Onset Of Als And Parkinsons
There are several different variants of ALS but it generally affects people between the age of 40 and 70. Juvenile onset ALS, however, can start in childhood or typically before the age of 25, although this form of ALS is particularly rare. The onset of ALS is estimated to be 20% more common in men compared with women and in 10% of cases there is likely to be a genetic component.
Parkinsons disease is usually diagnosed in people over the age of 60, though a small percentage exhibit the symptoms before the age of 50.
Once again, men are more likely to develop Parkinsons than women.
Myth : Parkinsons Medications Cause Symptoms
Fact: Even though the myth that Parkinsons disease medicines are toxic and make the condition progress faster was completely debunked, it persists. Levodopa is the main drug therapy for Parkinsons disease. Its a potent drug that helps patients with motor symptoms. But many people got the idea that over time, it makes the disease progress faster. The myth was that levodopa is somehow toxic and is somehow making the Parkinsons progression faster, hurting patients.
This misconception was debunked decades ago with a large clinical trial, where it was found that people exposed to levodopa versus a placebo werent worse. In fact, they were better at the end of the study.
Its true that levodopa isnt a cure as yet, there is no cure for Parkinsons disease but its not toxic.
What Is Parkinsons
Parkinsons disease is a movement disorder characterized by a decline in the dopamine level of the brain. The cause of this condition still remains controversial. The risk of Parkinsons disease significantly increases with advanced age. A familial inheritance of the disease has not yet been identified.
Recommended Reading: Activities For Parkinson’s Patients
How Is It Treated
Currently, there are no treatments to delay the progressive neurodegeneration of MSA, and there is no cure. There are treatments to help people cope with the symptoms of MSA.
In some individuals, levodopa may improve motor function however, the benefit may not continue as the disease progresses.
The fainting and lightheadedness from orthostatic hypotension may be treated with simple interventions such as wearing compression stockings, adding extra salt and/or water to the diet, and avoiding heavy meals. The drugs fludrocortisone and midodrine sometimes are prescribed. In 2014, the U.S. Food and Drug Administration approved the medication droxidopa for the treatment of orthostatic hypotension seen in MSA. Dihydroxyphenylserine helps to replace chemical signals called neurotransmitters which are decreased in the autonomic nervous system in MSA. Some medications used to treat orthostatic hypotension can be associated with high blood pressure when lying down, so affected individuals may be advised to sleep with the head of the bed tilted up.
Bladder control problems are treated according to the nature of the problem. Anticholinergic drugs, such as oxybutynin or tolteridine, may help reduce the sudden urge to urinate.
Fixed abnormal muscle postures may be controlled with injections of botulinum toxin.
Sleep problems such as REM sleep behavior disorder can be treated with medicines including clonazepam, melatonin, or some antidepressants.
The Impact Of Remotely Supervised Tdcs On Parkinsons Disease And Other Neurological Conditions
NYU Langone researchers are also looking into the benefits of RS-tDCS for other neurological conditions in several open-label studies.
A study conducted in collaboration with researchers at the , slated for publication in the Journal of NeuroEngineering and Rehabilitation, demonstrated the applicability of this methodology in Parkinsons disease, with improvements in fatigue and cognition similar to those seen in MS. Further, as published in 2018 in the Journal of Clinical Neuroscience, patients with moderate Parkinsons disease experienced a notable reduction in symptoms from using RS-tDCS in combination with cognitive training.
The use of telemedicine to supervise at-home tDCS will allow us to reach more patients and also to bypass common obstacles that prevent populations with mobility impairment or other accessibility barriers from participating in clinical trials and receiving health services, says Milton C. Biagioni, MD, assistant professor of neurology and coinvestigator on the study. This is the first time an RS-tDCS protocol has been designed for and tested in these patients.
According to study coinvestigator Milton C. Biagioni, MD, telemedicine allows people who have mobility impairments to access healthcare services and clinical trials.
Although studies currently focus on patients with moderate Parkinsons disease, researchers at the Fresco Institute anticipate expanding these investigations in the near future to include patients with advanced disease.
Recommended Reading: Ohio Parkinson Foundation Northeast Region
Common Misdiagnosis: Multiple Sclerosis
One of the most common answers to the question was multiple sclerosis . Both diagnoses have an effect on the central nervous system. These diagnoses also frequently cause muscle spasms, balance changes, tremor, and impaired memory. However, these are two separate diagnoses.
One difference is that MS is often diagnosed when someone is in their 20s, while most people receive a PD diagnosis in their 60s. Also, MS is an autoimmune disease that over time causes nerve damage. Parkinsons affects the brain. The brain starts producing less and less dopamine, which is responsible for controlling movement.
Yes, with MS which I was worried about for years, but right now I do not know which one is worse. However, my meds are helping a lot. My new saying is It is what it is, aka just live on. My neurologist says that I have stage one mild Parkinsons disease.
My husband was diagnosed with MS back in 1993 when he had a mini stroke. He was diagnosed with Parkinsons in 2014.
Als Vs Parkinsons Disease: Symptoms
ALS is a neurodegenerative disease that affects the neurons in the body. It usually starts as a localized issue in an area like the hands or legs. A person diagnosed with ALS will often feel weakness in a certain part of the body. The disease destroys the neurons and begins to spread throughout the whole body causing damage elsewhere.
Parkinsons disease is also a neurodegenerative disorder but it actually affects a particular part of the brain rather than all neurons. It specifically attacks parts of the brain called the basal ganglia and the substantia nigra. Early symptoms may include difficulty sleeping and loss of sense of smell rather than loss of motor movement.
Don’t Miss: Laser Light For Parkinson’s Disease
Conditions And Diseases Related To Multiple Sclerosis
Defining and diagnosing multiple sclerosis can be difficult, for both physicians and patients, which is why a rigorous battery of tests is required to get a definitive answer. There are a number of other ailments that easily mimic at least some of the more common symptoms of this neurodegenerative disease, making it easy to mistake one for the other. Finding a diagnosis is often crucial to treating not only MS but other diseases and conditions that could be detrimental to your health that appear to be similar.
How Therapy Helps Ms And Parkinsons
While there are differences in Parkinsons and MS, physical, occupational and speech therapy can help both MS and PD patients improve their independence and safety, as well as achieve and maintain optimal function and cognition. Therapy can help prevent complications such as de-conditioning, muscle weakness from lack of mobility and muscle contractures related to spasticity. Training in energy conservation techniques and the use of adaptive tools and devices can help simplify everyday tasks. Therapists can even recommend strategic modifications to your home to ensure accessibility and safety even as the disease progresses.
Clinicians certified in LSVT ® and PWR! therapeutic programs can provide Parkinsons-specific exercises to target weight shifting, posture, trunk rotation and stepping strategies to overcome rigidity and slowness of movement. Education on specific exercises and strategies helps increase safety and slow the progression of the disease.
Also Check: Any New Treatment For Parkinson’s Disease
Treatment Of Rls In Pd
Regardless of the above discussion, it is clear that many people with PD have difficulty falling asleep because of annoying sensations in the legs accompanied by a sometimes unbearable sense of restlessness in the legs. For these people, taking dopamine agonists before bed can be helpful. Caution is in order, of course, because in some patients with PD, especially older or more advanced patients, these medications can cause confusion and hallucinations and are thus not well-tolerated. A long-acting levodopa formulation or medications such as gabapentin, gabapentin enacarbil and pregabalin can also be effective. Trying to address sleep issues such as RLS in patients who have sleep complaints can be an important aspect of maximizing therapy for PD.
Tips and Takeaways
What Is The Cause Of Multiple Sclerosis Parkinsons Alzheimers And Als
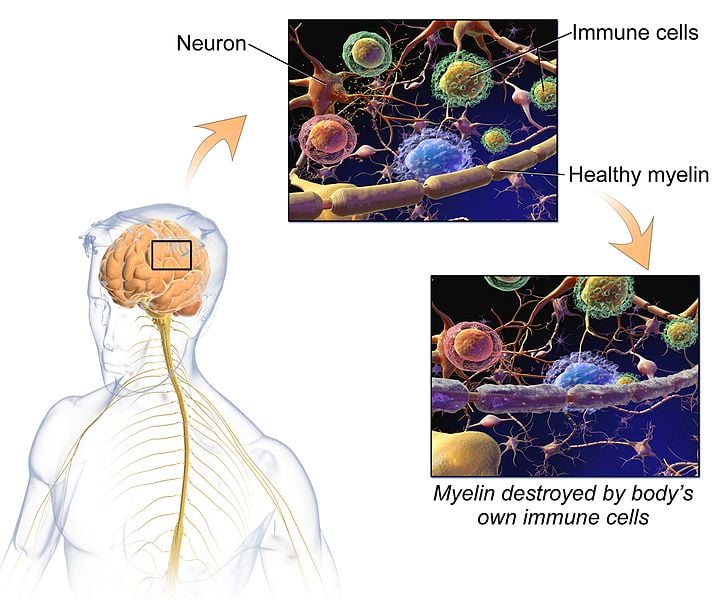
Despite the previous decades medical explanation, a description of the real Multiple Sclerosis, Alzheimers, Parkinsons and ALS occurs when the myelin sheath becomes sufficiently damaged from an over-acidic lifestyle and diet that causes decompensated acidosis of the interstitial fluids of the largest organ of the body called the Interstitium, as seen in the above picture.The myelin sheath is an electrically insulating phospholipid layer that surrounds the axons of many neurons. It is kind of like the rubber coating on a power cord that keeps the electricity traveling forward rather then shooting out in all directionsvirtually all over the place.
The main function of a myelin sheath is to increase the speed at which electrical impulses transmit and spread along the myelinated fibers. Along unmyelinated fibers impulses move continuously as waves. But in myelinated fibers, they hop or advance quickly by leaps. Myelin increases resistance across the cell membrane by a factor of 5,000 and decreases the ability to collect a charge of electricity by a factor of 50. Thus, the impulses keep moving and are not absorbed.
Myelination also helps prevent the electrical current from leaving the axon. When a peripheral fiber is severed, the myelin sheath provides a track along which regrowth can occur because it is essential that the body is able to repair itself.
Myelin is composed of about 80% lipid fat and about 20% protein.
Dont Miss: Zhichan Capsule
Also Check: Parkinson’s Disease Is Associated With
What Is Multiple Sclerosis
Multiple sclerosis is a progressive and debilitating disease of the central nervous system that disables the communication between the brain and other parts of the body. It involves an immune-mediated process in which an abnormal response of the bodys immune system is directed against the central nervous system.
Within the central nervous system , the immune system causes inflammation that damages myelinthe fatty substance that surrounds and insulates the nerve fibersas well as the nerve fibers themselves, and even the specialized cells that make myelin. When the nerve fibers are destroyed, messages within the CNS are altered or halted completely. Then, the damaged areas produce neurological symptoms that can vary among people in type and severity. These areas develop scar tissue, giving the disease its namemultiple areas of scarring or multiple sclerosis.
Know Your Specific Triggers
For instance, one of my biggest triggers is cervical tension especially when driving, traveling, or writing on the computer for hours. Another specific trigger for me and many others with migraines is skipping a meal which sometimes due to severe nausea or gastroparesis from PD. PD meds can make eating a difficult thing.
Don’t Miss: Parkinson’s And Swollen Feet And Ankles
Multiple Sclerosis Vs Parkinsons Disease: Risk Factors And Complications
Risk factors for multiple sclerosis include being female, having a family history of multiple sclerosis, having certain infections, being white of European descent, living furthest from the equator, living in temperate climate regions, already having an autoimmune disease, and smoking.
Complications resulting from multiple sclerosis include muscle stiffness and spasms, paralysis, problems with bladder, bowel, and sexual function, as well as forgetfulness, mood changes, depression, and epilepsy.
Risk factors for Parkinsons disease include being over the age of 50, being male, having a family history of Parkinsons disease, carrying gene variations, experiencing a head injury, being exposed to environmental toxins, and taking certain medications such as anti-anxiety medications or sleeping pills.
Complications associated with Parkinsons disease include difficulty thinking, depression, emotional changes, swallowing problems, sleep problems and disorders, bladder issues, constipation, changes in blood pressure, smell dysfunction, fatigue, pain, and sexual dysfunction.
What Makes Them Different
MS and Parkinsonâs have different causes. They usually start to affect you at different ages, too.
MS often affects people between ages 20 and 50, but children get it, too. Parkinsonâs usually starts at age 60 or older, but some younger adults get it.
MS is an autoimmune disease. That means your bodyâs immune system goes haywire for some reason. It attacks and destroys myelin. As myelin breaks down, your nerves and nerve fibers get frayed.
In Parkinsonâs, certain brain cells start to die off. Your brain makes less and less of a chemical called dopamine that helps control your movement. As your levels dip, you lose more of this control.
Some genes may put you at risk for Parkinsonâs, especially as you age. Thereâs a small chance that people who are exposed to toxic chemicals like pesticides or weed killers can get it, too.
These symptoms are more common if you have MS. They are not usually found in Parkinsonâs:
Also Check: Weight Loss In Late Stage Parkinson’s
Characteristics Of Restless Leg Syndrome
There are certain features of RLS that make it a unique and specific disorder.
Comparison Of Static Sway Performance Within One Group Between Different Tasks
Healthy adults showed a significant increase in sway area , velocity in ML direction , acceleration in ML direction and jerk in both AP and ML direction between the side-by-side and tandem stance . The sway area , velocity in ML direction , acceleration in ML direction and jerk in both AP and ML direction significantly increased between the semi-tandem and tandem stance .
Table 4. Significant changes of sway parameters between tasks.
MS patients showed a significant increase in sway velocity , acceleration in ML direction and jerk in ML and AP direction between side-by-side and tandem stance. Moreover, they showed a significant increase in sway acceleration in ML direction and jerk in ML direction between semi-tandem and tandem stance .
PD patients did not show a significant change in any of the sway parameters between the tasks .
Also Check: Link Between Sciatica And Parkinson’s
Is There A Connection Between The Two
Researchers have recently begun investigating a possible connection between MS and PD.
In a 2020 case study, researchers note a potential link between MS and PD. They find that people living with MS who have a mutated GBA1 gene may have a higher risk of developing PD. However, it is not clear why this is the case.
According to an earlier 2014 literature review , MS may affect a persons brain tissue and brain structure in a way that triggers the development of PD. Nonetheless, this connection is unlikely to be strong. The study authors note that there are only 34 reported cases of coexisting MS and PD, indicating that it is rare for people to develop both conditions.
More research is necessary to establish any firm connection between MS and PD.
Doctors treat both MS and PD using a combination of medications and therapies.
Treatment Approaches For The Neurological Progression Of Multiple Sclerosis And Parkinsons Disease
This course provides information on the specific neurological diseases processes of Multiple Sclerosis, Parkinsons and Muscular Dystrophy. Top neurologists specializing in Multiple Sclerosis will share information concerning the results from current research and clinical studies for patients with Multiple Sclerosis. Evidenced based research results will enable the clinician to understand the underlying mechanism of this disease process, diagnostic tools currently being utilized, medications and the importance of therapy and the future of MS treatments. Case presentations of patients diagnosed with Parkinsons, MS and Muscular Dystrophy will provide the clinician with the ability to observe common patterns seen with patients that are characteristic of each of these neurological diseases. The clinician will have the opportunity to get first hand information from the patients on their description of what it is like to be diagnosed with their neurological disease and the limitations and challenges they have encountered. Therapists will identify the appropriate assessment tools and measurement scales utilized for each disease and apply them to their rehab program. This will provide the clinician with the tools needed to effectively develop a program while maximizing the energy efficiency of their patients.
Instructor: Sara Koveleski Kraut, PT, DPT, NCS
Also Check: Multiple System Atrophy Vs Parkinson’s
How Do Treatments Differ
MS treatments can ease your symptoms during an attack or slow down the diseaseâs effects on your body.
Steroids like prednisone calm the inflammation that damages your nerves.
Plasma exchange is another therapy if steroids donât work. Your doctor will use a machine to remove the plasma portion of your blood. The plasma gets mixed with a protein solution and put back into your body.
Some people with both diseases who take anti-inflammatory medicines like steroids see their Parkinsonâs symptoms get better.
Disease-modifying treatments slow down MS nerve damage and disability. They include:
Medications to treat Parkinsonâs either raise your dopamine levels or offer a substitute. They can ease Parkinsonâs symptoms like tremors. Over time, they may become less effective.
Medicines used to treat Parkinsonâs include:
Deep-brain stimulation is another treatment for Parkinsonâs. A doctor places electrodes into your brain. They send out electric pulses that ease symptoms in your body.
Show Sources