Anesthetic Drugs May Interact With Medications Used For Parkinsons Disease
Lorri A. Lee, MD Tricia A. Meyer, PharmD, MS, FASHP
An estimated one million people in the United States have been diagnosed with Parkinsons Disease making it one of the most common neurological disorders in patients. This number is estimated to double in the next 30 years as PD is associated with increasing age. PD patients have a deficiency of dopamine in their brain and many of their medications are used to increase this neurotransmitter. They are frequently very sensitive to missing even one dose of their Parkinson medications and may exhibit increased rigidity, loss of balance, agitation, and confusion if their dosing schedule is delayed. Neuroleptic malignant syndrome or parkinsonism-hyperpyrexia syndrome can develop if their medications are held too long or as a result of serious infection.1 Many drugs used in the perioperative period, such as metoclopramide, butyrophenones , and phenothiazines have anti-dopaminergic activity that can worsen the symptoms of PD.
PD patients may be prescribed selective MAOI-B medications such as selegiline and rasagiline that inhibit metabolism of dopamine. Though caution is still advised, several studies have demonstrated that the risk of serotonin syndrome with these selective MAOI-B drugs is extremely low, even in combination with serotonergic antidepressants.
The authors have no conflicts of interest to declare for this article.
A Pragmatic Approach To The Perioperative Management Of Parkinsons Disease
Published online by Cambridge University Press: 22 September 2020
- Department of Neurology, Georgetown University Hospital, Washington, DC, USA
- Shivam Om Mittal
- Department of Neurology, Cleveland Clinic, Abu Dhabi, United Arab Emirates
- Guillaume Lamotte
- Department of Neurology, Mayo Clinic, Rochester, MN, USA
- Fernando Luis Pagan
- Department of Neurology, Georgetown University Hospital, Washington, DC, USA
- *
- Correspondence to: Dr. Abhishek Lenka MD, Ph.D., Department of Neurology, Georgetown University Hospital
Parkinson’s Disease And Anaesthesia Bja: British Journal
- Parkinson disease is a progressive, chronic condition affecting approximately 4 million people worldwide it is the second most common neurodegenerative disorder after Alzheimer disease. 1 In the United States, the prevalence of PD in the elderly population has been reported to be 1% to 2% in persons aged 65 years 2 and 4% to 5% in persons aged > 85 years, which is noticeably larger.
- Parkinson’s disease is the second most common neurodegenerative disease, with a prevalence of 1.8 per 100 in people aged 65 or over in Europe. 1 Historically, it has been regarded as a motor condition characterised by rigidity, bradykinesia and tremor. Increasingly, however, non-motor complications of the disease, such as depression, dementia and autonomic dysfunction, are being.
- Q: Should I stop my Parkinson’s disease medications before general surgery or an operation? A: Some neurologists recommend that medications be stopped 12 hours prior to general anesthesia for surgery.If you are on a complicated drug regimen, ask your surgeon prior to surgery to contact the physician responsible for your Parkinson’s disease therapy so that your drugs can be given appropriately
- Most side effects of general anesthesia occur immediately after your operation and don’t last long. Once surgery is done and anesthesia medications are stopped, you’ll slowly wake up in the.
- e response to fluid boluses. [ More
Don’t Miss: Neurostimulator For Parkinson’s Disease
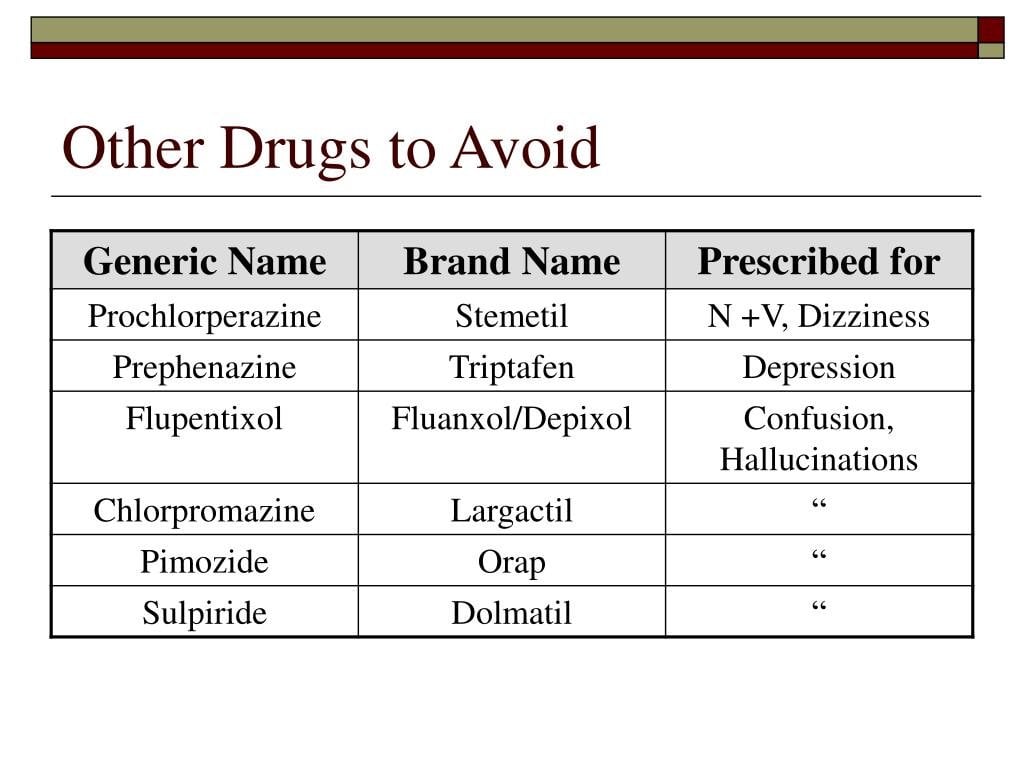
Medications To Avoid Before Outpatient Surgery
If you are considering having a procedure in the safe setting of an outpatient surgery center in the Triangle, it is recommended that you are prepared in the best way you can. Your doctors will make sure the outcome of the procedure is the most beneficial that it can be. But there are factors that you, as the patient, should take into consideration when getting ready for this important day.
One of these factors, among diet, physical therapy, stopping smoking, or keeping your doctors special instructions, is the use of certain medications, even up to two weeks before surgery.
Here is the list of those you should avoid or stop taking:
Cholinesterase Inhibitors Widely Used To Treat Dementia
Cholinesterase inhibitors, widely used to treat dementia, may cause worsened parkinsonism, primarily increased tremor . Large double-blind trials of rivastigmine, a cholinesterase-inhibiting drug, in both dementia with Lewy bodies and Parkinson disease dementia have demonstrated that rivastigmine is well tolerated without significant worsening of motor function overall, although tremor may increase . The other cholinesterase inhibitors have been less well studied but appear to have similar benefits and side effects.
You May Like: Can Parkinson’s Go Away
Delayed Administration And Contraindicated Drugs Place Hospitalized Parkinsons Disease Patients At Risk
Problem: One-third of all patients with Parkinsons disease visit an emergency department or hospital each year, making it a surprisingly common occurrence.1 The disease affects about 1 million people and is currently the fourteenth leading cause of death in the US. Hospitalization can be risky for patients with Parkinsons disease when viewed from the perspective of pharmacological management.
Patients with Parkinsons disease require strict adherence to an individualized, timed medication regimen of antiparkinsonian agents. Dosing intervals are specific to each individual patient because of the complexity of the disease. It is not unusual for patients being treated with carbidopa/levodopa to require a dose every 1 to 2 hours. When medications are not administered on time, according to the patients unique schedule, patients may experience an immediate increase in symptoms.2,3 Delaying medications by more than 1 hour, for example, can cause patients with Parkinsons disease to experience worsening tremors, increased rigidity, loss of balance, confusion, agitation, and difficulty communicating.2 Studies show that three out of four hospitalized patients with Parkinsons disease do not receive their medications on time, or have had doses entirely omitted.4 According to the National Parkinson Foundation, 70% of neurologists report that their patients do not get the medications they need when hospitalized.2
Two case examples
Other medication safety concerns
References
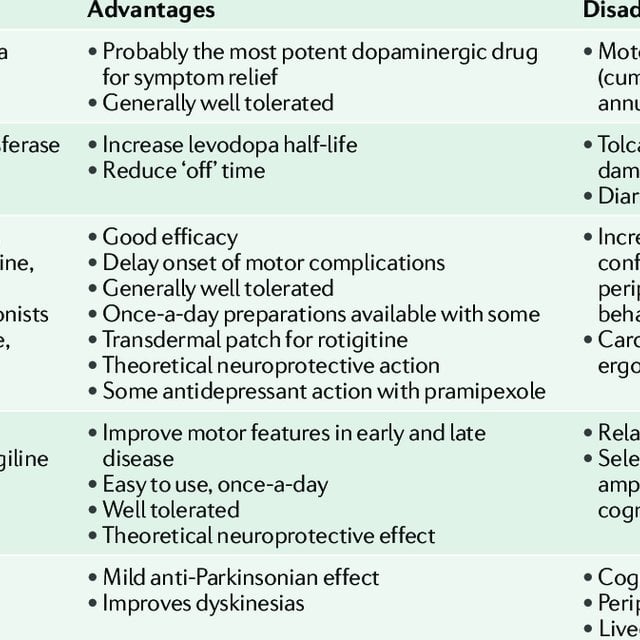
Ldopa And Dopamine Agonists
Apomorphine is a shortacting dopamine agonist that is administered subcutaneously, or sometimes sublingually or intranasally. An important sideeffect is nausea and vomiting, but with the concurrent use of domperidone it may be well tolerated. It is particularly useful administered as an infusion to smooth out motor fluctuations or rescue patients from off periods. It is not widely available, as expertise supervising the use of infusion pumps is essential.
Don’t Miss: How To Prevent Getting Parkinson’s Disease
Surgery Complications For People With Parkinson’s Apd
Nausea is a common problem that is often encountered as a side effect of Parkinson’s disease dopaminergic treatments-The most important first step is to determine if the nausea is caused by a the Parkinson medication (does it occur predictably after each dose, and did it begin shortly after beginning a new Parkinson’s disease medication in your overall pharmacological regimen The drug’s dosage is controlled by a mini-pump weighing about half a kilogram that the patient wears at the waist. The body transforms levodopa to dopamine to increase the amount of dopamine in the brain. Parkinson’s disease symptoms are linked to dopamine levels
Any Medication That Blocks Dopamine In The Body Can Cause Parkinsons Symptoms
You may have heard of Parkinsons disease , a movement disorder. Someone with it may have characteristic signs, such as a pill-rolling tremor in the fingers or a hunched forward posture. You may recognize someone with this disease from the faltering, tiny steps they take when they walk or by their rigidly emotionless face.
The cause of Parkinsons disease is mostly unknown. Some people develop Parkinsons-like symptoms after treatment with certain medications. This is called drug-induced parkinsonism or secondary parkinsonism. Certain medications can also worsen symptoms in someone who already has Parkinsons disease.
Any medication that blocks dopamine in the body can cause Parkinsons symptoms. Dopamine is a brain chemical that helps control movement. Common dopamine-blocking drugs are antipsychotics. They are used to treat certain mental illnesses or severe nausea. Less commonly, certain types of calcium channel blockers cause drug-induced parkinsonism. These drugs may be used to treat chest pain and high blood pressure, or irregular heart rate.
Recommended Reading: Stages Of Parkinson’s What To Expect
A Critical Reappraisal Of The Worst Drugs In Parkinsons Disease
What are the worst drugs for Parkinsons disease patients? Couldnt a simple list be assembled and disseminated to the Parkinson community? Recently Ed Steinmetz, an experienced neurologist in Ft. Meyers, FL pointed out to me, a list approach published in the Public Citizen Newsletter . The approach was to list every drug associated with a single confirmed or unconfirmed symptom of Parkinsons disease or parkinsonism. Parkinsons disease is defined as a neurodegenerative syndrome , whereas parkinsonism encompasses a wider net of drug induced and other potential causes. In parkinsonism symptoms are similar to Parkinsons disease, but patients do not have Parkinsons disease. Patients and family members confronted with a simple drug list approach may falsely conclude that most medicines are bad for Parkinsons disease, and that any medicine may cause parkinsonism. This concept is in general, incorrect. Although the approach is well-meaning, it is in need of a major revision, as Parkinsons disease and parkinsonism are too complex to summarize by simple lists. In this months column I will try to summarize the key information that patients and family members need to know about the worst pills, for Parkinsons disease and parkinsonism.
A Florida Parkinsons Treatment Blog by Michael S. Okun, M.D.
UF Center for Movement Disorders & Neurorestoration, Gainesville FL
Being Prepared & Anticipating Problems
Because of the concerns that we will discuss below, it is prudent to have your neurologist speak to your surgeon and anesthesiologist prior to the surgery so he/she can discuss the potential issues that may arise during and after the surgery. It is also very useful to have your neurologist write a letter with all the necessary information so it can be dispersed to other members of the medical team who will be responsible for your day-to-day care after the surgery.
Depending on the type of surgery, there may be more than one option for anesthesia. General anesthesia may not be the only option, and a more localized form of anesthesia may be possible. Local anesthesia typically causes fewer side effects. Discuss what anesthesia options you have with the surgeon and anesthesiologist prior to the surgery.
In addition, if the surgery requires you to stay in the hospital overnight, consider having a family member or friend stay with you. This person can provide a calming presence, helping to prevent agitation or distress. He or she can keep an eye on whether you are taking your own medications correctly and what additional medications you are bring given.
Also Check: How To Tell The Difference Between Essential Tremor And Parkinson’s
The Medication Question Parkinson’s Foundatio
- e agonists
- Try to schedule surgery in the early morning to avoid being off Parkinson’s medications for long periods. Also, see if you can avoid general.
- ergic neurones in the substantia nigra the part of the mid-brain responsible for managing movement and the dopa
- Avoid abrupt withdrawal of antiparkinsonian therapy Be alert to the possibility of Parkinsonism-hyperpyrexia syndrome Seek early specialist help Key points KEY WORDS: delirium, dysphagia, falls, Parkinson’s disease, palliative Fig 2. Maintaining Parkinson’s disease drug therapy during perioperative period (no
- Because most of the anesthesia drugs used in surgery can slow respiratory function, Parkinson’s patients are at higher risk for aspiration during surgery or recovery, she explains. can help a person with Parkinson’s avoid potential complications like.
Medications To Avoid That Worse Pd Parkinson’s Disease
Parkinson’s risk is significantly increased in people with the BChE K-variant and exposure to organophosphates. Eating organic, watching your exposure to pesticides , and avoid using pesticides in your home can reduce your exposure to organophosphates medications may cause confusion/ psychosis and constipation if patient is taking MaoB inhibitor such as selegiline or rasagiline , avoid meperidine ANESTHESIA request a consult with the anesthesiologist, surgeon and Parkinson’s doctor to determine best anesthesia given your Parkinson’s symptoms and medication Medications to treat symptoms. Your doctor may prescribe medications to treat other symptoms associated with Lewy body dementia, such as sleep or movement problems. If possible, avoid medications with anticholinergic properties, which can worsen cognition, or dopamine agonists, which can cause hallucinations The primary endpoint is the efficacy of the stimulation on motor symptoms assessed by the change in UPDRS-3 scores between OFF and ON stimulation evaluations at one year after surgery without any medical treatment . Unified Parkinson’s Disease Rating Scale 3 questionnaire: 0 to 132 points, with the highest score.
Read Also: What Age Can Parkinson’s Disease Start
Anesthetic Considerations Of Wp
- The goal during perioperative management of anesthesia was to avoid any factor that increases sympathetic activity such as pain, anxiety, fear, stress response of intubation/extubation, lighter plane of anesthesia, hypovolemia, and avoiding premedication with anticholinergic drugs. Patient was adequately counseled and reassured
- Effects of Anesthesia on Elderly Patients General anesthesia does carry a higher risk for the elderly population, admits Damon Raskin, MD, a board-certified internist and medical director for a hospice provider and two nursing homes in the Santa Monica, CA, area.According to Dr. Raskin, it takes longer for an older person’s body to rid itself of the chemicals involved in anesthesia.
- off et al., 2011). This was confirmed by an influential Canadian study.
- Veterinary Anesthesia & Analgesia Support Group: Practical Information for the Compassionate Veterinary Practitioner: Avoid in anemic patients. vi) Avoid in splenic disease patients , also used to treat Parkinson’s disease. b).
- This page includes the following topics and synonyms: Preoperative Guidelines for Medications Prior to Surgery, Preoperative Fasting Recommendation, Nothing by Mouth Prior to Surgery Guideline, Perioperative NPO Guidelines, Perioperative Medication Guidelines, Medication Management in the Perioperative Period, Medications to Avoid Prior to Surgery
Anesthetic Management For Steriotactic Pallidotomy/thalamotomy
Classically local anesthesia with minimal or no sedation has been used for patients undergoing stereotactic procedures. This allows for patient participation in target localization and immediate observation of effects of test and lesion. Antiparkinsonian mediations are withheld for 1224 h prior to surgery. Therapy for concurrent diseases must be continued till the day of surgery.
Under LA, in magnetic resonance imaging suite stereotactic frame applied. Extra padding and rolls can make the patient more comfortable. Also these patients are very motivated to co-operate, unless there is dementia present. LA again is used to do burr hole and if the patient becomes agitated, midazolam can be titrated to desired effect. It is important that level of sedation does not impair co-operation or interfere with communication between surgeon and patient. Age, varying levels of dementia, fatigue, and cumulative effects of medication make it necessary to titrate the drugs slowly. Since propofol may elicit abnormal movements and may at times improve parkinsonian tremor, it might not be ideally suited for patients with movement disorders undergoing functional stereotactic neurosurgery.
Read Also: Adaptive Silverware For Parkinson’s
Disadvantages Of Regional Anesthesia Over General Anesthesia
Regional anesthesia will not eliminate Parkinson’s symptoms, such as tremor or rigidity, except in the areas directly affected by the anesthetic.
Tremor can interfere with some monitoring device and makes it more difficult to interpret.
If the surgery is delicate, the surgeon may want the patient to be absolutely still.
The surgical procedure may not be possible under regional anesthesia.
Preoperative Use Of Levodopa
Patients with advanced Parkinson’s disease are at risk for exacerbations in the perioperative period. The timing of doses of Parkinson’s medication is very important, as abrupt withdrawal of drugs can often cause a very sudden return or even worsening of symptoms and in some cases can lead to the development of a condition known as neuroleptic malignant syndrome, which can be very dangerous. The half-life of levodopa is 13 h and so interruption should be as brief as possible, and therapeutic administration should be continued through the morning of surgery with sips of water. As it is absorbed from the proximal small bowel and thus has to first traverse the stomach making administration of tablets through gastric tube suboptimal or ineffective, because patients with Parkinson’s often have delayed gastric emptying. As such a duodenal feeding tube may be necessary when a prolonged period of normal feeding is expected. Patients may self-administer additional levodopa, so it is important to find out exactly how much they are taking.
Enteral levodopa has a clear advantage over intravenous levodopa and should be preferred. Treatment with and drug titration of levodopa for intravenous administration alone may be dangerous during general anesthesia because of interactions with anesthetic agents. It may increase the risk of a variety of arrhythmias or hypertension. These side effects of levodopa are mediated through its metabolite, dopamine.
Recommended Reading: Do I Have Parkinson’s Or Anxiety
Nicotine Alcohol Marijuana Or Cannabidiol Products
These substances, used both for medicinal or recreational use, may affect your heart rate, blood pressure, and pain control during and after your procedure. Go to www.facs.org/quitsmoking to help you quit smoking before the surgery.
Remember, it is important to fully inform your surgical team about all of the medications you are taking before your surgery, including prescriptions, vitamins, minerals, herbs, drugs, or any other supplements.
Here you will find a list of medications for you to fill out and pass to your surgeon, prepared by the American College Of Surgeons.
In the end, outpatient surgical centers provide many benefits and advantages for surgical patients. If you have any other questions concerning surgeries performed in outpatient surgery centers, or would like to know how our outpatient surgery center can cater to your needs, please contact our Outpatient Surgery Center, NC. We will be more than happy to answer all of them, in the most professional and understanding way.
The Raleigh Orthopaedic Surgery Centers board certified fellowship-trained surgeons bring together many years of experience to manage and treat joint complications resulting from degenerative joint diseases such as arthritis, musculoskeletal disease or joint trauma.
To schedule an appointment wit our Outpatient Surgery Center, NC, please call 919-719-3070.