What Are The Symptoms Of Parkinsons Disease
Symptoms of Parkinsons disease and the rate of decline vary widely from person to person. The most common symptoms include:
Other symptoms include:
- Speech/vocal changes: Speech may be quick, become slurred or be soft in tone. You may hesitate before speaking. The pitch of your voice may become unchanged .
- Handwriting changes: You handwriting may become smaller and more difficult to read.
- Depression and anxiety.
- Sleeping disturbances including disrupted sleep, acting out your dreams, and restless leg syndrome.
- Pain, lack of interest , fatigue, change in weight, vision changes.
- Low blood pressure.
What Are The Later Secondary Signs And Symptoms Of Parkinson’s Disease
While the main symptoms of Parkinson’s disease are movement-related, progressive loss of muscle control and continued damage to the brain can lead to secondary symptoms. These secondary symptoms vary in severity, and not everyone with Parkinson’s will experience all of them, and may include:
Parkinsons Disease Life Expectancy
Most people with Parkinsons can have a normalor close to normallife expectancy today, thanks to new medications, therapies, and other treatments. Survival rates for those with typical Parkinsons disease are either the same as for the general population or shortened by about a year, studies show.
Risk factors for earlier mortality with Parkinsons include:
-
Being diagnosed before age 70
-
Having early in the disease
-
Developing Parkinsons
People with Parkinsons dont die from the disease itself, but from associated complications, such as infections or injuries . Cardiovascular disease is another common cause of death.
Treatments and lifestyle improvements, can help forestall cognitive decline, lower your risk of falls and strengthen your cardiovascular system. These can help improve your quality of life and, by slowing progression of the illness, potentially keep you living longer.
Researchers are continuing to explore new treatments that they hope will one day lead to better therapies for Parkinsons, which will result in an improved prognosis.
Don’t Miss: What Is Drug Induced Parkinson’s Disease
What Happens In Stage 5 Parkinson’s
Stage 5Stage 5stageParkinson’s
. In respect to this, what is end stage Parkinson’s?
When patients reach stage five the final stage of Parkinson’s disease they will have severe posture issues in their back, neck, and hips. In end–stage of Parkinson’s disease, patients will also often experience non-motor symptoms. These can include incontinence, insomnia, and dementia.
Beside above, how long does a person live with stage 5 Parkinson’s? Parkinson’s Disease is a Progressive DisorderIndividuals with PD have a somewhat shorter life span compared to healthy individuals of the same age group. Patients usually begin developing the disease around age 60, and many live between 10 and 20 years after being diagnosed.
Thereof, what happens in stage 5 of Parkinson’s disease?
Stage Five of Parkinson’s DiseaseStage five is the most advanced and is characterized by an inability to arise from a chair or get out of bed without help. They may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
What do Parkinson’s patients usually die from?
But the most common cause of death in those with Parkinson’s is pneumonia, because the disease impairs patients‘ ability to swallow, putting them at risk for inhaling or aspirating food or liquids into their lungs, leading to aspiration pneumonia.
First Signs Of Impaired Righting Reflexes This Is Evident As The Patient Turns Or Is Demonstrated When He Or She Is Pushed From Standing Equilibrium With The Feet Together And Eyes Closed

Loss of balance, with the inability to make the rapid, automatic and involuntary movements necessary to protect against falling, is one of the most troubling and dangerous aspects of Parkinsonism and one of the least easily treated. Even when manifested by only slight unsteadiness, it is the criterion separating Stage II and Stage III. All other aspects of Parkinsonism are evident and usually diagnosis is not in doubt.
However, the most important factor identifying Stage III is that the patient is still fully independent in all activities of daily living Although somewhat restricted, has work potential depending upon the type of employment. A normal life can be.
Recommended Reading: Final Stages Of Parkinson’s Disease
What You Can Do
As of 2021, there is no definite cure for Parkinsons disease. There is also no definite known cause. Its likely due to a combination of an individuals susceptibility and environmental factors. Most cases of Parkinsons disease happen without a genetic link.
According to research published in 2012, only report having a family member with the disease. Many toxins are suspected and have been studied, but no single substance can be reliably linked to Parkinsons.
However, research is ongoing. Its estimated that
Myth : Parkinsons Disease Is Fatal
Fact: Although a diagnosis of Parkinsons is devastating, it is not as some people may still believe a death sentence. Parkinsons disease is not a direct killer, like stroke or heart attack. That said, much depends on the quality of your care, both from your medical team and yourself.
As the disease progresses, you may become more vulnerable to falls, which can be dangerous. Thats why exercise and physical therapy are so important.
Infection is another problem. In later stages of Parkinsons, people often miss those signals and may not notice somethings up until its too late. That can be, literally, a killer so be sure to stay up to date with checkups.
Read Also: Parkinson’s Disease Cause And Symptoms
What Are The Stages Of Parkinson’s Disease
Parkinson’s disease is a progressive neurological disorder. There are five generally recognized stages of Parkinson’s disease. The progression of the disease may vary from one patient to the next, and not all patients will experience all five stages of Parkinson’s disease in their generally accepted order. Symptoms may also vary throughout the progression of Parkinson’s disease.
While doctors have currently identified five distinct stages of Parkinson’s disease, not all patients will experience a straightforward disease progression that passes through all five stages, one after the other. Nor will all patients remain in all stages for the same length of time. The five stages of Parkinson’s often vary in duration from patient to patient. Disease progression is generally considered impossible to predict, with some patients experiencing all stages while other patients skipping from an early stage to an advanced stage without passing through the stages in between.
What Is Parkinsons Disease
Parkinsons is a neurological illness caused by degeneration or breaking down of cells in the nervous system, explained Dr. Shprecher. The nature of Parkinsons Disease is progressive, meaning that it gets worse over time. To comprehend the natural progression of the disease, we should understand its five stages, as explained by the Parkinsons Foundation.
Stage One
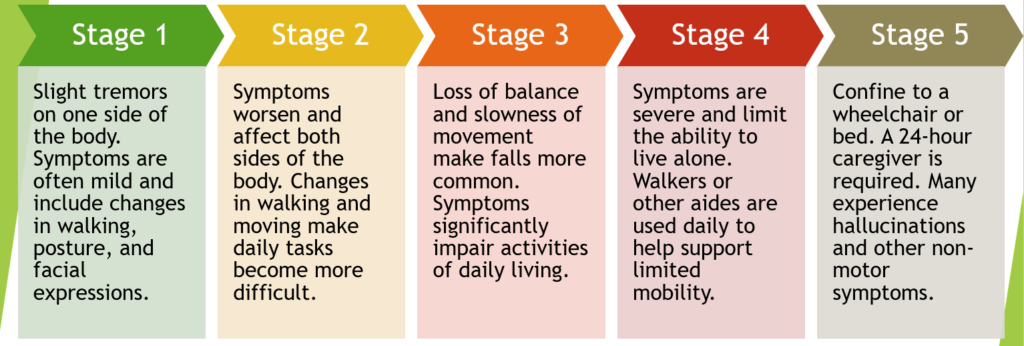
Individuals experience mild symptoms that generally do not interfere with daily activities. Tremor and other movement symptoms occur on one side of the body only. They may also experience changes in posture, walking and facial expressions.
Stage Two
Symptoms worsen, including tremor, rigidity and other movement symptoms on both sides of the body. The person is still able to live alone, but daily tasks are more difficult and lengthier.
Stage Three
This is considered mid-stage. Individuals experience loss of balance and slowness of movements. While still fully independent, these symptoms significantly impair activities such as dressing and eating. Falls are also more common by stage three.
Stage Four
Symptoms are severe and limiting. Individuals may stand without help, but movement likely requires a walker. People in stage four require help with daily activities and are unable to live alone.
Stage Five
Recommended Reading: Prostate Cancer And Parkinson’s Disease
Challenges To Classify Disease Stages At The Boundary Of Advpd And Atypical Parkinsonism
During disease progression and based on the predominant motor and non-motor features associated with advPD, the separation from atypical parkinsonism may be difficult and overlap syndromes like minimal change multiple system atrophy or progressive supranuclear palsy with predominant parkinsonism have been described . AP includes a heterogeneous bunch of syndromes, all characterized by clinically manifest parkinsonism in combination with other clinical features and a poor therapeutic response to dopaminergic medication. Only post-mortem analyses can clearly differentiate from advPD, as their neuropathology is characteristically different: in MSA, alpha-synuclein accumulation is found and defines an alpha-syncleinopathy as PD, but mainly in glial cells as cytoplasmic inclusions . In contrast, PSP and corticobasal degeneration are referred to as tauopathies due to characteristic intraneuronal tau aggregation and some TDP-43 proteinopathies might also develop clinical parkinsonism .
In this context, technical tests might further improve the quality of differential diagnosis. Autonomous tests, such as tests for cardiovascular, urinary, thermoregulatory or gastrointestinal dysfunction can be helpful for the diagnostic differentiation PD versus AP. Due to a marked overlap, the combination of several tests such as urodynamic investigation, tests for orthostatic dysregulation, RR-intervals and sympathetic skin response can contribute to support the correct diagnosis.
What Is Your Advice For People With Parkinsons Who Are Preparing For End Of Life
It is very important for people with Parkinsons disease and their families to be informed. They must recognise the personal needs that need to be managed, and consider incorporating palliative care.
For the best care, trustworthy multidisciplinary support can be very helpful particularly from healthcare professionals who specialise in solving broad-based problems. This might include a movement disorder physician, nurse, physiotherapist, occupational therapist, speech therapist or, importantly, a psychologist or chaplain to help manage psychosocial and spiritual problems, taking into consideration cultural and social specificities.
Recommended Reading: Stage 2 Parkinson’s Disease
How Can Palliative Care Help People With Parkinsons
Even with optimal medical support, the problems that people face in later stages of Parkinsons disease might be difficult to treat. They may in turn lead to a decrease in quality of life, increased burden to caregivers, distress for families, higher rates of emergency hospital admissions and extensive social and care services. A new concept is that people with Parkinsons disease may need variable palliative care applications in different stages of the disease, and suggests the need for early recognition and intervention.
This makes it essential for people with the condition to have reliable information and emotional support from a Parkinsons disease team. This support may include discussions on expectations for future, planning of advanced care, and arranging of end of life activities which take into account individual cultural background. Individual and proactive support would help to manage the progressive condition based on personal needs.
Dr Pille Taba.
Stage Two Of Parkinsons Disease
Stage two is still considered early disease in PD, and it is characterized by symptoms on both sides of the body or at the midline without impairment to balance. Stage two may develop months or years after stage one.
Symptoms of PD in stage two may include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities, soft voice, monotone voice, fading volume after starting to speak loudly, slurring speech, stiffness or rigidity of the muscles in the trunk that may result in neck or back pain, stooped posture, and general slowness in all activities of daily living. However, at this stage the individual is still able to perform tasks of daily living.
Diagnosis may be easy at this stage if the patient has a tremor however, if stage one was missed and the only symptoms of stage two are slowness or lack of spontaneous movement, PD could be misinterpreted as only advancing age.
Also Check: What Is The Difference Between Parkinson’s And Huntington’s Disease
Complications In Advanced Pd
While worsening of motor function and drug-induced motor complications represents a major challenge in patients with mid-stage to advanced disease, in the advanced stage of PD the most troublesome and distressful complications are usually nonmotor symptoms, including psychiatric and cognitive disorders, autonomic disturbances, and sleep disorders that significantly increase the need for supportive care. Unfortunately, these symptoms are frequently neglected in clinical practice due to limited consultation time, perception of the patient and caregivers that their symptoms are unrelated to the disease, or insufficient awareness of the clinicians, who generally focus on motor symptoms .
Proper supporting care becomes increasingly important in advanced PD. Rehabilitative and support services for patients and family become key interventions as the disease reaches its more debilitating stages and pharmacologic or surgical treatment becomes less relevant. Management of motor and nonmotor complications in advanced PD requires careful and ongoing assessment of whether symptoms are a side effect of medication or related to the progression of the disease .
Medication Issues
|
End of Dose Wears Off Symptoms in Advanced PD |
|---|
|
Systems affected |
|
Progression of motor symptoms Dystonia |
Fragmentation of Dosing
Dopamine Agonists Contraindicated
L-dopa and Dietary Proteins
Motor Issues
Dyskinesias
Dystonia
Freezing
Nonmotor Complications
Hallucinations, Delusions, Psychosis
Depression and Anxiety
Managing Advanced Parkinsons Disease
Advanced Parkinsons disease, stage 4 or 5 of the Hoehn and Yahr Scale, is characterized by very limited mobility without assistance, severe motor deficits, risk of falls, and cognitive and psychotic problems. With the advent of L-dopa and other dopaminergic treatments, the progression of PD has become markedly slower however, over the years treatment loses its efficacy, while a number of complicationssuch as motor fluctuations and dyskinesiadevelop, probably due to the progressive loss of dopaminergic neurons and their striatal and cortical connections. These complications are observed in 50% of patients after 5 years of disease and in 80% of patients after 10 years of treatment .
Treatment of the advanced stages of PD is entirely different from earlier stages. Early treatment is geared towards symptom relief and prevention of motor symptoms. During the later stages, the palliative care model is introduced to provide the patient with comfort and support. In the advanced stages, the focus of treatment shifts to treating nonmotor symptoms using a more supportive and palliative approach .
Also Check: Power Up For Parkinson’s
Myth : Aside From Medication There Isnt Much You Can Do
Fact: This it is what it is theres nothing I can do to help myself myth is counterproductive. There is a lot you can do chiefly, keeping as active as you can. A recent study found that patients with Parkinsons who took part in weekly, hourlong exercise sessions were able to do more in their daily lives than those who did not.
Fully Developed Severely Disabling Disease The Patient Is Still Able To Walk And Stand Unassisted But Is Markedly Incapacitated
The patient is unable to lead an independent life because of the need for help with some activities of daily living. It is this inability to live alone which marks the transition from Stage III to Stage IV. No matter how difficult it is for him/her, if the patient still is able to live alone, his/her disease is at Stage III not Stage IV. The patient at Stage IV however, does remain able to stand and walk unassisted.
Recommended Reading: Parkinson’s And Personality Changes
Two Areas In Which Parkinsons Disease May Bring About Death
I. Falls
PD patients are at an increased risk of falling and bad falls can lead to death. This usually occurs as a complication of a fall that requires hospitalization, particularly if it involves surgery. While most people do not fracture their hips when they fall, some do, and hip surgery, while routine, is still major surgery. It carries the risk of infection, delirium related to pain medications and anesthesia, heart failure, pneumonia, blood clots in the legs that then go to the lungs, and general weakness from immobility. Hip fractures are probably the main cause for death for those who fall, but people can fracture other bones and require surgery. They may fracture their ribs, which leads to reduced coughing, because of the pain, and an increased risk of lung infections . It is surprisingly uncommon for Parkinsons Disease patients to die from brain injuries related to falls, but it still may occur.
II. Pneumonia
PD patients also may develop pneumonias completely unrelated to difficulties with swallowing, just like their non-PD friends and relatives.
What Are The Different Stages Of Parkinsons Disease
Each person with Parkinsons disease experiences symptoms in in their own unique way. Not everyone experiences all symptoms of Parkinsons disease. You may not experience symptoms in the same order as others. Some people may have mild symptoms others may have intense symptoms. How quickly symptoms worsen also varies from individual to individual and is difficult to impossible to predict at the outset.
In general, the disease progresses from early stage to mid-stage to mid-late-stage to advanced stage. This is what typically occurs during each of these stages:
Early stage
Early symptoms of Parkinsons disease are usually mild and typically occur slowly and do not interfere with daily activities. Sometimes early symptoms are not easy to detect or you may think early symptoms are simply normal signs of aging. You may have fatigue or a general sense of uneasiness. You may feel a slight tremor or have difficulty standing.
Often, a family member or friend notices some of the subtle signs before you do. They may notice things like body stiffness or lack of normal movement slow or small handwriting, lack of expression in your face, or difficulty getting out of a chair.
Mid stage
Mid-late stage
Standing and walking are becoming more difficult and may require assistance with a walker. You may need full time help to continue to live at home.
Advanced stage
You May Like: Homeopathic Medicine For Parkinson Disease
Medicines For Parkinson’s Disease
Medicines prescribed for Parkinson’s include:
- Drugs that increase the level of dopamine in the brain
- Drugs that affect other brain chemicals in the body
- Drugs that help control nonmotor symptoms
The main therapy for Parkinson’s is levodopa, also called L-dopa. Nerve cells use levodopa to make dopamine to replenish the brain’s dwindling supply. Usually, people take levodopa along with another medication called carbidopa. Carbidopa prevents or reduces some of the side effects of levodopa therapysuch as nausea, vomiting, low blood pressure, and restlessnessand reduces the amount of levodopa needed to improve symptoms.
People with Parkinson’s should never stop taking levodopa without telling their doctor. Suddenly stopping the drug may have serious side effects, such as being unable to move or having difficulty breathing.
Other medicines used to treat Parkinsons symptoms include:
- Dopamine agonists to mimic the role of dopamine in the brain
- MAO-B inhibitors to slow down an enzyme that breaks down dopamine in the brain
- COMT inhibitors to help break down dopamine
- Amantadine, an old antiviral drug, to reduce involuntary movements
- Anticholinergic drugs to reduce tremors and muscle rigidity