How Is Deep Brain Stimulation Used To Treat Parkinsons Disease
Deep brain stimulation delivers electrical impulses to a targeted area of the brain that is responsible for the movement symptoms caused by Parkinsons disease. The electrical impulses disrupt the abnormal activity that occurs in the brains circuitry, which is causing the symptoms.
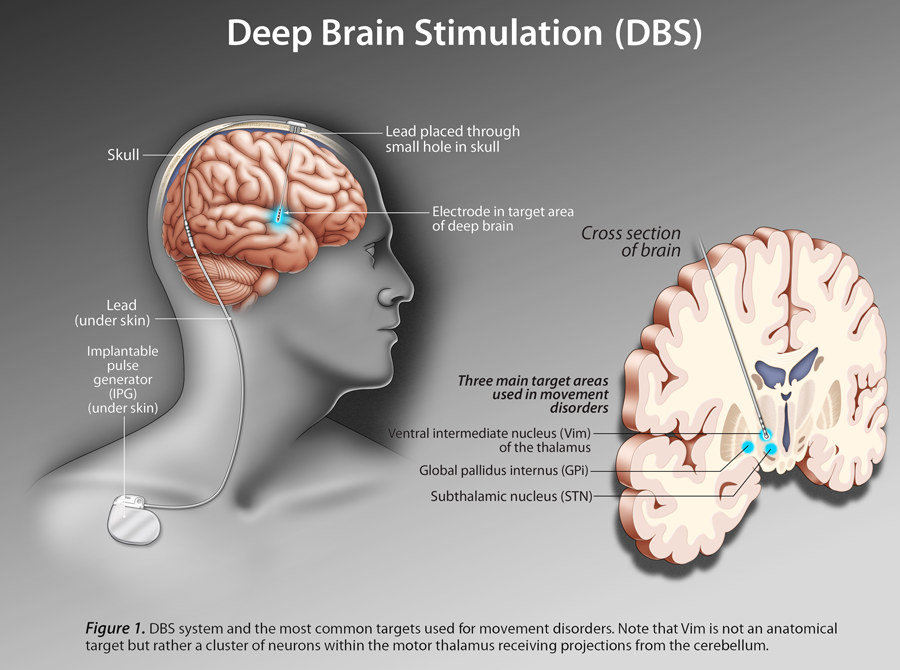
There are three areas in the brain that can be targets for deep brain stimulation in patients with Parkinsons disease. They are the subthalamic nucleus, the globus pallidus internus, and the ventral intermediate nucleus of the thalamus. Each of these areas plays a role in the brains circuitry that is responsible for the control of movement.
The specific area in the brain to target in an individual with Parkinsons disease depends on symptoms that need to be treated. For example, deep brain stimulation of subthalamic nucleus is effective for all major movement symptoms of Parkinson’s disease, such as tremor, slowness of movement , stiffness , and problems with walking and balance. Deep brain stimulation of globus pallidus is another effective target for a wide range of Parkinson’s symptoms. The thalamic target is sometimes selected for patients with tremor symptoms. The recommended target for each patient is made collaboratively with the neurologist, neurosurgeon and other caregivers involved in the decision making process.
What Results Can I Expect After Parkinsons Surgery
Deep brain stimulation does not cure Parkinsons disease or stop the degeneration of dopaminergic neurons.
However, deep brain stimulation reduces the severity of some motor symptoms such as severe tremors and slow movements.
Think of your best ON episode, i.e. when levodopa is most effective. This response is a good indicator of the best possible effect of deep brain stimulation on the extent and intensity of your symptoms.
Deep brain stimulation should significantly increase your ON time during the day and reduce your motor fluctuations. Your daily dose of levodopa should then decrease by half and therefore your dyskinesias caused by levodopa overdoses should partially disappear.
Deep brain stimulation substantially improves the quality of life of most patients who undergo surgery and usually gives them more autonomy in the performance of daily tasks.
However, this surgical procedure does not improve or only slightly improves Parkinsons disease non-motor symptoms. Your symptoms that are unaffected by levodopa will most likely not improve after surgery.
Symptoms such as speech disorders, balance problems and cognitive disorders are generally unaffected by deep brain stimulation. These symptoms may even intensify after surgery.
What You Need To Know
- Surgeons implant one or more small wires in the brain during a surgical procedure.
- The leads receive mild electrical stimulation from a small pulse generator implanted in the chest.
- Proper patient selection, precise placement of the electrodes and adjustment of the pulse generator are essential for successful DBS surgery.
- DBS does not fully resolve the symptoms of PD or other conditions, but it can decrease a patients need for medications and improve quality of life.
Read Also: Parkinson Bicycle Cleveland Clinic
Surgery To Implant The Deep Brain Stimulation Device
Deep brain stimulation requires the surgical implantation of an electrical device into the brain. A neurosurgeon uses imaging scans to pinpoint the right spot in the brain for implanting the electrode.
When surgeons have determined the correct location, they create a small opening in the skull and insert a thin, insulated wire, through which they insert the electrode. Surgery to implant the electrode takes about four hours and requires general anesthesia. You may then stay overnight in the hospital for observation.
The next day, doctors perform the second part of the surgery, which involves connecting the insulated wire to a battery-operated pulse generator that is implanted under the skin near the collarbone. Most people can return home after this procedure.
Several days after the surgery, you meet with your neurologist, who programs the pulse generator. Pushing a button on an external remote control sends electrical impulses from the pulse generator to the electrode in the brain.
People who use deep brain stimulation work closely with their neurologist to find the combination of settings that best controls their symptoms. After several visits, they are able to control the strength of the electrical impulses on their own. Following this adjustment period, most people require only occasional maintenance visits.
How Does Deep Brain Stimulation For Parkinsons Work
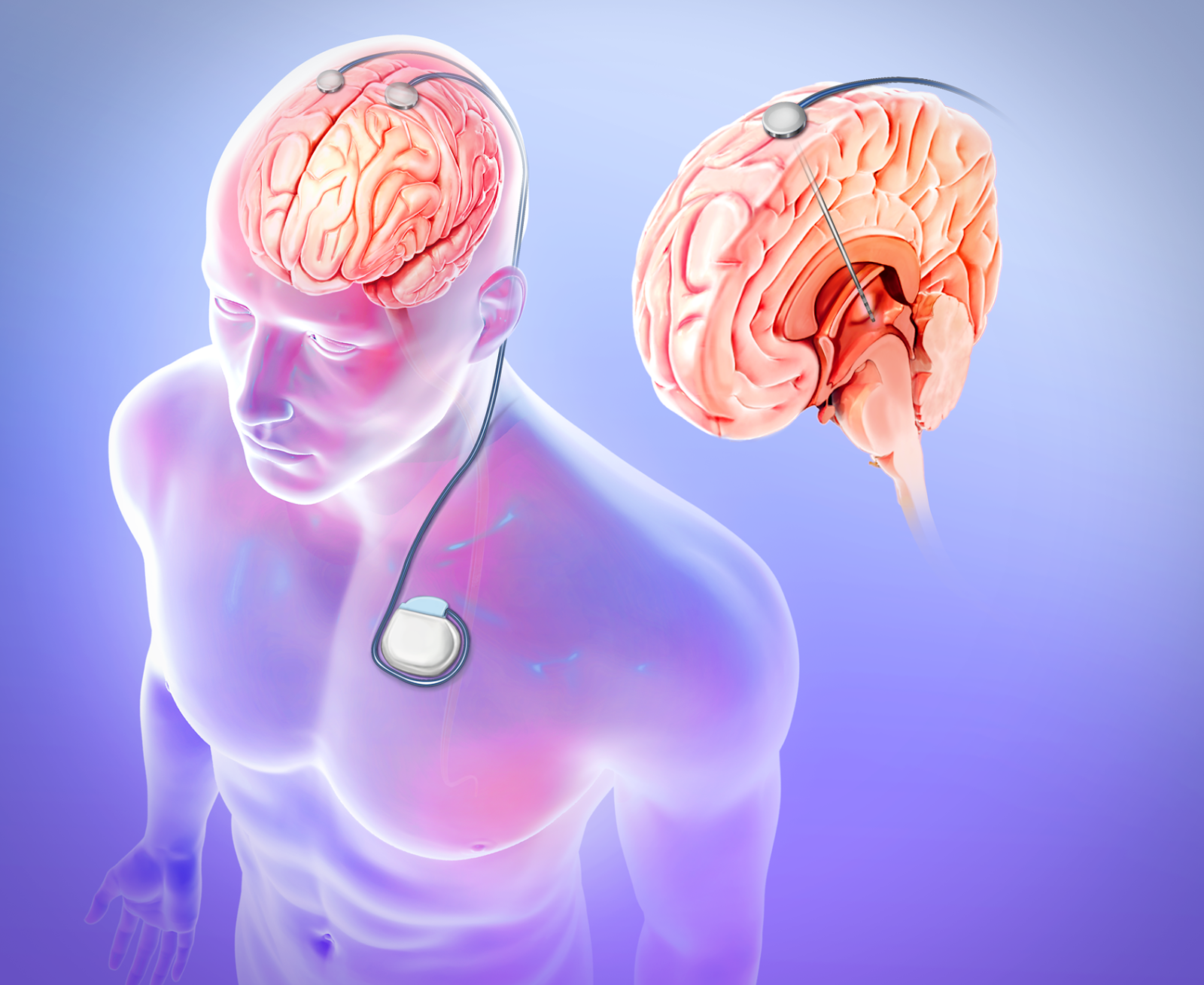
Deep brain stimulation works by modifying abnormal electrical activity in the brain. It was first approved for Parkinsons tremors in 1997 and has become an established treatment to control additional motor symptoms of Parkinsons disease.
DBS involves three main components:
- Leads: Leads are implanted in the brain in a region responsible for motor activity.
- Implantable pulse generator : A separate procedure is performed to implant a battery-operated device in the chest or in the abdomen. An IPG is similar to a pacemaker for the heart and has been coined by some as a pacemaker for the brain.
- Extension: A thin, insulated wire is passed beneath the skin between the leads and implantable pulse generator to deliver the electrical stimulation from the pulse generator to the leads.
The target area in the brain is first identified by magnetic resonance imaging or computed tomography . Then, the leads are placed via small holes that a surgeon drills in the skull.
This is considered a minimally invasive surgery that is done in the operating room with local anesthesia. It usually requires an overnight stay.
The IPG is inserted in a separate surgical procedure in the operating room roughly a week later.
After a few weeks, a neurologist begins to program the unit. This process can take several additional weeks to months. When this is completed, people are able to manage the device with a handheld remote control.
Read Also: Prayer For Parkinson’s Disease
Parkinsons Disease Dbs Surgery
Deep Brain Stimulation is a surgical treatment involving implantation of electrodes into deep structures of the brain involved in motor control.
The Food and Drug Administration approved DBS as a treatment for Parkinsons disease in 2002, but the first DBS surgery was done about 10 years prior. Electrodes are placed in the area of the brain involving motor control, and are connected to a programmable pacemaker-like device implanted under the skin in the chest wall. While it does not cure the disease, it can dramatically improve many symptoms associated with PD and patients quality of life.
Is DBS Right For You?
It is important to understand that DBS is not successful in treating all symptoms of PD. It is a proven and effective treatment for motor problems, caused by PD slowness, muscle stiffness, tremor, etc. Most non-motor symptoms of the disease, including cognitive decline, mood and behavior problems etc.., would not be expected to respond to DBS. In addition, balance problems and freezing of gait do not always improve with DBS.
Risks of DBS
Testing Before Deep Brain Stimulation
For patients with Parkinsons disease, the doctor must confirm that the PD is levodopa-responsive and determine which symptoms are most likely to respond to DBS and discuss these with the patient.
To accomplish these two objectives, the movement disorders neurologist will examine the patient in the absence of his or her PD medications, then again after having taken them. Seeing the effect of PD medications on the movement and non-motor symptoms helps the physician and patient identify good target symptoms for DBS.
A cognitive assessment can help determine a persons ability to participate in the procedure, which involves providing feedback to the doctor during surgery and throughout the neurostimulator adjustment process. This assessment also informs the team of the risk of having worsened confusion or cognitive problems following the procedure.
Some hospitals also perform an occupational therapy review or speech, language and swallowing assessment. A psychiatrist may examine the person to determine if a condition such as depression or anxiety requires treatment before the DBS procedure.
Recommended Reading: Does Vitamin B12 Help Parkinson’s
What Is Deep Brain Stimulation Or Dbs
Deep brain stimulation, or DBS, is often described as a pacemaker for the brain. It works much like a pacemaker, sending electrical signals to the brain instead of the heart. DBS is primarily utilized for patients who have Parkinsons disease, dystonia, or essential tremor, and who cant adequately control their disease with medication. Before any patient is considered for the surgery, they are evaluated by the U-M interdisciplinary team. That team includes a neurosurgeon, neurologist, clinical neuropsychologist, speech pathologist, social worker, and other team members who ensure that you and your family understand the procedure and discuss your expectations and concerns.
Its important to understand that DBS does not offer a cure for your disease, but a way to manage it more effectively. It can offer many benefits, including the need to take less medication and therefore experience fewer medication side effects.
How Do I Know If Im A Candidate For Deep Brain Stimulation
Before being considered a candidate for deep brain stimulation , patients with Parkinsons disease must undergo an extensive evaluation process. Ideally, a multidisciplinary team of specialists in the area of movement disorders will assess the patient. This clinical team typically includes a neurologist, neurosurgeon, neuropsychologist and psychiatrist.
If patients are well managed on medications, DBS is not considered. Candidates for DBS are patients who meet one or more of the following criteria:
- Symptoms are not well controlled despite receiving the appropriate dose of levodopa and other medications.
- Symptoms are significantly reducing patients quality of life.
- Abnormal or uncontrolled involuntary movements or motor fluctuations are not improving despite adjustments in medications.
- Four or more doses of levodopa are required a day.
- Tremors that have not been able to be controlled by medications.
Levodopa response test
Patients response to a single dose of levodopa is another test physicians use to identify which patients are likely to benefit from DBS. In this test, patients stop taking levodopa for 8 to 12 hours and then receive a single dose. Patients are likely to benefit from DBS if they have a clear positive response after receiving the single dose of levodopa.
Recommended Reading: Prayers For Parkinson’s Disease
Management Of Depression In The Preoperative And Postoperative Phases
The existence of depressive symptoms is not per se a contraindication to DBS surgery. However, ongoing severe depression, psychotic symptoms, and suicidal ideation should be considered absolute contraindications as they might worsen and increase suicidal risk, particularly in the first year after surgery . Less evidence is available regarding severe depressive patients who were eventually stabilized by psychotherapy and medication, months or years prior to undergoing DBS: a trend toward a slightly worse motor and mood outcome has been described, but this certainly does not constitute an absolute contraindication to surgery . In any case, most groups and guidelines support the recommendation of a thorough psychiatric assessment before DBS surgery, and of a careful post-operative follow-up. Of note, the post-operative psychiatric assessment should not be limited to the immediate post-operative period, as the occurrence of apathy, for instance, peaks at around 4 months after surgery, often accompanied by depressive symptoms . Particularly after STN-DBS, which allows for a steeper reduction of dopaminergic medication, dopamine withdrawal symptoms should be prevented, when possible favoring the continued treatment with dopamine agonists .
Pallidal Stimulation Versus Subthalamic Stimulation
As mentioned, there are two main anatomic targets for using DBS to treat PD the STN and the GPi. There have been several large randomized studies comparing STN and GPi DBS in PD. It is suggested that both STN DBS and GPi DBS overall equally and successfully improve motor symptom, and are similar in cost-effectiveness. However, although no differences were observed in the on phase between STN DBS and GPi DBS, significant differences were seen in the off phase STN DBS was more effective in terms of motor function improvement in the off phase. There are different opinions in terms of effects of STN DBS and GPi DBS on quality of life. Some authors have found no significant difference between the STN and GPi targets. However, others agree with that greater improvements in quality-of-life measures are achieved in patients with GPi DBS.
GPi DBS can be used for patients with more axial symptoms, gait issues, dyskinesias, depression, and word fluency problems. STN DBS is often favored in reducing medication post surgery, and for patients with greater tremor. STN-DBS has also demonstrated an improvement in the quality of sleep for patients.
Don’t Miss: Does Sam Waterston Have Parkinsons
Will I Be Able To Resume My Normal Daily Activities
For the first few weeks after surgery, you should avoid strenuous activity, arm movements over your shoulder, and excessive stretching of your neck. You may gradually want to try activities that were difficult before your surgery. Talk about this with your doctor first, and make sure you follow all of your doctor’s instructions.
Will I Have To Limit My Activity Following Deep Brain Stimulation Surgery
- You should not engage in light activities for 2 weeks after surgery. This includes housework and sexual activity.
- You should not engage in heavy activities for 4 to 6 weeks after surgery. This includes jogging, swimming, or any physical education classes. Anything strenuous should be avoided to allow your surgical wound to heal properly. If you have any questions about activities, call your doctor before performing them.
- You should not lift more than 5 lbs. for at least 2 weeks.
- You should not raise your arms above your shoulders or over bend or stretch your neck.
- Depending on the type of work you do, you may return to work within 4 to 6 weeks.
You May Like: What Foods Should Be Avoided When Taking Levodopa
Risks Associated With Dbs
Anytime surgery is involved, risk is involved, too. Some serious side effects include brain bleed, stroke, infection, or impacted memory. Also, part of the reason doctors screen potential DBS candidates for dementia and Alzheimers disease is to avoid worsening underlying memory problems.
As the Mayo Clinic notes, DBS is a potentially risky procedure, and patients should carefully weigh the risks and potential benefits of the procedure. Read more about possible side effects here.
How Long Will It Take For Me To Feel The Benefits Of Deep Brain Stimulation
The stimulator is not activated immediately after the surgery.
During the appointment with your specialized neurologist within two weeks of the operation, your stimulator will be activated. The medical team will then try different electrical current adjustments to maximize symptom control and minimize side effects.
In the next two months, your medical team will gradually increase the intensity of the electrical current and decrease your doses of levodopa. This adjustment period may take several months before you get the most out of this procedure.
Some devices allow patients to change the current intensity themselves according to their daily activities. In the near future, these DBS systems will be able to automatically adjust their intensity according to your needs.
Recommended Reading: Weighted Silverware For Parkinson’s
Efficacy Of Local Versus General Anesthesia Techniques
A meta-analysis of 145 studies of DBS in PD showed that the mean target error was not significantly different between LA and GA however the mean number of DBS lead passes were significantly less with GA as compared to LA .62 Post DBS complications were significantly lower with GA . The two techniques did not differ significantly in UPDRS II scores off medication, UPDRS III scores off and on medication or LED. UPDRS IV off medication score decreased more significantly in awake DBS versus sleep DBS cohorts .62 Hence, most DBS procedures should ideally be carried out under LA due to the lower side effect profile.
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Recommended Reading: Parkinson’s Hallucinations Commercial
How Is Deep Brain Stimulation Performed
Before the actual procedure begins, for most patients, a head frame is positioned on your head, which keeps your head still during brain imaging and is used to deliver the electrode to the target in the brain. Surgical pins or screws are used to secure the frame to your head. Sedation is typically given during this portion of the procedure.
Your neurosurgeon will implant the deep brain stimulation system in one to three stages.
First, a small hole is made in the skull. The leads, which have electrodes at the ends, are passed through this hole and surgically implanted in the areas of the brain identified as the site responsible for the movements caused by Parkinsons disease.
Most people with Parkinson’s disease will require one lead placed on each side of the brain unless symptoms are mostly one-sided . Each side of the brain controls the opposite side of the body, so each lead is inserted on the opposite side of where symptoms are occurring. Sometimes this procedure is done in stages one lead is placed at one time followed by another surgery for the other side. In other patients, both leads are placed during the same operation. Many times patients are awake during lead insertion. An intraoperative MRI is also sometimes used to image the lead location.
What To Expect After Deep Brain Stimulation
- Reactions 0 reactions
Deep brain stimulation is a treatment option that works well for some people with Parkinsons disease . This chronic disorder affects the nervous system and can greatly impact daily life. At times, doctors suggest DBS to help manage PD symptoms caused by the decline of neurons in the brain.1
DBS treatment involves several steps. A doctor places a special device in the persons body during surgery. This device is designed to send electrical currents to certain parts of the brain. A doctor or DBS expert adjusts the devices settings based on how the person responds to the impulses.1
Recommended Reading: Fitflop Shoes For Parkinson’s