Is Parkinsons Fatal What Can I Do About It
August 24, 2021 by Zach Galati
Is Parkinsons fatal? Can you die from Parkinsons disease? These questions have probably been asked by everyone who has ever been diagnosed with this disease. And while the answer to this question is simple, its still very important to understand, so that you can live a healthy and long life.
Gut Microbiome Of Patients Favors Inflammation Study Suggests
Here, an international team of scientists conducted analyses of data collected from 55 Parkinsons patients and 55 people without the disease . The collected data included evaluations of stool and blood samples, as well as clinical data.
In line with prior findings, this analysis found that Parkinsons patients had reduced levels of fecal butyrate, and lower abundances of butyrate-producing bacteria in their guts.
Statistical analyses also showed that, among those with Parkinsons, lower levels of butyrate were associated significantly with more severe depression, as measured by the Geriatric Depression Scale .
The scientists then conducted a series of analyses to look for epigenetic changes associated with altered butyrate levels. Epigenetics refers to chemical alterations made to DNA molecules that do not alter the genetic sequence, but can change how the DNA is read for instance, increasing or decreasing the activity of individual genes.
This study is the first to examine the possible role of epigenetic changes as a link between gut microbiota, its metabolites, and the pathophysiology of neural and immune cells in Parkinsons, the researchers wrote.
Our results suggest that butyrate may impact through epigenetic effects on innate immune cells, the researchers wrote.
You May Like: Sam Waterston Parkinsons
Treating And Managing Bowel Problems
The first step in dealing with bowel disorders is to talk to your doctor. He or she will probably review your medication to see if this is a contributory factor. Whilst it is usually possible to control any difficulties with diet, fluid intake and exercise, your doctor, or Parkinsons nurse specialist if you have one, will be able to advise further, and may, for example, prescribe laxatives in severe cases of constipation. If you have any alarm features such as unintentional weight loss or rectal bleeding, then you may need to be referred for specialist assessment.
The following healthcare professionals can also advise on aspects of bowel care:
- A dietician will be able to advise on diet and fluid.
- A physiotherapist may be able to help with advice and abdominal exercises which will help in passing stools.
- A speech and language therapist can help with swallowing problems. They may be able to advise on ways of relaxing your throat, and give guidance on posture and exercises to help overcome any difficulties you have.
- An occupational therapist may also be able to suggest practical ways to overcome any difficulties you have with eating and drinking.
You May Like: Parkinson’s Hallucinations Commercial
Hospice Eligibility For Parkinsons Disease
Due to the progressive nature of Parkinsons disease, it can be challenging for families to know when their loved one is eligible for the support of hospice care. If a loved one has been diagnosed with six months or less to live or if they have experienced a decline in their ability to move, speak, or participate in the activities of daily living without caregiver assistance, it is time to speak with a hospice professional about next steps.
What Examinations May I Need To Have
Your GP or specialist will probably ask a series of questions to find out what the problem is. These may include:
- When did the trouble start?
- How often does it happen?
- Can you feel when your bladder or bowel is full?
- Are you having difficulty emptying your bladder or bowel?
- How often are you using the toilet?
Parkinsons symptoms, such as slowness of movement and rigid muscles, affect the muscles in the bowel wall. This can make it harder to push stools out of the body. You may be asked to keep a chart for several days of how often you use the toilet and how much you drink.
You may also be asked for a urine sample to test for infection and they will normally carry out a physical examination.
Bladder or bowel problems can be complex in Parkinsons, so sometimes specialist tests or X-rays may be needed. All of these can usually be done in an outpatient department or clinic.
Recommended Reading: Similar To Parkinsons
Don’t Miss: Judy Woodruff Health Problems
What Is Parkinsons Disease
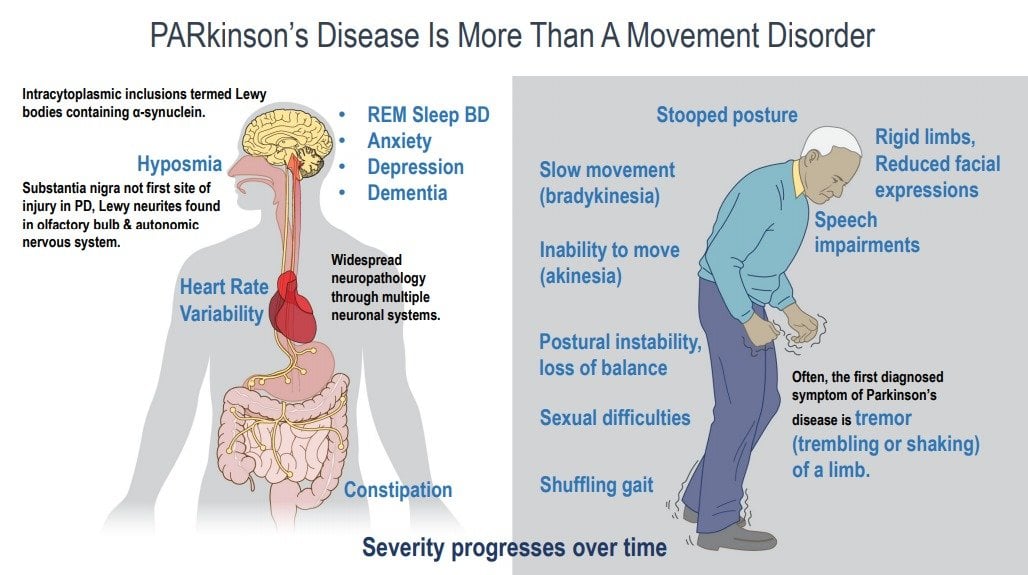
Parkinsons disease is the second most common neurodegenerative disorder and the most common movement disorder. Characteristics of Parkinsons disease are progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks.
The progression of Parkinsons disease and the degree of impairment vary from person to person. Many people with Parkinsons disease live long productive lives, whereas others become disabled much more quickly. Complications of Parkinsons such as falling-related injuries or pneumonia. However, studies of patent populations with and without Parkinsons Disease suggest the life expectancy for people with the disease is about the same as the general population.
Most people who develop Parkinsons disease are 60 years of age or older. Since overall life expectancy is rising, the number of individuals with Parkinsons disease will increase in the future. Adult-onset Parkinsons disease is most common, but early-onset Parkinsons disease , and juvenile-onset Parkinsons disease can occur.
Living With Parkinson Disease
These measures can help you live well with Parkinson disease:
- An exercise routine can help keep muscles flexible and mobile. Exercise also releases natural brain chemicals that can improve emotional well-being.
- High protein meals can benefit your brain chemistry
- Physical, occupational, and speech therapy can help your ability to care for yourself and communicate with others
- If you or your family has questions about Parkinson disease, want information about treatment, or need to find support, you can contact the American Parkinson Disease Association.
Recommended Reading: Diseases Similar To Parkinsons
Other Concerns To Be Aware Of
There are a few other possible concerns to be aware of when having surgery. Again, not everyone will experience these issues, but it is wise to understand them and be aware so that you can plan accordingly and be prepared.
- The effect of even mild dehydration may be exacerbated in PD.
- People with PD may have swallow dysfunction. This can be exacerbated by anesthesia and make people with PD at higher risk for aspiration, defined as the tendency for food or liquid to get into the airway. Therefore, it is best to introduce soft foods slowly after surgery.
- People with PD may have significant fluctuations of blood pressure which can be magnified in the post-operative period. Episodes of low blood pressure can cause dizziness and even fainting. This problem is most prominent when changing head position that is moving from lying down, to sitting to standing. Therefore, these changes should be made very slowly.
- Urinary dysfunction is common in PD, and people with PD may be particularly prone to urinary tract infections . It is important to note that UTIs or any infection may first manifest as an unexplained worsening of PD symptoms or initiation of hallucinations.
- People with PD are particularly prone to constipation and this can be exacerbated in the post-operative period. Taking a daily medication to prevent constipation may become necessary after surgery.
Tips and takeaways
Do you have a question or issue that you would like Dr. Gilbert to explore? Suggest a Topic
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Also Check: What Foods Should Be Avoided When Taking Levodopa
Apda In Your Community
APDAUncategorizedDeath in Parkinsons Disease
This article was written at the request of a Parkinsons patient who wanted to know how patients die from PD.
Most patients die with Parkinsons Disease and not from it. The illnesses that kill most people are the same as those that kill people with PD. These are heart conditions, stroke and cancer. As we age we become increasingly aware that more than one bad thing can happen to our bodies.
How Is Parkinson Disease Diagnosed
Parkinson disease can be hard to diagnose. No single test can identify it. Parkinson can be easily mistaken for another health condition. A healthcare provider will usually take a medical history, including a family history to find out if anyone else in your family has Parkinson’s disease. He or she will also do a neurological exam. Sometimes, an MRI or CT scan, or some other imaging scan of the brain can identify other problems or rule out other diseases.
Don’t Miss: On And Off Phenomenon
Fecal Incontinence In Advanced Parkinsons Disease
Fecal incontinence is a very debilitating symptom that can occur in advanced PD and refers to the involuntary release of fecal matter.
Once again, fecal incontinence, especially if it is a new symptom, should be fully evaluated to determine if there is a cause unrelated to PD. Diseases of the gut such as inflammatory bowel disease or compression of the lower spine cord can be the reason.
If related to PD, there are typically two situations to consider. One possibility is that severe constipation with impacted bowel movement allows loose stool from higher up in the gastrointestinal tract to escape around the edges of the obstruction. In this situation, fecal incontinence could be a harbinger of bowel obstruction. Aggressive and continuous treatment of constipation can help avoid this potential scenario.
Fecal incontinence can also be related to nerve dysfunction of the anal sphincter, or the ring of muscle that controls when feces is released. Cognitive dysfunction and mobility issues may further interfere with getting to the bathroom in time. Some treatment options are similar to urinary incontinence including the use of bedside equipment to minimize mobility issues and introduction of pelvic floor exercises to strengthen the musculature that keeps feces in place.
As with urinary incontinence, frequent and rapid exchange of dirtied incontinence products can keep skin intact and prevent infection.
Tips and Takeaways
Read Also: Exercise Class For Parkinsons Disease
What Lifestyle Changes Can I Make To Ease Parkinsons Symptoms

Exercise: Exercise helps improve muscle strength, balance, coordination, flexibility, and tremor. It is also strongly believed to improve memory, thinking and reduce the risk of falls and decrease anxiety and depression. One study in persons with Parkinsons disease showed that 2.5 hours of exercise per week resulted in improved ability to move and a slower decline in quality of life compared to those who didnt exercise or didnt start until later in the course of their disease. Some exercises to consider include strengthening or resistance training, stretching exercises or aerobics . All types of exercise are helpful.
Eat a healthy, balanced diet: This is not only good for your general health but can ease some of the non-movement related symptoms of Parkinsons, such as constipation. Eating foods high in fiber in particular can relieve constipation. The Mediterranean diet is one example of a healthy diet.
Preventing falls and maintaining balance: Falls are a frequent complication of Parkinson’s. While you can do many things to reduce your risk of falling, the two most important are: 1) to work with your doctor to ensure that your treatments whether medicines or deep brain stimulation are optimal and 2) to consult with a physical therapist who can assess your walking and balance. The physical therapist is the expert when it comes to recommending assistive devices or exercise to improve safety and preventing falls.
You May Like: Judy Woodruff Parkinson’s
So What Relationship Do The Health Effects Of Parkinsons Have With Death
The adverse health effects of Parkinsons are serious, and you should work with your doctor to explore the many ways to manage your Parkinsons symptoms. However, Parkinsonian symptoms do not directly cause death, but they do increase your risk for other factors that can lead to death. For instance, one of the symptoms of Parkinsons is postural instability which leads to an increased risk of falls. Postural instability by itself will not cause death but falls can lead to serious injuries that can result in death. So, Parkinsons symptoms can increase the risk for death but will not cause death in and of itself.
This is an important distinction to make because instead of seeing Parkinsons as a death sentence we should look at it as a manageable risk factor the same way we look at dieting. A poor diet will not kill you, but it will increase your risk for developing diseases that can. We should think of Parkinsons in the same way, that if we manage our symptoms of Parkinsons through exercise, medication, etc. we decrease the likelihood of risk factors that lead to death.
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Read Also: Does Vitamin B12 Help Parkinson’s
What Tests Are Used To Diagnose Narcolepsy
Overview Narcolepsy is a rare condition. According to the National Institute of Neurological Disorders and Stroke , it affects between 135,000 and 200,000 in the United States. Narcolepsy is a condition that causes one to feel sleepy during the day, thereby affecting your sleep-wake cycle. Proper diagnosis is required for …
Parkinsons Disease And The Gut
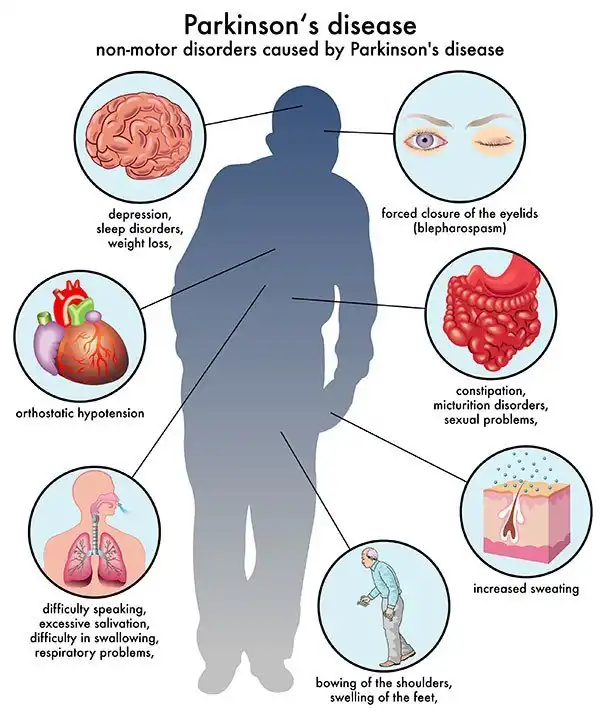
Parkinsons disease is primarily a neurological condition however, symptoms also manifest outside of the brain itself, including within the gut . This article aims to provide a simple background to Parkinsons disease, and some insights into how these GI symptoms may arise and how we can treat them. Increased awareness of these often-overlooked GI issues in Parkinsons might lead to better understanding of the condition by researchers, as well as improved treatment and quality of life for patients.
Read Also: Yopd Life Expectancy
Person With Parkinsons Glenda Kahlor 66 Lives In Georgia Usa With Her Family She Was Diagnosed With Parkinsons In 1993 At The Age Of 40
Glenda Kahlor
How did you come to be diagnosed with Parkinsons?
I fell frequently, and felt vibrations in my arm. When I had a massage, the masseuse said my muscles did not feel right and urged me to go to see a doctor. I saw several doctors, and was finally diagnosed with young-onset Parkinsons at the age of 40. Then, around three years ago, it was decided I cannot longer safely live by myself. So, I moved from rural Oklahoma, USA, to live with my daughter, son-in-law, and three teenage grandchildren in the suburbs of Atlanta, Georgia. I miss my home in the country but I love it here too.
Were you told bowel issues can affect people with Parkinsons when you were diagnosed?
In the early years, I dont recall ever having a doctor tell me that Parkinsons patients often have bowel problems.
How have you been affected by bowel issues?
My first major problems occurred in 2000. I had an intestinal blockage, and spent a week in the hospital. Severe constipation has been a problem for me a number of times.
Between the years 2000 and 2016 I was hospitalised or treated for bowel problems multiple times. Since 2016 when I moved to live with my daughter and family I have not been hospitalised. I attribute this improvement in my health to a better diet, and more exercise.
Since 2016 when I moved to live with my daughter and family I have not been hospitalised. I attribute this improvement in my health to a better diet, and more exercise
Overview Of Demyelinating Disorders
Demyelination occurs where theres damage to the myelin. Myline is the protective coating of nerve cells. When this happens, neurological problems can occur. Demyelination can result from various medical conditions, most common of which is multiple sclerosis . This article gives an overview on Demyelinating disorder. Its causes, possible …
Also Check: Voice Amplifiers For Parkinson’s
What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
Read Also: On-off Phenomenon
Schedule A Parkinson’s Gi Motility Clinic Appointment
This specialized clinic sees patients with gastrointestinal complications of Parkisnon’s disease. They will also discuss motility testing and refer you for the appropriate study if necessary. Call the clinic at .
At a newly opened clinic within the integrated UCLA Health system for treating the GI symptoms of patients with Parkinsons disease, two clinician-scientist members of the UCLA Vatche & Tamar Manoukian Division of Digestive Diseases faculty are gleaning important clues about the early manifestations of the neurodegenerative disease at the same time that they are applying their expertise as gastroenterologists to improve patients quality of life.
It is well established that gastrointestinal motor function can be negatively altered by Parkinsons disease, and an emerging body of research indicates that the disease may start in the gastrointestinal tract before later spreading to the brain. But the GI tracts role in the pathogenesis of Parkinsons disease, and the mechanisms by which Parkinsons disease alters gastrointestinal motor function, are not yet fully described.
In the lab, Dr. El-Nachef is working with Dr. Bronstein to study the involvement of the intestinal nervous system in a zebrafish model of Parkinsons disease. One of our goals in this research is to assess whether we see a loss of neurons in the intestine, what the timing of that is, and how it tracks with the development of motor symptoms in this model, Dr. El-Nachef says.
Read Also: Prayers For Parkinson’s Disease