Oncotelic Hopes To Leverage Intranasal Apomorphine To Treat Parkinsons Disease
Oncotelic Inc., an immuno-oncology company developing RNA therapeutics and small molecule drugs to treat cancers and infectious diseases, is branching out. On Monday, the company announced that it had licensed an intranasal apomorphine asset from Autotelic Inc. for the treatment of Parkinsons disease , Erectile Dysfunction and Female Sexual Dysfunction .
The Agoura Hills, CA-based company plans to develop intranasal apomorphine through the fast-to-market 5052 regulatory pathway. Oncotelic is hopeful that intranasal administration of the drug, which, contrary to its name, does not actually contain morphine, will have a unique effect in these high unmet need treatment areas.
Clinical trials have demonstrated that intermittent apomorphine injections provide rapid and effective relief from sudden, unexpected off periods brought on by primary Parkinsons medicine, levodopa. In addition, several studies have shown that continuous infusion of the drug reduced daily off time by approximately 50%. Apomorphine, a short-acting dopamine D1 and D2 receptor agonist was the first dopamine receptor agonist used to treat Parkinsons disease. It has been shown to have similar efficacy to levodopa. In ED, the specific focus will be on phosphodiesterase 5 non-responders.
The company said that AL-101 had shown a favorable safety and efficacy profile in six clinical trials with more than 200 patients treated and added that it is phase III ready.
Apda In Your Community
APDAUncategorizedRhinorrhea in Parkinsons disease
Rhinorrhea is the technical term for runny nose. It literally means fluid from the nose and can refer to anything flowing from it. Carol Jacques, the nurse practitioner who worked with me for several years, pointed out many years ago that a lot of our patients with Parkinsons disease had a runny nose. I didnt think much of it. She found that a nasal spray worked very well and shed prescribe it, with wonderful results. I patted her on the back and paid little attention.
At this point I decided to do a study. Better late than never.I simply compared people with Parkinsons Disease to people without Parkinsons Disease to determine if runny nose was more common in PD. After all, if rhinorrhea is common in PD, it also may be common in older folks in general, just like constipation or arthritis.
Using A Runny Nose As A Pre
This raised another question. There has been a lot of interest in the last several years in finding pre-motor symptoms of PD. That is, identifying people with Parkinsons Disease even before they have their first symptom of tremor, slowness, stiffness or anything else like that. If we finally find a medicine that will slow the progression, then if we can identify people who have Parkinsons Disease before they have movement problems, maybe we will prevent them, or at least forestall them.
In our studies weve had conflicting results about the connection between smell and runny nose, so we dont know whether runny nose interferes with smell or not.
We are hoping to extend our study to see if the problem of rhinorrhea affects all of Parkinsons Disease patients in the US or whether it is only a Rhode Island problem, possibly due to something in the air. As Yogi Berra said, You can see a lot just by looking. Keep tuned.
Recommended Reading: Weight Loss In Late Stage Parkinson’s
Mitochondrial Labelling And Isolation
Allogeneic mitochondria were isolated from rat livers. For tracking of mitochondria after delivery, mitochondrial DNA in hepatocytes was labeled with 5-Bromodeoxyuridine prior to isolation. Rats were sacrificed 36 h after a single intraperitoneal injection of BrdU . Livers were homogenized in ice cold buffer using a Precellys homogenizer . Through a series of filtration and centrifugation steps, as described previously, isolated mitochondria were re-suspended in ice-cold MiR05 respiration buffer and prepared for use. BrdU immunofluorescence was used to track internalized mitochondria in sample tissue.
New Nasal Spray Targets Parkinsons Disease
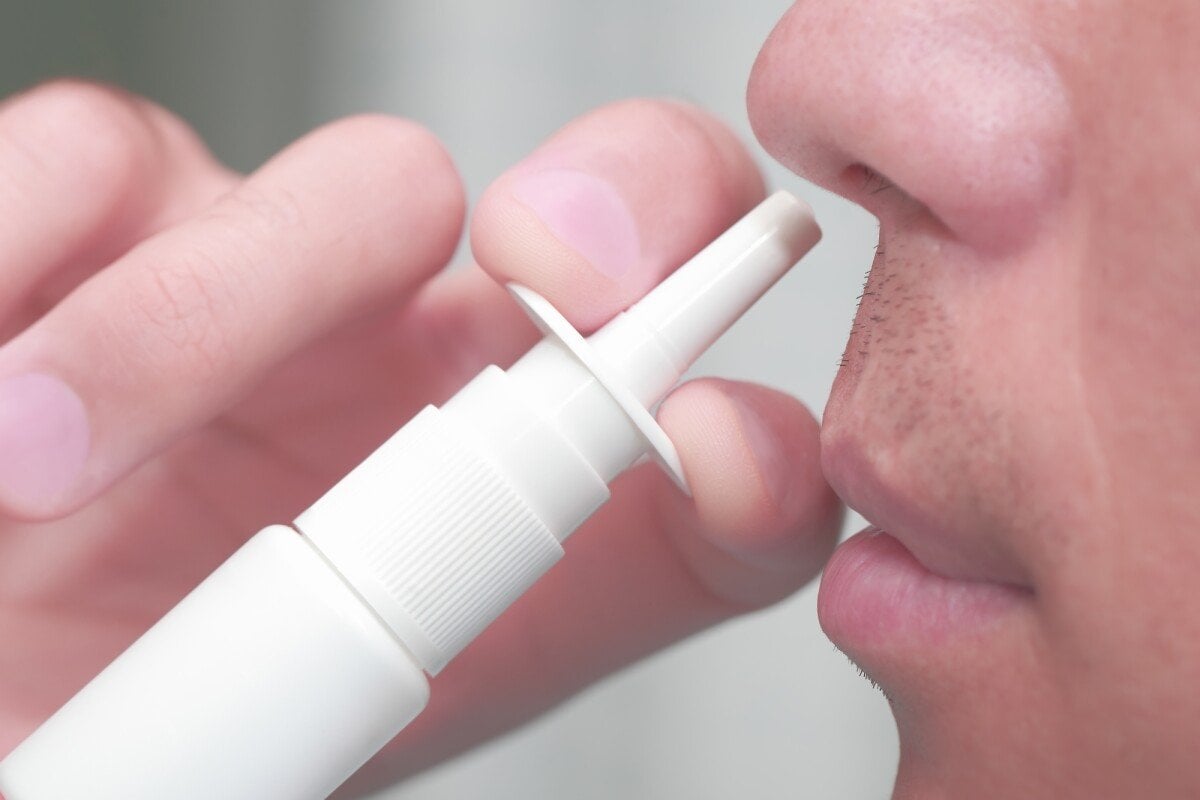
University of York researchers are developing a nasal spray to treat Parkinsons patients.
Although there is currently no cure for Parkinsons disease, theres no shortage of treatments in development. Its not a bad idea as the baby boomers enter old age, and the demand is higher than ever. A recent Technology.orgarticle discussed a new nasal spray intended to treat the millions of people suffering from the neurodegenerative condition.
Current treatments lose their efficacy over time as the body learns to break them down before they reach the brain. The nasal spray, called levodopa, could prove more effective as it works through the nerves that service the nose. It is converted into dopamine in the brain to help account for the lack of dopamine-producing cells in Parkinsons patients. However, a liquid nasal spray doesnt stay in the nose long enough for an effective release of the drug, so the team made the spray a gel, which stays in the nasal cavity longer.
You May Like: Parkinson’s Disease Journal Articles
Australian Researchers Hope Brain Gel Can Reverse Parkinsons Disease Symptoms
Australian researchers say they have developed a new type of gel that could radically transform the treatment of Parkinsons disease and could also help stroke patients.
The hydrogel is made from natural amino acids, the building blocks of proteins, and has been shown to safely deliver replacement cells into damaged parts of the brain.
The gel acts as a vehicle to safely transfer stem cells into the brain. Scientists believe the process can restore damaged tissue and replace lost neurons, which affect patients with Parkinsons disease, a nervous system disorder. About 100,000 Australians are estimated to suffer from the disease, which currently has no cure.
If you imagine a stroke, you have a whole bunch of dead cells where you are no longer getting blood flow, said professor David Nisbet, one of the lead researchers from the Australian National Universitys College of Health and Medicine. In terms of Parkinsons disease, you lost population of neurons, thats what results in the symptoms we are familiar with seeing. Basically, what we are doing we are introducing replacement cells into the brain to replace those ones that we can see some repair and regeneration. But they also have the added advantage that we have also shown they can actually protect some of the existing cells in the surrounding tissue once they are implanted.
Nisbet said the early results are encouraging.
It has been published in the journal Advanced Functional Materials.
Histological And Immunohistochemical Staining
Rats that survived 3 months after transplantation were sacrificed with an overdose of chloral hydrate and fixed by intracardiac perfusion with 300 mL of saline followed by 300 mL of 4% paraformaldehyde . Brains were removed, post-fixed in 4% paraformaldehyde for 4 h, and cryoprotected in 30% w/v sucrose in PBS for 20 h. Brains were then frozen and embedded in OCT medium and sectioned at 510-m.
For Nissl staining, sections mounted on glass slides were dried overnight. Slides were immersed in 0.025% cresyl violet in 90 mM acetic acid and 10 mM sodium acetate for 3 h, followed by dehydration in ascending ethanol and xylene series. Slides were then coverslipped with Histochoice mounting media .
You May Like: Early Parkinson’s Symptoms In Young Adults
Makes Up For Dopamine Deficit
Levodopa is converted to dopamine in the brain, which makes up for the deficit of dopamine-producing cells in Parkinsons patients, and helps treat the symptoms of the disease. Over extended periods of time, however, levodopa becomes less effective, and increased doses are needed, a media release from University of York explains.
The current drug used for Parkinsons Disease is effective to a point, but after a long period of use the body starts to breakdown the drug before it gets to the brain where it is most needed.
This means increased dosage is necessary, and in later stages, sometimes, instead of tablets, the drug has to be injected. Investigations into nasal sprays have long been of interest as a more effective delivery because of its direct route to the brain via the nerves that service the nose, but the challenge here is to find a way of making it adhere to the nasal tissue long enough to release a good dosage of the drug.
Professor David Smith, from the University of Yorks Department of Chemistry
The gel, loaded with levodopa, is designed to flow into the nose as a liquid and then rapidly change to a thin layer of gel inside the nose. The method was tested in animal models by a team at Kings College London, where levodopa was successfully released from the gel into the blood and directly to the brain.
Nasal Spray Could Be Used To Treat Parkinsons Disease
Parkinsons disease is an incurable neurodegenerative condition, affecting millions of people in the world. It is one of the leading causes of age-related dementia as well as a very common cause of disability or death.
Now scientists at the University of York are pushing to make a nasal spray treatment for patients with Parkinsons disease.
While Parkinsons disease is incurable, it doesnt mean that there are no treatment options. Symptomatic treatment is possible, even if it is not too effective, and it does improve the quality of life of the patients. The problem is that these drugs lose their effectiveness over time, because the body simply learns to break them down even before they have the opportunity to reach the brain. Therefore, the dosage is increased over time, pills are replaced with injections and with time the condition worsens anyway. Nasal spray could be a more effective solution, working through the nerves that service the nose.
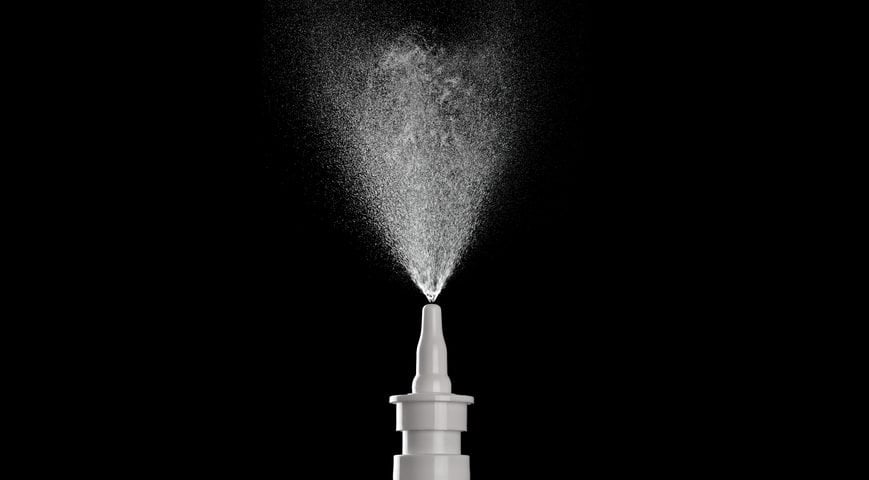
Nasal spray delivers gel into the patients nose, which sticks long enough to release the drugs. Image credit: NIAID via Wikimedia
Khuloud Al-Jamal, one of the authors of the study from Kings College London, said: Not only did the gel perform better than a simple solution, but the brain uptake was better than that achieved using intravenous injection of the drug. This suggests that nasal delivery of Parkinsons drugs using this type of gel may have clinical relevance.
Also Check: Nutritional Support For Parkinson’s Disease
Searching To Control Symptoms: New Methods Of Delivery
In recent months, symptomatic treatment of PD has had some new developments as well. A new drug for PD, rotigotine, has been introduced in Europe and elsewhere as Neupro. This compound is a dopaminergic agonist, a class of drugs that also includes drugs that have been available for many years in the U.S., including Mirapex, Requip, and Permax . Neupro is unique in how it is delivered: it is absorbed through the skin and so has been marketed as a transdermal patch with continuous delivery over 24 hours. So far, experience with Neupro suggests that it is effective and well tolerated. However, whether this drug or its unique mode of delivery will offer a significant advantage over currently marketed medications of the same class still remains to be learned.
PD still presents many challenges for the medications of the future. Among the unmet needs are ways to reverse the problem of imbalance, especially falling backward. The flexed posture of PD, swallowing and speech difficulties, and situation-specific “freezing” are all challenges for improved drug therapy. Scientists have not yet determined where in the brain and what types of biochemical disturbance underlie these problems.
Anticholinergic Nasal Spray Eases Rhinorrhea In Parkinson’s
Megan Brooks
STOCKHOLM, Sweden Rhinorrhea in patients with Parkinson’s disease may respond to anticholinergic nasal spray, hints a small pilot study.
“All of our patients responded very well without any significant side effects,” Rachana Gandhi, MD, from the Department of Neurology, Cleveland Clinic Florida in Weston, Florida, told Medscape Medical News.
Rhinorrhea is a common nonmotor symptom of PD, with a reported prevalence between 24% and 50%. Yet, “it’s not well recognized or studied,” Dr. Gandhi said.
“A persistent runny nose is not only bothersome, but can also lead to postnasal drip and coughing. Eating may make it worse, so many patients avoid social meal and gatherings,” she explained. “Many of our patients as well as family members found it emotionally disturbing.”
While many medications are available for rhinorrhea, “none of them is actually well studied, which prompted us to do a pilot study to assess efficacy of anticholinergic spray in PD patients,” Dr. Gandhi said.
She presented the study at the recent International Parkinson and Movement Disorder Society 18th International Congress of Parkinson’s Disease and Movement Disorders.
Symptom Relief, Improved Quality of Life
The study included 5 patients who were at least 60 years of age and who had rhinorrhea and a diagnosis of PD for less than 7 years. Two of the 5 patients developed rhinorrhea within the first year of being diagnosed with PD.
Table. Change in SNOT-22 Score After Treatment
| Patient |
| 77 |
You May Like: Parkinson Disease And Driving An Evidence Based Review
Symptoms That May Be Related To Pd But That Few People Know About
People with PD and care partners may suspect that a particular symptom is related to PD, but they cant find information about it, so they are not sure. Two symptoms that pop up in this category are runny nose and breathing problems, which well focus on today. Of course, if these are new symptoms for you, they could be indicative of a new problem, including infection with COVID-19, so make sure to get yourself checked out by your doctor. However, if all else is ruled out, PD could be to blame. Excessive sweating and specific skin disorders are in this category as well and have been addressed previously.
Runny Nose And Parkinsons Disease
Runny nose, or rhinorrhea in medical jargon, is an annoying symptom that has been shown in a number of studies to be more common among people with PD than those without PD. The rhinorrhea of PD is not associated with a viral infection or environmental allergies, or any other common cause of runny nose.
Rhinorrhea can be an early feature of PD, sometimes present at the time of diagnosis. In fact, studies have shown that rhinorrhea is not correlated with disease duration, disease severity, or whether the PD is characterized more by tremor or gait difficulties. One study tested the smell of those with runny nose versus those without and determined that the presence of rhinorrhea did not correlate with deficits in the sense of smell.
There are no studies in the medical literature addressing how to treat the runny nose associated with PD. Ipratropium bromide is an anti-cholinergic medication that does not cross the blood-brain barrier and is available in two forms an inhaled form to treat asthma, chronic bronchitis and emphysema and a nasal spray that is used to treat allergic and non-allergic runny nose. The nasal spray may be worth a try in PD-related rhinorrhea.
Read Also: Difference Between Parkinson’s And Dementia
What Is Gimoti Nasal Spray
Gimoti is a new FDA approved nasal spray formulation of metoclopramide. We do not recommend this for use in Parkinsons or movement disorders. This medication formulation has been associated with movement disorders similar to the pill form. The company also states that there are potential effects such as other changes in muscle control and movement, such as, uncontrolled spasms of your face and neck muscles, or muscles of your body, arms, and legs , parkinsonism slight shaking, body stiffness, and trouble moving or keeping your balance, being unable to sit still or feeling that you need to move your hands, feet, or body , Neuroleptic Malignant Syndrome a very rare but very serious condition. NMS can lead to death and must be treated in a hospital, and depression, thoughts about suicide, and suicide.
To read more books and articles by Michael S. Okun MD check on and these websites with blogs and information on his books and #Livingwith Parkinsons #EndingPD #Parkinsonsecrets #LessonsFromTheBedside
He also serves as the Medical Advisor for the Parkinsons Foundation.
To see more on Dr. Indu Subramanian she does live interviews of experts in Parkinsons for the PMD Alliance.
The blog artist is Jonny Acheson.
Gastrointestinal Issues In Parkinsons
Domperidone, despite being anti-dopamine, works only in the peripheral blood and not in the brain. Thus, domperidone does not have a significant effect at the level of the brain cells and will not worsen Parkinsons disease symptoms. This is an excellent choice for treatment of gastrointestinal symptoms of Parkinsons.
You May Like: Best Time To Take Parkinson’s Medication
Nasal Spray For Parkinsons Disease Delivers Treatment Directly To Brain
Parkinsons disease is a progressive nervous system disorder that affects movement. Symptoms start gradually, sometimes starting with a barely noticeable tremor in just one hand. Tremors are common, but the disorder also commonly causes stiffness or slowing of movement.
Development of a nasal spray treatment for patients with Parkinsons disease has attained significant progress by the scientists at the University of York.
Parkinsons disease is a progressive neurodegenerative disorder that primarily affects movement due to loss of nerve cells neurons that produce a chemical messenger in the brain called dopamine . It is characterized by the formation of inclusion proteins called Lewy bodies.
A new gel has been developed by the team, that could flow into the nose as a liquid and then rapidly change to a thin layer of gel inside the nose alongside the drug levodopa.
This helps in delivering the levodopa successfully from the gel into the blood and then directly to the brain. The levodopa is then converted to dopamine in the brain, which makes up for the deficit of dopamine-producing cells in Parkinsons patients and helps treat the symptoms of the disease.
Levodopa is a dopamine agonist drug that is most commonly used to treat Parkinsons patients. Over extended periods, levodopa becomes less effective, which mandates increased doses.
Magnetic Resonance Measurement Unique
The 15 study participants, each with mid-stage Parkinsons disease, gave themselves a single dose of the antioxidant nasal spray while undergoing magnetic resonance spectroscopy. Using the brain scans of participants before the dose and at intervals in the hour following, the research team was able to observe how well the antioxidant was delivered across the blood brain barrier. Padowski assisted with data interpretation and analysis of the study.
The use of magnetic resonance spectroscopy to observe changes in chemical composition of the brain over time is novel, and glutathione happens to be one of the few antioxidants you can detect with this approach, said Padowski.
The proof-of-concept study was the first of its kind to demonstrate a noninvasive, self-administered therapy that has potential for boosting glutathione levels in the brain.
Also Check: Glutathione Injections For Parkinson’s