Parkinson’s Disease Symptoms: Life Expectancy
Even though Parkinson’s disease is a serious, progressive condition, it is not considered a fatal illness. People who have Parkinson’s disease usually have the same average life expectancy as people without the disease.
But when the disease is in its advanced stages, Parkinson’s symptoms can lead to life-threatening complications, including:
- Falls that lead to fractured bones
- Pneumonia
- Choking
Thinking about the progression of Parkinson’s disease can be frightening. But proper treatments can help you live a full, productive life for years to come. And researchers hope to one day find ways to halt the progression of Parkinson’s and restore lost functioning.
Stages Of Parkinsons Disease: Progression Of Parkinsons
The Parkinsons disease stages are well-known among doctors. If you are diagnosed with Parkinson’s, it’s important to be aware of these stages so you can prepare yourself and your family for the future. As the disease progresses, you may develop further needs or require full-time care. Find out everything you need to know about the five stages of Parkinsons disease and the progression of Parkinsons symptoms.
What Are The Non
Parkinson’s disease stages are defined by the severity of a patient’s motor symptoms and how much those symptoms impact one’s ability to function every day. But there are non-motor symptoms that are more likely to develop later in the disease, too, and a doctor may take those into consideration when assessing someone with the disorder.
For example, people with late-stage Parkinson’s disease might have difficulty chewing, eating, speaking, or swallowing , which is considered both a motor and non-motor symptom. Dysphagia in particular can lead to serious health problems like malnutrition, dehydration, and aspiration.
In the final stages of Parkinson’s disease, a person might develop cognitive changes, including slowness of memory or thinking, trouble planning and accomplishing tasks, and difficulty concentrating. Or they might notice changes in their bone health or vision.
But there’s no telling for sure if or when these symptoms will occur in any individual because Parkinson’s disease symptoms vary from person to person.
Don’t Miss: Coffee And Parkinson’s Protection In The Making
General Approach To Management
The primary goal in the management of PD is to treat the symptomatic motor and nonmotor features of the disorder, with the objective of improving the patients overall quality of life. Appropriate management requires an initial evaluation and diagnosis by a multidisciplinary team consisting of neurologists, primary care practitioners, nurses, physical therapists, social workers, and pharmacists., It is also important that the patient and his or her family have input into management decisions.
Effective management should include a combination of nonpharmacological and pharmacological strategies to maximize clinical outcomes. To date, therapies that slow the progression of PD or provide a neuroprotective effect have not been identified., Current research has focused on identifying biomarkers that may be useful in the diagnosis of early disease and on developing future disease-modifying interventions.,
If You Live In South Jersey And Have Questions About The Final Stages Of Parkinsons Disease Or Hospice Care For Your Loved One Please Call Samaritan At 229
Samaritan is a member of the National Partnership for Healthcare and Hospice Innovation, a network of not-for-profit hospice and palliative providers across the country. If you know someone outside of our service area who is living with advanced illness and can benefit from hospice or palliative care, please call 1 -GET-NPHI for a referral to a not-for-profit provider in your area.
Also Check: New Developments In Parkinson’s Disease Treatment
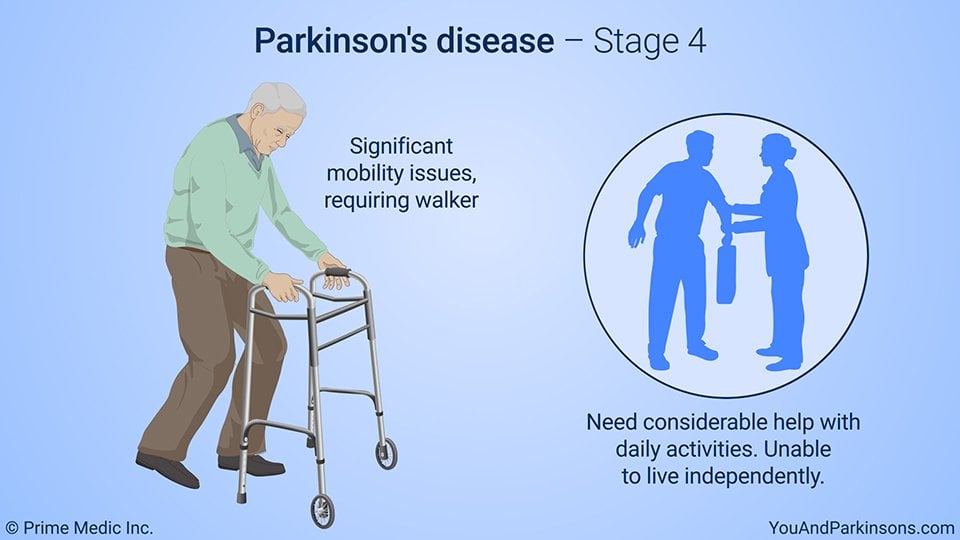
Stage Four Of Parkinsons Disease
In stage four, PD has progressed to a severely disabling disease. Patients with stage four PD may be able to walk and stand unassisted, but they are noticeably incapacitated. Many use a walker to help them.
At this stage, the patient is unable to live an independent life and needs assistance with some activities of daily living. The necessity for help with daily living defines this stage. If the patient is still able to live alone, it is still defined as stage three.
Unified Parkinsons Disease Rating Scale
The Unified Parkinsons Disease Rating Scale has four parts. Each part has multiple points that are individually scored, using zero for normal or no problems, 1 for minimal problems, 2 for mild problems, 3 for moderate problems, and 4 for severe problems.
These scores are tallied to indicate the severity of the disease, with 199 points being the worst and total disability and 0 meaning no disability.3
In 2001, the Movement Disorder Society updated the rating scale with involvement from patients and caregivers. The updated scale is referred to as the UPDRS-MDS, and it was published in 2008. It now includes the following sections:3
Also Check: What Medications Can Cause Parkinson’s
Can You Die From Parkinson’s
Advanced symptoms of a long-term condition like Parkinsons can make people more vulnerable to poor health and increased disability. These complications can sometimes result in someone dying. When this happens, Parkinsons can be recorded as a cause of death.
Complications can include:
- aspiration pneumonia
- falls
- chest infections and pneumonia
This is one of the reasons why its important to manage your condition as well as you can, with the support of specialist healthcare professionals.
Can Parkinsons Disease Be Prevented
Unfortunately, no. Parkinsons disease is long-term disease that worsens over time. Although there is no way to prevent or cure the disease , medications may significantly relieve your symptoms. In some patients especially those with later-stage disease, surgery to improve symptoms may be an option.
Don’t Miss: Speech Therapy For Parkinson’s Disease
What Are The 5 Stages Of Parkinson’s Disease
Parkinson’s disease is a neurological movement disorder that’s progressive, meaning symptoms worsen over time. According to the Parkinson’s Foundation, most people move through the stages of Parkinson’s disease gradually .
There’s no lab test that can tell a person which stage their disease is in. Instead, it’s based on how severe a person’s movement symptoms are, and how much the disease impacts their ability to go about daily life.
While the stages of Parkinson’s disease can look a little different for everyone, here’s a typical pattern of the disease, per the Parkinson’s Foundation:
Another View Of Parkinsons Progression
A newer theory of Parkinsons progression called Braak’s hypothesis suggests that Parkinsons may begin years before motor symptoms develop. According to Braaks hypothesis, loss of smell and digestive symptoms such as constipation are the earliest signs of Parkinsons, showing up many years before motor issues. While these early symptoms do not show up on an official Parkinsons stage yet, many researchers are working on ways to identify and treat Parkinsons earlier, even before stage one.
Condition Guide
Read Also: Israeli Treatment Of Parkinson Disease
Stage 5 Of Parkinsons Disease
In the final and most severe stage of Parkinsons disease, confusion, delusions and hallucinations may occur. Patients experience advanced stiffness in the legs and may freeze or stumble when attempting to walk. Around-the-clock assistance is needed, and many people require wheelchairs or are confined to a bed. At this stage, dementia also occurs in up to 75% of people with Parkinsons.
It bears repeating that the progression of the disease varies from individual to individual. For example, not everyone with Parkinsons disease will experience the severity of stage 5. While Parkinsons disease itself isnt fatal, the symptoms associated with it can be, such as injuries from falls, problems related to dementia or immobility leading to heart issues.
The Five Stages Of Parkinsons
The stages of Parkinsons are based on the Hoehn and Yahr scale introduced in 1967. The Hoehn and Yahr staging system focuses on disability caused by motor symptoms such as bradykinesia , tremor, and loss of balance. Some neurologists also use a newer scale called the Unified Parkinsons Disease Rating Scale . The UPDRS scale takes into account changes in mood, cognitive function such as thinking and remembering, and social behavior.
Don’t Miss: Big And Loud Therapy For Parkinson’s
Stage 2 Of Parkinsons Disease
During stage 2, Parkinsons disease symptoms are much more noticeable. At this point, the disease begins to affect your entire body. Changes in facial expressions, speech abnormalities and increased tremors or stiffness may occur. Routine daily activities take longer to complete and posture changes are more visible. Stage 2 may occur months or even years after stage 1.
Parkinsons Disease Late Stage Complications
During the most advanced stage of Parkinsons typically between stages four and five a persons symptoms and medication regime become more complex.
Supporting care becomes especially important in advanced Parkinsons, with an estimated 50 to 80% of people eventually experiencing dementia and an increased number of falls.
Read Also: Can You Drive If You Have Parkinson’s Disease
What Are The Five Stages Of Parkinson’s Disease
Researchers may disagree on the number of stages of Parkinsons disease . However, they all agree the disease is a progressive disease with symptoms that usually occur in one stage may overlap or occur in another stage. The stage increase in number value for all stage naming systems reflect the increasing severity of the disease. The five stages used by the Parkinsons Foundation are:
- Stage 1: mild symptoms do not interfere with daily activities and occur on one side of the body.
- Stage 2: Symptoms worsen with walking problems and both sides of the body affected.
- Stage 3: Main symptoms worsen with loss of balance and slowness of movement.
- Stage 4: Severity of symptoms require help usually person cannot live alone.
- Stage 5:Caregiver needed for all activities patient may not be able to stand or walk and may be bedridden and may also experience hallucinations and delusions.
A neurologist who specializes in movement disorders will be able to make the most accurate diagnosis. An initial assessment is made based on medical history, a neurological exam, and the symptoms present. For the medical history, it is important to know whether other family members have Parkinson’s disease, what types of medication have been or are being taken, and whether there was exposure to toxins or repeated head trauma previously. A neurological exam may include an evaluation of coordination, walking, and fine motor tasks involving the hands.
The diagnosis of Parkinson’s disease is more likely if:
Medicines For Parkinson’s Disease
Medicines prescribed for Parkinson’s include:
- Drugs that increase the level of dopamine in the brain
- Drugs that affect other brain chemicals in the body
- Drugs that help control nonmotor symptoms
The main therapy for Parkinson’s is levodopa, also called L-dopa. Nerve cells use levodopa to make dopamine to replenish the brain’s dwindling supply. Usually, people take levodopa along with another medication called carbidopa. Carbidopa prevents or reduces some of the side effects of levodopa therapysuch as nausea, vomiting, low blood pressure, and restlessnessand reduces the amount of levodopa needed to improve symptoms.
People with Parkinson’s should never stop taking levodopa without telling their doctor. Suddenly stopping the drug may have serious side effects, such as being unable to move or having difficulty breathing.
Other medicines used to treat Parkinsons symptoms include:
- Dopamine agonists to mimic the role of dopamine in the brain
- MAO-B inhibitors to slow down an enzyme that breaks down dopamine in the brain
- COMT inhibitors to help break down dopamine
- Amantadine, an old antiviral drug, to reduce involuntary movements
- Anticholinergic drugs to reduce tremors and muscle rigidity
Read Also: Parkinson’s Lewy Body Dementia Life Expectancy
Stages Of Parkinsons Disease
Parkinsons disease affects people differently. Though everyone with PD will experience slowness of movement and stiffness, not everyone will experience the full range of possible symptoms.
The presence and severity of symptoms, both motor and non-motor, and their progression varies greatly between people with PD. This variation makes it difficult to grade the severity of PD. The following classification of stages is one that is easy to apply in the clinical setting.
Parkinsons disease is seen to progress through 4 broad clinical stages. The speed of this progression varies between people and may see some people not progressing to stage 4.
Early stage of the disorder is when symptoms are mild and initially affect one side of the body. The common motor symptoms include tremor, slowness of movement in the leg or arm on one side, stiffness and decreased facial expression. The person is still able to perform their usual activities and they are fully independent, unless they have another health condition. Symptoms are well controlled by medications. This period usually lasts for a maximum of 5 years from the time of diagnosis.
Late stage sees the person severely disabled by their symptoms. Falls risk is very high and a walking aid is usually needed all of the time. They need assistance to remain at home. Non-motor symptoms, such as hallucinations, generally worsen in the late stage.
Change Language
Are There Any Factors That Slow Or Increase The Pace Of Parkinsons
Though there is currently no drug to halt the progression of the Parkinsons, there are some factors that can alter how quickly it develops. There is a growing body of evidence to suggest that regular exercise and healthy eating can slow the progression of Parkinsons, says Dr Stott.
For example, researchers in the Netherlands have recently demonstrated in a randomised clinical trial that six months of exercising slowed the progression of 65 people with Parkinsons .
Inactivity and social isolation also appear to be associated with faster progression, hence the need to encourage affected individuals to partake in regular exercise ideally in a social environment, he adds.
An investigation into the genetics of Parkinsons shows some promise as to explaining the difference in progression among patients. Dr Stott explains: There is evidence indicating that some genetic variations can influence the speed of progression some variations are associated with increased rate of progression, while others result in a slower rate. We are not sure why these genetic variations are having these effects, but the biology is currently being explored.
You May Like: Can You Be Tested For Parkinson’s
Parkinson’s Disease Diet And Nutrition
Maintaining Your Weight With Parkinson’s Disease
Malnutrition and weight maintenance is often an issue for people with Parkinson’s disease. Here are some tips to help you maintain a healthy weight.
- Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily.
- If you have an unexplained weight gain or loss , contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition.
- Avoid low-fat or low-calorie products. . Use whole milk, whole milk cheese, and yogurt.
What Can You Do For Someone Who Has Parkinsons Disease

If you want to offer help to an individual suffering from Parkinsons disease, you should:
- Know and learn everything about Parkinsons disease to fully understand the condition of the person.
- Do volunteer when they need some assistance and take note of their symptoms. Notice if they get worse over time.
- Listen and be patient with their recovery.
- Help them get some fun to make them feel normal.
You May Like: Is Beer Good For Parkinson’s
How Can Inpatient Rehabilitation Help
As a senior physical therapist at Encompass Health Fayetteville, Hammel works with Parkinsons patients at various stages of the disease. He said inpatient rehabilitation for Parkinsons can benefit even those who are only experiencing Parkinsons early signs and symptoms.
Honestly, I would say the moment you are diagnosed, rehabilitation can help, he said. Once youre diagnosed, one of the best things you can do is therapy. We can help with education and trying to regain independence or modify how you used to do things.
At an inpatient rehabilitation hospital such as Encompass Health, you will receive three hours of therapy five days a week, along with frequent visits from a rehabilitation physician. Occupational therapy can help you with activities of daily living, such as eating and grooming, physical therapy can help you build strength and balance, and speech therapy can help with speech and swallowing, as well as cognitive issues.
The goal of rehabilitation for Parkinsons patients, Hammel added, is to allow you to remain independent at home for as long as possible. If you or a loved one was recently diagnosed with Parkinsons disease or is experiencing more progressed symptoms, find an Encompass Health location near you, and talk to a rehabilitation specialist to see if inpatient rehabilitation could benefit you.
What Is A Rating Scale
A rating scale is a means of providing information on a particular feature by assigning a value to it. In Parkinsons, rating scales require the rater to put a value to the feature or symptom in question, according to a set scale. The rater may be the person with Parkinsons or a healthcare professional.
Parkinsons rating scales are a means of assessing the symptoms of the condition. They provide information on the course of the condition and/or assess quality of life. They may also help to evaluate treatment and management strategies, which can be useful to researchers as well as to people with Parkinsons, their carers and medical team.
Motor scales are the best-known and most widely used, but non-motor symptom scales are equally important. Combined with a motor scale, these give a more balanced picture of how a person is affected by the condition. A low motor score may suggest that a person has mild Parkinsons but, at the same time, the person may have disabling non-motor symptoms, which impact on quality of life.
Recommended Reading: Physiotherapy Management For Parkinson’s Disease Ppt
Confinement To Bed Or Wheelchair Unless Aided
The patient may exhibit: inability to arise from a chair or get out of bed without help a tendency to fall when standing or turning freezing, stumbling or pulsion when walking. Without someone immediately present to provide assistance, the patient is in danger of falling.A typical example of diagnosis using this method of staging would be: a 64 year old with Stage III PD, more marked on the left than the right, of seven years duration. Another would be: A 55 year old with severe fluctuations in response to Sinemet, with PD of Stages II/IV, of ten years duration. The second example indicates that the patient is at Stage II when at his best or on and at stage 3 IV when at his worst or off. This gives the reader a succinct description of the progression of the disease and the current status of the patient.This method of grading severity is rather a potpourri, combining the symptoms of the patient, the physical signs as observed by the physician and the patients functional ability. In some instances, it is not applicable. For example, while general experience has been that is the onset of disturbances of balance that heralds future disability, some patients may have such severe tremor that they are incapacitated even though balance in intact. Others may have mild disturbance of balance for many years without losing independence. There are occasional patients who are more incapacitated by severe unilateral disease than are others by milder bilateral disease.