Strengthening Exercises Or Stretching May Be Helpful
Imagine that the spine is like a telephone pole or the mast of a sailboat. If the pole is not exactly upright, even a slight tilt requires a great force to keep it from tilting further and falling. In the human body, this means that the lower back muscles are under great stress. It also means that the tension on the back bones is much increased as well. This worsens whatever problems, like arthritis, that are already present. The same process applies to the neck, although the forces are less great. Strengthening exercises or stretching may be helpful. Almost everyone over the age of 60 has arthritis in their spine. Luckily most dont have pain from it, but those who do will have it worsened by the spine curvature caused by the PD.
PD patients also frequently have an aching discomfort in their muscles, particularly in the thighs and shoulders. I think this is due to the rigidity, or stiffness, that is part of the Parkinsons Disease syndrome, but Ive seen many patients with this pain and no apparent stiffness on examination, hence not explained. It is common and it often, but not always, responds to alterations of the usual Parkinsons Disease medications for movement. Exercise and stretching may be helpful as well and should always be tried first before increasing medications.
Pain is a challenge in PD. We cant measure it and often cannot find its cause. It is, however, often treatable, and reducing pain improves quality of life.
Pain Is An Unfortunately Common Problem In Parkinsons Disease
Of course, pain is common in the general population, especially among older people. A recent American study found that pain affected about twice as many people with Parkinsons Disease than those of the same age and gender without PD. About 50% of Parkinsons Disease patients in that study suffered from painful disorders. Men and women seem to be about equally affected. A very well described scenario is the patient who is followed for a painful frozen shoulder for a year or so before a tremor develops leading to a diagnosis of PD. Pain clearly plays a major role in quality of life. Everyone with chronic pain enjoys life less, leading to a vicious cycle in which pain causes depression or isolation which in turn leads to more pain.
Parkinson patients suffer from the same pain problems that other people have, often amplified by the motor dysfunction, but they also have additional pain problems which are unique to PD.
One recent review classified the types of pain Parkinsons Disease patients have into: musculoskeletal, in which the pain results from problems with the muscles , bones or joints dystonic, which is due to abnormal muscle contractions caused by the Parkinsons Disease or the medications used to treat it radicular pain, which is feels like the pain caused by pinched nerves central pain, which is presumed due to abnormalities in the brain, and is a continuously present pain that cannot be explained otherwise and discomfort related to an unpleasant urge to move.
Effects Of Interventions Depend On Severity Of The Postural Abnormality
Investigating the patients with camptocormia separately showed significant effects of medication and stimulation for the TCC angles . Patients with camptocormia were more likely to have a substantial improvement, while those 19% of the patients with normal TCC still remained unchanged. Of the 131 patients with stooped posture, 55 were improved to a normal angle of < 10.9° after the intervention. The mean TCC of 35.9° in the 13 patients with camptocormia improved to 21.0°, and two of them improved to within the normal range. When analyzing the patients with upper camptocormia separately, no significant effect of medication or stimulation was found. For the two patients with the Pisa syndrome, no further statistical analysis was performed because of the small group size.
Figure 3. Effects of the different treatment conditions pre- and post-surgical regarding total camptocormia and upper camptocormia angles only in those patients with postural disorders .
Figure 4. Treatment effects for the conditions presurgical Med-Off and post-surgical Med-On/Stim-On for the three subgroups of Parkinson’s disease patients for total camptocormia angle and upper camptocormia angle TCC_Normal/UCC_Normal: patients with postural alignment within the range of healthy TCC_Stooped/UCC_Stooped: patients with a stooped posture TCC_CC/UCC_CC: patients with clinically diagnosed TCC camptocormia or UCC CC.
Recommended Reading: Asbestos And Parkinson’s Disease
Tremor Rigidity Bradykinesia And Dyskinesia
One of the first visible motor symptoms to emerge in PD is resting tremor of a limb that is supported and at rest. Tremor typically begins on one side of the body with a tremor rate of 3 to 7 cycles per second. Tremors are usually less severe or even absent with voluntary movement and can increase during times of emotional stress. Tremor is considered one of the cardinal symptoms of Parkinsons diseasesome studies report it to be present in up to 80% of patients with autopsy-proven PD .
Rigidity is another common visible motor symptom associated with PD. It is a type of increased muscle tone generally defined as an increased resistance to passive movement of a joint. Rigidity tends to be more prominent in the flexor muscles of the trunk and limbs, causing a characteristic stooped posture. There are two types of rigidity: lead pipe and cogwheel. Lead pipe rigidity is defined as a constant resistance to motion throughout the entire range of movement. Cogwheel rigidity refers to resistance that stops and starts as the limb is moved through its range of motion.
Bradykinesia, another cardinal motor feature of PD, is of unknown cause and remains the subject of debate. It is defined as slowed voluntary movement, although we now know that rigidity also affects automatic movements such as arm and leg swing during gait.
Lower Back Pain And Back Of The Neck Pain Are Most Common
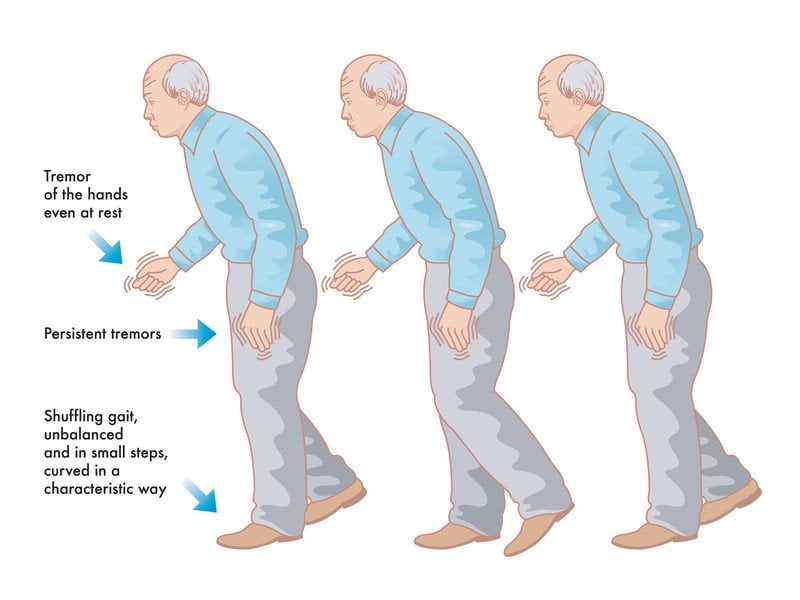
Pain occurs for a number of reasons and its not always clear what the cause is, making it difficult to figure out how best to treat it. I believe that most common pain problems in Parkinsons Disease are the same as in the general population, but amplified. Low back pain and back of the neck pain are probably the most common pain conditions in PD. The reason Parkinsons Disease patients have so many problems with their low back and their neck is their posture. Parkinsons Disease causes a stooped posture. Some of this happens with age anyway, particularly in women after menopause when their bones soften, but is always worse from the PD. All Parkinsons Disease patients have some degree of stooped posture and many also tilt to one side. Because of the stooped posture, the muscles in the lower back have to pull much harder to keep the spine upright.
Recommended Reading: How Does Parkinson’s Disease Spread From Person To Person
Parkinsons Disease: Better Diet
Its important to have a well-balanced diet, with calcium and vitamin D for bone strength. Although protein can interfere with levodopa, you can avoid the problem by taking the medicine about a half-hour before mealtime. If you have nausea, take your medicine with crackers or ginger ale. Eating a high-fiber diet with lots of fluids can prevent constipation.
Pd Community Blogread Blog
Parkinson’s Posture
Friday March 21, 2014
How does posture change with Parkinson’s?
Postural Change with Aging
Not all changes are caused by Parkinson’s disease. Degenerative changes from arthritis increase with aging. Osteoporosis can also also cause changes such as compression or fracture of the vertebral bones causing both pain and flexed posture.
- DEXA or bone density scan – Ask your doctor about ordering this test to see if you have osteoporosis or osteopenia.
- Calcium and vitamin D keep your bones strong. Be sure your get the calcium you need in your diet. Ask your doctor if a vitamin D level is appropriate.
- Weight bearing exercise weight lifting helps you keep your bone mass
How does postural change affect mobility?
With normal posture our weight is well centered over the middle of our feet making it much easier to balance. When our spine is bent forward, the head also comes forward and our center of mass shifts ahead of the feet. To keep from falling, the forward flexed person tends to bend his or her knees and hips. This leads to difficulty in taking big steps and requires more energy to walk. Falls are more likely to happen due to the reduced foot clearance or shuffling that occurs while walking with knees bent. Also forward slouching limits arm swing, can cause shoulder and neck problems, reduces the lung volume which can lead to shortness of breath and or softness of speech.
What are the treatments?
- Swimming
- Dancing
How can I get started?
Monique L. Giroux, MD
Read Also: 1st Sign Of Parkinson’s
Posture Changes As You Age
The human body goes through many changes as a normal part of the aging process. Hair gets a little thinner on top, skin wrinkles, and bones shrink. Even our posture changes. Shoulders become stooped or rounded, our lower back loses some of its curvature, and our head cranes forward involuntarily. The good news is that, unlike a receding hairline, postural changes are entirely preventable with the right lifestyle choices. But more on that later.
Losing Height As You Age
On average, people lose between a 1/4 to a 1/2 inch in height each decade after your forties or fifties. Women tend to lose more height than men, but the reason is not yet known.
People lose height as a result of the discs between their vertebrae dehydrating and compressing, which leads to a loss of vertebral height. The vertebrae can also collapse because of bone loss density associated with some diseases or loss of muscle, which contributes to a stooped posture.
While height loss is an inevitable part of aging, it can also be an indicator of an underlying health condition. Stooped posture, as well as a loss of vertebral height and loss of disc height, are symptoms of some serious health conditions.
Height loss is serious if it is the result of spinal compression and can cause severe pain and disrupted mobility. It is important to have your height measured as part of your annual exam, to ensure that the inches lost are within the normal ranges of age-related height loss.
Also Check: Ed Begley Jr Parkinson’s
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Loose Women: Ayda Field On Her Mums Parkinson’s Diagnosis
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
Parkinson’s disease progressively becomes more apparent as time goes on. However, in the earlier stages, it’s possible to detect with some visual clues.
The charity Parkinson’s Foundation noted that the brain condition “affects control of automatic activities”.
Without the brain’s automatic reminder to stand up straight, people with the condition can be prone to posture changes.
Such posture change would include stooped or rounded shoulders, decreased low back curve and a forward lean of the head or the whole body.
Don’t Miss: Do You Capitalize Parkinson’s Disease
How To Maintain Your Posture
These tips will help you improve your baseline posture and guard against some of the bad habits Parkinsons pushes you into. As with all bad habits, they are best worked against before things really deteriorate. So even if you still have relatively good posture, it will be helpful to follow these tips to maintain what you have.
Regardless of your condition, you will probably find yourself falling into poor posture at one point or another. That’s ok, the important thing is to make sure you reset when you become aware that you are off. With consistent practice, you can attain more upright and functional physical carriage and a more poised and energetic outlook.
Alignment is intimately tied up with how your entire body moves. If you are able to preserve your posture, you will also fortify your ability to do a large list of other physical motions. Parkinson’s causes more damage when you are unaware of the body parts it is affecting. Treating posture as a verb is another tactic for maintaining vigilance, and therefore, the possibility to prolong better functioning. Stand tall!
To leave a comment, follow these three steps: 1) Write your comment in the text box below, and click the “Post Comment” button 2) A black screen will appear. Write your name or “Anonymous” in the first text box 3) Click the gray “Comment As Guest” button. Voila! Thanks for your thoughts!
How Dystonia Is Caused In Parkinsons Cases

First and foremost, dystonia can be a symptom of Parkinsons disease itself. Particularly in young onset PD, foot dystonia may appear as the first motor symptom that is experienced. If dystonia occurs in isolation, the diagnosis of PD may only become clear as other symptoms appear. If dystonia occurs as the predominant symptom of PD, the patient and his/her doctor must decide how to treat it either by starting dopaminergic medications to see if this helps the dystonia or by targeting the dystonia itself, possibly with Botulinum toxin injections.
Once medications for PD have been started, dystonia may appear when there is a decrease in brain dopamine levels, which could occur first thing in the morning before taking medication or when a dose of medication is wearing off. If this is the pattern that is noted, there are various strategies that can be implemented to decrease OFF time. Depending on when the OFF time occurs, these approaches may include taking a long-acting Levodopa formulation before bed, increasing the number of doses per day or adding a medication to lengthen the amount of time that a dose works.
Read Also: Is Blurred Vision A Symptom Of Parkinson’s
Spectrum Of Postural Alignments In The Examined Patients
Patient characteristics for the entire cohort are shown in Table 1.
For the TCC angle, 11 participants had TCC angles within the range of healthy controls , 157 patients had a stooped posture , and 13 of the 192 participants had a TCC angle 30° and were diagnosed as suffering from camptocormia .
For the UCC angle, 37 subjects were considered to be within the range of healthy controls , 104 had a stooped posture , and 40 patients were diagnosed with upper camptocormia defined by an UCC angle 45° . Nine participants had both a clinically diagnosed TCC and UCC.
For the Pisa angle, 61 subjects were within the range of healthy controls regarding the lateral bending , 120 had a postural alignment between healthy and postural changes, and 2 patients had a Pisa syndrome with an angle of lateral deviation 10° . Missing values of the postural angles appear due to the inability to stand up and walk independently without any aid in some of the patients or as the quality of some videos was too low to rate them.
Why Do Some People Develop Severe Postural Problems
The reasons why some people experience severe postural problems in Parkinsons are very poorly understood. People who have a history of back problems or injuries do seem to be at higher risk but other than that it is very difficult to predict who may be affected.
In some cases, taking certain medications including antipsychotics or anti-Parkinsons medications, or surgical treatments such as deep brain stimulation, can trigger the sudden appearance, or worsening, of postural problems. In these cases, simply adjusting medication or the level of stimulation being delivered is often enough to reverse or ease the problems.
However, for most people the development of postural problems is gradual and there is no clear, single cause. Research suggests that there may be a number of complex and connected factors involved. These may involve:
Changes in muscle tone with either some muscles becoming overactive other muscles becoming weakened or a combination of both. For some, if these changes cause the muscles supporting the spine and trunk to become imbalanced it may lead to the emergence of severe postural changes.
Interestingly, although you would probably expect people to lean towards the side of the body that is more severely affected by their Parkinsons symptoms, studies that have looked at Pisa syndrome have found that there is no clear pattern in which way people with Parkinsons lean.
You May Like: Parkinson And Degenerative Disc Disease
How Are Postural Problems Treated
Treating postural problems is complex but there are ways to both alleviate the pain that many people experience and to try and correct the postural problems themselves.
In terms of drug treatment, there is a range of things that can help:
- Adjusting Parkinsons medication may be helpful if the postural problems worsen when drugs start wearing off but this doesnt work for everyone.
- Injections of muscle relaxants can be used to ease tense muscles to improve posture, but finding the right muscles to target can be tricky and again its effectiveness can be unpredictable.
- Injections of anaesthetic drugs into the muscles can provide effective pain relief.
SurgeryThere is now also a growing body of evidence that deep brain stimulation may be beneficial. A recent study which looked at cases in Germany found that if DBS was effective in 60% of camptocormia cases, and other studies have suggested it may also be beneficial for Pisa syndrome.
These findings offer additional evidence that changes in the brain may play a crucial role in causing postural changes. But it appears that surgical approaches need to be used early within 2 years of the onset of severe postural changes to have these benefits.
However, the most important thing is that people continue to exercise regularly to get the most out of it, and that means that its vital that people try out different types of exercise and find something that they really enjoy and can stick to.