What Is The Outlook For Persons With Parkinsons Disease
Although there is no cure or absolute evidence of ways to prevent Parkinsons disease, scientists are working hard to learn more about the disease and find innovative ways to better manage it, prevent it from progressing and ultimately curing it.
Currently, you and your healthcare teams efforts are focused on medical management of your symptoms along with general health and lifestyle improvement recommendations . By identifying individual symptoms and adjusting the course of action based on changes in symptoms, most people with Parkinsons disease can live fulfilling lives.
The future is hopeful. Some of the research underway includes:
- Using stem cells to produce new neurons, which would produce dopamine.
- Producing a dopamine-producing enzyme that is delivered to a gene in the brain that controls movement.
- Using a naturally occurring human protein glial cell-line derived neurotrophic factor, GDNF to protect dopamine-releasing nerve cells.
Many other investigations are underway too. Much has been learned, much progress has been made and additional discoveries are likely to come.
Treating Parkinsons With Complementary Medicine
Complementary medicine incorporates many different practices that can be used alongside conventional medicine to try to ease PD symptoms. There is typically not as much rigorous data to support the use of complementary medicine techniques, as compared to conventional medicine, but many patients find them helpful. These include yoga and massage.
Neurosurgical Treatments Of Parkinsons Disease
It is beyond the scope of this manuscript to comprehensively review neurosurgical treatment of PD. Only a brief review will be provided here and the reader is referred to other published literature on for additional information about this important therapeutic strategy. The renewed interest in surgical treatment of movement disorders has been stimulated in part by improved understanding of the functional anatomy underlying motor control, as well as refinement of methods and techniques in neurosurgery, neurophysio logy, and neuroimaging .
Besides thalamotomy and pallidotomy, another promising surgical approach for the treatment of tremors and other movement disorders is high-frequency DBS via electrodes implanted in the VIM nucleus of the thalamus, GPi, STN or other subcortical nuclei. The mechanism of electrical stimulation is not known, but the following explanations have been offered: 1) disruption of the network , 2) depolarization block, 3) preferential activation of inhibitory neurons, and 4) a functional ablation by desynchronizing a tremorogenic pacemaker.
Recommended Reading: Cluster Headaches Parkinson’s Disease
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
Alternative Treatments For Parkinson’s Disease
Alternative therapy may also be used to treat Parkinson’s disease. The most touted in recent years has been the effect of Vitamin E on reversing the progression of the disease although, this effect is still being debated by the scientific community.
Relaxation and guided imagery have also been suggested to help with stress, depression, and anxiety. Medical studies have shown that relaxation and guided imagery may help slow the progression of symptoms as well as quicken healing time after surgeries or injuries.
Recommended Reading: Drugs That Cause Parkinson Like Symptoms
Who Gets Parkinson Disease
The exact cause of Parkinson disease is unknown, but it is assumed to be the result of a combination of environmental influences superimposed on genetic predisposition or susceptibility . There is increasing evidence that the genetic and environmental insults leading to Parkinson disease commonly lead to abnormal forms of a normal protein, -synuclein, which seems to contribute to cell death., The onset of Parkinson disease can be categorized as juvenile , early onset and late onset ., The juvenile form is rare, is often familial , is most frequently associated with a parkin gene mutation and has an atypical presentation., Of patients with Parkinson disease, 10%16% have an affected first- or second-degree relative first-degree relatives may have double the risk of Parkinson disease compared with the general population. In early- and late-onset Parkinson disease, the frequency of a positive family history is not statistically different.
What Medications Are Used To Treat Parkinsons Disease
Medications are the main treatment method for patients with Parkinsons disease. Your doctor will work closely with you to develop a treatment plan best suited for you based on the severity of your disease at the time of diagnosis, side effects of the drug class and success or failure of symptom control of the medications you try.
Medications combat Parkinsons disease by:
- Helping nerve cells in the brain make dopamine.
- Mimicking the effects of dopamine in the brain.
- Blocking an enzyme that breaks down dopamine in the brain.
- Reducing some specific symptoms of Parkinsons disease.
Levodopa: Levodopa is a main treatment for the slowness of movement, tremor, and stiffness symptoms of Parkinsons disease. Nerve cells use levodopa to make dopamine, which replenishes the low amount found in the brain of persons with Parkinsons disease. Levodopa is usually taken with carbidopa to allow more levodopa to reach the brain and to prevent or reduce the nausea and vomiting, low blood pressure and other side effects of levodopa. Sinemet® is available in an immediate release formula and a long-acting, controlled release formula. Rytary® is a newer version of levodopa/carbidopa that is a longer-acting capsule. The newest addition is Inbrija®, which is inhaled levodopa. It is used by people already taking regular carbidopa/levodopa for when they have off episodes .
Recommended Reading: Most Common Parkinson’s Medications
Who Gets Parkinsons Disease
Risk factors for PD include:
- Age. The average age of onset is about 70 years, and the incidence rises significantly with advancing age. However, a small percent of people with PD have early-onset disease that begins before the age of 50.
- Sex. PD affects more men than women.
- Heredity. People with one or more close relatives who have PD have an increased risk of developing the disease themselves. An estimated 15 to 25 percent of people with PD have a known relative with the disease. Some cases of the disease can be traced to specific genetic mutations.
- Exposure to pesticides. Studies show an increased risk of PD in people who live in rural areas with increased pesticide use.
Symptomatic And Neuroprotective Therapy
Pharmacologic treatment of Parkinson disease can be divided into symptomatic and neuroprotective therapy. At this time, there is no proven neuroprotective or disease-modifying therapy.
Levodopa, coupled with carbidopa, a peripheral decarboxylase inhibitor , remains the gold standard of symptomatic treatment for Parkinson disease. Carbidopa inhibits the decarboxylation of levodopa to dopamine in the systemic circulation, allowing for greater levodopa distribution into the central nervous system. Levodopa provides the greatest antiparkinsonian benefit for motor signs and symptoms, with the fewest adverse effects in the short term however, its long-term use is associated with the development of motor fluctuations and dyskinesias. Once fluctuations and dyskinesias become problematic, they are difficult to resolve.
Monoamine oxidase -B inhibitors can be considered for initial treatment of early disease. These drugs provide mild symptomatic benefit, have excellent adverse effect profiles, and, according to a Cochrane review, have improved long-term outcomes in quality-of-life indicators by 20-25%.
Neuroprotective therapy aims to slow, block, or reverse disease progression such therapies are defined as those that slow underlying loss of dopamine neurons. Although no therapy has been proven to be neuroprotective, there remains interest in the long-term effects of MAO-B inhibitors. Other agents currently under investigation include creatine and isradipine.
Also Check: Can You Diagnose Parkinson’s With A Blood Test
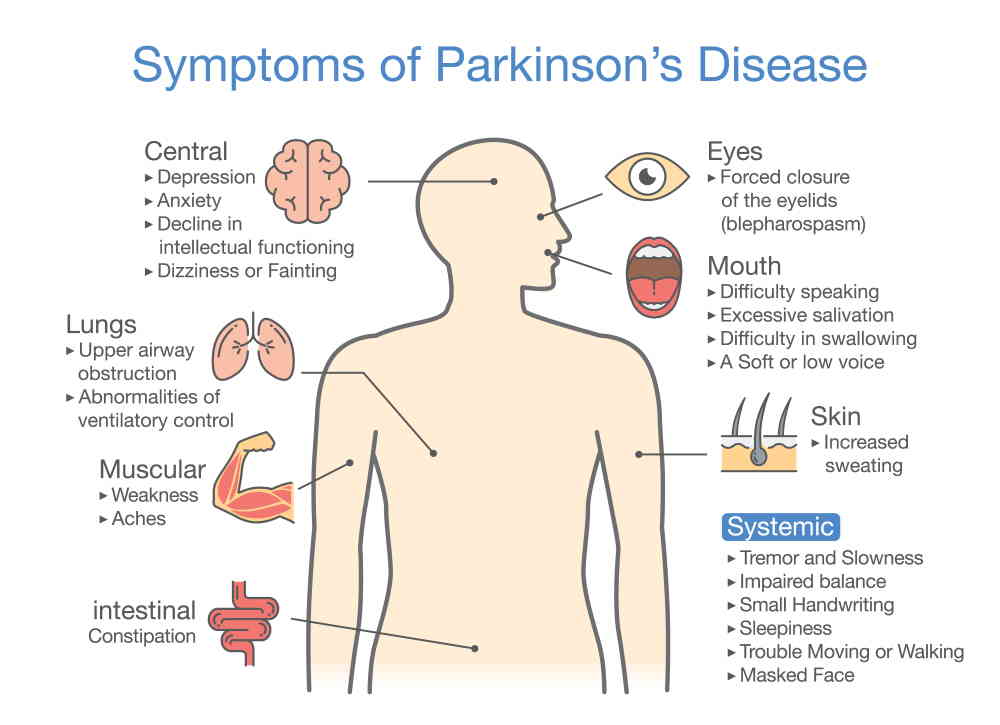
What Are The Symptoms Of The Disease
The four primary symptoms of PD are:
- Tremor. Tremor often begins in a hand, although sometimes a foot or the jaw is affected first. The tremor associated with PD has a characteristic rhythmic back-and-forth motion that may involve the thumb and forefinger and appear as a pill rolling. It is most obvious when the hand is at rest or when a person is under stress. This tremor usually disappears during sleep or improves with a purposeful, intended movement.
- Rigidity. Rigidity , or a resistance to movement, affects most people with PD. The muscles remain constantly tense and contracted so that the person aches or feels stiff. The rigidity becomes obvious when another person tries to move the individuals arm, which will move only in ratchet-like or short, jerky movements known as cogwheel rigidity.
- Bradykinesia. This slowing down of spontaneous and automatic movement is particularly frustrating because it may make simple tasks difficult. The person cannot rapidly perform routine movements. Activities once performed quickly and easilysuch as washing or dressingmay take much longer. There is often a decrease in facial expressions.
- Postural instability. Impaired balance and changes in posture can increase the risk of falls.
How Do I Prevent Falls From Common Hazards
- Floors: Remove all loose wires, cords, and throw rugs. Minimize clutter. Make sure rugs are anchored and smooth. Keep furniture in its usual place.
- Bathroom: Install grab bars and non-skid tape in the tub or shower. Use non-skid bath mats on the floor or install wall-to-wall carpeting.
- Lighting: Make sure halls, stairways, and entrances are well-lit. Install a night light in your bathroom or hallway and staircase. Turn lights on if you get up in the middle of the night. Make sure lamps or light switches are within reach of the bed if you have to get up during the night.
- Kitchen: Install non-skid rubber mats near the sink and stove. Clean spills immediately.
- Stairs: Make sure treads, rails, and rugs are secure. Install a rail on both sides of the stairs. If stairs are a threat, it might be helpful to arrange most of your activities on the lower level to reduce the number of times you must climb the stairs.
- Entrances and doorways: Install metal handles on the walls adjacent to the doorknobs of all doors to make it more secure as you travel through the doorway.
Also Check: Tea For Parkinson’s Disease
What Is The Pathophysiology Of The Disease
Parkinson disease is a neurodegenerative syndrome involving multiple motor and nonmotor neural circuits., It is characterized by two major pathologic processes: premature selective loss of dopamine neurons the accumulation of Lewy bodies, composed of -synuclein, which become misfolded and accumulate in multiple systems of patients with Parkinson disease. It is unclear which process occurs first. Based on pathologic studies, there is a stepwise degeneration of neurons over many years, with each affected site corresponding to specific symptomatology in Parkinson disease . When motor symptoms become evident, there is 3070% cell loss evident in the substantia nigra on pathologic examination. The mainstay of therapy aims to replace dopamine with dopaminergic medications and modulate the dysfunctional circuit. Cognitive dysfunction, mood disorders and impulse control disorders are related to deficits of dopamine outside the basal ganglia or in serotonergic and noradrenergic systems., Autonomic dysfunction has been related to pathologies outside the brain, including the spinal cord and peripheral autonomic nervous system.
An Update On The Diagnosis And Treatment Of Parkinson Disease

Parkinson disease is the second most common neurodegenerative disorder after Alzheimer disease. Parkinson disease typically develops between the ages of 55 and 65 years and occurs in 1%2% of people over the age of 60 years, rising to 3.5% at age 8589 years. About 0.3% of the general population is affected, and the prevalence is higher among men than women, with a ratio of 1.5 to 1.0. Parkinson disease may be more common among white people than those of Asian or African descent however, the data are conflicting., In 2011, the estimated number of people living with Parkinson disease in Canada had reached 85 200. By 2031, the projected number of people with this disease will double.,
Management remains complicated over the course of the disease and should be individualized based on the patients quality of life at each stage of disease. There have been many advancements in the management of Parkinson disease and ongoing research. Many options are now available. This review presents current treatment strategies and recommendations in managing motor and nonmotor symptoms in the various stages of Parkinson disease. Methods for developing this review are outlined in .
Recommended Reading: Parkinson’s Support Group Long Island
What Causes The Disease
The precise cause of PD is unknown, although some cases of PD are hereditary and can be traced to specific genetic mutations. Most cases are sporadicthat is, the disease does not typically run in families. It is thought that PD likely results from a combination of genetics and exposure to one or more unknown environmental factors that trigger the disease.
The protein alpha-synuclein. The affected brain cells of people with PD contain Lewy bodiesdeposits of the protein alpha-synuclein. Researchers do not yet know why Lewy bodies form or what role they play in the disease. Some research suggests that the cells protein disposal system may fail in people with PD, causing proteins to build up to harmful levels and trigger cell death. Additional studies have found evidence that clumps of protein that develop inside brain cells of people with PD may contribute to the death of neurons.
Genetics. Several genetic mutations are associated with PD, including the alpha-synuclein gene, and many more genes have been tentatively linked to the disorder. The same genes and proteins that are altered in inherited cases may also be altered in sporadic cases by environmental toxins or other factors.
Environment. Exposure to certain toxins has caused parkinsonian symptoms in rare circumstances . Other still-unidentified environmental factors may also cause PD in genetically susceptible individuals.
Current Treatment Options For Parkinsons Disease
There are currently no disease-modifying treatments for PD, and management predominantly consists of dopaminergic drugs. The most commonly used of these are preparations of levodopa, the precursor of dopamine, which is administered in combination with a dopa-decarboxylase inhibitor which acts to limit some of the side effects, such as nausea. Dopamine agonists, such as ropinirole or rotigotine, are also used. Monoamine oxidase B inhibitors, such as rasagiline and selegiline, and catechol-O-methyltransferase inhibitors such as entacapone, can be used to reduce the metabolism of endogenous dopamine. These treatments can restore dopaminergic activity in the striatum, heralding improvements in the motor features of PD. However, they do not treat many of the non-motor features, which are particularly disabling for many patients. Indeed, in some cases treatments may exacerbate some of the non-motor symptoms, such as postural hypotension and neuropsychiatric problems .
Other treatment options include deep brain stimulation , which can be very effective in controlling the movement disorder of PD, but like the dopaminergic medications it does not help with most of the non-motor manifestations . Though DBS is a safe treatment approach, there are other potentially problematic adverse effects including speech dysfunction and psychiatric disturbance, as well as the general risks associated with a neurosurgical procedure, and this treatment is only suitable in a minority of PD cases .
You May Like: Cleveland Clinic Parkinson’s Center Of Excellence
Updates On Currently Approved Pd Treatments
Table 1 Approved dopaminergic drugs
Later, DA receptor agonists, such as those shown in Table , were developed either as monotherapies or combination therapies with L-DOPA for the treatment of PD. Five types of DA receptors, D1D5, exist in the brain. The D1 and D5 receptors are grouped together as D1-like receptors based on their stimulatory effects on adenylyl cyclase , and the D2, D3, and D4 receptors are classified as D2-like receptors due to their inhibition of cAMP activity. Many synthetic DA agonists, including pramipexole and apomorphine, activate D2-like receptors, and have a lower incidence of motor fluctuations and dyskinesia .
Multifunctional Agents With D3 Receptor Agonist And Antioxidant Activities
The Dutta group also developed novel multifunctional agents with D3-preferring agonist activity along with antioxidant activity, such as the selective full D3 agonists D440 , -34 , and -9b 2019-12-1933, and the selective partial D3 agonist -8b . D440 not only exhibits in vivo efficacy in rats with 6-OHDA-induced unilateral lesions but also protects dopaminergic MN9D cells from MPP+- and 6-OHDA-induced toxicity. Both -34 and -9b significantly increase locomotor activity in an animal model of reserpine-induced PD. Moreover, -9b also exhibits strong in vivo activity in rats with 6-OHDA-induced unilateral lesions and protects MN9D cells from MPP+-induced toxicity. Of note, -8b is a selective partial D3 agonist, but it also exhibits strong in vivo activity, both in reversing akinesia in reserpine-treated rats and inducing rotation in rats with 6-OHDA-induced unilateral lesions additionally, its activity is more potent than that of -9b. However, -8b shows no neuroprotective effects against MPP+-induced toxicity in MN9D cells.
Read Also: Sean Penn Parkinson’s Disease
How Can People Cope With Parkinson’s Disease
While PD usually progresses slowly, eventually daily routines may be affectedfrom socializing with friends to earning a living and taking care of a home. These changes can be difficult to accept. Support groups can help people cope with the diseases emotional impact. These groups also can provide valuable information, advice, and experience to help people with PD, their families, and their caregivers deal with a wide range of issues, including locating doctors familiar with the disease and coping with physical limitations. A list of national organizations that can help people locate support groups in their communities appears at the end of this information. Individual or family counseling may also help people find ways to cope with PD.
People with PD may also benefit from being proactive and finding out as much as possible about the disease in order to alleviate fear of the unknown and to take a positive role in maintaining their health. Many people with PD continue to work either full- or part-time, although they may need to adjust their schedule and working environment to accommodate their symptoms.