Research To Improve Deep Brain Stimulation
Researchers are working to improve upon existing DBS devices and methods to help treat more symptoms and more people. Some researchers are putting electrodes in a different area of the brain the pedunculopontine nucleus to treat walking and balance problems that don’t typically improve with present-day DBS. Others are developing a “smart” DBS device that can record a person’s unique brain signals and deliver electrical stimulation only when needed, such as when symptoms return, rather than continuously, as the current systems do. This could help reduce side effects such as numbness and weakness and lengthen the battery life of the neurostimulator, which would result in a longer time between battery replacement procedures.
Scientists also are planning to test deep brain stimulation in the first years after a Parkinson’s diagnosis to see if the therapy may slow or stop disease progression. Testing in Parkinson’s models showed the therapy may help protect brain cells, and a small human trial showed motor symptoms improved after early-stage DBS.
What Happens Before Surgery
In the doctor’s office you will sign consent forms and complete paperwork to inform the surgeon about your medical history, including allergies, medicines, anesthesia reactions, and previous surgeries. Presurgical tests may need to be done several days before surgery. Consult your primary care physician about stopping certain medications and ensure you are cleared for surgery.You may also need clearance from your cardiologist if you have a history of heart conditions.
Stop taking all non-steroidal anti-inflammatory medicines and blood thinners 7 days before surgery. Stop using nicotine and drinking alcohol 1 week before and 2 weeks after surgery to avoid bleeding and healing problems.
You may be asked to wash your skin and hair with Hibiclens or Dial soap before surgery. It kills bacteria and reduces surgical site infections.
No food or drink, including your Parkinson’s medication, is permitted after midnight the night before surgery.
Try to get a good night’s sleep. The DBS surgery involves multiple steps and lasts most of the day, during which you may be awake and off medication.
Morning of surgery
Arrive at the hospital 2 hours before your scheduled surgery time to complete the necessary paperwork and pre-procedure work-ups. An anesthesiologist will talk with you and explain the effects of anesthesia and its risks.
Will I Have To Limit My Activity Following Deep Brain Stimulation Surgery
- You should not engage in light activities for 2 weeks after surgery. This includes housework and sexual activity.
- You should not engage in heavy activities for 4 to 6 weeks after surgery. This includes jogging, swimming, or any physical education classes. Anything strenuous should be avoided to allow your surgical wound to heal properly. If you have any questions about activities, call your doctor before performing them.
- You should not lift more than 5 lbs. for at least 2 weeks.
- You should not raise your arms above your shoulders or over bend or stretch your neck.
- Depending on the type of work you do, you may return to work within 4 to 6 weeks.
Recommended Reading: Drugs That Can Mimic Parkinson’s Disease
Inclusion Criteria And Search Strategy
We included articles that met the following criteria: meta-analyses and primary studies including PD patients who had undergone DBS that assessed personality characteristics encompassed by the multilayer framework described previously. To compile our list of articles, we relied on previous knowledge of the relevant research, conducted searches on Google Scholar including the terms Deep Brain Stimulation,DBS,Parkinson’s Disease,personality, and personality change , and used connectedpapers.com to discover relevant papers that cited articles we decided to include in the review.
Reduces Dyskinesia And Fluctuations
Medtronic DBS therapy reduces complications of drug therapy, such as dyskinesia and fluctuations in on and off time.3,4,5,6 Medtronic DBS therapy reduces complications of drug therapy by 37% to 61% compared to medication alone.4,5 Without DBS, people receiving best medical therapy experience between a 5.4% reduction to a 13% increase in drug-related complications compared with their baseline.4,5
You May Like: Cbd Dosage For Parkinsons
You May Like: Can You Drive If You Have Parkinson’s Disease
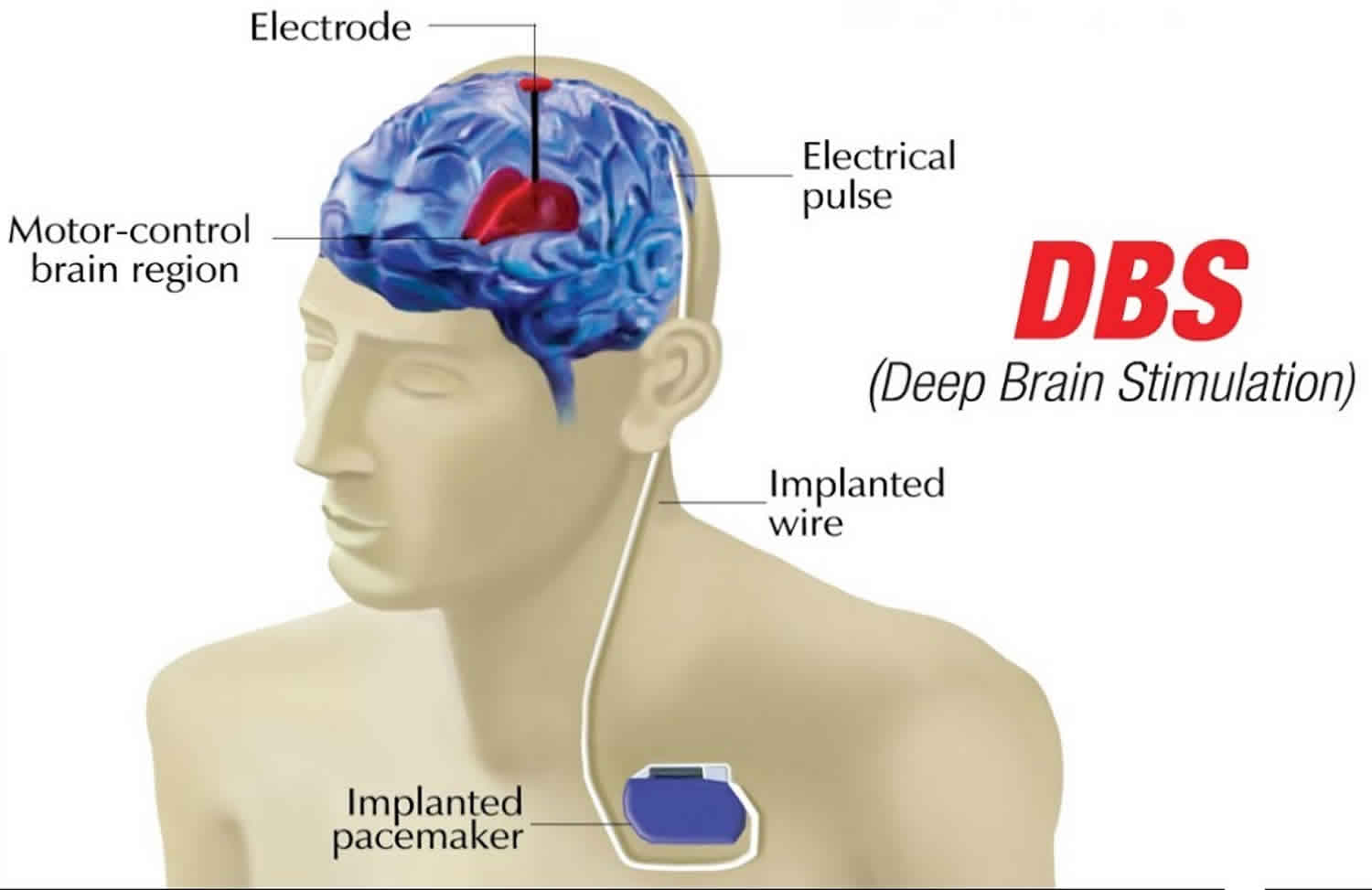
How Is Deep Brain Stimulation Used To Treat Parkinsons Disease
Deep brain stimulation delivers electrical impulses to a targeted area of the brain that is responsible for the movement symptoms caused by Parkinsons disease. The electrical impulses disrupt the abnormal activity that occurs in the brains circuitry, which is causing the symptoms.
There are three areas in the brain that can be targets for deep brain stimulation in patients with Parkinsons disease. They are the subthalamic nucleus, the globus pallidus internus, and the ventral intermediate nucleus of the thalamus. Each of these areas plays a role in the brains circuitry that is responsible for the control of movement.
The specific area in the brain to target in an individual with Parkinsons disease depends on symptoms that need to be treated. For example, deep brain stimulation of subthalamic nucleus is effective for all major movement symptoms of Parkinson’s disease, such as tremor, slowness of movement , stiffness , and problems with walking and balance. Deep brain stimulation of globus pallidus is another effective target for a wide range of Parkinson’s symptoms. The thalamic target is sometimes selected for patients with tremor symptoms. The recommended target for each patient is made collaboratively with the neurologist, neurosurgeon and other caregivers involved in the decision making process.
Deep Brain Stimulation Success Rate For Non
Patients with Parkinsons disease have non-movement problems as well. These include sleep problems, constipation, pain and many others. You can find articles on these problems on the site.
Thankfully, DBS decreases many of these non-motor problems. For example, sleep improves after DBS. I, along with my colleagues at Kings college, published a research paper on improvement in sleep after DBS in 2018.
The effect of DBS on some non-motor symptoms is unknown. For example, we dont know if DBS reduces excessive sweating and urinary problems.
Unfortunately, DBS may worsen a few non-motor symptoms.
- If you already have thinking/memory problems, DBS may worsen them.
- If you already have severe depression, DBS may worsen it.
This possible worsening is important to consider. Please read these two articles to know more: .
Recommended Reading: Amino Acid Used To Treat Parkinson’s Disease
Risks Associated With Dbs
Anytime surgery is involved, risk is involved, too. Some serious side effects include brain bleed, stroke, infection, or impacted memory. Also, part of the reason doctors screen potential DBS candidates for dementia and Alzheimers disease is to avoid worsening underlying memory problems.
As the Mayo Clinic notes, DBS is a potentially risky procedure, and patients should carefully weigh the risks and potential benefits of the procedure. Read more about possible side effects here.
How Does Dbs Treat Parkinsons
Parkinsons disease causes irregular electrical signals in parts of the brain that control movement. DBS uses electrical stimulation to modulate these control centers deep to the surface of the brain, improving communication between brain cells.
This helps to reduce symptoms such as tremor, slowness, and stiffness. It doesnt have much of an effect on non-motor symptoms or balance issues. Here are some additional tips for improving motor skills with Parkinsons.
DBS is the most commonly performed surgical procedure for symptoms of Parkinsons disease.
DBS isnt a first-line therapy. Its intended for people whose symptoms are still unmanageable even with medication. Learn about other advanced and future treatments for Parkinsons.
You might be a good candidate for DBS if:
- youve had symptoms for at least five years
- your symptoms respond to medication, but the effect doesnt last as long as it used to
- youve tried various doses and combinations of medications
- your symptoms interfere with everyday life
Your doctor is unlikely to recommend DBS if:
- Parkinsons medications havent helped much
- you have memory and thinking problems
- you have anxiety or depression that hasnt stabilized with treatment
- you have dementia
Recommended Reading: Mucuna Plants For Parkinson’s Disease
What Is The Dbs Surgery Process
Patients suitable for this surgery will be brought to the hospital and taken through the necessary preoperative evaluations. They will undergo DBS surgery on the second day, where the actual brain surgery part of the intervention is. The patients are awake, able to talk with us and communicate their experiences during the surgery.
During this approximate 2.5-hour process, the medical team creates the physiological map of the brain using the Microelectrode Recording and Stimulation technique and by establishing cooperation with the patient. The surgeon places DBS electrodes by locating the brain cells responsible for the disease with an error margin of fewer than 80 microns.
Afterward, within half an hour, when the patient is anesthetized, the surgeon places the neurostimulator in the chest area and connects it to the DSB electrodes with extension cables. After the operation, the treating doctor provides neurostimulator programming, reduces and adjusts the patient’s medications within 2-3 weeks of outpatient clinic control.
What Happens After Surgery
After surgery, you may take your regular dose of Parkinson’s medication immediately. You are kept overnight for monitoring and observation. Most patients are discharged home the next day.
During the recovery time after implanting the electrodes, you may feel better than normal. Brain swelling around the electrode tip causes a lesion effect that lasts a couple days to weeks. This temporary effect is a good predictor of your outcome once the stimulator is implanted and programmed.
About a week later, you will return to the hospital for outpatient surgery to implant the stimulator in the chest/abdomen. This surgery is performed under general anesthesia and takes about an hour. Patients go home the same day.
Step 7: implant the stimulator You will be taken to the OR and put to sleep with general anesthesia. A portion of the scalp incision is reopened to access the leads. A small incision is made near the collarbone and the neurostimulator is implanted under the skin. The lead is attached to an extension wire that is passed under the skin of the scalp, down the neck, to the stimulator/battery in the chest or abdomen. The device will be visible as a small bulge under the skin, but it is usually not seen under clothes.
You should avoid arm movements over your shoulder and excessive stretching of your neck while the incisions heal. Pain at the incision sites can be managed with medication.
Also Check: How To Tell Difference Between Parkinson’s And Essential Tremor
Some Common Concerns And Misconceptions About Dbs
My condition is not bad enough to necessitate DBS.In Parkinsons disease, there is a window of opportunity wherein one can undergo DBS. If a patient has progressed to moderate or severe dementia, DBS is not an option. Furthermore, DBS is appropriate when medication still has a positive effect but is becoming less reliable, or, when side effects are intolerable. Once medications are ineffective, DBS will not be a treatment option. One should inquire about DBS when PD symptoms and effectiveness of medications change, and before dementia sets in. A neurosurgeon or neurologist can help to monitor your symptoms. DBS does not cure PD, and if it progresses we can fine tune programming for continued effectiveness.
The battery needs to be replaced often and will include an invasive procedure.Generator replacement takes 15 minutes, can be accomplished under local anesthesia and is done every three-to-five years on average.
I cannot afford DBS.DBS is covered by all major insurances, including Medicare and Medicaid.
- Categories
Up To Five Additional Hours Of Good Movement Without Dyskinesia
Good movement control means no troubling symptoms like shaking, stiffness, and difficulty moving. DBS therapy can provide up to five additional hours of good movement control without dyskinesia per day, compared with medication alone.*2,3,4 What would you do with five additional hours every day?
*Measured by the UPDRS IV
Recommended Reading: Parkinsons Disease And Cbd
Read Also: Is Coughing A Sign Of Parkinson’s Disease
Efficacy Of Local Versus General Anesthesia Techniques
A meta-analysis of 145 studies of DBS in PD showed that the mean target error was not significantly different between LA and GA however the mean number of DBS lead passes were significantly less with GA as compared to LA .62 Post DBS complications were significantly lower with GA . The two techniques did not differ significantly in UPDRS II scores off medication, UPDRS III scores off and on medication or LED. UPDRS IV off medication score decreased more significantly in awake DBS versus sleep DBS cohorts .62 Hence, most DBS procedures should ideally be carried out under LA due to the lower side effect profile.
Deep Brain Stimulation Surgery
A team of experts, including a movement disorder specialist and a brain surgeon, conducts an extensive assessment when considering DBS for someone. They review your medications and symptoms, examine you when you’re on and off Parkinson’s medication, and take brain imaging scans. They also may do detailed memory/thinking testing to detect any problems that could worsen with DBS. If your doctors do recommend you for DBS and you are considering the surgery, discuss with your care team the potential benefits as each person’s experience is unique. It’s also critical to discuss the potential surgical risks, including bleeding, stroke and infection.
In DBS surgery, the surgeon places thin wires called electrodes into one or both sides of the brain, in specific areas that control movement. Usually you remain awake during surgery so you can answer questions and perform certain tasks to make sure the electrodes are positioned correctly. Some medical centers now use brain imaging to guide the electrodes to the right spot while a person is asleep. Each method has its pros and cons and may not be suitable for everyone or available everywhere.
Once the electrodes are in place, the surgeon connects them to a battery-operated device , which usually is placed under the skin below the collarbone. This device, called a neurostimulator, delivers continuous electrical pulses through the electrodes.
Recommended Reading: Parkinson’s Disease Symptoms And Treatment
How Is Deep Brain Stimulation Performed
Before the actual procedure begins, for most patients, a head frame is positioned on your head, which keeps your head still during brain imaging and is used to deliver the electrode to the target in the brain. Surgical pins or screws are used to secure the frame to your head. Sedation is typically given during this portion of the procedure.
Your neurosurgeon will implant the deep brain stimulation system in one to three stages.
First, a small hole is made in the skull. The leads, which have electrodes at the ends, are passed through this hole and surgically implanted in the areas of the brain identified as the site responsible for the movements caused by Parkinsons disease.
Most people with Parkinsons disease will require one lead placed on each side of the brain unless symptoms are mostly one-sided . Each side of the brain controls the opposite side of the body, so each lead is inserted on the opposite side of where symptoms are occurring. Sometimes this procedure is done in stages one lead is placed at one time followed by another surgery for the other side. In other patients, both leads are placed during the same operation. Many times patients are awake during lead insertion. An intraoperative MRI is also sometimes used to image the lead location.
Read Also: How To Tell The Difference Between Essential Tremor And Parkinsons
During The Deep Brain Stimulation Surgery
In general, heres how surgery for deep brain stimulation works:
Brain surgery
For the brain surgery portion, your care team fits you with a special head frame to keep your head still during the procedure . Then, team members use magnetic resonance imaging to map your brain and identify the area in your brain where theyll place the electrodes.
Surgery can be done under general anesthesia so that youll be unconscious. Or the procedure can be done with you awake and alert. If youre awake for surgery, youll be given a local anesthetic to numb your scalp before the procedure, but you wont need an anesthetic in your brain itself because the brain has no pain receptors.
Your surgeon implants a thin wire lead with a number of contacts at the tips into a specific area of your brain. Or one lead is implanted into each side of the brain . A wire runs under your skin to a pulse generator implanted near your collarbone.
During surgery, both the neurologist and surgeon carefully monitor your brain to help ensure correct electrode placement.
Chest wall surgery
During the second portion of the surgery, the surgeon implants the part of the device that contains the batteries under the skin in your chest, near your collarbone.
General anesthesia is used during this procedure. Wires from the brain electrodes are placed under your skin and guided down to the battery-operated pulse generator.
Read Also: Parkinson’s Disease And Sleep Disorders
Who Is Not A Good Dbs Candidate
You are not a good candidate for DBS if:
- You have Parkinsons plus symptoms or do not have a clear diagnosis of Parkinsons.
- You need full-body MRI scans, or certain head and chest MRI scans.
- You cannot operate the internal pulse generator, also called the stimulator or IPG.
- Test stimulation does not work.
- You have certain brain conditions such as ischemic brain disease, demyelinating brain disease or brain tumors.
- You have significant intellectual or memory impairment.
- You are not healthy enough to have surgery or have other untreated or chronic illnesses.
DBS can work well for certain people. But it can make certain symptoms of Parkinsons worse. People with certain symptoms should not have DBS. These include:
- Having Parkinsons that is not a typical form of the disease.
- Having Parkinsons plus symptoms such as multiple system atrophy, progressive supranuclear palsy or vascular parkinsonism.
- Not functioning well, even with medication for example, not being able to walk even when taking medication.
- Having end-stage Parkinsons.
At OHSU, we are committed to providing the best treatment for everyone with Parkinsons, so our specialists will talk with you about other options if DBS is not right for you.
You May Like: Parkinsons Staring Into Space