Diagnosing And Treating Parkinsons Disease
The diagnosis of Parkinsons disease is largely based upon the type of symptoms that the patient experiences. When someone has symptoms such as tremors or shaking of arms or legs while at rest, muscle stiffness or slow movements, Parkinsons disease must be a consideration, particularly if the individual is at a typical age for the onset of the disorder. Not all patients have every symptom, and often the symptoms start on one side of the body and then progress over time to include the other side. A good response to a trial of Parkinsons disease medication also helps to add confidence to the diagnosis.
The symptoms of Parkinsons disease can be similar to the symptoms of other conditions, and it is frequently misdiagnosed. Skilled doctors who specialize in the treatment of Parkinsons disease are the best practitioners to see for an accurate diagnosis.
The diagnostic process begins with a full medical history and neurological exam, testing movement, strength, coordination, balance, and reflexes. A doctor will often order additional tests to make sure that there are no other conditions present that could explain the patients symptoms. These tests may include an MRI of the brain and/or spine, or diagnostic tests of the electrical responses of muscles and nerves. In Parkinsons disease, these are usually normal and are performed to make sure that there are not problems other than Parkinsons disease that could explain symptoms.
Treatment Options
What Doctors Look For When Diagnosing Parkinsons
Certain physical signs and symptoms noticed by the patient or his or her loved ones are usually what prompt a person to see the doctor. These are the symptoms most often noticed by patients or their families:
-
Shaking or tremor: Called resting tremor, a trembling of a hand or foot that happens when the patient is at rest and typically stops when he or she is active or moving
-
Bradykinesia: Slowness of movement in the limbs, face, walking or overall body
-
Rigidity: Stiffness in the arms, legs or trunk
-
Posture instability: Trouble with balance and possible falls
Once the patient is at the doctors office, the physician:
-
Takes a medical history and does a physical examination.
-
Asks about current and past medications. Some medications may cause symptoms that mimic Parkinsons disease.
-
Performs a neurological examination, testing agility, muscle tone, gait and balance.
What Can You Detect With A Parkinsons Mri
Generally, you can receive a Parkinsons diagnosis in a clinical setting, but an MRI can help to assess various aspects of the disease and its progress. In particular, a Parkinsons MRI can do the following for patients who have or are suspected to have Parkinsons disease:
- Evaluate tissue loss and how the brain is atrophying
- Check for changes to the basal ganglia region of the brain
- Find out if there are abnormal iron deposits in the basal ganglia or brainstem
- Look at changes to white matter
- Examine the diffusion of restricted tissues in acute infarction and neurodegenerative diseases
- Help to diagnose atypical parkinsonism
- Exclude treatable causes of parkinsonism such as normal pressure hydrocephalus
Read Also: Seroquel And Parkinson’s Disease
Preparing For A Parkinsons Mri
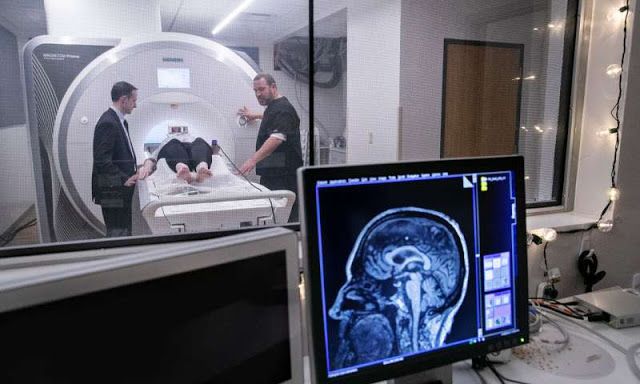
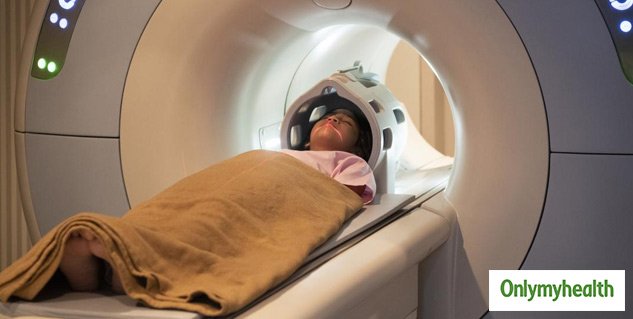
A Parkinsons MRI is completely painless, but you do have to lie still while being scanned. Some patients feel claustrophobic in this situation. If youre worried about that, talk with your doctor about the possibility of having an anti-anxiety medication before the procedure.
On the day of the appointment, follow any instructions provided to you by your doctor. Remove metal jewelry and dont wear make-up as that can also have metal in it. If you are in the advanced stages of Parkinsons or if you are taking a sedative, you should arrange transportation to and from the appointment.
Resting State Functional Mri
Resting state fMRI detects blood-oxygen-level-dependent low-frequency spontaneous fluctuations across the brain while an individual is at rest, and can be used to study functional connectivity within and across spatially distributed brain networks. The most validated analytical approach examines the resting state fMRI Parkinsons Disease Related Pattern , which was initially characterized using PET . Similar to PET, there are significant increases in fPDRP expression in PD relative to control subjects , however, further research is necessary to evaluate its utility as a diagnostic and monitoring biomarker. At this time, there are numerous additional analytical approaches taken to examine rs-fMRI in PD, that suggest widespread dysfunction in PD, but also numerous inconsistencies based on recent reviews . This is partially related to the impact of various preprocessing approaches and observations showing rs-fMRI varies as a function of medication status . Further, networks appear to dynamically adapt to disease progression and functional brain circuitry dysfunction may differ dependent on the nature of the motor symptoms . Indeed, investigation of more targeted analytic approaches will be necessary to identify potential diagnostic and monitoring biomarkers, which is discussed further in the next section.
Don’t Miss: Parkinson’s Disease Continuing Education Physical Therapy
Mri In Parkinson’s Testing
One of the more common tests done during a neurologic workup is an MRI scan and one may think that in the investigation of a disease that affects the brain such as Parkinsons, this imaging test would be a necessity. In the context of Parkinsons disease, however, an MRI is not particularly helpful. It looks at the structure of the brain which, for all intents and purposes, appears normal in this disease. An MRI may, however, be indicated when symptoms appear in younger people or if the clinical picture or the progression of symptoms is not typical for Parkinsons. In these situations, MRI can be used to rule out other disorders such as stroke, tumors, hydrocephalus , and Wilsons Disease .
Mri And Parkinsons Treatment
Tremors in hand or shaky legs are the first and most common signs of Parkinsons disease. Ignoring the initial signs make things worse and the problems get complicated as time passes by. Theres a hope given by a recent research. As per the findings published in the journal Brain suggests that theres a new MRI technique which claims to detect this disorder and treat without surgery.
MRI technology is used to closely monitor a part of the brain. This technique can also help in targeting the part of the brain which causes tremors and is linked to Parkinsons. This discovery can help in treating the problem without surgery and side-effects.
Also Read: Know How Living Near Highway Causes Dementia and Other Problems
Dr. Bhavya R. Shah is an M.D. and Assistant Professor of Radiology and Neurological Surgery at Peter ODonnell Jr. Brain Institute, UT Southwestern, Dallas, Texas. Shah who lead this research and said: “The benefit for patients is that we will be better able to target the brain structures than we want. And because were not hitting the wrong target, well have fewer adverse effects.”
Without opening the skull and conducting the surgery, Parkinsons patient can be given the treatment. However, this still needs to be tested thoroughly before it can be implemented to treat the patients.
Read More in Latest Health News
Read Also: Very Early Parkinson’s Symptoms
What Is Parkinsons Disease
Parkinsons disease is a chronic neurological condition. It is progressive and symptoms worsen over time. It is named after Dr James Parkinson who first described the condition in 1817.
People with Parkinsons disease experience a loss of nerve cells in the part of their brains responsible for controlling voluntary movements. This part of the brain is called the substantia nigra . The nerve cells in the substantia nigra usually produce a chemical called dopamine which helps transmit messages from the brain to the rest of the body via the central nervous system . As these cells are lost, people with Parkinsons disease experience a loss of dopamine and the messages controlling movement stop being transmitted efficiently.
Parkinsons disease is more common as people get older but it can affect younger adults. Men tend to be affected in slightly higher numbers than women.
Tests To Rule Out Other Conditions
Blood tests can help rule out other possible causes of the symptoms, such as abnormal thyroid hormone levels or liver damage.
An MRI or CT scan can check for signs of a stroke or brain tumor, which may cause similar symptoms.
Hydrocephalus due to atrophy can occur with some types of dementia and would be visible with one of these imaging tests. If the person has neurologic symptoms but a normal scan result, Parkinsons disease may be present.
The doctor a lumbar puncture to rule out inflammation or a brain infection.
Recommended Reading: Medicine For Parkinson’s Disease In India
Mri Changes In Patients With Pdnd And Pdd
Patients with PDD versus controls
Patients with PDD had reductions in grey matter concentration in the limbic lobes and both temporal lobes, compared with the controls. On the left side, there was also reduced grey matter density in the frontal lobe, limbic lobe and brain stem red nucleus. On the right side, there was reduced grey matter density in the middle occipital gyrus . When we included age, sex and Parkinson’s disease duration as covariates in ANCOVA, the results were unchanged. We found no areas where controls had more grey matter atrophy than patients with PDD. Using an SVC and correcting for multiple comparisons, the bilateral reduction in grey matter in the middle temporal gyrus and amygdala, and also in the left brain stem red nucleus, was significant at p FWE < 0.05.
Patients with PDD compared with those with PDND
In patients with PDD, there were areas of marked grey matter reduction in the frontal lobes, limbic, parietal and temporal lobes bilaterally. On the right side, there was also reduced grey matter density in the pulvinar of the thalamus . The areas surviving SVC with correction for multiple comparisons using FWE are marked with an asterisk in the table. The results did not change when age, sex and duration of Parkinson’s disease were included as covariates in ANCOVA.
There were no areas where patients with PDND had more grey matter atrophy than patients with PDD.
Patients with PDND compared with normal controls
Mri Brain Scans Detect People With Early Parkinson’s
Oxford University researchers have developed a simple and quick MRI technique that offers promise for early diagnosis of Parkinson’s disease.
The new MRI approach can detect people who have early-stage Parkinson’s disease with 85% accuracy, according to research published in Neurology, the medical journal of the American Academy of Neurology.
‘At the moment we have no way to predict who is at risk of Parkinson’s disease in the vast majority of cases,’ says Dr Clare Mackay of the Department of Psychiatry at Oxford University, one of the joint lead researchers. ‘We are excited that this MRI technique might prove to be a good marker for the earliest signs of Parkinson’s. The results are very promising.’
Claire Bale, research communications manager at Parkinson’s UK, which funded the work, explains: ‘This new research takes us one step closer to diagnosing Parkinson’s at a much earlier stage one of the biggest challenges facing research into the condition. By using a new, simple scanning technique the team at Oxford University have been able to study levels of activity in the brain which may suggest that Parkinson’s is present. One person every hour is diagnosed with Parkinson’s in the UK, and we hope that the researchers are able to continue to refine their test so that it can one day be part of clinical practice.’
We think that our MRI test will be relevant for diagnosis of Parkinson’s
Dr Michele Hu
Read Also: Development Of Parkinson’s Disease
Imaging Studies Can Differentiate Parkinsons From Other Causes Of Parkinsonism
Catherine L. Gallagher, MD
Although Parkinsons disease remains a clinical diagnosis, imaging studies are an important ancillary test for differential diagnosis of movement disorders. Imaging studies may be used to rule out structural and other causes of parkinsonian symptoms. Single-photon emission computed tomography scans using labeled tracers for dopamine transporters can also be used to confirm parkinsonism or differentiate PD from secondary causes of parkinsonian motor symptoms. Finally, imaging studies are being used in research to better understand the pathophysiology of PD and elucidate causative mechanisms that could be therapeutic targets in the future.
Is The Imaging Metric Appropriate For The Question Being Asked
Neuroanatomy Relevant to Parkinsons Disease
A. Braak staging of -synuclein pathology. At death, PD patients exhibit the following stages of -Syn pathology: stage I olfactory bulb only , Stage IIa brainstem predominant , stage IIb limbic predominant , stage III brainstem and limbic and stage IV neocortical . While not all patients with pathology will exhibit clinical symptoms , the progression of neuropathology generally corresponds to the progression of both motor and non-motor symptoms . B. The SN is subdivided into the ventral pars reticulata and the dorsal pars compacta , the latter is composed of dopaminergic neurons. The SNc is further divided into the dorsal and ventral tier, with the loss of dopaminergic neurons occurring first in the caudal and ventrolateral tier . Within A9, there are five nigrosomes , with N1 exhibiting the earliest loss of dopaminergic neurons . Dopaminergic neuronal loss typically spreads to neighboring groups from the N1 in PD . C. Fronto-subcortical loops comprise the motor, associative, and limbic domains, which respectively transit through the posterior, anterior, and ventral striatum, thus segregated functionally and anatomically. GPe = globus pallidus externa. GPi = globus pallidus interna. STN = subthalamic nucleus. SNc = substantia nigra pars compacta. SNr = substantia nigra pars reticulata. Adapted with permission from: .
Also Check: How Long Does Parkinson’s Last
What Tests Diagnose Parkinson’s Disease
There currently are no tests that can definitively diagnose Parkinsons Disease. A diagnosis is based on the clinical findings of your physician in combination with your report on the symptoms you are experiencing.
In situations where an older person presents with the typical features of Parkinsons and they are responsive to dopamine replacement therapy, there is unlikely to be any benefit to further investigation or imaging.
What Happens At The Exam
If your doctor thinks you might have Parkinsonâs disease, theyll recommend that you see a specialist who works with nervous system issues, called a neurologist. One whoâs also trained in movement disorders, like Parkinsonâs, may be able to make the right diagnosis faster.
Your neurologist will probably want to see how well your arms and legs move and check your muscle tone and balance.
They may ask you to get out of a chair without using your arms for support, for example. They also may ask a few questions:
- What other medical conditions do you have now or have you had in the past?
- What medications do you take?
- Has your handwriting gotten smaller?
- Do you have trouble with buttons or getting dressed?
- Do your feet feel âstuckâ to the floor when you try to walk or turn?
- Do people say your voice is softer or your speech is slurred?
Tell your doctor if youâve noticed a change in your sense of smell or you have trouble with sleep, memory, or mood.
Parkinsonâs disease can look different from person to person. Many people have some symptoms and not others.
You May Like: What Are The Symptoms Of Early Onset Parkinson’s
If Its Not Parkinsons Disease What Could It Be
Here are some possibilities:
Side effects of medication: Certain drugs used for mental illnesses like psychosis or major depression can bring on symptoms like the ones caused by Parkinsonâs disease. Anti-nausea drugs can, too, but they typically happen on both sides of your body at the same time. They usually go away a few weeks after you stop taking the medication.
Essential tremor: This is a common movement disorder that causes shaking, most often in your hands or arms. Itâs more noticeable when youâre using them, like when you eat or write. Tremors caused by Parkinsonâs disease usually happen when youâre not moving.
Progressive supranuclear palsy: People with this rare disease can have problems with balance, which may cause them to fall a lot. They donât tend to have tremors, but they do have blurry vision and issues with eye movement. These symptoms usually get worse faster than with Parkinson’s disease.
Normal pressure hydrocephalus : This happens when a certain kind of fluid builds up in your brain and causes pressure. People with NPH usually have trouble walking, a loss of bladder control, and dementia.
When Brain Mri Is Recommended To Help Diagnose Parkinsonism
Differentiating atypical parkinsonism from Parkinsons disease can be a challenge in patients presenting with symptoms in early disease stages. A diagnosis cannot be made from a brain magnetic resonance imaging scan, but brain MRI can be of added value when there is uncertainty about the clinical diagnosis.
The appropriateness of and the added diagnostic value of a brain MRI scan in the work-up of parkinsonism is described in a newly published article in the Journal of Parkinsons Disease. Lead author Frederick J.A. Meijer, MD, PhD, a neuroradiologist in the department of radiology and nuclear medicine at Radboud University Medical Center in Nijmegen, The Netherlands, offers advice on the scanning protocol to use, and also discusses its diagnostic value with respect to specific abnormalities that can be seen.
The authors of the article, who also include neurologists from the Radboud University Medical Center and Donders Institute for Brain, Cognition and Behavior, conducted a 3-year long prospective study on the contribution of routine brain MRI to the differential diagnosis of parkinsonism.1 Based on this research, the authors refuted clinical guidelines recommending standard use of cerebral MRI for all patients presenting with parkinsonism.
3T brain MRI including DTI tractography in a patient presenting with parkinsonism.
Read Also: Botox For Drooling In Parkinson’s
Response To Parkinsons Drugs
After examining you, and depending on the severity of your symptoms, your specialist may suggest you take medication for Parkinsons. If your symptoms improve after taking Parkinsons medication for a few weeks or months, your specialist may confirm a Parkinsons diagnosis. However, some people with other forms of parkinsonism will also respond well to these drugs.
Your specialist may suggest you have a scan to help make a diagnosis. However, scans alone cant make a definite diagnosis of Parkinsons, so they are not commonly used.