Other Studies Of Interest
Three high-quality papers were found but not included in the meta-analysis as they did not report age- and gender-specific incidence rates or proportions. These studies provided information on Asian and Eastern European populations that were not well represented in the meta-analysis.
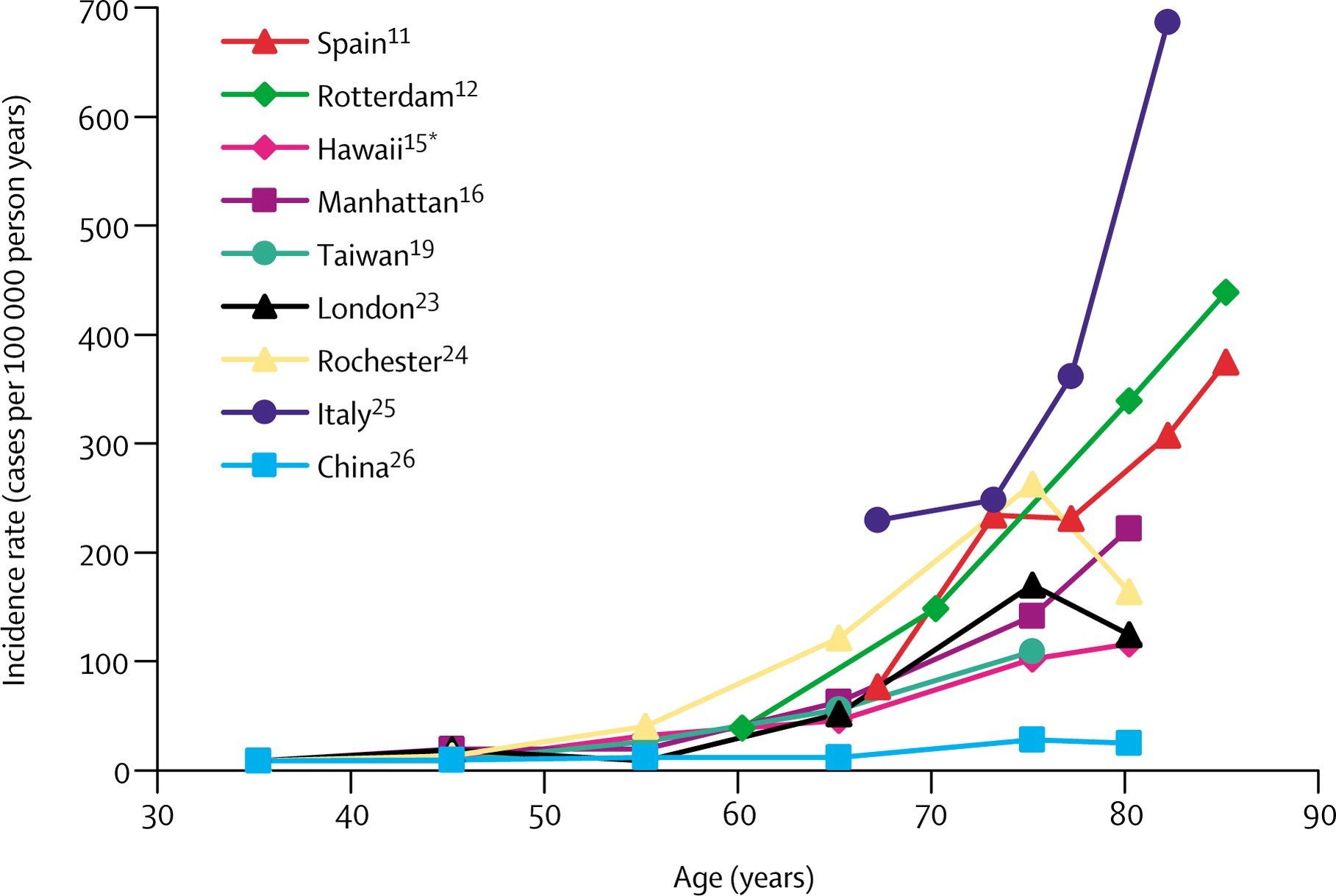
Das et al. was the only study that examined PD in a south Asian Indian population, reporting average annual incidence rates for males and females in different age categories. AAIRs peaked earlier for males, than females. Male AAIRs peaked at 60-69 years female AAIRs continued to rise in 70-79 years before dropping off in the 80+ age group. Hristova et al. and Kyrozis et al. both provided incidence rates not stratified by gender and age and therefore could not be included in the meta-analysis. Both represented unique European populations and found peak incidence between 70 and 80 years.
Occurring Diseases/complications And Mortality In Pd
Importantly, PD-associated diseases, such as depression, dementia and autonomous dysfunction, may exert a larger impact on quality of life in many PD patients than the characteristic PD motor symptoms .
In the present study, the mortality rate in PD patients was almost twice as high as in controls. A meta-analysis showed standardized mortality ratios ranging from 0.9 to 3.8 , thus the mortality ratio of 1.84 in the present study was within the mid-range of previous reports.
What Is The Prevalence
It is estimated that about 10 million people worldwide are living with PD. The incidence of the disease is higher in industrialized countries.3,4
The incidence of PD increases with age: while PD affects 1 percent of the population over the age of 60, this increases to 5 percent of the population over the age of 85.1
Approximately 5 percent of people with PD are diagnosed before the age of 60.1
Also Check: How To Care For Someone With Parkinson’s Disease
The Impact Of Parkinsons Disease On Overall Health
Based on the Blue Cross Blue Shield Health Index, the overall health of those affected by Parkinsons is significantly lower than the general population. In 2017, the average BCBS Health Index for someone aged 30-64 with Parkinsons was 57, compared to 88 for the entire commercially insured population in this age range. This translates to an average of 10.7 years of healthy life lost for those with the condition compared to 3.4 years for the 30-64 population as a whole.4
Caring for someone with Parkinsons Disease
The majority of Parkinsons patients are cared for by informal caregivers, such as a family member. The physical, mental and emotional work this requires can be significant. The Impact of Caregiving on Mental and Physical Health found that caregivers have 26% poorer health compared to a benchmark population, as measured by the BCBS Health Index. In addition, a national survey conducted by the Blue Cross Blue Shield Association found that 1 in 4 unpaid caregivers are feeling more stress trying to balance work and family due to COVID-19.5
What Are The Stages Of Parkinsons Disease
Parkinsons disease is often divided into two parts: early stage and advanced stage disease.
- Early stage: when symptoms appear and start to affect everyday activities, such as washing, getting dressed and walking.
- Advanced stage: when motor complications occur from the long term use of one of the main treatments for Parkinsons disease, levodopa.
Recommended Reading: What Age Parkinson’s Disease
Incidence Across Race And Ethnicty
Several studies have found that PD is more common in Whites than in Blacks or Asians. It is estimated that the prevalence of PD is 50 percent lower in Blacks and Asians than in Whites.5,6
However, the highest incidence of PD is found in Hispanics, followed by non-Hispanic Whites, Asians, and Blacks. According to one older study, the incidence of PD in Hispanics is 16.6 per 100,000 persons, compared to 13.6 per 100,000 in non-Hispanic Whites, 11.3 per 100,000 in Asians, and 10.2 per 100,000 in Blacks.5,6
Urban areas have a higher prevalence and incidence of PD.5
Study Design And Study Population
The present study was designed as a retrospective cohort study to estimate the population-based prevalence and incidence of PD per 100,000 persons in Germany in 2015. Moreover, we compared the prevalence of occurring symptoms and diseases, mortality, and utilization of healthcare resources between prevalent PD cases and individuals without PD.
Subjects were eligible to enter the cohort if they fulfilled the following inclusion criteria: continuous insurance in 2015 or until death, a diagnosis of PD in 2015 , continuous insurance or birth in 2013 and 2014 , and absence of a diagnosis of PD in the baseline period .
Prevalent cases of PD fulfilled one of the following criteria in 2015: Main hospital discharge diagnosis of PD , at least two diagnoses of PD in two different quarters, PD diagnoses by at least two different physicians, and/or at least one diagnosis of PD and at least one prescription for an antiparkinsonian medication in 2015 . Only primary and secondary hospital diagnoses and verified ambulatory diagnoses were considered. As suggested previously , we aimed to increase validity of ambulatory diagnoses by at least one subsequent PD diagnosis and by an additional anti-PD drug prescription in 2015. Supporting the validity of the PD diagnosis 79% of prevalent PD cases and 59% of incident PD cases fulfilled more than one of these criteria .
You May Like: Lifespan Of Someone With Parkinson’s Disease
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Ethnicity Genetics And Parkinsons
One way to explain the differences seen in PD symptoms between ethnicities is by genetic differences among these groups. Certain genes have been identified that are linked to PD. Several specific mutations in these genes tend to be more common in certain ethnic and geographic groups.
For instance, certain mutations of the LRRK2 gene are more common in Asian populations, while other mutations of the same gene are seen more commonly in North African Arab and Ashkenazi Jewish populations. Some of these mutations are also linked to increased occurrence of specific symptoms.
Recommended Reading: Foot Pain And Parkinson’s
Treatments And Healthcare Utilization
Compared to controls, PD patients were treated by a higher number of physicians , and had a higher overall number of physician contacts in 2015. The numbers of GP and psychiatrist contacts were similar between PD patients and controls, whereas treatment by a neurologist occurred more than twice a year in PD patients and only 0.3 times per year in controls. Hospital treatment in general was more frequent in PD patients compared to controls. Here, nearly two-fold higher numbers of hospitalizations and total days of hospital treatment in PD patients compared to controls were observed . The utilization of other forms of treatment and healthcare services is shown in Table 5. Treatments and support as indicated by therapeutic remedies and aids were provided more frequently for PD patients compared to controls . More than one third of PD patients was treated with physical therapy, whereas speech therapy, occupational therapy and psychotherapy were relatively rarely prescribed. Complex treatment regimes, such as apomorphine/pump treatment, deep brain stimulation , and diagnostic polysomnography were rarely prescribed in PD patients.
Table 4. Physician contacts and hospital treatment in 2015.
Table 5. Other treatments, diagnostic measures and healthcare services in PD patients and controls.
Estimation Of The 2020 Global Population Of Parkinsons Disease
N. Maserejian, L. Vinikoor-Imler, A. Dilley
Category:Epidemiology
Objective: To estimate the number of individuals living with PD globally in 2020.
Background: Although previous studies have estimated PD prevalence in many countries, the number of individuals with PD globally in 2020 has not been estimated.
Method: We comprehensively reviewed the literature for recent and reliable prevalence estimates of PD globally. The Global Burden of Disease Study was the only source available that provided an overall global estimate, with 2017 the most recent year available from the published manuscript or online tools . We verified the estimates of the PD prevalence of several countries that comprised the GBD summary estimate, by reviewing the individual publications and comparing them to the GBD estimates. GBD estimates tended to be in the lower range but close to estimates from the individual papers. For all but two countries , we applied the GBD prevalence proportions in 2017. For the US and Canada, we applied more recent prevalence proportions by Marras et al. 2018 . We assessed the worldwide PD population in 2020 by multiplying the most reliable prevalence proportions by the corresponding 2020 population, using CDC data for US, Statistics Canada for Canada, Eurostat for European countries and UN population estimates for the rest of the world.
To cite this abstract in AMA style:
Mov Disord.
Don’t Miss: Arthritis And Parkinson’s Disease
Highlights From The Canadian Chronic Disease Surveillance System
Parkinsonism, including Parkinsons disease, can have significant impacts for those affected, their caregivers, and society. With a growing and aging population, it is estimated that the number of Canadians living with parkinsonism will double between 2011 and 2031 and that the incidence will increase by 50%.Footnote 1
The Public Health Agency of Canada , in collaboration with all Canadian provinces and territories, conducts national surveillance of parkinsonism to support the planning and evaluation of related policies, programs, and services. This fact sheet presents an overview of the data on diagnosed parkinsonism, including Parkinsons disease, from the Canadian Chronic Disease Surveillance System .
Epidemiology Of Parkinsons Disease
Benjamin C.L. Lai, MD, MSc Joseph K.C. Tsui, MD, FRCP, FRCPC
ABSTRACT: The etiology of the majority of cases of Parkinsons disease remains unknown, with multifactorial theories of genoenvironmental interaction being postulated. The prevalence and incidence of PD increase exponentially with age, and are slightly higher in men than in women. A number of putative risk factors are associated with PD, age being the one most consistently agreed-upon. Exposure to pesticides is one proposed risk factor, while an inverse association between smoking and consumption of coffee and PD has been reported in other studies. The mortality rate for PD increases in older patients. The most common cause of death is pneumonia.
Exposure to pesticides is one proposed risk factor for Parkinsons disease, while coffee consumption and smoking have been claimed as protective factors, though the mechanism remains unclear.
IntroductionParkinsons disease is one of the most common age-related neurodegenerative disorders, second in frequency only to Alzheimers disease. In the United States, at least half a million people are diagnosed as having PD, and the frequency of PD is predicted to triple over the next 50 years as the average age of the population increases.
Epidemiology of Parkinsons disease
Prevalence
AcknowledgmentsThe authors thank the Medical Research Council of Canada and the Pacific Parkinsons Research Institute for their support.
You May Like: If My Parent Has Parkinson’s Will I Get It
What Does This Research Mean For People With Parkinsons
Age, sex, and ethnicity can all influence the risk of developing PD, but how is this information useful? Growing older and being white, Hispanic, or male are all associated with increased risk of Parkinsons, but these factors are not ones that you have any control over.
However, research on racial and ethnic differences in PD is helping to shed light on ways to treat PD better in specific populations. Research is also being used to look for inequities in how Parkinsons is diagnosed and treated in people of different ethnicities and in different parts of the country.
Ultimately, these findings may lead to better care for people with a diagnosis of Parkinsons. Knowledge can lead to hope. The more we know about a disease, the better we can treat it.
Who Is Affected By Parkinsons Disease
Parkinsons disease affects both men and women. Statistically, however, men have a slightly higher chance of developing the disease. The risk of developing Parkinsons disease also increases with age, with the average age of onset being 65 years old. Five to ten per cent of people develop the condition before the age of 40 years old. When symptoms appear in people aged 21-40, this is known as young-onset Parkinsons disease. Juvenile Parkinsons disease is the term used when symptoms appear before the age of 18 years old, although this is extremely rare.
To-date, no one knows exactly why people get Parkinsons disease, but viral infection or environmental toxins may play a role. People with a parent, sibling or child with Parkinsons disease, are twice as likely to get it as people in the general population.
Also Check: Can Mold Cause Parkinson’s Disease
Characteristics Of The Administrative Data Used For The Study
We conducted an observational study to determine PD prevalence based on administrative de-identified data from two Colombian HMOs using claims from 2015. Access was obtained in the settings of a research agreement with Icesi University . According to national records from 2015, 97.6% of the Colombian population is insured by the National Healthcare System. The two HMOs that provided us with claims data have 4,312,928 beneficiaries distributed across different regions of the country, mainly in the southwest. These claims are filled only by physicians certified by the government and other regulatory entities. The information is compiled by the institutions providing health services , and is prepared annually and submitted to the national government for regulatory purposes.
The analyzed data include individual records of all services provided to each affiliate: medical consultation, pharmacy, laboratory, medical props , and surgical procedures. These records are encoded through a complete, expandable and standardized system called CUPS . CUPS are defined by a decision-making group composed by medical scientific societies of the country and are used universally by all HMOs. Since each patient may use the HMO more than once per year or receive more than one service per visit, claims were grouped using a randomly assigned ID number to obtain the total patients per year and period.
Ethnicity And Parkinsons Symptoms
Ethnicity may also affect the likelihood of developing specific symptoms of Parkinsons. An analysis of data from multiple studies has found that some symptoms of PD are more common in certain countries and ethnic groups. Symptoms of PD varied in research from different countries as well.
For instance, people with PD in East Asia tended to be more likely to have nausea, vomiting, constipation, and difficulty swallowing. Excessive daytime sleepiness has been reported much more frequently in studies from North America and Europe compared to studies in Asia.
In another study, people of Afro-Caribbean and Indian backgrounds living in the United Kingdom were found to have an increased risk of atypical Parkinsons marked by bradykinesia and early dementia. This same population did not respond as well as other groups to medications such as levodopa.
In the United States, research has found higher rates of Parkinsons dementia in African American and Hispanic populations.
Comorbidities of Parkinsons can also have ethnic variation. In studies from Peru, Mexico, China, and Korea, most people with PD also had depression, while studies in the UK and the United States showed lower rates of depression.
Read Also: Parkinson’s Disease Research Paper
What Are The Management Options For Canadians Living With Parkinsonism
There is currently no cure for Parkinsons disease and most other parkinsonism cases. However, treatment options are available to help mitigate the symptoms and health impacts associated with these conditions. Most often the primary treatment is pharmacological, but it may also include other therapeutic options and, in the case of Parkinsons disease, surgical interventions. Studies have shown that specially tailored exercise programs, supervised by physiotherapists or other trained professionals, may help affected individuals maintain or improve their physical functionality and general well-being.Footnote 2 Footnote 3 Footnote 4 Footnote 5
Box 1: What’s in the data?
The data used in this publication are from the Canadian Chronic Disease Surveillance System , a collaborative network of provincial and territorial chronic disease surveillance systems, led by the Public Health Agency of Canada . The CCDSS identifies chronic disease cases from provincial and territorial administrative health databases, including physician billing claims and hospital discharge abstract records, linked to provincial and territorial health insurance registry records using a unique personal identifier. Data on all residents eligible for provincial or territorial health insurance are captured in the health insurance registries.
Definition of diagnosed parkinsonism, including Parkinsons disease, in the CCDSS
Estimated Healthcare Costs Related To Pd In The Us
The combined direct and indirect cost of Parkinsons, including treatment, social security payments and lost income, is estimated to be nearly $52 billion per year in the United States alone.
Medications alone cost an average of $2,500 a year and therapeutic surgery can cost up to $100,000 per person.
You May Like: What Is The Average Age For Parkinson’s Onset
How Many People Does Parkinsons Disease Affect
Parkinsons disease affects 1 in every 500 people in Canada. Over 100,000 Canadians are living with Parkinsons today and approximately 6,600 new cases of PD are diagnosed each year in Canada . Most are diagnosed over the age of 60 however, at least 10% of the Parkinsons population develops symptoms before the age of 50. Approximately four million people worldwide are living with the condition.
Parkinson Disease Case Definition
To define probable PD cases, we built an algorithm taking into account the clinical diagnoses and the pharmacological prescriptions of each subject. Selection of diagnostic codes was made by a neurologist trained in movement disorders taking into account previous works on administrative data in PD.According to the ICD-10 manual, G20X code is applicable to hemi-parkinsonism, idiopathic parkinsonism, primary parkinsonism, and paralysis agitans. These terms are defined as progressive, degenerative diseases of the central nervous system characterized by tremor, rigidity, postural instability, bradykinesia, and gait disturbances, which is consistent with the commonly accepted criteria for diagnosing PD. Based on previous studies, we chose levodopa as an inclusion criterion. This medication, also known as L-3,4-dihydroxyphenylalanine, represents the standard of treatment for most PD cases, regardless of clinical stage, because of its efficacy.
You May Like: Different Stages Of Parkinson’s