One Touch Stockings Of Cambridge
What does this task measure?OTS evaluates executive function, spatial planning and working memory based upon the Tower of Hanoi test.What does this task involve?The participant is shown two displays of coloured balls held in stockings suspended from a beam. There is a row of numbered boxes along the bottom of the screen. The participant is asked to solve problems by working out how they would move the balls in the bottom display in order to make them match the arrangements of the ball sin the top display. After some training and practice problems, the participant is asked to work out in their head how many moves the solutions to these problems require, and then touch the appropriate box at the bottom of the screen to indicate their response.Why use this task?Performance on the OTS task by Parkinsons patients is associated with the COMT genotype in the early stages of the disease8. In this sense, the COMT gene is responsible for levels of hormones and communication of neurotransmitters. When the COMT gene is no longer fully functioning, dopamine levels may drop and serotonin may rise. Following this, communication between neurotransmitters can fail. This can lead to an inability to spatially plan as communication within the frontal lobe, responsible for planning, solving and organising, has failed.
What Tests Diagnose Parkinson’s Disease
There currently are no tests that can definitively diagnose Parkinsons Disease. A diagnosis is based on the clinical findings of your physician in combination with your report on the symptoms you are experiencing.
In situations where an older person presents with the typical features of Parkinsons and they are responsive to dopamine replacement therapy, there is unlikely to be any benefit to further investigation or imaging.
How Do I Take Care Of Myself
If you have Parkinsons disease, the best thing you can do is follow the guidance of your healthcare provider on how to take care of yourself.
- Take your medication as prescribed. Taking your medications can make a huge difference in the symptoms of Parkinson’s disease. You should take your medications as prescribed and talk to your provider if you notice side effects or start to feel like your medications aren’t as effective.
- See your provider as recommended. Your healthcare provider will set up a schedule for you to see them. These visits are especially important to help with managing your conditions and finding the right medications and dosages.
- Dont ignore or avoid symptoms. Parkinsons disease can cause a wide range of symptoms, many of which are treatable by treating the condition or the symptoms themselves. Treatment can make a major difference in keeping symptoms from having worse effects.
Don’t Miss: Community Resources For Parkinson’s Disease
Understanding The Progression Of Parkinsons Disease
- The Parkinsons disease staging system is a helpful tool to track movement-related symptoms and to monitor disease progression.
- People with advanced Parkinsons are typically in stages 4 or 5, at which point symptoms have become severe and limiting.
- Effective treatment options are available for people with advanced Parkinsons.
Parkinsons disease is a neurological movement disorder that changes and often progresses the longer someone has it. There are several ways to assess and monitor disease progression of Parkinsons. One of those ways is to understand the five stages of Parkinsons.
It is important to note that everyone with Parkinsons experiences their own unique symptoms and disease progression. No two people will have the same Parkinsons journey. A person can develop advanced Parkinsons disease after many years, or they may experience a faster disease progression.
Is Early Diagnosis Possible

Experts are becoming more aware of symptoms of Parkinsons that precede physical manifestations. Clues to the disease that sometimes show up before motor symptoms and before a formal diagnosis are called prodromal symptoms. These include the loss of sense of smell, a sleep disturbance called REM behavior disorder, ongoing constipation thats not otherwise explained and mood disorders, such as anxiety and depression.
Research into these and other early symptoms holds promise for even more sensitive testing and diagnosis.
For example, biomarker research is trying to answer the question of who gets Parkinsons disease. Researchers hope that once doctors can predict that a person with very early symptoms will eventually get Parkinsons disease, those patients can be appropriately treated. At the very least, these advances could greatly delay progression.
You May Like: Big And Loud Parkinsons Exercises
Physical Examination And Tests
A trip to the neurologists office often includes what seems like dozens of questions, along with multiple tests.
There currently are no diagnostic blood tests for Parkinson’s disease, but your healthcare provider may do some routine blood and urine tests to assess your overall health. Your blood pressure will be taken sitting and standing to look for orthostatic hypotension.
A movement disorder specialist will do a variety of physical tests to assess you as well.
Physical Exam For Parkinson’s
During a physical exam, the doctor examines the patients body for signs of disease. The doctor will include a visual inspection , palpation , ascultation , and percussion . The physical exam for PD is generally conducted by a neurologist and may also be called a neurological exam. It is recommended that a patient see a neurologist with special training in movement disorders as these specialists have the most knowledge about the symptoms and medications. During a neurological exam, the patient may be asked to sit, stand, walk, and extend their arms as the doctor evaluates balance and coordination. Most neurologists recommend a spouse or caregiver attend the exam with the patient to help with answering important questions.1,2
Don’t Miss: Does Richard Branson Have Parkinsons
Discuss With Your Physician
Non-motor symptoms can sometimes be difficult to recognize. Therefore, it is important to make your doctor aware of them.
One useful resource is the PD NMS Questionnaire. You can use this to record your symptoms and discuss them with your doctor.
Dr. Ron Postuma, whose research was funded by donations to the Parkinson Canada Research Program, has also developed tools to help people with Parkinsons and their physicians identify and manage non-motor symptoms.
Determining Diagnosis Through Response To Parkinsons Medication
If a persons symptoms and neurologic examination are only suggestive of Parkinsons disease or if the diagnosis is otherwise in doubt, the physician may, nevertheless, prescribe a medication intended for Parkinsons disease to provide additional information. In the case of idiopathic Parkinsons, there is typically a positive, predictable response to Parkinsons disease medication in the case of some related Parkinsonian syndromes, the response to medication may not be particularly robust, or it may be absent entirely.
Unfortunately, there are no standard biological tests for the disease, such as a blood test. However, researchers are actively trying to find biomarkers in blood and other bodily fluids that could help confirm the diagnosis.
Recommended Reading: Bike Therapy For Parkinson’s Disease
What Can I Expect If I Have This Condition
Parkinsons disease is a degenerative condition, meaning the effects on your brain get worse over time. However, this condition usually takes time to get worse. Most people have a normal life span with this condition.
You’ll need little to no help in the earlier stages and can keep living independently. As the effects worsen, youll need medication to limit how the symptoms affect you. Most medications, especially levodopa, are moderately or even very effective once your provider finds the minimum dose you need to treat your symptoms.
Most of the effects and symptoms are manageable with treatment, but the treatments become less effective and more complicated over time. Living independently will also become more and more difficult as the disease worsens.
How long does Parkinsons disease last?
Parkinsons disease isnt curable, which means its a permanent, life-long condition.
Whats the outlook for Parkinsons disease?
Parkinson’s disease isn’t fatal, but the symptoms and effects are often contributing factors to death. The average life expectancy for Parkinson’s disease in 1967 was a little under 10 years. Since then, the average life expectancy has increased by about 55%, rising to more than 14.5 years. That, combined with the fact that Parkinson’s diagnosis is much more likely after age 60, means this condition doesn’t often affect your life expectancy by more than a few years .
Depression May Be An Early Symptom Of Parkinsons
Depression is one of the most common, and most disabling, non-motor symptoms of Parkinsons disease. As many as 50 per cent of people with Parkinsons experience the symptoms of clinical depression at some stage of the disease. Some people experience depression up to a decade or more before experiencing any motor symptoms of Parkinsons.
Clinical depression and anxiety are underdiagnosed symptoms of Parkinsons. Researchers believe that depression and anxiety in Parkinsons disease may be due to chemical and physical changes in the area of the brain that affect mood as well as movement. These changes are caused by the disease itself.
Here are some suggestions to help identify depression in Parkinsons:
- Mention changes in mood to your physician if they do not ask you about these conditions.
- Complete our Geriatric Depression Scale-15 to record your feelings so you can discuss symptoms with your doctor. Download the answer key and compare your responses.
- delusions and impulse control disorders
Read Also: Parkinson’s Device That Stops Tremors
Ruling Out Other Conditions
The symptoms of PD are similar to symptoms caused by other conditions, and an important part of the diagnosis process is excluding other diseases that may be the source of the patients symptoms. Other diseases that could cause similar symptoms include stroke, hydrocephalus, or other neurodegenerative disorders. Some medications can also cause Parkinsons like symptoms, and the doctor will assess these. Good responsiveness to levodopa for the motor symptoms is indicative of PD. However, many clinical trials need patients newly diagnosed with PD that have never taken levodopa. So, it may be worthwhile discussing participation in clinical trials with the doctor first.1
How Parkinsons Disease Is Diagnosed
Parkinsons disease is usually diagnosed clinically, meaning that a physician looks for the presence or absence of the possible symptoms of Parkinsons disease by interviewing the patient and performing a detailed neurologic examination.
While there is presently no definitive test for Parkinsons, it can often be identified by a general neurologist, who is trained to diagnose and treat neurologic disorders. To avoid misdiagnosis, consultation with a movement disorder specialist is recommended. A movement disorder specialist is a physician who has undergone additional, subspecialty training in the diagnosis and treatment of movement disorders, such as Parkinsons, after training in general neurology.
What to expect during your visit with a physician
Typically, a trained physician will only consider the diagnosis of Parkinsons disease if the person being examined has at least two of the core motor symptoms of Parkinsons, including tremor, the characteristic bradykinesia , or rigidity. At the end of your visit, the physician should discuss with you why you may or may not have Parkinsons disease and the level of certainty about the diagnosis. This determination is based on your medical history and examination at this visit.
Brain imaging and other tools to aid diagnosis of Parkinsons
Also Check: Is Dystonia A Form Of Parkinson’s
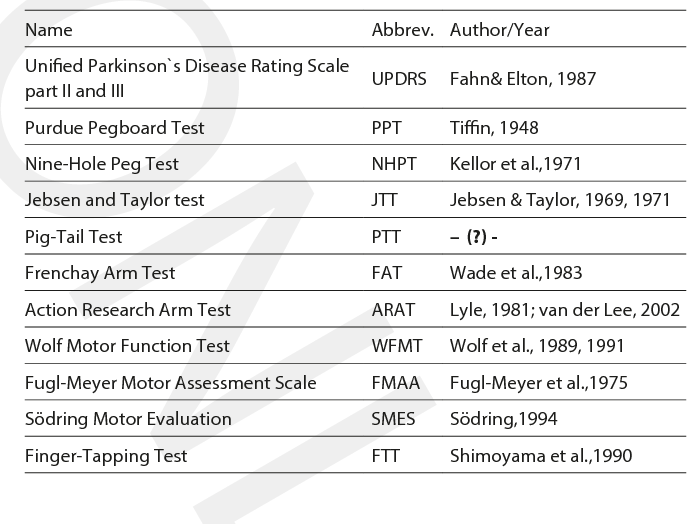
Use Of Rating Scales For Screening For Parkinsonism
Although the UPDRS was not developed for diagnostic use, it has been applied for mass screenings for parkinsonism . Note the use of the term parkinsonism rather than PD. Parkinsonism refers to the clinical manifestations, but makes no specific inference regarding the pathophysiology or etiology of the condition. Thus, these types of mass screenings attempt to identify the more general condition parkinsonism that may include drug-induced parkinsonism, multisystems atrophy, or progressive supranuclear palsy, as well as Parkinson disease. Furthermore, ratings on the UPDRS can reflect nonparkinsonian conditions. A hemiparesis due to a stroke may enhance or produce bradykinesia in a limb that is not distinguished from parkinsonism on the rating scale. Nevertheless, there have been several attempts to use modified forms of UPDRS subscale 3 as a screening for parkinsonism . In fact, mass screenings can include blinded videotape-based ratings that exclude assessment of rigidity, since that must be done in person. The key feature is to determine what value of UPDRS subscale 3 indicates parkinsonism. A score of nine on subscale 3 has been demonstrated to have 100% sensitivity and 81% specificity in identification of parkinsonism in a large video-based screening of more than 2000 people with welding exposure, an environmental factor under investigation for its potential relationship to the development of parkinsonism.
Further Testing In Parkinson’s
In other situations, where perhaps the diagnosis is not as clear, younger individuals are affected, or there are atypical symptoms such as tremor affecting both hands or perhaps no tremor at all, further testing may help. For example, imaging can play a role in differentiating between essential tremor and Parkinsons. It can also be important to confirm what is initially a clinical diagnosis of Parkinsons prior to an invasive treatment procedure such as surgical DBS
Read Also: Neuropathy And Parkinson’s Disease
Assessment Of Symptomatic Effects
Ratings such as the UPDRS, either in its entirety or with motor subscale 3 alone, have been used to assess symptomatic benefit from therapeutic interventions. A critical factor in longitudinal studies is to try to control the variables in the temporal responses to individual doses of medication. Ideally, repeated ratings should be done at the same time of day, at the same time after the last dose of medication, and by the same rater. Other factors also may influence these ratings, such as diet, fatigue, or other potential stresses that may alter PD manifestations.
Why We Need A Laboratory Test For Parkinsons Disease
It is known that the cell loss of PD begins decades before motor symptoms develop and that often certain non-motor symptoms appear first. Therefore, scientists and clinicians are searching for ways to diagnose PD earlier. Diagnosing the disease earlier may allow people with PD to take measures to improve their health earlier, and may be an essential element to developing a neuroprotective medication, a drug that slows down or reverses the nerve damage of PD. It is possible that such a medication would only work at the earliest stages of the disease.
In addition, there are a number of neurologic syndromes that share features of PD. While neurologists are trained to differentiate between these syndromes, researchers are looking for ways to distinguish between different diagnostic possibilities more accurately.
Theres no consensus for a Parkinsons biomarker, making lab tests difficult.
The major obstacle to earlier and more accurate diagnosis of PD, is the current lack of an agreed-upon, simple biomarker for PD. A biomarker is a measurable characteristic in the body that indicates that disease is present. A biomarker can be a lab test, an imaging test, or a clinical test. Common biomarkers include hemoglobin A1c for diabetes, or ejection fraction for heart failure. You can read more about the development of a biomarker for PD in a prior blog.
Recommended Reading: Foods To Help With Parkinson’s Disease
What Tests Will Be Done To Diagnose This Condition
When healthcare providers suspect Parkinsons disease or need to rule out other conditions, various imaging and diagnostic tests are possible. These include:
- Blood tests .
- Positron emission tomography scan.
New lab tests are possible
Researchers have found possible ways to test for possible indicators or Parkinsons disease. Both of these new tests involve the alpha-synuclein protein but test for it in new, unusual ways. While these tests cant tell you what conditions you have because of misfolded alpha-synuclein proteins, that information can still help your provider make a diagnosis.
The two tests use the following methods.
- Spinal tap. One of these tests looks for misfolded alpha-synuclein proteins in cerebrospinal fluid, which is the fluid that surrounds your brain and spinal cord. This test involves a spinal tap , where a healthcare provider inserts a needle into your spinal canal to collect some cerebrospinal fluid for testing.
- Skin biopsy. Another possible test involves a biopsy of surface nerve tissue. A biopsy includes collecting a small sample of your skin, including the nerves in the skin. The samples come from a spot on your back and two spots on your leg. Analyzing the samples can help determine if your alpha-synuclein has a certain kind of malfunction that could increase the risk of developing Parkinsons disease.
Will I Get A Parkinsons Disease Diagnosis
Its important to see your doctor if you notice Parkinsons disease symptoms over a period of time, especially if they are interfering with your daily life. You will be given a confirmed diagnosis if you meet Parkinsons disease diagnosis criteria, as long as your symptoms cannot be explained by another condition.
To be diagnosed with Parkinsons, you must show signs of bradykinesia a marked slowing of movement and reduced arm swing when walking as well as one or more of the following symptoms:
- Muscular rigidity
- Postural instability
You May Like: Is Beer Good For Parkinson’s
How Soon After Treatment Will I Feel Better And How Long Will It Take To Recover
The time it takes to recover and see the effects of Parkinson’s disease treatments depends strongly on the type of treatments, the severity of the condition and other factors. Your healthcare provider is the best person to offer more information about what you can expect from treatment. The information they give you can consider any unique factors that might affect what you experience.
How Is Parkinsons Diagnosed
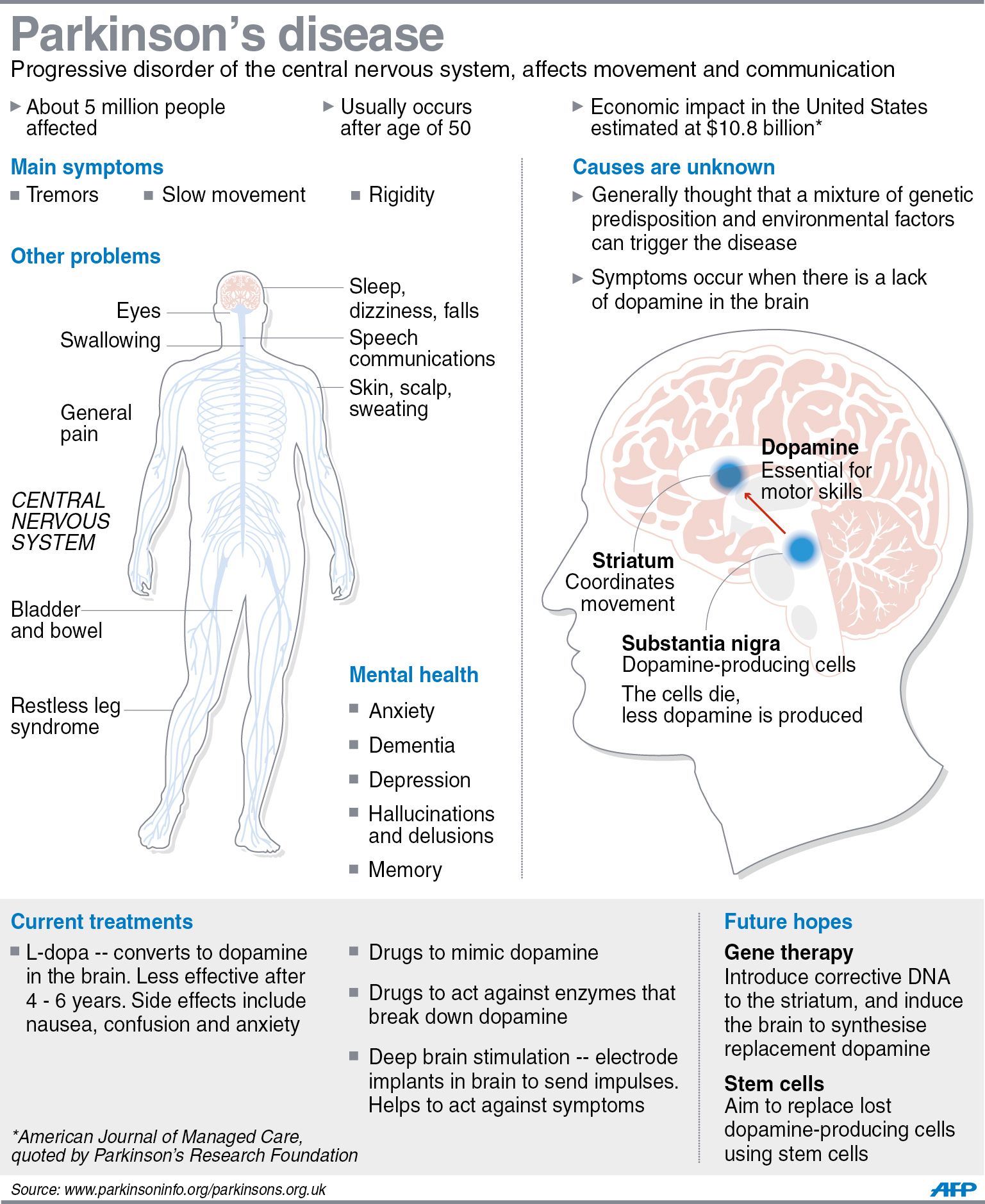
Doctors use your medical history and physical examination to diagnose Parkinson’s disease . No blood test, brain scan or other test can be used to make a definitive diagnosis of PD.
Researchers believe that in most people, Parkinson’s is caused by a combination of environmental and genetic factors. Certain environmental exposures, such as pesticides and head injury, are associated with an increased risk of PD. Still, most people have no clear exposure that doctors can point to as a straightforward cause. The same goes for genetics. Certain genetic mutations are linked to an increased risk of PD. But in the vast majority of people, Parkinsons is not directly related to a single genetic mutation. Learning more about the genetics of Parkinsons is one of our best chances to understand more about the disease and discover how to slow or stop its progression.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
Men are diagnosed with Parkinsons at a higher rate than women and whites more than other races. Researchers are studying these disparities to understand more about the disease and health care access and to improve inclusivity across care and research.
Aging is the greatest risk factor for Parkinsons, and the average age at diagnosis is 60. Still, some people get PD at 40 or younger.
The Michael J. Fox Foundation has made finding a test for Parkinsons disease one of our top priorities.
Recommended Reading: Lifespan Of Someone With Parkinson’s Disease