Subgroup Analysis With Apoe 4
In those with APOE genotyping, 47.5% had one or two APOE 4 alleles. Patients with missing analysis for APOE were older and more commonly PDD patients . Comparison of baseline variables between carriers and non-carriers of APOE4 showed no significant differences .
Unadjusted bivariate Cox regression showed an HR of 1.45 in carriers of APOE4. Investigating the interaction between diagnosis and APOE4, displayed that patients with DLB and APOE4 had increased hazard in an age- and sex-adjusted model. A significant increased hazard was not found in APOE4 PDD patients .
In the relative survival model, adjusting for expected mortality, eHR was 1.77 for APOE4 carriers. Testing the model with the interaction between DLB and APOE4 showed an eHR of 2.00 . No significant effect was seen for PDD patients .
Study Setting Design And Participants
We retrospectively identified all patients who received a diagnosis of DLB or PDD at the Memory Clinic in Malmö, Skåne University Hospital, Sweden, between 19972014. All data was collected from the clinics electronical medical records.
The Memory Clinic in Malmö is a secondary care clinic specializing in cognitive disorders, situated in Swedens third largest city Malmö . According to regional guidelines, all patients with suspected DLB or PDD should be referred to the Memory Clinic from their primary care physician or other care institutions, where the patients will receive a diagnosis after a structured medical history, physical, psychiatric and neurological examination, cognitive testing, blood samples, CT or MRI of the brain. Further investigations, such as EEG, molecular imaging or CSF analysis, are conducted when judged appropriate by the responsible clinician. A small number of patients are also referred for post-mortem examination.
Patients with a diagnostic code of DLB or PDD in the electronic medical records were identified up until 31st of December 2014. Author VL reviewed the medical records to confirm the diagnoses according to consensus criteria for DLB and criteria for PDD . Patients lacking information to fulfill the diagnostic criteria or with a diagnosis prior to the introduction of electronic medical records in 1997 were excluded.
What Is The Self
Protein in the diet may affect the absorption of levodopa, the major medication used to treat Parkinson’s disease. Fluctuations in the level of levodopa may worsen some behavioral and cognitive symptoms. A low-protein diet may reduce fluctuations in dopamine levels. In some patients with these fluctuations, dietary changes can improve symptoms. However, it is important to ensure that the person is getting adequate calories and other nutrients.
People with Parkinson’s disease should remain as active as possible. Physical therapy helps the person maintain mobility.
In general, people with Parkinson’s disease plus dementia should no longer drive vehicles. Movement problems may prevent quick reactions in hazardous driving situations. Certain medications, especially those given to treat symptoms of dementia, may make them less alert. However, this should be determined on an individual basis and in compliance with the laws of the state.
YOU MAY ALSO LIKE
Read Also: Weighted Silverware
Palliative Care In Dementia
The first evaluated palliative care program specific to dementia was described in 1986 . The volume of research has grown exponential after 2000 . There are few randomized controlled trials, and therefore, there is still little evidence on effectiveness . However, many western countries have funded observational studies resulting in numerous publications describing patient, family and professional caregiver needs .
Research specific to dementia is important because the course of the disease is highly variable and uncertain. Because of the progressive dementia, patients themselves often cannot remain involved in decision making. Also, health services and changes such as transfer to a hospice, do not necessarily represent optimal care for people with dementia . Palliative care in dementia needed a clear conceptualization, and the European Association for Palliative Care along with experts agreed to a distinct concept in terms of eleven domains, different from usual palliative care .
What Are The Signs Of End
It is important for caregivers to know when an individual with dementia is close to the end of their life, because it helps ensure they receive the right amount of care at the right time. It can be difficult to know exactly when this time is due to the variable nature of dementias progression, but understanding common end-of-life symptoms of seniors with dementia can help. Below is a timeline of signs of dying in elderly people with dementia:
Final Six Months
- A diagnosis of another condition such as cancer, congestive heart failure or COPD
- An increase in hospital visits or admissions
Final Two-to-Three Months
- Speech limited to six words or less per day
- Difficulty in swallowing or choking on liquids or food
- Unable to walk or sit upright without assistance
- Incontinence
- Hands, feet, arms and legs may be increasingly cold to the touch
- Inability to swallow
- Terminal agitation or restlessness
- An increasing amount of time asleep or drifting into unconsciousness
- Changes in breathing, including shallow breaths or periods without breathing for several seconds or up to a minute
Patients with dementia are eligible to receive hospice care if they have a diagnosis of six months or less to live if the disease progresses in a typical fashion. Once a patient begins experiencing any of the above symptoms, it is time to speak with a hospice professional about how they can help provide added care and support.
Recommended Reading: Does Sam Waterston Have Parkinsons
Do You Die From Pd Dementia
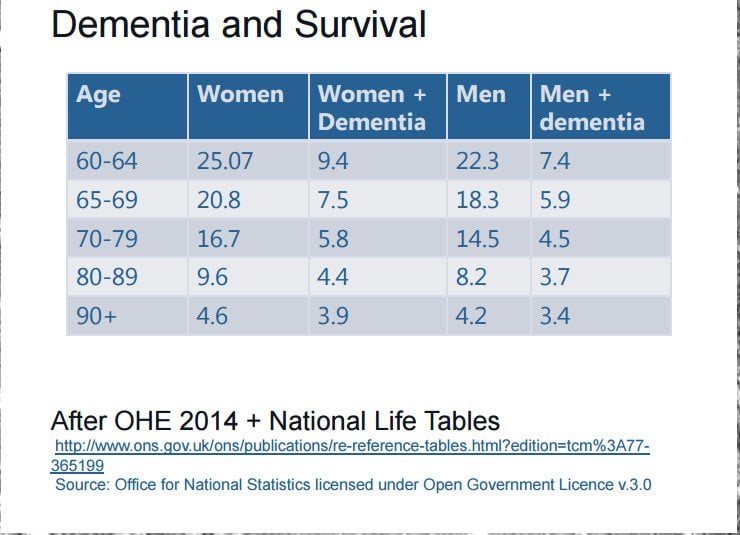
People with Parkinsons-related dementia often want to know how the disease can impact their lifespan. While people with Parkinsons can expect a similar lifespan to the general population, studies show both Parkinsons disease dementia and Lewy body dementia can shorten lifespan, generally due to medical complications from the disease, rather than the disease itself.
Professional Treatments & Lifestyle Changes
After being diagnosed with Parkinsons, the average person is going to be put on at least one or two medications. These drugs are usually designed to trigger the production of dopamine, which lessens the symptoms. Some seniors also undergo alternative treatments, such as deep brain stimulation, and many of those procedures have very high success rates. In addition to getting professional treatment, seniors with Parkinsons must also dedicate themselves to making healthy lifestyle choices. Exercising, socializing, getting plenty of sleep, and sticking to a nutritious diet can all be very beneficial.
A professional caregiver can be a wonderful source of support for a senior with Parkinsons. Families looking for top-rated senior care providers can reach out to Home Care Assistance. From respite care to specialized Alzheimers, dementia, stroke, and Parkinsons care, there are many ways we can make life easier for seniors and their loved ones. To learn about our high-quality in-home care options, give us a call at 573-4213 today.
Don’t Miss: Yopd Life Expectancy
Why Knowing Life Expectancy Is Useful
Knowing what to expect, including life expectancy helps with planning. Someone predicted to survive for five or six years, as opposed to two years, will want to make more extensive plans, including getting an estate in order, activity planning, and budget. Knowing how quickly the disease is expected to progress symptomatically can impact care decisions. If the disease is predicted to come on very quickly, for example, then skipping traditional assisted living and looking into memory care or a nursing home might be the best option.
Knowing when full-time care becomes a requirement, either at-home or in a memory care residence, is especially useful given the high cost of care. It is estimated that 50% of nursing home residents have some level of dementia and over 60% of nursing home residents care is paid for by Medicaid. Medicaid eligibility is complicated, and families can spend up to 5 years waiting for a loved one with dementia to become Medicaid-eligible. Therefore, knowing how soon care is required can make a huge financial difference.
Contribute anonymously to our dementia life expectancy database. Start here.
Thanks For Signing Up
We are proud to have you as a part of our community. To ensure you receive the latest Parkinsons news, research updates and more, please check your email for a message from us. If you do not see our email, it may be in your spam folder. Just mark as not spam and you should receive our emails as expected.
Don’t Miss: Prayers For Parkinson’s Disease
Signs Of Dying In The Elderly With Dementia
Dementia is a general term for a chronic or persistent decline in mental processes including memory loss, impaired reasoning, and personality changes. Alzheimers disease is the most common form of dementia, accounting for 60-80% of all cases of dementia. It is also the 6th leading cause of death in the United States, and over 5 million Americans are currently living with Alzheimers disease.
Alzheimers disease and most progressive dementias do not have a cure. While the disease inevitably worsens over time, that timeline can vary greatly from one patient to the next.
Caring for a loved one can be challenging and stressful, as the individuals personality changes and cognitive function declines. They may even stop recognizing their nearest and dearest friends and relatives. As dementia progresses, the individual will require more and more care. As a family caregiver, its important to be able to recognize the signs of dying in elderly with dementia. Hospice can help by offering care wherever the individual resides, providing physical, emotional and spiritual care to the patient and support their family.
Life Expectancy Of Parkinsonism Patients In The General Population
Absolute life expectancy estimates of parkinsonism are easy to translate to patients.
-
Patients with parkinsonism have a reduced life expectancy compared to matched controls.
-
The most prominent decrease in life expectancy is observed if parkinsonism is diagnosed before the age of 70.
-
The number of years lived with parkinsonism in the general population is relatively low.
Recommended Reading: Judy Woodruff Parkinson’s
Is There A Test To Diagnose Pd Dementia
There is no single test for PDD. The diagnosis is made clinically. If you or someone you spend time with notices cognitive changes, it is important to discuss them with your care team. If you dont have a care team in place, its important to find a specialist or physician familiar with dementia or geriatric medicine. Call the Parkinson’s Foundation Helpline 1-800-4PD-INFO for a referral.
Definition Of Parkinsons Disease

Parkinsons syndrome is characterized by the clinical triad of rigor, tremor, and akinesia as well as possible postural instability.
Based on etiology, one can further distinguish between idiopathic Parkinsons disease, which is synonymous with Parkinsons disease, and atypical and symptomatic parkinsonism.
Idiopathic Parkinsons disease or Parkinsons disease is considered a diagnosis of exclusion, in the absence of a specific cause.
Symptomatic Parkinsonism, however, is triggered by certain identifiable factors. For example, in the context of intoxication, manganese or lead may cause the disease. Parkinsons syndrome is also triggered by medication, e.g., neuroleptics.
Parkinsons syndrome occurring in the context of other neurodegenerative diseases is referred to as atypical Parkinsonism.
Recommended Reading: Does Vitamin B12 Help Parkinson’s
How Can We Support The Sleep/wake Cycle Of Pdd
For people with PDD who are confused about the day-night cycle, some daily strategies can be helpful. At night, starting a lights out routine that happens at the same hour every day, where all curtains are closed and lights are turned off, can help the person understand that it is sleep time. During the day, opening the curtains, allowing the person with PDD to spend as much time in the daylight as possible, avoiding naps, and organizing stimulating activities, can be helpful. Having lots of calendars and clocks in every room might also help a person with PDD be less confused about the time of day.
What Are Parkinson’s Disease Dementia Medical Treatment And Medications
There is no specific therapy for dementia in Parkinson’s disease. Although cognitive symptoms initially may appear to respond to drugs that promote dopamine production, the improvement is mild and transient in contrast to the early responses to motor control improvement with medication in patients with Parkinson’s disease.
Parkinson’s disease dementia medications
Various medications are used to treat the movement disorders of Parkinson’s disease, some may exacerbate symptoms related to dementia.
- These include dopamine given in the form of levodopa medications known as dopamine agonists that act on the dopamine receptor and medications that slow down the metabolism of dopamine. They are often used in conjunction with monoamine oxidase inhibitors such as rasagiline. In addition, anticholinergic drugs are sometimes used.
- Unfortunately, these drugs may affect cognitive symptoms and mood disorders.
- Anticholinergic drugs, for example, help balance levels of dopamine and acetylcholine, another neurotransmitter, in the brain. These drugs can improve movement disorders but often make memory loss worse.
The dementia of Parkinson’s disease may respond to drugs used in patients with Alzheimer’s disease. However, these drugs, called cholinesterase inhibitors , lead to only small and temporary improvements in cognition.
Mood disorders and psychoses are usually treated with other medication.
You May Like: Fitflop Shoes For Parkinson’s
Michael J Fox Says Having Parkinson’s Disease ‘sucks’
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
It’s thought around one in 500 people are affected by Parkinson’s disease, according to the NHS. The disease is known to affect the brain, and well-known symptoms include problems like a tremor. According to studies, taking two vitamins could help to lower your risk in later life.
Eat Healthy Meals Throughout The Day
- Consuming a variety of foods from all five food groups provides consistent energy and keeps your immune system healthy. Focus on eating a minimum of five fruits and vegetables each day, eating a variety of high fiber foods, and staying hydrated, all of which help prevent constipation, which is often an issue for people diagnosed with YOPD.
- Watch this to learn how to use nutrition to help you live well with Parkinsons.
You May Like: Parkinson’s Double Vision
Who Gets Early Onset Parkinsons Disease
About 10%-20% of those diagnosed with Parkinsons disease are under age 50, and about half of those are diagnosed before age 40. Approximately 60,000 new cases of Parkinsons are diagnosed each year in the United States, meaning somewhere around 6,000 12,000 are young onset patients.
Is it genetic or hereditary?
The cause of Parkinsons disease is not yet known. However, Parkinsons disease has appeared across several generations of some families, which could indicate that certain forms of the disease are hereditary or genetic. Many researchers think that Parkinsons disease may be caused by genetic factors combined with other external factors. The field of genetics is playing an ever greater role in Parkinsons disease research, and scientists are continually working towards determining the cause or causes of PD.
You May Like: Can Head Injury Cause Parkinsons
How Is Parkinsons Disease Dementia Diagnosed
No single test can diagnose Parkinsons disease dementia. Instead, doctors rely on a series or combination of tests and indicators.
Your neurologist will likely diagnose you with Parkinsons and then track your progression. They may monitor you for signs of dementia. As you get older, your risk for Parkinsons dementia increases.
Your doctor is more likely to conduct regular testing to monitor your cognitive functions, memory recall, and mental health.
Read Also: Parkinson’s Bike Therapy
Parkinson’s Disease Dementia Surgery And Gene Therapy
- Great strides have been made in the surgical treatment of Parkinson’s disease. Several different procedures are now available, and they are successful in many patients in relieving movement symptoms. Unfortunately, surgery has no effect on cognitive symptoms. In fact, most people with dementia are not candidates for surgery.
- Gene therapy is in its infancy there are ongoing human and animal trials with various methods to insert genes into neuronal cells to reduce or stop Parkinson’s disease symptoms by causing cells to produce dopamine coded by the newly inserted genes. Early results with the treatment termed ProSavin are encouraging. However, it is not clear if such therapy could prevent or reverse Parkinson’s disease dementia.
What Is Parkinson’s Disease Dementia
Parkinson’s disease is an age-related degenerative disorder of certain brain cells. It mainly affects movements of the body, but other problems, including dementia, may occur. It is not considered a hereditary disease, although a genetic link has been identified in a small number of families.
- The most common symptoms of Parkinson’s disease are tremor of the hands, arms, jaw, and face rigidity of the trunk and limbs slowness of movement and loss of balance and coordination.
- Other symptoms include shuffling, speaking difficulties, , facial masking , swallowing problems, and stooped posture.
- The symptoms worsen gradually over years.
Depression, anxiety, personality and behavior changes, sleep disturbances, and sexual problems are commonly associated with Parkinson’s disease. In many cases, Parkinson’s disease does not affect a person’s ability to think, reason, learn, or remember .
About 500,000 people in the United States have Parkinson’s disease, and about 50,000 new cases are diagnosed each year. The number of those who have some cognitive symptoms is difficult to pinpoint because accurate data are lacking for the following reasons:
Most people have the first symptoms of Parkinson’s disease after the age of 60 years, but Parkinson’s disease also affects younger people. Early-onset Parkinson’s disease strikes people around the age of 40 years, or even earlier.
You May Like: Parkinson’s Hallucinations Commercial
Identifying Risk Factors For Parkinson’s
The risk for early death increased by about 40% for every 10-year increase in age at diagnosis.
Parkinsonâs researcher Tobias Kurth, MD, agrees that identifying risk factors for early death could help clinicians better manage the disease.
Kurth is an adjunct associate professor of epidemiology at Harvard School of Public Health.
âThis is important research that adds to our understanding of the impact of specific features of Parkinsonâs disease on outcomes,â he tells WebMD.
His own study of Parkinsonâs-associated death matched Parkinsonâs patients with people without the disease who had similar non-Parkinsonâs-related illnesses.
Like the newly reported study, patients who were older when their Parkinsonâs disease was diagnosed had a greater risk for early death.
Show Sources