Getting Closer To A Definitive Biomarker For Parkinsons Disease
Parkinsons disease is a devastating, incurable, progressive and degenerative neurological disease that affects movement. There are no biomarkers available and it is diagnosed by symptomology alone. Unfortunately, the symptoms can be similar to many other neurological diseases. This often leads to misdiagnoses resulting in delayed treatment. Currently, definitive diagnosis can only be made at autopsy. A new skin test has been developed that may be able to diagnose Parkinsons in living patients and at an earlier time in the disease.
The development and use of biomarkers comes with numerous ethical and legal concerns. How do we determine disease and disability? Could biomarkers exacerbate the disparities between diseases that have objective findings and those that do not, making it more difficult for physicians to recognize a condition even in the absence of a marker? Additionally, we should be concerned about who has access to biomarker information and how that information might be misused.
Further studies will be needed to determine if a-synuclein seeding activity can be detected in skin before clinical signs develop in Parkinsons disease. This possibility is supported by findings reported by Wang et al. that skin prion activity is detectable not only in all patients with Creutzfeldt-Jakob disease but also far in advance of neuronal damage and clinical signs of prion disease in rodents.
Response To Parkinsons Drugs
After examining you, and depending on the severity of your symptoms, your specialist may suggest you take medication for Parkinsons. If your symptoms improve after taking Parkinsons medication for a few weeks or months, your specialist may confirm a Parkinsons diagnosis. However, some people with other forms of parkinsonism will also respond well to these drugs.
Your specialist may suggest you have a scan to help make a diagnosis. However, scans alone cant make a definite diagnosis of Parkinsons, so they are not commonly used.
Mri In Parkinson’s Testing
One of the more common tests done during a neurologic workup is an MRI scan and one may think that in the investigation of a disease that affects the brain such as Parkinsons, this imaging test would be a necessity. In the context of Parkinsons disease, however, an MRI is not particularly helpful. It looks at the structure of the brain which, for all intents and purposes, appears normal in this disease. An MRI may, however, be indicated when symptoms appear in younger people or if the clinical picture or the progression of symptoms is not typical for Parkinsons. In these situations, MRI can be used to rule out other disorders such as stroke, tumors, hydrocephalus , and Wilsons Disease .
Don’t Miss: Sam Waterston Tremor
Ological Limitations Of The Diagnostic Studies
When interpreting the literature about diagnosis, the following methodological issues should be considered:
- lack of long-term prospective clinical and pathological as a reference standard
- lack of operational definitions such as defining specialists or clinical diagnostic criteria
- unclear whether investigators were blinded to initial diagnosis
- sample sizes necessarily limited by the number of cases available with neuropathological outcomes
- trial age groups are often young as studies were performed by neurologists who see a younger population of people with PD
- most studies included people with established disease lasting some years
- varying geographical locations
- some studies are in specialised units and may not reflect the diagnostic accuracy of other units in the UK
- exclusion of some studies using magnetic resonance volumetry and magnetic resonance spectroscopy as they lacked appropriate population, intervention and outcome criteria
- lack of statistical details of diagnostic accuracy such as sensitivity, specificity and positive predictive values
- lack of economic evaluations of SPECT.
From Evidence To Recommendation
The pathological studies emphasise the need for particular care in making a clinical diagnosis of . There is limited evidence to suggest that the UK Brain Bank Criteria have adequate sensitivity and specificity in comparison with post-mortem findings. The accuracy of diagnosis using the Brain Bank criteria increases as the condition progresses.
The availability of brain tissue has fostered much valuable research in recent years and should be encouraged in the future. Diagnostic information derived from post-mortem examination can also be of value to the families of individual patients.
RECOMMENDATIONS
- R9.
-
should be diagnosed clinically and based on the UK Parkinsons Disease Society Brain Bank Criteria.
- R10.
-
Clinicians should be encouraged to discuss with patients the possibility of tissue donation to a brain bank for purposes of diagnostic confirmation and research.
You May Like: Does Sam Waterston Have Parkinsons
Tom Thought That Because Some Pink Tablets Relieved His Symptoms This Meant He Was Ok He Didn’t
I first suspected there was something wrong when I was travelling and I was writing a postcard to a friend of mine in, in Australia whose name is Anthony Diecopolis. And, and I got to the Anthony Diec and I couldnt finish the opolis. And its very strange my hand had sort of gone into a sort of spasm and it just wouldnt, wouldnt finish writing the, the, the word. And so thats a bit strange.
And so I went when, when I got I, I went to the doctor and said, What on earths going on? And I had since then Id also developed this slight tremor in my right hand. He said, Well its probably, Essential Tremor or trapped nerve or something like that. And anyway, then it got a bit worse and then I was, I was recommended to go to a neurologist. And the neurologist had a look at me and gave me some pills. And he said, Come back and tell me if these work.
This is about, about sort of, nine months after my, my not being able to finish the, the postcard. And, and he said, Take these pills. And the pills worked. Magically the tremors stopped and I thought this is wonderful. And so I went back to the neurologist and I said, Yes everythings fine now. The pills have, the pills have worked. And far from looking happy about this he looked rather, rather grave and he said, I think youd better go to another neurologist.
Enabling Early Diagnosis Of Life
Every hour, someone in the UK is told they have Parkinsonâs disease â a progressive neurological condition with no definitive diagnostic test and no cure. At The University of Manchester we are tackling the development of a non-invasive diagnostic test that may have the ability to diagnose early Parkinsonâs â possibly even before physical symptoms are displayed.
You May Like: Parkinson Silverware
Currently There Is No Cure And No Definitive Test For Parkinson’s Diagnosis Can Take Years
A simple skin-swab test could be used to help diagnose Parkinsons disease, a degenerative brain condition if UK scientists are to go by. As per a latest study, it is possible to identify Parkinsons based on the compounds found on ones skin. The University of Manchester scientists have developed a technique that quickly detects tell-tale compounds in sebum the oily substance that protects the skin and identifies changes in people with the disease.
Currently, there is no cure and no definitive test for Parkinsons. Also, diagnosis can take years.
Sebum, which is rich in lipid-like molecules, is one of the lesser-studied biological fluids in the diagnosis of the condition. People with Parkinsons tend to produce more sebum than normal which is called seborrhoea.
Researchers discovered this after a woman amazed doctors with her ability to detect Parkinsons through smell. Retired nurse Joy Milne, 68, from Perth, noticed the musky smell on her husband, Les, years before his Parkinsons diagnosis.
The research team used a mass-spectrometry machine to detect the compounds, and now has data from 500 people, showing the skin test can correctly distinguish those with Parkinsons more than eight out of every 10 times.
The research, funded by charities Parkinsons UK and Michael J Fox Foundation as well as The University of Manchester Innovation Factory, analysed the samples taken from the peoples upper backs.
Early Signs Of Parkinson’s
Early physical signs include the common motor symptoms: tremor, muscle rigidity and slowness. They may also include the following:
- Symptoms starting on one side of the body
- Change in facial expression
- Failure to swing one arm when walking
- Stooped posture
- Loss of sense of smell
- Depression or anxiety
Some of these symptoms are quite common and by no means exclusive to Parkinsons, so if you have some of them, it does not mean you have Parkinsons.
Also Check: Pfnca Wellness Programs
Referral To A Specialist
If your GP suspects Parkinson’s disease, you’ll be referred to a specialist.
This will usually be:
- a neurologist, a specialist in conditions affecting the brain and nervous system
- a geriatrician, a specialist in problems affecting elderly people
The specialist will most likely ask you to perform a number of physical exercises so they can assess whether you have any problems with movement.
A diagnosis of Parkinson’s disease is likely if you have at least 2 of the 3 following symptoms:
- shaking or tremor in a part of your body that usually only occurs at rest
- slowness of movement
- muscle stiffness
If your symptoms improve after taking a medication called levodopa, it’s more likely you have Parkinson’s disease.
Special brain scans, such as a single photon emission computed tomography scan, may also be carried out in some cases to try to rule out other causes of your symptoms.
How The Florey Is Making A Difference
The Institute has a number of research projects in its laboratories underway, for example:
- Scientists looking for the cause of Parkinsons disease continue to search for possible factors that may trigger the disorder, and study genetic factors to determine how genes could play a role
- Other scientists are working on developing new protective drugs that can delay, prevent, or reverse the disease
- Trialling improved methods of diagnosis and treatment monitoring
Don’t Miss: Yopd Life Expectancy
A Step Closer To A Skin Swab Test For Parkinson’s
Complete the form below and we will email you a PDF version of“A Step Closer to a Skin Swab Test for Parkinson’s “
First Name*Would you like to receive further email communication from Technology Networks?Technology Networks Ltd. needs the contact information you provide to us to contact you about our products and services. You may unsubscribe from these communications at any time. For information on how to unsubscribe, as well as our privacy practices and commitment to protecting your privacy, check out our Privacy Policy
Tests To Rule Out Other Conditions

Blood tests can help rule out other possible causes of the symptoms, such as abnormal thyroid hormone levels or liver damage.
An MRI or CT scan can check for signs of a stroke or brain tumor, which may cause similar symptoms.
Hydrocephalus due to atrophy can occur with some types of dementia and would be visible with one of these imaging tests. If the person has neurologic symptoms but a normal scan result, Parkinsons disease may be present.
The doctor a lumbar puncture to rule out inflammation or a brain infection.
Don’t Miss: Cleveland Clinic Parkinson’s Bicycle Study 2017
Global Problem: Lack Of Diagnosis Negates Treatment Impact
Parkinsons disease affects 127,000 people in the UK and 7.5 million worldwide, leaving many patients struggling to walk, speak and sleep.
The lack of a definitive test for Parkinsons means that, typically, too many neurons in the brain are lost irretrievably by the time of diagnosis, making treatment difficult and a cure impossible.
Is Early Diagnosis Possible
Experts are becoming more aware of symptoms of Parkinsons that precede physical manifestations. Clues to the disease that sometimes show up before motor symptoms and before a formal diagnosis are called prodromal symptoms. These include the loss of sense of smell, a sleep disturbance called REM behavior disorder, ongoing constipation thats not otherwise explained and mood disorders, such as anxiety and depression.
Research into these and other early symptoms holds promise for even more sensitive testing and diagnosis.
For example, biomarker research is trying to answer the question of who gets Parkinsons disease. Researchers hope that once doctors can predict that a person with very early symptoms will eventually get Parkinsons disease, those patients can be appropriately treated. At the very least, these advances could greatly delay progression.
Parkinson’s Disease and Movement Disorders Center
Our center provides compassionate and timely treatment to patients with movement disorders, such as dystonia, ataxia, essential tremor and similar conditions. But our mission goes beyond patient care excellence. By offering educational events and support groups, we empower patients and caregivers to become better partners in their health.
Read Also: Judy Woodruff Parkinson’s
What Is Parkinsons Plus Syndrome
Parkinsons plus syndrome is the name for a group of neurological conditions that are very similar to Parkinsons disease. Because these conditions cause symptoms that are very similar to Parkinsons, they are often incorrectly diagnosed. However, these conditions can even be treated using many of the same medications and therapies as Parkinsons.
Conditions that are considered Parkinsons plus syndromes include:
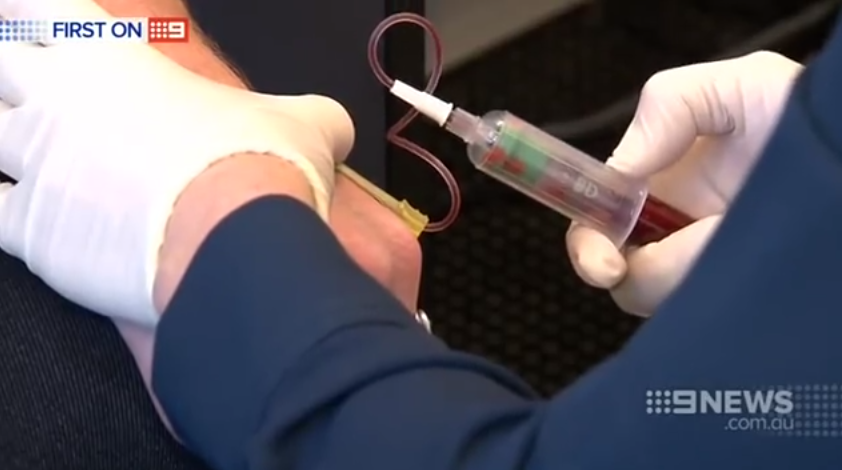
Blood Test May Help Distinguish Parkinsons From Similar Diseases
Researchers have found that people with Parkinsons disease have lower levels of a certain protein in their blood than people with similar diseases. The results suggest that testing for the protein might help doctors to accurately differentiate between PD and similar diseases early on. The study appears in the February 8 online edition of Neurology.
Because there are no definitive diagnostic tests for Parkinson’s, the diagnosis can be unclear especially early on in the disease. When diagnosis is uncertain, some people may be diagnosed with parkinsonism,” which refers to a category of diseases, including Parkinson’s, that cause slowness of movement, stiffness and rest tremor. Other diseases in the category include multiple system atrophy , progressive supranuclear palsy and corticobasal degeneration .
Earlier studies found that a spinal fluid test may help distinguish PD from these other diseases, but this test is difficult to do during a routine visit to the doctor.
Results
- Blood levels of NfL protein were generally lower in people with PD and in healthy individuals than in people with other Parkinsonian disorders.
- This result held both for those recently diagnosed and those who had been living with their disease for four to six years.
- The test for NfL could not distinguish between MSA, PSP and CBD.
What Does It Mean?
References
Hansson O, Janelidze S, Hall S, et al. . Blood-Based NfL: A Biomarker for Differential Diagnosis of Parkinsonian Disorder. Neurology 88: 1-8
You May Like: What Foods Should Be Avoided When Taking Levodopa
Looking For Signs Of Parkinsons
Your specialist will examine you to look for common signs of Parkinsons. You may be asked to:
- write or draw to see if your writing is small or gradually fades
- walk to see whether theres a reduction in the natural swing of your arm or in your stride length and speed
- speak to see if your voice is soft or lacks volume
The specialist will also look at and ask you about your:
- face to see if there is a masked look or if you have difficulty with facial expressions
- limbs to see if you have a tremor, any stiffness or slowness of movement
As well as examining you for any of the typical signs of Parkinsons, the specialist will also look for signs that may suggest a different diagnosis.
It may be helpful to take someone with you for support when seeing a specialist. Taking a list of questions you want to ask can also be useful so you dont forget to mention something you want to know about. If a healthcare professional says something you dont understand, dont be afraid to ask them to explain what they mean.
What Causes It
Researchers arent sure what causes Parkinsons or Parkinsons plus syndrome. There might be some genetic or environmental risk factors that can increase the likelihood of developing Parkinsons plus syndrome. For example, some scientists theorize that exposure to toxins could cause your risk, but more research needs to be done to prove this link.
Although the underlying cause isnt known, we do know what changes to your body can cause each Parkinsons plus syndrome:
- PSP. When you have PSP, a buildup of protein in your brain cells causes them to deteriorate. Your condition will progress as this continues.
- MSA. As with PSP, proteins accumulate in the cells of your brain that control your central nervous system and other vital functions.
- CBGD. A protein called tau builds up in your brain cells when you have CBGD. This buildup causes the symptoms of CBGD.
- LBD. Protein clusters called Lewy bodies grow in your brain when you have LBD. Over time, the Lewy bodies cause changes to your brain that impact your ability to function.
Also Check: Prayers For Parkinson’s Disease
Who Can Get It
While anyone can develop Parkinsons disease, age is the greatest factor in receiving a diagnosis. The average age of developing this disease is 60, and men are more likely to receive a diagnosis than women. Having a close relative, like a parent or sibling, who has Parkinsons disease doubles your risk factor.
Dementia With Lewy Bodies
DLB is characterized by the early development of cognitive symptoms and psychotic symptoms such as hallucinations. Parkinsonian motor symptoms occur later in the progression of the disease. After Alzheimers, DLB is the leading cause of dementia. DLB typically does not occur before the age of 65. In DLB, alpha synuclein protein builds up throughout the cerebral cortex of the brain, forming collections called Lewy bodies.
DLB is often misdiagnosed as Alzheimers. Symptoms of DLB may respond to medications for Parkinsons or Alzheimers, but certain Alzheimers medications carry high risk for dangerous side effects if given to those with DLB. DLB and Parkinsons disease dementia have many features in common, and together they are known as the Lewy body dementias.
Recommended Reading: Adaptive Silverware For Parkinson’s