous system, which controls many functions of the body, such as heart rate and blood pressure. The loss of norepinephrine might help explain some of the non-movement features of Parkinsons, such as fatigue, irregular blood pressure, decreased movement of food through the digestive tract, and sudden drop in blood pressure when a person stands up from a sitting or lying position.
Many brain cells of people with Parkinsons disease contain Lewy bodies, unusual clumps of the protein alpha-synuclein. Scientists are trying to better understand the normal and abnormal functions of alpha-synuclein and its relationship to genetic mutations that impact Parkinsons andLewy body dementia.
Read Also: What Is The Va Disability Rating For Parkinson’s Disease
What Other Things Help
There are various ways to help a person with DLB. Speech therapy may help improve communication between people with DLB and others. Physical therapy may help strengthen and stretch stiff muscles and help to prevent falls.
Research has shown that physical exercise helps to enhance brain health and improves mood and general fitness. A balanced diet, enough sleep, and limited alcohol intake are other important ways to promote good brain health. Other illnesses that affect the brain, such as diabetes, high blood pressure, and high cholesterol, should also be treated if present.
Anxiety And Parkinsons Disease
Anxiety is another common mood disorder of PD and is characterized by excessive nervousness or worry over several months. Patients with generalized anxiety disorder may experience symptoms such as:
- Restlessness, feeling wound-up or on edge
- Difficulty controlling the worry
- Sleep problems, such as difficulty falling or staying asleep, or restless or unsatisfying sleep1,3
Anxiety is not linked with disease of PD. It may develop before or after a PD diagnosis. It is often experienced along with depression in people with PD, as the disease process of PD changes the chemistry of the brain. Treatment for anxiety may include anti-anxiety medications, psychological counseling, exercise, relaxation techniques, and/or meditation.1
You May Like: Parkinson’s Disease In Older Adults
Diagnosis Of Parkinsons Disease
There are currently no blood or laboratory tests to diagnose non-genetic cases of Parkinsons. Doctors usually diagnose the disease by taking a persons medical history and performing a neurological examination. If symptoms improve after starting to take medication, its another indicator that the person has Parkinsons.
A number of disorders can cause symptoms similar to those of Parkinsons disease. People with Parkinsons-like symptoms that result from other causes, such as multiple system atrophy and dementia with Lewy bodies, are sometimes said to have parkinsonism. While these disorders initially may be misdiagnosed as Parkinsons, certain medical tests, as well as response to drug treatment, may help to better evaluate the cause. Many other diseases have similar features but require different treatments, so it is important to get an accurate diagnosis as soon as possible.
Treatments For Parkinsons Disease Dementia And Dementia With Lewy Bodies
Treatments for DLB are similar to PDD and are aimed at symptom control. The motor symptoms of slowness, stiffness and walking difficulties can be treated with Levodopa. However, Levodopa can cause or exacerbate hallucinations, making it difficult to use it as a treatment for patients who have or are at risk of having hallucinations. Sometimes, clinicians will need to treat the hallucinations more aggressively in order for a patient to tolerate Levodopa given to help the motor symptoms. On the flipside, anti-psychotic medications to control hallucinations can worsen motor symptoms, so treating all the symptoms of LBD simultaneously can be a tricky balancing act.
Don’t Miss: Do Parkinson’s Tremors Come And Go
What Are Pd Dementia Safety Concerns
Safety issues should be considered and monitored from the time of diagnosis. As PDD progresses, ensure that your loved one is not left alone.
- Evaluate driving privileges before safety is a concern. Your doctor can make a driving evaluation referral.
- Work out legal and financial issues and safeguard finances. People with dementia are at greater risk of falling victim to scams and fraud.
- Minimize prescription risks. Confirm with the doctor the medication names and doses of the person with PD. If the person is in dementias early stages and capable, fill up their weekly pill box together and monitor use.
- Medical alert systems can be critical in case your loved one falls or wanders outside of the home. Many types of systems are available, from bracelets and pendants to smart watches with fall detection and one-button connections to 911.
- Evaluate gun safety. If your loved one owns a firearm or has one in the home, consider speaking with their doctor about the subject and taking appropriate safety precautions.
Recommended Reading: Apps For Parkinsons Patients
Approximate Lewy Body Dementia Phases Symptoms And Considerations
Lewy Body Dementia Stage 1 Possibilities
Most caregivers are concerned/worried that something is not right. Symptoms from later stages can also appear this early on the continuum. At the end of this phase, cognitive impairment is difficult to deny.
Symptoms and subtle changes may include:
- Increased daytime sleep: two-plus hours
- Hallucinations
- May accuse spouse of infidelity
Lewy Body Dementia Stage 2 Possibilities
Caregivers consult with an elder law attorney by this point: at very least have a Power of Attorney and Medical Power of Attorney document on the patient. Protect assets: family, friends, caregivers may be able to take financial advantage of LO. Caregivers need to familiarize themselves with all finances and assets to possibly consult with a financial advisor.
Symptoms are usually clearer by this point:
Increased difficulty with:
Lewy Body Dementia Stage 3 Possibilities
Lewy Body Dementia Stage 4 Possibilities
Lewy Body Dementia Stage 5 Possibilities
Strength to all!
You May Like: Nonprofit Organizations For Parkinson’s Disease
Diagnostic Criteria For Dementia With Lewy Bodies
The consensus criteria for a clinical diagnosis of DLB reflect the clinical features described previously in this article . Progressive cognitive decline to dementia is required, often involving attention, executive function, and visual-spatial skills. The core features of these criteria include the following: recurrent visual hallucinations that are well formed and detailed fluctuations in attention and alertness and parkinsonian motor signs. Supportive features, also common in PD, include the presence of REM sleep behavior disorder, severe neuroleptic sensitivity, or low DAT uptake in the basal ganglia on SPECT or PET. A diagnosis of clinically probable DLB requires at least two out of three of the core features to be present or one core feature and one supportive feature. A diagnosis of clinically possible DLB requires only one of the three core features to be present.
Recommended Reading: Best Time To Take Parkinsons Medication