Can A Patients Ability To Make Decisions In The Last Days Of Life Be Impaired And How Is This Managed
In a North American study of 47 carers of idiopathic PD patients in the last months of life most described the goal of care as comfort, and almost half of the patients were described as unable to make any decisions in the last month of life. 10
When presenting, the patient may already be unable to communicate their symptoms and care preferences due to cognitive impairment and confusion. Also, there might be a physical difficulty in communication from severe rigidity. Care should be taken in considering the presence and consequent treatment of an intercurrent illness, and whether dopaminergic medication is exacerbating confusion due to hallucinations and/or psychosis.27
Continued attempts at verbal and non-verbal communication should be made throughout given the often fluctuating symptoms associated with PD and possible improvement in the intercurrent illness. In the absence of a next of kin or other person who is able to inform the clinical team, decisions should be made on a best interest basis as recommended in end of life care guidance.30
You May Like: How Long Does A Person Live With Parkinsons Disease
Study Design And Participants
All the clinical data and 123I-FP-CIT SPECT images used in this study were downloaded from the PPMI database. The PPMI is an ongoing longitudinal, international, multicentre, observational clinical study of patients with early Parkinsons disease aimed at identifying disease biomarkers . The study ascertains patients with a clinical disease duration of < 2 years who periodically undergo clinical motor evaluation and imaging with 123I-FP-CIT SPECT. The diagnosis of Parkinsons disease had to be supported by an in vivo evidence of nigrostriatal dopaminergic dysfunction all patients with tremor and normal scans were followed up as a separate group . The full list of inclusion and exclusion criteria can be found in the PPMI study protocol, available online at .
Our analysis was focused on the period from baseline to the 2-year follow-up, as not enough patients had completed longer follow-ups. We therefore downloaded clinical motor assessments and 123I-FP-CIT SPECT images at both baseline and 2-year follow-up from the PPMI database in August 2015. For patients who did not have a 2-year assessment the previous or successive one was used.
Stage Four Of Parkinsons Disease
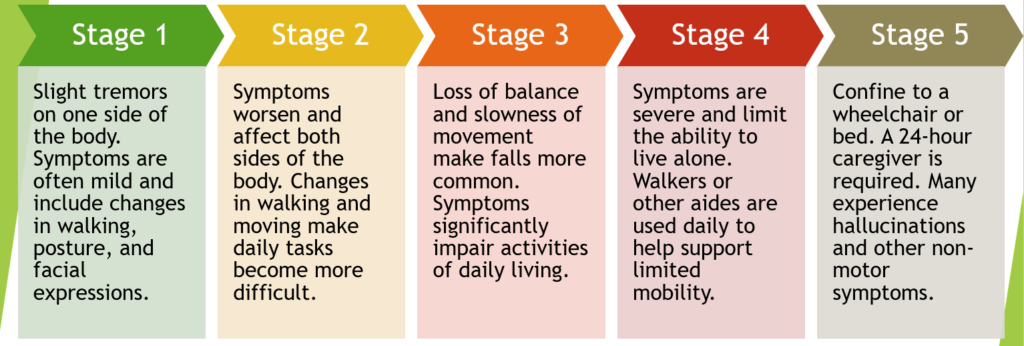
In stage four, PD has progressed to a severely disabling disease. Patients with stage four PD may be able to walk and stand unassisted, but they are noticeably incapacitated. Many use a walker to help them.
At this stage, the patient is unable to live an independent life and needs assistance with some activities of daily living. The necessity for help with daily living defines this stage. If the patient is still able to live alone, it is still defined as stage three.
Also Check: On Off Phenomenon
What Are The Considerations For Pain Management In The Last Days Of Life In Pd
It is important to consider that pain can be a risk factor for, and associated with, many other symptoms which might be the presenting features in a patient with complex or advanced PD. These include a new or worsened confusion, hallucinations, agitation and symptoms of depression or apathy.
As well as being an underlying cause of another symptom, pain can also be the symptom of other features of PD, such as rigidity, dyskinesia, but also non-motor features, for example, depression and fatigue.
Identifying whether pain is at the root of the presenting complaint and what might be causing the pain is therefore the most important part of the initial history from the patient and the carer. Then using the clinical examination to confirm findings from the history and identify any features not already elicited such as abnormal posturing, or dystonia.
A recent review into the pathophysiology and treatment of pain in PD suggests simple analgesia with paracetamol and non-steroidal anti-inflammatory drugs but advises caution with opiate analgesia as constipation is a recognised problem in PD patients.25 The review mentions, however, the lack of evidence for many widely used analgesics specifically in PD.26
Recommended Reading: Rehabilitation Programs For Parkinsons Disease
General Approach To Management
The primary goal in the management of PD is to treat the symptomatic motor and nonmotor features of the disorder, with the objective of improving the patients overall quality of life. Appropriate management requires an initial evaluation and diagnosis by a multidisciplinary team consisting of neurologists, primary care practitioners, nurses, physical therapists, social workers, and pharmacists., It is also important that the patient and his or her family have input into management decisions.
Effective management should include a combination of nonpharmacological and pharmacological strategies to maximize clinical outcomes. To date, therapies that slow the progression of PD or provide a neuroprotective effect have not been identified., Current research has focused on identifying biomarkers that may be useful in the diagnosis of early disease and on developing future disease-modifying interventions.,
You May Like: Parkinson’s Double Vision
Bilateral Or Midline Involvement Without Impairment Of Balance
Months or years later similar symptoms and signs are noticed on the opposite side of the body, or other signs appear in midline what physicians call Axial signs. These may include: bilateral loss of facial expression decreased blinking speech abnormalities soft voice, monotony, fading volume after starting to speak loudly, slurring, stiffness of truncal muscles making the patient appear awkward and stiff or resulting in neck and back pain postural abnormalities causing stooping, generalized slowness in, but still capable of, carrying out all activities of daily living, sometimes an aggravation to those waiting for the patient to complete tasks.
Usually the diagnosis is easy at this Stage if it has been preceded by a clear cut tremor or other symptom on one side. But not all Parkinson’s patients have tremor or other definite signs of Stage I unilateral Parkinsonism. If Stage I was missed and the predominant symptoms at Stage II are only slowness and a lack of spontaneous movement, the diagnosis may still be in doubt. For example, even in Stage II, Parkinsonism may be interpreted as only advancing age.
What Are The Stages Of Parkinsons
Doctors sometimes use five stages to describe the progress of Parkinsons disease. Each stage presents changing or new symptoms that a person is likely to encounter.
It is worth noting that not everyone will reach the advanced stages. For some people, the symptoms remain mild, and they can continue to live independently and be mobile.
Dividing the condition into stages helps doctors and caregivers understand and address some of the challenges a person is experiencing as it progresses.
Don’t Miss: What Foods Should Be Avoided When Taking Levodopa
Confirmed: No Slowing Of Parkinson’s Progression With Rasagiline
Erik Greb
A 1-mg daily dose of rasagiline has no disease-modifying effect for patients with Parkinson’s disease , new research confirms.
Results from a randomized, double-blind, placebo-controlled trial support previous observations that free-water accumulation in the posterior substantia nigra is a valid biomarker of disease progression.
However, at 1 year, pSN free-water accumulation was the same for the patients who received rasagiline and for those who received placebo.
Dr David Vaillancourt
“We’re using an imaging biomarker of the substantia nigra as the outcome variable, which has not been done before,” corresponding investigator David E. Vaillancourt, PhD, professor and chair of applied physiology and kinesiology at the University of Florida, Gainesville, Florida, told Medscape Medical News.
“We did not find evidence that rasagiline slows down the progression of the substantia nigra over time,” Vaillancourt said.
The findings were November 1 in Movement Disorders.
What You Can Expect
Parkinson does follow a broad pattern. While it moves at different paces for different people, changes tend to come on slowly. Symptoms usually get worse over time, and new ones probably will pop up along the way.
Parkinsonâs doesnât always affect how long you live. But it can change your quality of life in a major way. After about 10 years, most people will have at least one major issue, like dementia or a physical disability.
Read Also: Fitflop Shoes For Parkinson’s
Assessment Of Biomarkers’ Influence On Parkinson’s Disease Progression Model
Due to the great difference between the absence of biomarkers and other clinical variables, the initial inclusion would result in smaller amounts of data. So, biomarkers were added after model construction based on the clinical and scale scores data to evaluate their influence on the basic model. First, correlation analysis was performed between biomarkers and disease progression. Then the variables with significant correlation were selected to improve the models and we compared the model difference between before and after adding the biomarkers variables.
Stage Five Of Parkinsons Disease
Stage five is the most advanced and is characterized by an inability to rise from a chair or get out of bed without help, they may have a tendency to fall when standing or turning, and they may freeze or stumble when walking.
Around-the-clock assistance is required at this stage to reduce the risk of falling and help the patient with all daily activities. At stage five, the patient may also experience hallucinations or delusions.
While the symptoms worsen over time, it is worth noting that some patients with PD never reach stage five. Also, the length of time to progress through the different stages varies from individual to individual. Not all the symptoms may occur in one individual either. For example, one person may have a tremor but balance remains intact. In addition, there are treatments available that can help at every stage of the disease. However, the earlier the diagnosis, and the earlier the stage at which the disease is diagnosed, the more effective the treatment is at alleviating symptoms.
Recommended Reading: Parkinson’s Hallucinations Commercial
How Can Inpatient Rehabilitation Help
As a senior physical therapist at Encompass Health Fayetteville, Hammel works with Parkinsons patients at various stages of the disease. He said inpatient rehabilitation for Parkinsons can benefit even those who are only experiencing Parkinsons early signs and symptoms.
Honestly, I would say the moment you are diagnosed, rehabilitation can help, he said. Once youre diagnosed, one of the best things you can do is therapy. We can help with education and trying to regain independence or modify how you used to do things.
At an inpatient rehabilitation hospital such as Encompass Health, you will receive three hours of therapy five days a week, along with frequent visits from a rehabilitation physician. Occupational therapy can help you with activities of daily living, such as eating and grooming, physical therapy can help you build strength and balance, and speech therapy can help with speech and swallowing, as well as cognitive issues.
The goal of rehabilitation for Parkinsons patients, Hammel added, is to allow you to remain independent at home for as long as possible. If you or a loved one was recently diagnosed with Parkinsons disease or is experiencing more progressed symptoms, find an Encompass Health location near you, and talk to a rehabilitation specialist to see if inpatient rehabilitation could benefit you.
Are You Newly Diagnosed With Parkinsons
You have Parkinsons. Hearing these words from your doctor must have started an avalanche of emotions and thoughts in your mind, ranging from disbelief to sadness to disappointment and fear. It might be a moment you will never forget. Being diagnosed with a chronic condition can make you worry, especially with all the information available about potential changes in your body and difficulties with daily activities you may start to experience. A variety of questions would have risen in your mind about how it would be to live with or manage life with a chronic illness. You may have started asking yourself WHY ME?
Read Also: Does Vitamin B12 Help Parkinson’s
Stage 5 The Most Advanced Stage Of Parkinsons Disease
This is the late stage of Parkinsons disease where the patient completely depends on others for functioning. The patient finds it difficult to move and need a wheelchair. This stage is also accompanied by behavioral symptoms such as delusions and hallucinations. Moreover, the patient becomes sensitive to infections such as pneumonia.
One main limitation of the Hoehn and Yahr scale is that it entirely relies on motor symptoms and doesnt take into account the cognitive or other non-motor symptoms. Due to this, some physicians may prefer to use an alternative method known as the Unified Parkinsons disease Rating Scale. This scale is more inclusive as it covers both the motor symptoms and the non-motor symptoms, including mental functions, mood, behavior.
Disclaimer: The information shared here should not be taken as medical advice. The opinions presented here are not intended to treat any health conditions. For your specific medical problem, consult with your health care provider.
How Is Parkinsons Disease Treated
There is no cure for Parkinsons disease. However, medications and other treatments can help relieve some of your symptoms. Exercise can help your Parkinsons symptoms significantly. In addition, physical therapy, occupational therapy and speech-language therapy can help with walking and balance problems, eating and swallowing challenges and speech problems. Surgery is an option for some patients.
Also Check: How Do They Check For Parkinsons Disease
Also Check: Sam Waterston Parkinson’s
Hospice Eligibility For Parkinsons Disease
Due to the progressive nature of Parkinsons disease, it can be challenging for families to know when their loved one is eligible for the support of hospice care. If a loved one has been diagnosed with six months or less to live or if they have experienced a decline in their ability to move, speak, or participate in the activities of daily living without caregiver assistance, it is time to speak with a hospice professional about next steps.
Read Also: Can A Datscan Diagnose Parkinsons
What Can Be Done
The first step is to get a referral to a speechlanguage pathologist . This professional will take a medical history and interview you about eating and swallowing. Next you will probably have a swallowing evaluation, using either a video x-ray or an endoscopic exam. During this procedure, you will swallow different consistencies of food and liquids, and the SLP can observe the entire swallowing process: from your first sip and bite, through the mouth, down the throat and esophagus, and into the stomach. This is the best way to find out the extent and cause of swallowing problems. Then the SLP can recommend treatment.
You May Like: Does Sam Waterston Have Parkinsons
Vascular Defects Appear To Underlie The Progression Of Parkinson’s Disease
- Date:
- Georgetown University Medical Center
- Summary:
- In an unexpected discovery, researchers have identified what appears to be a significant vascular defect in patients with moderately severe Parkinson’s disease. The finding could help explain an earlier outcome of the same study, in which the drug nilotinib was able to halt motor and non-motor decline in the long term.
In an unexpected discovery, Georgetown University Medical Center researchers have identified what appears to be a significant vascular defect in patients with moderately severe Parkinson’s disease. The finding could help explain an earlier outcome of the same study, in which the drug nilotinib was able to halt motor and non-motor decline in the long term.
The researchers say their finding, detailed in a study published November 12, 2021, in Neurology Genetics, suggests that blood vessel walls called the blood brain barrier, which normally act as a crucial filter to protect the brain against toxins as well as allow passage of nutrients to nourish it, doesn’t work correctly in some Parkinson’s patients: it prohibits toxins from leaving the brain and inhibits nutrients such as glucose from entering. Perhaps even more damaging, the dysfunctional barrier allows inflammatory cells and molecules from the body to enter and damage the brain.
Explore the latest scientific research on sleep and dreams in this free online course from New Scientistâ
Story Source:
Stage Three Of Parkinsons Disease
Stage three is considered mid-stage and is characterized by loss of balance and slowness of movement.
Balance is compromised by the inability to make the rapid, automatic and involuntary adjustments necessary to prevent falling, and falls are common at this stage. All other symptoms of PD are also present at this stage, and generally diagnosis is not in doubt at stage three.
Often a physician will diagnose impairments in reflexes at this stage by standing behind the patient and gently pulling the shoulders to determine if the patient has trouble maintaining balance and falls backward . An important clarifying factor of stage three is that the patient is still fully independent in their daily living activities, such as dressing, hygiene, and eating.
Read Also: Parkinson Bicycle Cleveland Clinic
Fully Developed Severely Disabling Disease The Patient Is Still Able To Walk And Stand Unassisted But Is Markedly Incapacitated
The patient is unable to lead an independent life because of the need for help with some activities of daily living. It is this inability to live alone which marks the transition from Stage III to Stage IV. No matter how difficult it is for him/her, if the patient still is able to live alone, his/her disease is at Stage III not Stage IV. The patient at Stage IV however, does remain able to stand and walk unassisted.
Unified Parkinsons Disease Rating Scale

The UPDRS contains four parts. The first part assesses intellectual function, mood, and behavior. The second one assesses activities of daily living. The third part assesses one motor function, and the fourth assesses motor complications.
Each part includes scores that altogether rate the severity of the disease. The maximum score is 199, reflecting total disability, whereas a score of zero means no disability.
Recommended Reading: Parkinson’s Bike Therapy
Prediction Model Construction And Performance Measures
After eliminating the missing data, a total of 849 cases were left, among which 633 cases were placed in the training set and 216 in the test set according to the aforementioned dividing principles. The disease progression as expressed by the MDS-UPDRS Part III score of the coming year was predicted based on the information from the previous year. We built regression models based on five algorithms, and their performances are shown in Table 3. The models can be divided into three categories: linear, Bayesian and ensemble methods. The adjusted R2 of all the models reached above 0.75. The feature combinations obtained by the RFE method for models in the same category were similar and the feature importance or coefficient of each model is shown in Table 4. The models from each of the categories jointly selected the same three features: MDS-UPDRS Part III score, MOCA Score and RBDSQ score. All coefficients of regression models are shown in Table 5.
Table 3. The performance of five regression models.
Table 4. The feature importance or coefficient of features selected through RFE method in five regression models.
Table 5. All coefficients of regression models.
Figure 2. Prediction results and intervals of different widths in the RF regression model. Note that half width represents half of the width of the threshold range and acc represents the proportion of the true value that falls into the range.