Parkinsons: Autoimmune Attack May Start Years Before Diagnosis
A new study adds to evidence that autoimmunity plays a role in the development of Parkinsons disease. The research also offers hope that early preventive treatment could offset the damage.
Parkinsons disease is a chronic, progressive disorder. Its characteristics tend to include tremor, rigidity, slowness of movement, and impaired balance.
Around 1 million people in the United States and 10 million people throughout the world have the disease.
Parkinsons results from a loss of nerve cells in a part of the brain called the substantia nigra. These cells produce dopamine, a chemical messenger, or neurotransmitter, involved in controlling movement.
Most people with Parkinsons are older than 50 when they receive the diagnosis, but some develop motor symptoms, involving problems with muscle control, at an earlier age.
Years before motor symptoms arise, other symptoms of Parkinsons can appear, including a reduced sense of smell, constipation, mood changes, and REM sleep behavior disorder, which involves physically acting out dreams.
The existence of these prediagnostic symptoms suggests that damage to dopamine-producing nerve cells begins long before the person experiences trouble with movement.
A new study spearheaded by researchers from the La Jolla Institute for Immunology , in California adds to evidence that the immune system may be responsible for the damage to nerve cells.
Limitations Of The Study
The authors report that one of the limitations of their study was that they did not have information about how far the disease had progressed in patients.
In addition, they studied T cells in the bloodstream and did not have direct evidence that these cells actually target neurons in the brains of people with Parkinsons.
In the future, they plan to study post-mortem brain samples to discover whether this is the case.
The scientists hope that the genetic signature of Parkinsons in memory T cells could one day help doctors identify people who will develop the disease.
Their discovery could also inspire new treatments that target the proteins that these particular genes make.
Now that we can see what these T cells are doing, we think intervening with antibody therapies could have an impact on the disease progression, especially early on, says Prof. Sette.
A growing number of researchers are becoming interested in the potential of targeting the immune system in the development of treatments that may slow the loss of cells in Parkinsons something that no treatment, to date, had been shown to do, said Professor David Dexter, Ph.D., associate director of research at Parkinsons U.K.
This research helps increase our understanding of which targets could provide an opportunity to develop treatments that address the underlying causes of the condition, he added.
Vps35 Mutations In Pd
RAB10, a member of the small RAB GTPase family, is a known substrate of LRRK2 and the D620N mutation in Vps35 leads to LRRK2-dependent increases in RAB10 phosphorylation in the spleens of Vps35D620N knock-in mice relative to non-transgenic littermates. Furthermore, neutrophils and monocytes from patients with PD who carry the D620N mutation exhibited this same increase in LRRK2-mediated RAB10 phosphorylation relative to idiopathic PD and healthy controls. Such data support the idea that the D620N mutation results in a toxic gain-of-function in an upstream regulator of the LRRK2 kinase pathway. How this interaction and PD-associated mutations affect neutrophil and monocyte function has yet to be elucidated.
Also Check: Can Parkinson’s Start In The Legs
Clinical Features And Autoimmunity In Pd
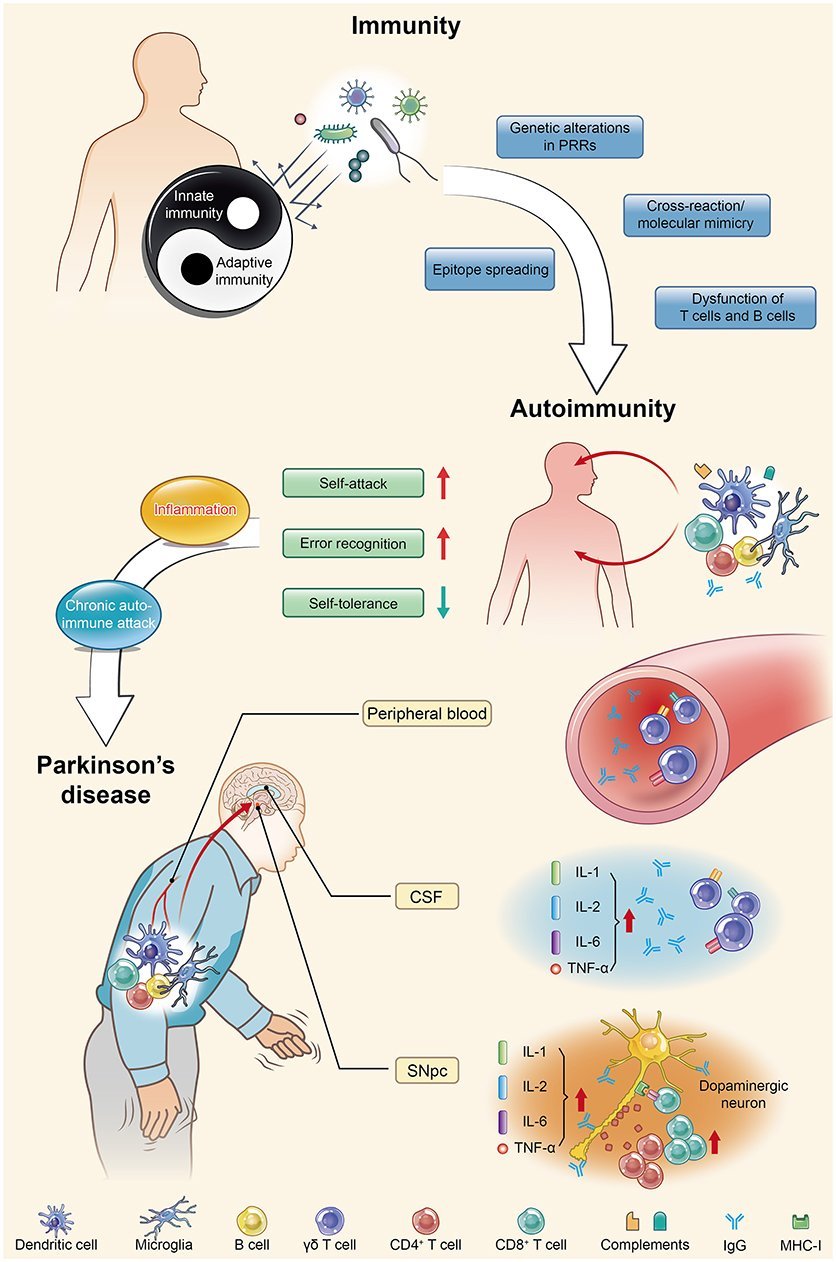
-Synuclein participates in autoimmunity and is involved in the pathological progression of PD. -Syn, as the main disease-causing protein, first appears in the gut and is related to gut dysbiosis, which disturbs the intestinal immune system, leading to one of the main non-motor symptoms of PD: constipation. Then, this protein transmits to the dorsal motor nucleus through the vagus nerve and acts as a self-antigen targeted by effector T cells, B cells, and microglia. This autoimmunity attack finally results in the damage and death of DNs. SIBO, small intestinal bacterial overgrowth.
Other Causes Of Parkinsonism
Parkinsonism is the umbrella term used to describe the symptoms of tremors, muscle rigidity and slowness of movement.
Parkinsons disease is the most common type of parkinsonism, but there are also some rarer types where a specific cause can be identified.
These include parkinsonism caused by:
- medication where symptoms develop after taking certain medications, such as some types of antipsychotic medication, and usually improve once the medication is stopped
- other progressive brain conditions such as progressive supranuclear palsy, multiple systems atrophy and corticobasal degeneration
- cerebrovascular disease where a series of small strokes cause several parts of the brain to die
You can read more about parkinsonism on the Parkinsons UK website.
Page last reviewed: 30 April 2019 Next review due: 30 April 2022
You May Like: Treatment Of Tremor In Parkinson’s Disease
Genetic Regulation Of Autoimmunity In Pd
In addition to these observations, DJ-1 has also been reported to affect the development of natural Tregs and induced Tregs . Mature Tregs with normal function, which modulate not only adaptive immunity but also innate immunity, are pivotal for maintaining thymic function, peripheral immune self-tolerance and immune system homeostasis. nTregs are generated in the thymus, while iTregs are derived from naïve CD4+ T cells encountering antigens in the peripheral organs. Both cell types are generally immunosuppressive through the suppression or downregulation of effector T cell proliferation . Their self-check function successfully prevents excessive effector cell reactions. On the other hand, the abnormal proliferation of both types of Tregs leads to the failure of self-/non-self-discrimination, resulting in autoimmune disease . Evidence reported by Singh et al. has demonstrated that DJ-1, one of the most classical key players responsible for PD pathogenesis, is strongly linked with neuroimmunology and multiple autoimmune responses in PD . In addition, DJ-1-deficient animal models have shown compromised iTreg induction, cell cycle progression, and cell survival and proliferation. DJ-1/ iTregs are more proliferative, more susceptible to cell death signals and deficient in cell division compared with wild type counterparts, as analyzed by flow cytometry and Western blotting.
Implications For Diagnosis And Therapeutics
Understanding the extent of the role of the immune response in the pathogenesis of PD opens up new avenues of diagnosis and treatment for patients. Identifying people who are carriers of HLA alleles that place them at risk for -syn-specific T cells to be monitored can help early diagnosis and treatment of PD. In addition, -syn-specific T cells could be use as early biomarkers of the disease, identifying autoimmunity to self proteins prior to the onset of motor symptoms. Large-scale, longitudinal studies monitoring -syn reactivity and the development of PD would need to be conducted before establishing T cells as PD biomarkers.
Currently, new treatment avenues targeting the immune system are being tested on PD patients. Sargramostim is a human recombinant granulocyte-macrophage colony-stimulating factor approved by the Food and Drug Administration for the recovery of patients receiving bone marrow transplantation and cancer therapies . It functions by promoting myeloid recovery and inducing Treg responses . In a preliminary randomized, double-blind phase 1 clinical trial, Sargramostim-treated patients showed modest improvements after 6 and 8 weeks of treatment and increases in Treg numbers and function compared to PD patients receiving placebo . Further clinical investigation will shed light on the potential of immunomodulatory drugs for treatment of PD.
You May Like: Glasses For Parkinson’s Disease
Parkinsons An Autoimmune Disease
Discovering the cause or etiology of diseases such as Parkinsons is essential to finding a treatment to prevent it. There are more and more advances in this field. And one of the latest ones is that Parkinsons could be an autoimmune disease.
Índice
Autoimmune Targeting Of Mitochondria As A New Biomarker For Parkinsons Disease
Study Rationale:Parkinsons disease is a complex, age-related disorder for which there are currently no biomarkers available to diagnose or predict the onset of disease. However, growing evidence suggests that brain inflammation and autoimmunity are associated with PD and could thus serve as clinically relevant biomarkers. We recently found that PINK1 and Parkin, proteins that are disabled in early-onset PD, actively repress the processes that lead to the targeting of cellular mitochondria by the immune system. When PINK1 and Parkin are absent, immune cells inappropriately recognize and destroy these vital cell structures damage that is associated with Parkinson’s disease.
Impact on Diagnosis/Treatment of Parkinsons Disease: The ability to monitor the engagement of mitochondria-specific autoimmune mechanisms will open new avenues for the treatment of PD, which had not previously been linked to autoimmunity. Furthermore, our results hold the promise to better categorize people with PD and identify those that will most likely benefit from treatments.
Next Steps for Development:We will recruit independent cohorts to validate the autoimmune signature we identify and to evaluate whether our results can be used as a biomarker to reliably identify individuals with Parkinson’s.
Don’t Miss: What Medication Is Used To Treat Parkinson’s Disease
Box 1 Pd Genetics Indicate A Role Of The Immune System In Pathogenesis
A brief overview of the biological relevance of genetic variants that modulate the risk of idiopathic Parkinson disease is provided below their link to immune mechanisms is described in more detail in the main text.
GBA, PRKNandPINK1, SNCA, VPS35, andPARK7
The GBA gene encodes for the lysosomal enzyme glucocerebrosidase that mediates conversion of glucocerebroside to glucose and ceramide. Heterozygous GBA mutation carriers have an increased risk of developing PD GBA mutations are now identified as the most common genetic risk factor for PD. The PRKN and PINK1 genes are two of the most well-characterized autosomal recessive genes associated with PD,. Five missense point mutations, A30P, E46K, H50Q, G51D and A53T, in the -synuclein encoding gene SNCA may cause autosomal dominant PD. Moreover, duplication and triplication of the -synuclein gene locus has been described in familial and sporadic PD and in dementia with Lewy bodies,,,. Heterozygous changes in the gene encoding the VPS35 cargo-binding component of the retromer complex are associated with late-onset PD,, with D620N being the only mutation characterized to date,. Mutations in the PARK7 gene, which encodes DJ1, cause autosomal-recessive PD. DJ1 is a multifunctional redox-sensitive protein that may mediate neuroprotection by dampening mitochondrial oxidative stress and regulating anti-apoptotic and anti-oxidative gene expression,.
BST1, SYT11, TMEM175andGRN
Pesticides And Pd Risk
Pesticides and occupational exposure to chemicals can increase the risk of PD,. Paraquat is the chemical most linked to risk, and even rotenone, a natural plant-derived pesticide used by home gardeners, has been associated with disease. Both compounds inhibit mitochondrial respiration, which could impact an already dysfunctional endolysosomal pathway in individuals with particular genetic mutations,. In addition to paraquat and rotenone, exposure to the toxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine , after its accidental discovery as an agent that caused dopaminergic neuronal loss in humans during recreational drug use, has become one of the main methods to induce dopaminergic neuronal loss and degeneration in animal models,,. Studies have shown that paraquat, rotenone and MPTP all induce both central and peripheral inflammation and oxidative stress,,,,.
Also Check: Latest Treatment For Parkinson’s
Is There A Cure For Parkinsons
Theres currently no cure for Parkinsons, a disease that is chronic and worsens over time. More than 50,000 new cases are reported in the United States each year. But there may be even more, since Parkinsons is often misdiagnosed.
Its reported that Parkinsons complications was the
Complications from Parkinsons can greatly reduce quality of life and prognosis. For example, individuals with Parkinsons can experience dangerous falls, as well as blood clots in the lungs and legs. These complications can be fatal.
Proper treatment improves your prognosis, and it increases life expectancy.
It may not be possible to slow the progression of Parkinsons, but you can work to overcome the obstacles and complications to have a better quality of life for as long as possible.
Parkinsons disease is not fatal. However, Parkinsons-related complications can shorten the lifespan of people diagnosed with the disease.
Having Parkinsons increases a persons risk for potentially life threatening complications, like experiencing:
- falls
Parkinsons often causes problems with daily activities. But very simple exercises and stretches may help you move around and walk more safely.
Is Parkinsons An Autoimmune Disease What Does The Current Research Say
Published Apr 11, 2021 By Courtney Johnson
Parkinsons disease is a long-term neurodegenerative disease that affects movement. The disease, which affects around half a million Americans, currently has no cure.
In honor of World Parkinsons Day, we wanted to shine a light on groundbreaking research that has the potential to one day lead to a cure!
What does recent research say about Parkinsons disease? Is Parkinsons an autoimmune disease? What could this mean for the future of Parkinsons treatments?
We break it down in our article!
You May Like: Treating Hallucinations In Parkinson’s Disease
Pitfalls Limitations And Alternative Interpretations
Given that the Swedish health care system typically offers everyone a life-long follow-up, it is unlikely that RA remains undiagnosed in RA-affected individuals or that PD remains undiagnosed in PD-affected individuals. It is impossible to fully exclude that the association we detected was caused by a confounder, however, we took great care to match PD cases and controls in order to make the groups as similar as possible. A potential confounder that we did not account for could be, for example, educational attainment. Shorter education is associated with increased prevalence of RA in Sweden . Since it has conversely been shown that men attaining higher IQ scores during military conscription in Sweden exhibit higher risk of developing PD , education level is potentially a confounder that could influence the risk for both diseases.
It is important to highlight that our working dataset was limited to only individuals who were first-degree relatives of a person diagnosed with diabetes mellitus or celiac disease. While this dataset was limited, it still allowed us to include 3.6 million individuals, or more than 20% of the entire population followed in the registry. We took precautions to ensure that PD cases and controls were also matched based on the exact type of a relative who had PD and RA. The matching was intended to prevent potential fictitious associations that could arise, due to unequal distribution of family-size affecting factors between PD case and control groups.
Immunotherapy To Treat Parkinsons
Researchers have studied how they may use the immune system to treat PD in the future in an approach called immunotherapy, although this is still experimental. Scientists hope to one day be able to slow the disease progression.
Scientists have investigated sargramostim , a drug that works by stimulating immune cells, as a potential treatment for PD. Although approved by the Food and Drug Administration for people recovering from cancer therapies and bone marrow transplants, sargramostim has shown moderate improvement in studies of the T-cell response of people with PD.
Researchers are also now discussing using monoclonal antibody therapy to target alpha-synuclein and possibly slow the progress of Parkinsons.
In another study, researchers in neurology looked at the link between medications that suppress the immune system and the risk of PD. They found evidence that using corticosteroids and other immune system blockers may help lower the chance of developing Parkinsons.
Despite these promising initial findings, more research is needed to understand the connection between PD and autoimmunity. This information will provide better ways to diagnose and treat PD going forward.
Recommended Reading: Parkinson’s Foundation San Diego
T Cells In The Midbrain Of Pd Patients
Perhaps as a result of peripheral inflammation, changes in lymphocyte subtype populations, and BBB breakdown, T cells can infiltrate the affected brain regions of PD patients. First reported by the McGeers in 1988, CD3+ cells, a marker for T cells, were detected within the CNS of PD brains . Brochard et al. showed that both CD4+ and CD8+ T cells, but not B and natural killer cells, infiltrated the SN of PD patients and were present at much far greater levels than in healthy controls. These T cells were located near blood vessels and neuromelanin-containing dopaminergic neurons . The presence of T cells in the region affected in the disease suggests a targeted extravasation, rather than a random consequence of increased BBB permeability by peripheral inflammation. If T cells that had escaped self-tolerance circulate in the blood of PD patients, it is plausible that they could infiltrate into the brain permitted by a leaky BBB. The causal role of infiltrating T cells is further elucidated in studies from mouse models of PD.
Also Check: Does Weed Help With Parkinsons
New Research Gives Further Evidence That Autoimmunity Plays A Role In Parkinsons Disease
Member for
ScienMag
A new study co-led by scientists at the La Jolla Institute for Immunology adds increasing evidence that Parkinsons disease is partly an autoimmune disease. In fact, the researchers report that signs of autoimmunity can appear in Parkinsons disease patients years before their official diagnosis. The research could make it possible to someday detect Parkinsons disease before the onset of debilitating motor symptomsand potentially intervene with therapies to slow the disease progression. The Parkinsons Foundation supports this research.
Don’t Miss: Will There Ever Be A Cure For Parkinson’s Disease
Best Evidence Yet That Parkinsons Could Be Autoimmune Disease
Parkinsons begins with abnormal clumping of a protein called synuclein in the brain
R. Bick, B. Poindexter, UT Medical School/SPL
EVIDENCE that Parkinsons disease may be an autoimmune disorder could lead to new ways to treat the illness.
Parkinsons begins with abnormal clumping of a protein called synuclein in the brain. Neighbouring dopamine-producing neurons then die, causing tremors and difficulty moving.
The prevailing wisdom has been that these neurons die from a toxic reaction to synuclein deposits. However, Parkinsons has been linked to some gene variants that affect how the immune system works, leading to an alternative theory that synuclein causes Parkinsons by triggering the immune system to attack the brain.
An argument against this theory has been that brain cells are safe from immune system attack, because most neurons dont have antigens the markers immune cells use to recognise a target. But by studying postmortem brain tissue samples, David Sulzer at Columbia University and his team have discovered that dopamine-producing neurons do display antigens. The team has now conducted blood tests to reveal that people with Parkinsons show an immune response to these antigens, while people who dont have the condition do not .
This article appeared in print under the headline Parkinsons may be the result of immune attack
More on these topics: