Surgical Therapies With Transplantation And Gene Therapy
Cell transplantation is regarded as a potential future PD treatment. There have been trials using autologous and non-autologous cells. Human embryonic stem cells and induced pluripotent stem cells are few of the cells that have been included in these transplantation studies. One of the concerns with cell transplantation using stem cells is the ethical bounds that must be considered.
Since the first clinical trial in 1987 involving the transplantation of dopaminergic- neuron-rich human fetal mesencephalic tissue into PD patients striatums, more research has aimed to explore whether the grafted dopaminergic neurons will live and form connections in the brain, if the patients brain can harmonize and make use of the grafted neurons, and if the grafts can generate significant clinical improvement. Clinical trials with cell therapy intend to discover if there are long-lasting improvements following restoration of striatal DA transmission by grafted dopaminergic neurons. Experimental data from rodents and nonhuman primates show that fetal ventral mesencephalon intrastriatal grafted DA neurons demonstrate many morphological and functional characteristics of normal DA neurons. Significant improvements of PD-like symptoms in animal models have been demonstrated after successful reinnervation by the grafts. Dopaminergic grafts can reinnervate the striatum in the brain, restore regulated release of DA in the striatum, and can become functionally integrated into neural circuitries.
Parkinsons Treatment For Motor Symptoms
The majority of medications developed specifically to treat Parkinsons disease target common motor symptoms. Many of these treatments are designed to increase the level of the dopamine, a neurotransmitter that transfers signals between nerve cells. Dopamine is involved in regulating signals for movement, which is reduced in the brains of Parkinsons disease patients.
When Is It Best To Start The Parkinsons Drug Levodopa
Earlier treatment with levodopa provides symptomatic relief to those with symptoms but does not appear to slow Parkinsons disease from progressing. Therefore, timing is best determined by symptoms.
The treatment of Parkinsons disease is complex. Levodopa is the main drug used to reduce tremors and muscle stiffness. Whether it modifies the course of the disease or becomes less effective over time is debated, and it can have side effects, so patients and clinicians sometimes prefer to delay starting treatment.
This Dutch trial involved 445 participants with a recent diagnosis of Parkinsons disease, enrolled over five years. About half took levodopa for 80 weeks, and half placebo for the first 40 weeks and levodopa for the last 40 weeks. There was no difference in symptoms between the groups at the end of the study.
This evidence supports current guidance to start levodopa when symptoms begin to affect the quality of life and confirm that it has insufficient impact on disease progression to justify earlier treatment.
You May Like: What Does Parkinson’s Feel Like
The Characteristics And Treatment Patterns Of Patients With Parkinsons Disease In The United States And United Kingdom: A Retrospective Cohort Study
-
Roles Conceptualization, Formal analysis, Methodology, Writing review & editing
Affiliation UCB Pharma, Slough, United Kingdom
-
Roles Conceptualization, Formal analysis, Methodology, Writing review & editing
Affiliation UCB Pharma, Slough, United Kingdom
-
Roles Conceptualization, Methodology, Writing review & editing
Affiliation UCB Pharma, Raleigh, North Carolina, United States of America
What Did It Find
- According to the UPDRS score, there was no difference in the progress of disease between the early-start group and the delayed-start group , .
- The estimated rate of change in progression of the disease, a secondary outcome, was similar in both groups between 4 and 44 weeks .
- Due to needing symptomatic relief, 87 people in the delayed-start group had levodopa before week 40.
- The estimated rate of change in progression was faster between weeks 44 and 80 in the early-start group . This means starting levodopa earlier did not slow disease progression.
- At 80 weeks, a similar proportion of participants were suffering complications, such as involuntary movements, from levodopa treatment .
Also Check: Flexibility Exercises For Parkinson’s Disease
Treatment Of Neurobehavioral Features
Treatment of cognitive deficits associated with PD is as challenging as the treatment of Alzheimers disease and other dementias. While the general assumption has been that cognitive deficits are a feature of late-stage PD, clinically inapparent cognitive changes on neuropsychiatric testing may be found . With the introduction of cholinesterase inhibitors such as donepezil , rivastigmine , and galantamine and the NDMA antagonist memantine , it is possible that cognition, orientation and language function will improve, and that such improvement will lead to a meaningful improvement in function. Both donepezil and rivastigmine improve cognition to the same effect, but donepezil is better tolerated . The largest and best-designed study of rivastigmine in dementia associated with PD involved 541 patients enrolled in a 24-week randomized, multicenter, double-blind clinical trial . The patients had a relatively mild dementia , with onset of dementia about 2 years after onset of PD symptoms. The mean ADAS-cog score, the primary efficacy variable, improved by 2.1 points in the rivastigmine group, compared to 0.7 in the placebo group , and the MMSE improved by 0.8 in the rivastigmine group and worsened by 0.2 in the placebo group . At the end of the study, 55.5% were receiving 9 to 12 mg. The adverse effects that were significantly more frequent in the rivastigmine group were nausea, vomiting, dizziness, and tremor.
Pathogenesis Of Parkinsons Disease
According to National Institute of Neurological Disorders and Stroke, the pathogenesis of PD involves overlapping mechanisms of excitotoxicity, calcium accumulation within cells, increased ROS production, mitochondrial defects, cytoskeletal abnormalities, and aberrations in nerve growth factors.17 It is postulated that normal aging of neural cells may also be driven by some of these mechanisms, in particular the accumulation of ROS that leads to apoptotic pathway activation.18 The late onset of neurodegenerative diseases in general is corroborating evidence for the possible role of ROS accumulation in neurodegenerative diseases.
Metabolism of dopamine is only one of many cellular processes that are producing free radicals in neural cells. Many normal cellular processes, most notably energy generation within the mitochondria, result in the production of several types of free radicals, including superoxide anion, hydrogen peroxide and hydroxyl. Excitotoxicity, whether by endogenous glutamate or exogenous toxins, is also a known contributor of ROS generation within cells. Higher free iron levels, which are found in patients with PD, also promote oxidation and result in the production of free radicals. CoQ10 acts as a potent antioxidant within cells and may help to reduce oxidative damage to the mitochondrial membrane, thus protecting cells from ROS driven triggers of apoptosis.21
Recommended Reading: Is Massage Good For Parkinson’s
The Evolution Of Treatments
The history of Parkinson’s disease is tightly linked to therapeutic interventions, ranging from serendipitous observations to controlled clinical trials of specifically designed agents.
Parkinson devoted a chapter of his monograph to considerations respecting the means of cure . In humility and perhaps with a vision toward current concepts of neuroprotection, he hoped for the identification of a treatment by which the progress of the disease may be stopped . To this end, he advocated very early therapeutic intervention when signs were largely confined to the arms without balance and gait impairments. Reflecting therapeutic approaches of the early nineteenth century, Parkinson recommended venesection, specifically advocating bloodletting from the neck, followed by vesicatories to induce blistering and inflammation of the skin. Small pieces of cork were purposefully inserted into the blisters to cause a sufficient quantity of purulent discharge . All these efforts were designed to divert blood and inflammatory pressure away from the brain and spinal cord, and in this way, decompress the medulla that Parkinson considered the seat of neurological dysfunction.
Inhibikase Doses First Subject In Phase Ib Parkinsons Treatment Trial
The trial will evaluate the safety, pharmacokinetics and tolerability of IkT-148009 in 24 Parkinsons patients.
Inhibikase Therapeutics has commenced dosing of the first subject in the Phase Ib clinical trial of its drug, IkT-148009, to treat Parkinsons disease, a neurodegenerative disorder that is progressive.
IkT-148009 is an inhibitor of Abelson Tyrosine Kinase or c-Abl, a clinically established target that is triggered on affected neurons in the brain and gut internalising plaques of alpha-synuclein.
The randomised, placebo-controlled Phase Ib extension trial will analyse the safety, pharmacokinetics and tolerability of IkT-148009 in Parkinsons patients assessed over seven to 14 days.
It will have 24 subjects categorised into a 3:1 ratio to receive one of the three escalating doses of IkT-148009.
Inhibikase previously submitted the interim 13-week toxicology study data to the US Food and Drug Administration, which subsequently reviewed and accepted the firms plans to dose subjects for three months.
Exploratory goals of the trial will include cognitive and motor function, as well as gut motility and alpha-synuclein aggregate clearance measures in various compartments.
As we look ahead, we anticipate completing this study and advancing into a Phase IIa study in 2022.
According to data from the Phase I trial in 56 healthy elderly subjects, IkT-148009 attained greater drug exposure between 12.5-100mg without any clinically substantial adverse events reported.
Recommended Reading: Cluster Headaches Parkinson’s Disease
Basics Of Parkinsons Disease
Parkinsons disease , or paralysis agitans, is a common neurodegenerative condition, which typically develops between the ages of 55 and 65 years. This disease was first named and described by James Parkinson in 1817. The progression of this disease is gradual and prolonged. It has a plausible familial incidence, although the estimates of these occurrences are low and usually sporadic. This disease is organized into two classifications: genetic and sporadic. Genetic PD follows Mendelian inheritance. Sporadic PD, which accounts for about 90% of all Parkinsons cases, is a more complex category in which the pathogenic mechanisms that underlie it are not yet fully understood. Nonetheless, it is known that the byzantine interactions of genetic and environmental influences play roles in the determination of sporadic PD. Several subtypes of PD exist. Each has its own set of causative factors and susceptibilities, pathology, and treatment courses. General risk factors, symptoms, and pathology will be discussed first, before addressing some of the subtypes.
Anticholinergics For Early On
The first pharmacological agents used in PD therapy were anticholinergic drugs. They reduce the activity of acetylcholine by acting as antagonists at choline receptors, hoping to restore the balance between dopamine and acetylcholine levels that was disturbed by PD. These drugs have largely been replaced by L-DOPA and other centrally acting dopaminergic agonists, but they still remain available for use in the treatment of PD. Benztropine, biperiden, diphenhydramine, ethopropazine, orphenadrine, procyclidine, and trihexyphenidyl are included in this therapeutic class of drugs, though there is little pharmacokinetic information available on them because of their low plasma drug concentrations. Typically, anticholinergic drugs have a greater role in tremor-predominant PD and can be a monotherapy in early stages, but are usually done in adjunct with L-DOPA or other prescribed medications.
Read Also: Parkinson’s Help For Caregivers
Pharmacological Advances: Charcot And Gowers
Early treatment of Parkinson’s disease. Prescription dated 1877 from the College of Physicians of Philadelphia Library. In treating Parkinson’s disease, Charcot used belladonna alkaloids as well as rye-based products that had ergot activity, a feature of some currently available dopamine agonists. Charcots advice was empiric and preceded the recognition of the well-known dopaminergic/cholinergic balance that is implicit to normal striatal neurochemical activity .
Everything, or almost everything, has been tried against this disease. Among the medicinal substances that have been extolled and which I have myself administered to no avail, I need only enumerate a few .
Choosing The Best Treatment Plan For You
As you may know, medications are the backbone of the Parkinsons treatment plan. But because the disease affects everyone differently, and each persons response to therapy will vary, there is no hard-and-fast rule about when you should begin taking medication and what to take first. Some doctors prescribe medication upon diagnosis. Others believe that drugs, especially levodopa, should be delayed as long as possible to avoid earlier onset of medication-related side effects.
Your involvement from the very start is important because you want to be sure your doctor is addressing your individual needs. When your doctor writes a new prescription, or makes a change to an existing one, take the opportunity to ask for an explanation. If her response goes something like, I always start my Parkinsons patients on X dosage of Y, a dopamine agonist, you might want to consider switching to a movement disorders specialist, a neurologist who has had special training in Parkinsons disease and other movement disorders.
You May Like: What Is Bradykinesia In Parkinson’s
Family History Tops List Of Risk Factors For Pd
While PD occurs in less than 1% of the population 40 years of age, its prevalence increases with age, becoming significantly higher by age 60 years, with a slight predominance toward males.4
A variety of factors increase the risk of developing PD. A well-conducted meta-analysis showed that the strongest risk factor is having a family member, particularly a first-degree relative, with a history of PD or tremor.5 Repeated head injury, with or without loss of consciousness, is also a factor 5 risk increases with each occurrence.6 Other risk factors include exposure to pesticides, rural living, and exposure to well water.5
Researchers have conducted several studies regarding the effects of elevated cholesterol and hypertension on the risk of PD, but results are still without consensus.5 A study published in 2017 reported a significantly increased risk of PD associated with having hepatitis B or C, but the mechanism for the associationincluding whether it is a consequence of treatmentis unknown.7
The Palliative Care Offered Can Be Improved
Region Skåne is participating in the study and funding it, which is expected to be completed in the spring and be evaluated next year.
Many of these patients are not receiving adequate treatment. There is a whole lot that needs to be improved and we are also building in the palliative concept. It may sound sad, but it is positively meant that in the final phase of the disease, the focus is no longer on maximum mobility but on the patients quality of life, which includes medication, provision of nutrition, where the patient should reside and additional related matters. The treatment of the non-motor symptoms becomes even more important in these stages, stresses Per Odin.
Region Skåne has shown significant interest in the concept and sees it partly as a pilot project and then later a model for the university hospitals to reach out to patients to a greater degree than has occurred so far. A model that can also be used with other diseases and disorders with similar problems.
These disease groups, perhaps eventually all people, should have the right to palliative therapies at the end of life. If people knew they would be well cared for, I think much of the anxiety for the latter parts of life and finally death would diminish a bit. We are focusing on Parkinsons disease, however I believe that our palliative work can serve as a model in the work with many other diseases.
Also Check: Do Parkinson’s Patients Get Violent
Aan Releases Recommendations On Treatment Of Parkinson’s Disease
Am Fam Physician. 2007 Mar 15 75:922-924.
-
Guideline source: American Academy of Neurology
-
Literature search described? Yes
-
Evidence rating system used? Yes
-
Available at:
Parkinson’s disease is the second most common neurodegenerative disease and is characterized by bradykinesia tremor at rest rigidity and abnormalities of balance, posture, and gait. Its etiology remains unknown in most patients. Recommendations from the Quality Standards Subcommittee of the American Academy of Neurology discuss the following aspects of this condition in a collection of articles in the April 2006 issue of Neurology: diagnosis and prognosis neuroprotective strategies and alternative therapies treatment and evaluation and treatment of depression, psychosis, and dementia in patients with Parkinson’s disease.
Initial Drug Treatment In Parkinsons Disease
The bottom line
-
First line treatments for Parkinsons disease include levodopa, non-ergot dopamine agonists, and monoamine oxidase B inhibitors
-
Consider starting levodopa treatment in all patients, especially those with serious motor impairment or cognitive impairment
-
Monitor for motor complications and impulsivity and adjust doses accordingly
-
Do not stop treatment abruptly because this may cause malignant hyperthermia
A 69 year old retired bus driver with no medical history of note presented to the outpatients department with a three year history of progressive tremor of the right hand slowness of movement and difficulty turning in bed at night, buttoning shirts, and using cutlery. He is keen to know what is wrong and whether it can be treated.
Read Also: Cleveland Clinic Parkinson’s Doctors
Medication Guidelines For Parkinson’s Disease
There is no one best mix of Parkinsonâs medicines. You and your doctor will have to try a few treatment approaches to figure out the best one for you.
But there are some general guidelines for taking your medication. Be sure to ask your doctor or pharmacist for any specific tips for your treatment.
Second Brain Becomes The First Line Of Defense
Neuroprotective and anti-inflammatory effects of hormone modulation treatment of the enteric nervous system in Parkinsons disease
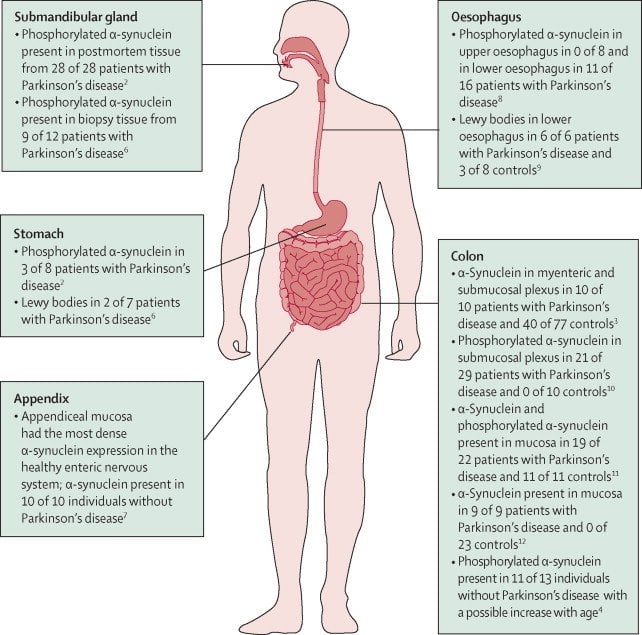
The intricate features of the gastrointestinal system are so sophisticated that medical researchers refer to this as the bodys second brain. That description may be especially appropriate for researchers examining Parkinsons disease, since it is likely this condition may originate in the gut and emerge through digestive problems rather than the better-known symptoms involving stiffness, tremors and other movement disorders.
There are a lot of non-motor symptoms that might appear as early as 20 years before motor symptoms emerge, says Andrée-Anne Poirier, a doctoral candidate and researcher at Laval University. Thats why we think that the disease begins in the periphery before the brain.
Poirier believes Parkinsons disease may begin to kill dopamine-producing brain cells after a pathogen or environmental toxin enters the intestinal tract, initiates the disease process and then moves to the brain through the vagus nerve. The vagus nerve is the longest cranial nerve and extends from the abdomen to the brainstem.
Poirier has been investigating ways to create this neuroprotection without the side effects. The search has led her to test raloxifene, a drug initially approved by Health Canada to treat osteoporosis in menopausal women.
Search
Don’t Miss: How Does Occupational Therapy Help Parkinson Disease